Abstract
The paracrine loop involving inflammatory cytokines between adipocytes and macrophages establishes a vicious cycle that aggravates pro-inflammatory changes in adipose tissue. The serum level of hepatocyte growth factor (HGF) is increased in metabolic syndrome, but whether HGF is beneficial or detrimental in inflammatory conditions is unclear. We previously reported that HGF has strong anti-inflammatory effects. We therefore hypothesized that HGF may inhibit chronic inflammation in adipose tissue by inhibiting the vicious cycle between adipocytes and macrophages. We stimulated the macrophage cell line RAW264 with HGF and evaluated pro-inflammatory cytokines. Coculturing differentiated 3T3-L1 adipocytes with RAW264 results in marked upregulation of pro-inflammatory cytokines. We examined whether HGF suppresses the upregulation of pro-inflammatory cytokines in this coculture system. Cardiac-specific HGF transgenic mice (HGF-Tg) were crossed with ApoE KO (knockout) mice, to yield ApoE KO/HGF-Tg mice, which were treated with a high-fat diet (HFD) and received angiotensin (Ang) II. The phenotypes of ApoE KO and ApoE KO/HGF-Tg mice were compared. Treatment with HGF reduced the expression of pro-inflammatory cytokine genes (Tumor necrosis factor-α, monocyte chemoattractant protein-1 and interleukin-6) in RAW264 and the coculture system. The anti-inflammatory effects of HGF were also confirmed in in vivo studies. Macrophage infiltration in epididymal adipose and fatty liver was reduced in ApoE KO/HGF-Tg. Adipocyte diameter was reduced in ApoE KO/HGF-Tg, and the serum adiponectin level was upregulated. These beneficial effects in ApoE KO/HGF-Tg mice under HFD and Ang II infusion were abrogated by an anti-HGF neutralizing antibody. These results suggest that HGF inhibits the vicious cycle of adipocytes and macrophages through the inhibition of macrophage-mediated pro-inflammatory cytokines and upregulation of adiponectin in adipocytes. These favorable effects may suppress chronic inflammation in adipose tissue.
Similar content being viewed by others
Introduction
Metabolic syndrome, an extremely frequent condition characterized by dyslipidemia, insulin resistance, abdominal obesity and hypertension, is associated with an elevated risk of cardiovascular events. Chronic inflammation in fat is believed to have a crucial role in the development of obesity-related insulin resistance.1 Obesity is associated with macrophage accumulation in adipose tissue.2 As one of the key factors that could stimulate chronic inflammation, vascular endothelial growth factor is believed to exaggerate chronic inflammation and contribute to the progression of metabolic syndrome.3 Indeed, the circulating level of vascular endothelial growth factor is increased in adipose tissue in metabolic syndrome. In contrast, previous studies showed that hepatocyte growth factor (HGF) mediated multiple biological effects including anti-fibrotic, anti-inflammatory and anti-apoptotic activity in various cells and in vivo using HGF transgenic mice (HGF-Tg).4 Our report also demonstrated that HGF attenuated the senescence of endothelial progenitor cells induced by angiotensin (Ang) II through a reduction in oxidative stress.5 HGF inhibited the proliferation of vascular smooth muscle cells and inflammation induced by Ang II.6 Moreover, Shimizu et al.7 revealed that HGF inhibited lipopolysaccharide-induced oxidative stress and inflammation using HGF-Tg. Iwabayashi et al.8 reported that HGF inhibited atherosclerosis, senescence and oxidative stress mediated by lipoprotein (a), one of the risk factors for peripheral artery disease.
Interestingly, there was a significant association between serum HGF level and the degree of abnormality of the components of metabolic syndrome.9 HGF level is reported to be significantly related to waist circumference, high-density lipoprotein cholesterol and liver enzymes. Another study showed that elevated serum HGF level was also significantly associated with the development of insulin resistance.10 Thus, it is noteworthy to understand whether HGF exaggerates inflammation or mediates anti-inflammatory effects in adipose tissue. In this study, we employed ApoE KO (knockout) mice with continuous infusion of Ang II as an animal model of chronic inflammation in adipose tissue with hypertension. Using ApoE KO mice crossed with cardiac-specific HGF-Tg, the present study demonstrated anti-inflammatory effects of HGF in adipocytes and macrophages in vitro and in vivo.
