Abstract
The incidence of cardiovascular disease (CVD) is lower in younger women than in men of the same age, but it increases after menopause, implicating the atheroprotective action of endogenous estrogen. Although observational studies have suggested the efficacy of estrogen therapy in postmenopausal women, placebo-controlled, randomized trials, such as the Women's Health Initiative, have not confirmed effects of estrogen therapy on CVD. Conversely, basic, experimental research has progressed and provided mechanistic insight into estrogen's action on blood vessels. By contrast, the vascular effects of androgens remain poorly understood and have been controversial for a long time. In recent years, an increasing body of evidence has suggested that androgens may exert protective effects against the development of atherosclerosis, at least in elderly men. Epidemiological studies have shown that the incidence of and mortality due to CVD were increased in elderly men with low testosterone levels, although the efficacy of androgen therapy remains unknown. Furthermore, recent experimental studies have demonstrated the direct action of androgens on the vasculature. In this review, we illustrate the effects of sex steroids on the cardiovascular system, focusing on the action of testosterone on the blood vessels.
Similar content being viewed by others
Introduction
Since the 1940s, it has been recognized that sex steroids have important roles in the cardiovascular system.1, 2 A number of epidemiological studies have shown that sex differences are apparent in the incidence of atherosclerotic disease. The incidence of cardiovascular diseases (CVDs), such as hypertension and coronary artery disease, is lower in younger women than in men of the same age.3, 4, 5 However, it rises after menopause and, with age, catches up to that among men. These phenomena have been explained by the atheroprotective action of endogenous estrogen and its deprivation in postmenopausal women. In the past 20–30 years, many studies have suggested the efficacy of hormone replacement therapy (HRT) in postmenopausal women for the prevention of CVD and the putative vasoprotective effects of estrogen. However, reports from the Heart and Estrogen-Progestin Replacement Study (HERS)6 and the Women’s Health Initiative (WHI)7 denied the efficacy of estrogen therapy in CVD.
By contrast, the actions of androgens on the cardiovascular system remain unclear. In the process of atherosclerosis, androgens may exert complex effects on vessel walls. Both beneficial and detrimental effects have been reported. For many years, it was widely believed that androgens have unfavorable roles in the development of atherosclerosis. Recently, however, the link between androgen deficiency and atherosclerosis has been demonstrated in a number of studies.8, 9, 10 Various epidemiological and experimental studies have also demonstrated that androgens exert beneficial influences on CVD via the direct and indirect action of androgens on the blood vessels.
As the effects of estrogen on the cardiovascular system have been extensively studied and reviewed,11, 12, 13, 14 we allocated a small portion of our research to estrogen, highlighting recent developments. A larger part of this review focuses on androgens, particularly testosterone, to discuss the biological role of testosterone in vascular physiology and pathology in aging men.
Action of estrogen on the cardiovascular system
Effects of estrogen on cardiovascular risk factors
A number of studies have reported that estrogen therapy in postmenopausal women decreases the serum levels of both total and low-density lipoprotein cholesterol while raising high-density cholesterol and triglycerides, primarily by influencing the expression of hepatic apoprotein genes.11, 15 Also, estrogen inhibits the lipid peroxidation of low-density lipoprotein in vitro and in vivo.16, 17 Furthermore, estrogen can modulate glucose metabolism and prevent other risk factors for CVD, such as obesity (Table 1).18, 19
Direct vascular action of estrogen