Methods
Cell culture
The RAW264 macrophage cell line (RIKEN BioResourceCenter, Saitama, Japan) and 3T3-L1 preadipocytes (American Type Culture Collection, Manassas, VA, USA) were maintained in Dulbecco's modified Eagle’s medium (Nacalai Tesque, Kyoto, Japan) containing 10% fetal bovine serum (Sanko Junyaku, Tokyo, Japan) and antibiotics, and incubated at 37 °C in a humidified 5% CO2/95% air atmosphere. Differentiation of 3T3-L1 preadipocytes to mature adipocytes was induced, as described previously. Human recombinant HGF was purchased from PeproTech EC, London, UK.
RAW264 cells were plated in 6-cm dishes maintained at 37 °C in a humidified atmosphere containing 5% CO2 for 24 h. Cells were treated with the indicated concentrations of HGF for 48 h and harvested.
Coculture of adipocytes and macrophages
Coculture of adipocytes and macrophages was performed as follows (Figure 2A). In the contact system, serum-starved differentiated 3T3-L1 were cultured in 6-cm dishes, and RAW264 macrophages (1 × 105 cells per dish) were plated onto 3T3-L1. The cells were cultured for 48 h in contact with each other and harvested. To promote pro-inflammatory conditions, Ang II (Sigma, St Louis, MO, USA) was added to this coculture system. 3T3-L1 adipocytes were pretreated with HGF (50 ng ml−1) for 12 h before coculture. As control, adipocytes and macrophages, the numbers of which were equal to those in the contact system, were cultured separately and mixed after harvest.
Quantitative real-time PCR
Total RNA was extracted from cultured cells and quantitative real-time PCR was performed with an ABI Prism 7000 Sequencer (Foster City, CA, USA). Primer sets were as follows:
Mouse monocyte chemoattractant protein-1 (MCP-1): forward 5′-CCACTCACCTGCTGCTACTCAT-3′,
reverse 5′-TGGTGATCCTCTTGTAGCTCTCC-3′,
Interleukin (IL)-6: forward 5′-ACAACCACGGCCTTCCCTACTT-3′,
reverse 5′-CACGATTTCCCAGAGAACATGTG-3′,
Tumor necrosis factor (TNF)-α: forward 5′-ACCCTCACACTCAGATCATCTTC-3′,
reverse 5′-TGGTGGTTTGCTACGACGT-3′,
GAPDH: forward 5′-TGCACCACCAACTGCTTAG-3′,
reverse 5′-GGATGCAGGGATGATGTTC-3′.
Levels of messenger RNA were normalized to that of GAPDH.
ApoE/HGF-Tg mouse model and animal experiment protocol
Mice (C57BL6 background) with cardiac-specific (α-myosin heavy chain-driven) overexpression of human HGF with a high level of heart-derived serum HGF were generated, as previously reported.5 ApoE KO mice were used as a murine model exhibiting fatty liver and hyperlipidemia as a terminal outcome of chronic inflammation in adipose tissue. Male ApoE KO mice with a C57/BL6 background were obtained from the Jackson Laboratory (Bar Harbor, ME, USA). HGF-Tg were crossed with ApoE KO mice to yield ApoE KO/HGF-Tg mice. Anti-HGF neutralizing antibody was purchased from Kringle Pharma (Osaka, Japan).
Ang II promotes the release of these pro-inflammatory cytokines from both mature adipocytes and preadipocytes.11, 12, 13 In order to promote the pro-inflammatory phenotype of ApoE KO mice, Ang II (0.7 mg kg−1 per day) was administered to ApoE KO mice via an osmotic minipump (Alzet, Cupertino, CA, USA, model 1002) for 4 weeks after 4 weeks of high-fat diet (HFD) treatment (Figure 3A).
Eight-week-old mice (n=5 per group) were fed HFD (MF plus 0.5% (wt/wt) cholesterol and 10% yashi oil; Oriental Yeast, Tokyo, Japan). Mice were divided into three groups: (i) ApoE KO mice with HFD for 8 weeks and Ang II for 4 weeks; (ii) ApoE KO/HGF-Tg mice with HFD for 8 weeks and Ang II for 4 weeks; (iii) ApoE KO/HGF-Tg mice with HFD for 8 weeks and Ang II for 4 weeks, and 200 μg per week anti-HGF neutralizing antibody (Figure 3A). There were five mice per group, which were housed in the animal facilities of Osaka University (Osaka, Japan). The mice had free access to water and food during the experimental period. Following 3 months of drug and HFD treatment, the mice were killed. Samples of epididymal adipose tissue and liver were evaluated.
Measurement of HGF and adiponectin
HGF concentration was measured by an enzyme-linked immunosorbent assay (ELISA), using an IMMUNIS mouse HGF ELISA kit (Institute of Immunology, Tokyo, Japan). Mouse liver samples were disintegrated with IMMUNIS HGF extraction buffer, using a Multi-beads shocker (Yasui Kikai, Osaka, Japan) at 2000 g for 15 s. Homogenates were centrifuged at 14 000 g for 30 min. The supernatant was used for the HGF assay according to the manufacturer’s instructions. Serum adiponectin level was also measured using an ELISA kit (Otsuka Pharmaceuticals, Tokyo, Japan).
Immunohistochemical staining
Tissues fixed with 4% formalin and embedded in paraffin were subjected to immunohistochemical staining, as described previously.14 Immunostaining of F4/80 was performed using an anti-mouse F4/80 antibody (ab6640; Abcam, Cambridge, UK). Immunostained images were quantified using NIH Image J software (http://rsb.info.nih.gov/ij/) and then analyzed visually under a light microscope by two investigators blinded to treatment.
Statistical analysis
Data were expressed as mean±s.e.m. Comparisons were made using analysis of variance followed by Tukey–Kramer’s simultaneous multiple comparisons. P<0.05 was considered to indicate a statistically significant difference.
Results
Effect of HGF on pro-inflammatory cytokines in RAW264 macrophages and coculture system
As expected, in RAW264 cells, HGF significantly decreased messenger RNA levels of MCP-1, IL-6 and TNF-α from the basal level in a dose-dependent manner (Figure 1). Coculture of differentiated 3T3-L1 and RAW264 in the contact system revealed a significant increase in the expression of pro-inflammatory cytokines such as MCP-1, IL-6 and TNF-α as compared with the control culture (Figure 2, P<0.01). Moreover, addition of Ang II to this coculture system further stimulated the expression of these pro-inflammatory genes (Figure 2B). Importantly, pretreatment with HGF significantly attenuated the increases in messenger RNA levels of these cytokines (P<0.01). These data demonstrated that HGF exhibited anti-inflammatory effects in adipocytes and macrophages.
(A, B) Effects of hepatocyte growth factor on messenger RNA levels of monocyte chemoattractant protein-1 (a), tumor necrosis factor-α (b) and interleukin-6 (c) in the coculture contact system. Differentiated 3T3-L1 adipocytes were cocultured with RAW264 macrophages (1 × 105 cells per dish) for 24 h, and stimulated with angiotensin II (1 × 10−6 M). *P<0.01, †P<0.05 vs. Co-culture (n=4) #P<0.05 vs. Co-culture+Ang II. A full color version of this figure is available at the Hypertension Research journal online.
Anti-inflammatory effects of HGF in vivo
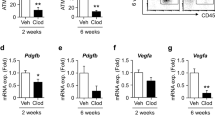
To confirm the anti-inflammatory effects of HGF in vivo, we generated HGF-Tg mice using ApoE KO mice (Figure 3A). Consistent with our previous reports,6 the serum HGF level was increased by 1.5- to 2-fold in ApoE KO/HGF-Tg mice (Figure 3B). Treatment with anti-HGF neutralizing antibody did not change the serum HGF level. Interestingly, the serum adiponectin level was significantly increased in ApoE KO/HGF-Tg mice (Figure 3C, P<0.05), whereas this increase in adiponectin level was attenuated by treatment with anti-HGF antibody. These data demonstrated that an increase in serum level of HGF stimulated an increase in the circulating adiponectin level. On the contrary, although lipid levels such as low-density lipoprotein cholesterol and triglyceride were not different among mice, serum high-density lipoprotein cholesterol was significantly increased in ApoE KO/HGF-Tg mice. In contrast, the serum free fatty acid level was significantly decreased in ApoE KO/HGF-Tg mice (Table 1). Importantly, anti-HGF antibody inhibited the increase in high-density lipoprotein cholesterol and the decrease in free fatty acid (Table 1, P<0.05).