Two estrogen receptor (ER) subtypes, ERα and ERβ, have been identified and are expressed in the vasculature, and experimental studies have demonstrated the vasodilator effects of estrogen/ER through their action on the endothelium, smooth muscle and extracellular matrix. Estrogen enhances endothelium-dependent vasorelaxation via increased release of nitric oxide (NO),20, 21, 22 endothelium-derived hyperpolarizing factor23 and PGI224, 25 and decreased production of endothelin-1 (Table 1).26 Several studies have demonstrated that estrogen inhibits calcium influx27, 28 and stimulates calcium efflux29 in vascular smooth muscle cells (VSMCs), leading to endothelium-independent vasodilation. Moreover, estrogen inhibits neointima formation in response to balloon injury30, 31 and perivascular cuff placement.32 Endothelial regeneration,33 inhibition of endothelial apoptosis34 and inhibition of VSMC migration and proliferation32 may account for the inhibitory effects of estrogen on neointima formation. Analyses of knockout mice for ERα and ERβ have provided more information regarding the molecular mechanism of estrogen’s action on the blood vessels.5 Recent progress in nuclear receptor research has also clarified the non-genomic action of estrogen on the vasculature,14 such as the direct interaction of ERα with the regulatory subunit of phosphatidylinositol-3-OH kinase.35
Role of the novel ER G protein coupled receptor 30 (GPR30) in the cardiovascular system
In addition to the two classical ER subtypes, ERα and ERβ, a third membrane-bound and G-protein-coupled ER, GPR30, has been identified in human vascular endothelial cells (ECs) and smooth muscle cells.36, 37, 38 Haas et al.37 reported that G-1, a selective stimulator of GPR30, acutely blocked vasoconstrictor-induced changes in intracellular calcium concentrations and vascular tone, resulting in lowering of blood pressure in normotensive rats. Similar vasodilator effects of GPR30 have been confirmed in other studies.39, 40, 41 It has also been reported that stimulation of GPR30 blocks VSMC proliferation.37, 42
The vasodilator action of G-1 may be mediated by NO-independent40 and NO-dependent37, 39, 40 pathways; the latter involves GPR30-induced endothelial NO synthase (eNOS) phosphorylation.43 Also, G-1 decreases nicotinamide adenine dinucleotide phosphate-stimulated superoxide production by the carotid and intracranial arteries, indicating the scavenging effects of GPR30 on superoxide anions.39 In the heart, G-1 reduces ischemia/reperfusion injury and preserves cardiac function through the phosphatidylinositol 3-kinase/Akt and extracellular signal-regulated kinase pathways and by eNOS phosphorylation.44, 45 Treatment with G-1 for 2 weeks reduced the expression of angiotensin II type 1 receptor and angiotensin-converting enzyme.40 The non-selective ER antagonist ICI 182780 and selective ER modulators, such as tamoxifen and raloxifene, have been shown to act as GPR30 ligands.46 Moreover, both GPR30 and ER are required for estrogen action in some situations, whereas GPR30 can act alone in the absence of ER,46, 47 suggesting a complex network between GPR30 and ER.
HRT and CVD
Observational studies have suggested that HRT decreases the risk of CVD in postmenopausal women.48, 49 However, large-scale, placebo-controlled, randomized trials, such as the HERS6 and the WHI,7 did not confirm the findings of the observational studies. In the WHI, HRT with conjugated equine estrogen plus medroxyprogesterone acetate increased the incidence of CVD instead, particularly in women older than 60 years of age, although women who started HRT soon after menopause tended to have a decreased risk for coronary heart disease.50
Additional data from other studies have supported the concept that the vasoprotective effects of estrogen are evident only when hormone therapy is initiated soon after the onset of menopause and before the development of atherosclerosis. In a meta-analysis of hormone therapy, CVD mortality was lower in younger women on hormone therapy (mean age of 55 years old) than in age-matched controls.51 Women aged 50–59 years who were enrolled in the conjugated equine estrogen trial of the WHI had significantly lower scores for coronary artery calcification 8.7 years after randomization than with placebo.52
Two ongoing clinical trials, the Kronos Early Estrogen Prevention Study53 and the Early Versus Late Intervention Trial with Estradiol Study (available at http://clinicaltrials.gov/ct2/show/NCT00114517; accessed 16 November 2011), were designed to examine the timing, dosage, route and limited duration of administration on patients’ cardiovascular outcomes and to prove the benefits of HRT in atherosclerosis when HRT is initiated soon after menopause. In the near future, these trials will provide additional insight into HRT and cardiovascular health in younger postmenopausal women.