Serum levels of hepatocyte growth factor (HGF) and adiponectin. (A) Experimental protocol. ApoE knockout mice (KO) mice with high-fat diet (HFD) for 8 weeks and angiotensin (Ang) II infusion for 4 weeks were divided into three groups: (a) ApoE KO mice with HFD for 8 weeks and Ang II for 4 weeks; (b) ApoE KO/HGF transgenic mice mice with HFD for 8 weeks and Ang II for 4 weeks; (c) ApoE KO/HGF-Tg mice with HFD for 8 weeks, Ang II for 4 weeks and anti-HGF neutralizing antibody (200 μg per week). (B) Serum HGF levels in each group. (C) Serum adiponectin levels in each group. *P<0.05 vs. ApoE KO mice, †P<0.05 vs. ApoE KO/HGF-Tg mice (n=5).
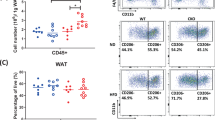
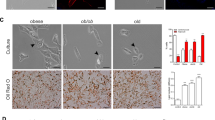
Although there was no significant difference in body weight and food intake between ApoE KO mice and ApoE KO/HGF-Tg mice, epididymal and retroperitoneal adipose tissue weight were significantly lowered in ApoE KO/HGF-Tg mice (P<0.05, Figure 4). Consistently, histological examination showed smaller adipocyte size and crown-like structures (formed by the gathering of macrophages) in ApoE KO/HGF-Tg mice, as demonstrated by F4/80 (a macrophage marker)-positive areas (Figure 5A). Consistent with the histological findings, F4/80-positive areas were also significantly decreased in ApoE KO/HGF-Tg mice (P<0.01, Figure 5B). Similarly, adipocyte diameter was significantly decreased in ApoE KO/HGF-Tg mice (Figure 5C). These beneficial changes in adipocytes were owing to HGF, as anti-HGF antibody significantly attenuated these changes (P<0.01). In this model, ApoE KO mice demonstrated a unique phenotype of severe fatty liver with marked deposition of lipid, as assessed by oil-red O staining (Figure 6a). Notably, ApoE KO/HGF-Tg mice exhibited a significant reduction in lipid accumulation, whereas anti-HGF antibody treatment significantly attenuated the decrease in lipid area (Figure 6b). There was no difference in blood pressure in each group both before and after 4 weeks of Ang II infusion (Table 2).
Macrophage infiltration and adipocyte diameter in adipose tissue of ApoE knockout mice (KO) mice and ApoE KO/hepatocyte growth factor transgenic mice mice. (A) Typical micrographs of immunostaining for F4/80 in periodic cross-sections of epididymal adipose tissue after 8 weeks of high-fat diet and 4 weeks of angiotensin II. Brown-stained area shows the F4/80 protein-positive area. (B) Quantitative data of immunohistochemical staining for macrophages (F4/80) (%). (C) Quantitative analysis of diameter of adipose cells (μm) *P<0.01 vs. ApoE KO mice, †P<0.01 vs. ApoE KO/HGF-Tg mice (n=5).
Lipid accumulation in liver of ApoE knockout mice (KO) mice and ApoE KO/hepatocyte growth factor transgenic mice mice. (a) Upper panels: typical micrographs of periodic cross-sections of liver with oil-red O staining after 8 weeks of high-fat diet and 4 weeks of angiotensin II; *P<0.01 vs. ApoE KO mice, †P<0.01 vs. ApoE KO/HGF-Tg mice (n=5).
Discussion
The present study demonstrated that HGF significantly reduced the expression of pro-inflammatory cytokines (MCP-1, TNF-α and IL-6) in not only RAW264 macrophages, but also in a RAW264 and 3T3-L1 adipocyte coculture system. It has been known that HGF exerts its anti-inflammatory action by disrupting NF-κB signaling.15 Previously, we proved HGF counteracts the progression of renal fibrosis by mediating the inhibition of phosphatase and tensin homolog. It is supposed that these mechanisms may underlie the anti-inflammatory effects by HGF.16 In a previous study, HGF suppressed the production of IL-6 in bone marrow-derived macrophages in vitro,17 and the expression of MCP-1 in tubular epithelial cells in vitro18 by its anti-inflammatory effects such as NF-κB inactivation. It is supposed that HGF inhibits inflammation mediated by M1-polarized macrophages. The summary of this study is shown in Figure 7.
Summary of anti-inflammatory effects of hepatocyte growth factor on the vicious cycle of macrophages and adipocytes. 1. Activated macrophages secreted pro-inflammatory cytokines (monocyte chemoattractant protein-1, interleukin-6 and tumor necrosis-α). 2. Adipocytes stimulated by pro-inflammatory cytokines became larger. 3. These hypertrophied adipocytes resulted in lower levels of adiponectin and higher levels of saturated fatty acids (such as FFA), which induced pro-inflammatory feedback to macrophages. 4. HGF inhibited this vicious cycle between macrophages and adipocytes by inhibiting pro-inflammatory cytokines from macrophages. 5. When the vicious cycle was inhibited by HGF, the adipocytes became smaller and the adiponectin level increased. A full color version of this figure is available at the Hypertension Research journal online.
To investigate the anti-inflammatory effects of HGF in vivo, we employed ApoE KO mice with HFD and Ang II infusion. This model showed a phenotype of chronic inflammation, including macrophage infiltration in adipose tissue, adipocyte hypertrophy and fatty liver. These findings were significantly reduced in ApoE KO/HGF-Tg mice as compared with ApoE KO alone mice. In our previous study, we demonstrated that irbesartan (a PPARγ agonistic ARB) mediated similar effects in ApoE KO mice. As PPARγ agonists are known to stimulate the expression of HGF, irbesartan could partially inhibit inflammation through the upregulation of HGF.19 The present study successfully proved the anti-inflammatory effects of HGF directly in vivo. Serum adiponectin level was increased in ApoE KO/HGF-Tg mice, and this was reversed by anti-HGF neutralizing antibody. HGF inhibited the vicious cycle mediated by macrophages and adipocytes by inhibiting pro-inflammatory cytokines from macrophages. These effects might maintain a small adipocyte size, and also induce adiponectin production from small adipocytes in vivo. It is well known that adiponectin improves many aspects of metabolic disorders such as obesity, atherosclerosis,20 type 2 diabetes,21 fatty liver22 and insulin resistance.23 Thus, the anti-inflammatory effects of HGF might be partially mediated by upregulation of adiponectin.
Recently, we reported that HGF inhibited/regressed myocardial fibrosis in a heart failure model using HGF-Tg mice, suggesting that circulating HGF could mediate cardioprotective effects.24 In dialysis patients with ischemic cardiomyopathy, circulating levels of HGF were reported to be increased.25, 26 As HGF secreted endogenously may act to protect against organ damage in local tissues such as the heart, a similar phenomenon might occur in chronic inflammation in adipose tissue.
Rehman et al. reported that obesity was associated with an increase in circulating HGF. Serum HGF levels in obese subjects were more than threefold higher than those in lean subjects. The increase in HGF concentration in obese subjects may not be secondary to insulin resistance or hypertension, as they also reported that freshly isolated human adipose cells secreted HGF.27 Recently, it was reported that mesenchymal stromal cells derived from adipose tissue also secreted HGF and improved acute kidney injury via paracrine/endocrine effects.28, 29 It is also reported that adipose-derived stem cells secreted HGF and improved brain damage in a murine stroke model.30 It is also reported that adipose tissue-derived stromal cells secreted HGF and showed potential as an angiogenic cell therapy in peripheral arteries for ischemic disease.31, 32 One possible explanation for these findings is that stem cells or mesenchymal stromal cells in adipose tissue could secrete HGF to repair tissue damage.
Currently, the relationship between HGF and non-alcoholic steatohepatitis and hepatocyte growth factor (NASH) is the center of interest, as HGF reduced liver fibrosis in NASH. It is also reported that HGF reduced fatty liver in murine models.33 In addition, serum HGF level was reported to be higher in NASH patients than in controls.34 Consistently, the present study demonstrated that HGF inhibited the lipid area in the liver in a fatty liver model. Bertola et al.35 reported that HGF induced glucose uptake in 3T3-L1 adipocytes and counteracted TNF-α. It is reported that HGF has a key role in the increase in islet cell mass and hyperinsulinemia in diet-induced obese rats, suggesting its role in insulin signaling in the liver.36 Further investigation is needed to clarify whether HGF improves other aspects of metabolic disorders such as insulin resistance and glucose tolerance. In conclusion, the present study demonstrated that the anti-inflammatory effects of HGF ameliorated the vicious cycle between adipocytes and macrophages in vitro and in vivo. HGF could be a novel therapeutic target to inhibit chronic inflammation in adipose tissue.
References
Xu H, Barnes GT, Yang Q, Tan G, Yang D, Chou CJ, Sole J, Nichols A, Ross JS, Tartaglia LA, Chen H . Chronic inflammation in fat plays a crucial role in the development of obesity-related insulin resistance. J Clin Invest 2003; 112: 1821–1830.
Weisberg SP, McCann D, Desai M, Rosenbaum M, Leibel RL, Ferrante AW . Obesity is associated with macrophage accumulation in adipose tissue. J Clin Invest 2003; 112: 1796–1808.
Hursting SD, Hursting MJ . Growth signals, inflammation, and vascular perturbations: mechanistic links between obesity, metabolic syndrome, and cancer. Arterioscler Thromb Vasc Biol 2012; 32: 1766–1770.
Taniyama Y, Azuma J, Iekushi K, Sanada F, Iwabayashi M, Kusunoki H, Okayama K, Otsu R, Rakugi H, Morishita R . The HGF/c-Met Receptor System Under Pathological Conditions. Immun Endocr Metab Agents Med Chem 2012; 12: 122–129.
Sanada F, Taniyama Y, Azuma J, Iekushi K, Dosaka N, Yokoi T, Koibuchi N, Kusunoki H, Aizawa Y, Morishita R . Hepatocyte growth factor, but not vascular endothelial growth factor, attenuates angiotensin II-induced endothelial progenitor cell senescence. Hypertension 2009; 53: 77–82.
Sanada F, Taniyama Y, Iekushi K, Azuma J, Okayama K, Kusunoki H, Koibuchi N, Doi T, Aizawa Y, Morishita R . Negative action of hepatocyte growth factor/c-Met system on angiotensin II signaling via ligand-dependent epithelial growth factor receptor degradation mechanism in vascular smooth muscle cells. Circ Res 2009; 105: 667–675.
Shimizu K, Taniyama Y, Sanada F, Azuma J, Iwabayashi M, Iekushi K, Rakugi H, Morishita R . Hepatocyte growth factor inhibits lipopolysaccharide-induced oxidative stress via epithelial growth factor receptor degradation. Arterioscler Thromb Vasc Biol 2012; 32: 2687–2693.
Iwabayashi M, Taniyama Y, Sanada F, Azuma J, Iekushi K, Okayama K, Chatterjee A, Rakugi H, Morishita R . Inhibition of Lp(a)-induced functional impairment of endothelial cells and endothelial progenitor cells by hepatocyte growth factor. Biochem Biophys Res Commun 2012; 423: 79–84.
Hiratsuka A, Adachi H, Fujiura Y, Yamagishi S, Hirai Y, Enomoto M, Satoh A, Hino A, Furuki K, Imaizumi T . Strong association between serum hepatocyte growth factor and metabolic syndrome. J Clin Endocrinol Metab 2005; 90: 2927–2931.
Tsukagawa E, Adachi H, Hirai Y, Enomoto M, Fukami A, Ogata K, Kasahara A, Yokoi K, Imaizumi T . Independent association of elevated serum hepatocyte growth factor levels with development of insulin resistance in a 10-year prospective study. Clin Endocrinol (Oxf) 2013; 79: 43–48.
Yvan-Charvet L, Quignard-Boulangé A . Role of adipose tissue renin-angiotensin system in metabolic and inflammatory diseases associated with obesity. Kidney Int 2011; 79: 162–168.
Skurk T, van Harmelen V, Hauner H . Angiotensin II stimulates the release of interleukin-6 and interleukin-8 from cultured human adipocytes by activation of NF-kappaB. Arterioscler Thromb Vasc Biol 2004; 24: 1199–1203.
Tsuchiya K, Yoshimoto T, Hirono Y, Tateno T, Sugiyama T, Hirata Y . Angiotensin II induces monocyte chemoattractant protein-1 expression via a nuclear factor-kappaB-dependent pathway in rat preadipocytes. Am J Physiol Endocrinol Metab 2006; 291: E771–E778.
Kusunoki H, Taniyama Y, Azuma J, Iekushi K, Sanada F, Otsu R, Iwabayashi M, Okayama K, Rakugi H, Morishita R . Telmisartan exerts renoprotective actions via peroxisome proliferator-activated receptor-γ/hepatocyte growth factor pathway independent of angiotensin II type 1 receptor blockade. Hypertension 2012; 59: 308–316.
Giannopoulou M, Dai C, Tan X, Wen X, Michalopoulos GK, Liu Y . Hepatocyte growth factor exerts its anti-inflammatory action by disrupting nuclear factor-kappaB signaling. Am J Pathol 2008; 173: 30–41.
Iekushi K, Taniyama Y, Kusunoki H, Azuma J, Sanada F, Okayama K, Koibuchi N, Iwabayashi M, Rakugi H, Morishita R . Hepatocyte growth factor attenuates transforming growth factor-β-angiotensin II crosstalk through inhibition of the PTEN/Akt pathway. Hypertension 2011; 58: 190–196.
Coudriet GM, He J, Trucco M, Mars WM, Piganelli JD . Hepatocyte growth factor modulates interleukin-6 production in bone marrow derived macrophages: implications for inflammatory mediated diseases. PLoS One 2010; 5: e15384.
Gong R, Rifai A, Tolbert EM, Biswas P, Centracchio JN, Dworkin LD . Hepatocyte growth factor ameliorates renal interstitial inflammation in rat remnant kidney by modulating tubular expression of macrophage chemoattractant protein-1 and RANTES. J Am Soc Nephrol 2004; 15: 2868–2881.
Chatterjee A, Kusunoki H, Taniyama Y, Rakugi H, Morishita R . Improvement of metabolic syndrome by irbesartan via the PPARγ/HGF pathway in apolipoprotein E knockout mice. Biomed Reports 2013; 1: 65–70.
Díez JJ, Iglesias P . The role of the novel adipocyte-derived hormone adiponectin in human disease. Eur J Endocrinol 2003; 148: 293–300.
Ukkola O, Santaniemi M . Adiponectin: a link between excess adiposity and associated comorbidities? J Mol Med (Berl) 2002; 80: 696–702.
Ezaki H, Yoshida Y, Saji Y, Takemura T, Fukushima J, Matsumoto H, Kamada Y, Wada A, Igura T, Kihara S, Funahashi T, Shimomura I, Tamura S, Kiso S, Hayashi N . Delayed liver regeneration after partial hepatectomy in adiponectin knockout mice. Biochem Biophys Res Commun 2009; 378: 68–72.
Yamauchi T, Kamon J, Waki H, Terauchi Y, Kubota N, Hara K, Mori Y, Ide T, Murakami K, Tsuboyama-Kasaoka N, Ezaki O, Akanuma Y, Gavrilova O, Vinson C, Reitman ML, Kagechika H, Shudo K, Yoda M, Nakano Y, Tobe K, Nagai R, Kimura S, Tomita M, Froguel P, Kadowaki T . The fat-derived hormone adiponectin reverses insulin resistance associated with both lipoatrophy and obesity. Nat Med 2001; 7: 941–946.
Okayama K, Azuma J, Dosaka N, Iekushi K, Sanada F, Kusunoki H, Iwabayashi M, Rakugi H, Taniyama Y, Morishita R . Hepatocyte growth factor reduces cardiac fibrosis by inhibiting endothelial-mesenchymal transition. Hypertension 2012; 59: 958–965.
Malatino LS, Mallamaci F, Benedetto FA, Bellanuova I, Cataliotti A, Tripepi G, Zoccali C . Hepatocyte growth factor predicts survival and relates to inflammation and intima media thickness in end-stage renal disease. Am J Kidney Dis 2000; 36: 945–952.
Malatino LS, Cataliotti A, Benedetto FA, Stancanelli B, Bellanuova I, Belluardo P, Bonaiuto L, Tripepi G, Mallamaci F, Castellino P, Zoccali C . Hepatocyte growth factor and left ventricular geometry in end-stage renal disease. Hypertension 2003; 41: 88–92.
Rehman J, Considine RV, Bovenkerk JE, Li J, Slavens CA, Jones RM, March KL . Obesity is associated with increased levels of circulating hepatocyte growth factor. J Am Coll Cardiol 2003; 41: 1408–1413.
Katsuno T, Ozaki T, Saka Y, Furuhashi K, Kim H, Yasuda K, Yamamoto T, Sato W, Tsuboi N, Mizuno M, Ito Y, Imai E, Matsuo S, Maruyama S . Low serum cultured adipose tissue-derived stromal cells ameliorate acute kidney injury in rats. Cell Transplant 2013; 22: 287–297.
Yasuda K, Ozaki T, Saka Y, Yamamoto T, Gotoh M, Ito Y, Yuzawa Y, Matsuo S, Maruyama S . Autologous cell therapy for cisplatin-induced acute kidney injury by using non-expanded adipose tissue-derived cells. Cytotherapy 2012; 14: 1089–1100.
Ikegame Y, Yamashita K, Hayashi S, Mizuno H, Tawada M, You F, Yamada K, Tanaka Y, Egashira Y, Nakashima S, Yoshimura S, Iwama T . Comparison of mesenchymal stem cells from adipose tissue and bone marrow for ischemic stroke therapy. Cytotherapy 2011; 13: 675–685.
Nakagami H, Morishita R, Maeda K, Kikuchi Y, Ogihara T, Kaneda Y . Adipose tissue-derived stromal cells as a novel option for regenerative cell therapy. J Atheroscler Thromb 2006; 13: 77–81.
Nakagami H, Maeda K, Morishita R, Iguchi S, Nishikawa T, Takami Y, Kikuchi Y, Saito Y, Tamai K, Ogihara T, Kaneda Y . Novel autologous cell therapy in ischemic limb disease through growth factor secretion by cultured adipose tissue-derived stromal cells. Arterioscler Thromb Vasc Biol 2005; 25: 2542–2547.
Kosone T, Takagi H, Horiguchi N, Ariyama Y, Otsuka T, Sohara N, Kakizaki S, Sato K, Mori M . HGF ameliorates a high-fat diet-induced fatty liver. Am J Physiol Gastrointest Liver Physiol 2007; 293: G204–G210.
Balaban YH, Sumer H, Simsek H, Us D, Tatar G . Metabolic syndrome, non-alcoholic steatohepatitis (NASH), and hepatocyte growth factor (HGF). Ann Hepatol 2006; 5: 109–114.
Bertola A, Bonnafous S, Cormont M, Anty R, Tanti JF, Tran A, Le Marchand-Brustel Y, Gual P . Hepatocyte growth factor induces glucose uptake in 3T3-L1 adipocytes through A Gab1/phosphatidylinositol 3-kinase/Glut4 pathway. J Biol Chem 2007; 282: 10325–10332.
Araújo TG, Oliveira AG, Carvalho BM, Guadagnini D, Protzek AO, Carvalheira JB, Boschero AC, Saad MJ . Hepatocyte growth factor plays a key role in insulin resistance-associated compensatory mechanisms. Endocrinology 2012; 153: 5760–5769.
Acknowledgements
We thank the members of the Department of Clinical Gene Therapy, Osaka University Graduate School of Medicine, for much helpful discussion and technical support. This work was partially supported by a Grant-in-Aid from the Organization for Pharmaceutical Safety and Research, a Grant-in-Aid from the Ministry of Public Health and Welfare, a Grant-in-Aid from Japan Promotion of Science, and funds from the Ministry of Education, Culture, Sports, Science and Technology of the Japanese Government.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
RM received honoraria, consulting fees and funds from Novartis, Takeda, Shionogi, Asteras, Boehringer Ingelfim, Daiichi-Sankyo and Pfizer. The remaining authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kusunoki, H., Taniyama, Y., Otsu, R. et al. Anti-inflammatory effects of hepatocyte growth factor on the vicious cycle of macrophages and adipocytes. Hypertens Res 37, 500–506 (2014). https://doi.org/10.1038/hr.2014.41
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2014.41
Keywords
This article is cited by
-
Cryopreserved cGMP-compliant human pluripotent stem cell-derived hepatic progenitors rescue mice from acute liver failure through rapid paracrine effects on liver cells
Stem Cell Research & Therapy (2024)
-
Suppression of lipopolysaccharide-induced corneal opacity by hepatocyte growth factor
Scientific Reports (2022)
-
HGF can reduce accumulation of inflammation and regulate glucose homeostasis in T2D mice
Journal of Physiology and Biochemistry (2021)
-
Topical cell-free conditioned media harvested from adipose tissue-derived stem cells promote recovery from corneal epithelial defects caused by chemical burns
Scientific Reports (2020)
-
NG2 glial cells regulate neuroimmunological responses to maintain neuronal function and survival
Scientific Reports (2017)