Association of low testosterone levels with CVD
Plasma testosterone levels decrease with aging, and >20% of healthy men older than 60 years of age have testosterone levels below the standard range in young men aged 20–30 years.54, 55 Lower testosterone levels are associated with cognitive dysfunction, muscle weakness, anemia, osteoporosis, mood disturbances and impaired general and sexual health in aging men.56, 57 Recently, many studies have demonstrated the relationship of testosterone with CVD, indicating a consistent inverse relationship between endogenous testosterone and adverse cardiovascular events.
A case–control study among 117 Indian men aged 30–60 years with old myocardial infarction showed that testosterone concentrations were significantly lower in the patients with myocardial infarction than in the control subjects.58 Similar results were reported in men with acute myocardial infarction.59 Cross-sectional results from the Massachusetts Male Aging Study (1709 men aged 40–70 years) showed that serum total and free testosterone levels bear an inverse relationship with CVD, independent of cardiovascular risk factors.60 Recently, epidemiological studies have found that low testosterone levels are a predictor of all-cause and cardiovascular mortality in elderly men.61, 62 These findings were followed by studies investigating the incidence of CVD and testosterone levels.63, 64 According to these observations, endogenous testosterone appears to exert beneficial effects on the cardiovascular system.
Association of low testosterone with surrogate markers of atherosclerosis
The mechanisms underlying the epidemiological associations of low testosterone with CVD are complex and poorly understood. However, it is assumed that endogenous testosterone has physiological effects on the blood vessels and exerts atheroprotective effects. Actually, an increasing body of evidence has shown that low levels of endogenous androgens are associated with atherosclerosis progression in elderly men. Carotid artery intima-media thickness, a common marker of clinical and subclinical atherosclerosis, has been shown to be correlated inversely with testosterone levels.65, 66, 67 Demirbag et al.68 reported a similar finding by examining the intima thickness of the thoracic aorta in older men. Similarly, in the Rotterdam Study population, Hak et al.69 demonstrated that both bioavailable and total testosterone levels were negatively associated with calcified deposits in the abdominal aorta in men older than 55 years of age.
Arterial stiffness, measured as pulse wave velocity or augmentation index, is a predictor of cardiovascular events.70 Yaron et al.71 reported that age- and blood pressure-adjusted pulse wave velocity was significantly higher in hypogonadal men. Similarly, low testosterone levels in male hemodialysis patients were associated with increases in pulse wave velocity and CVD mortality.72 Clinical and preclinical evidence exists linking endothelial dysfunction to androgen deficiency. In 187 Japanese men aged 47±15 (s.d.) years, flow-mediated dilatation of the brachial artery, a reliable marker of endothelial function, was positively correlated with plasma testosterone levels, independent of other atherosclerosis risk factors.73 Comparable results were reported from Europe74 and specifically from Turkey.75
Clinical effects of androgen replacement therapy
As early as the 1940s, Lesser2 demonstrated that testosterone administration alleviates symptoms and ECG abnormalities in men with angina. Subsequent studies have shown that short-term testosterone administration in men with coronary artery disease results in coronary artery dilation and resistance to ischemia. Indeed, testosterone infusion into the coronary arteries induces vasodilation,76 and intravenous administration of testosterone reduces the exercise-induced ischemic response in men with stable angina.77, 78 Furthermore, acute administration of testosterone in men with chronic heart failure reduces peripheral vascular resistance and cardiac afterload, resulting in an increased cardiac index.79 Chronic administration of testosterone also improves functional capacity and symptoms in heart failure patients.80
Several reports have shown that testosterone administration improves arterial stiffness and endothelial vasomotor function in men. Testosterone replacement in hypogonadal men results in acute (48 h) and chronic (3 months) decreases in pulse wave velocity.71 It was also reported that testosterone replacement in men with coronary heart disease and low plasma testosterone decreased radial and aortic augmentation indices.81 Acute intravenous infusion82 and 8-week oral administration of testosterone83 improved flow-mediated vasodilation of the brachial artery.
Testosterone therapy in hypogonadal men with type 2 diabetes mellitus suppressed the production of inflammatory cytokines by circulating monocytes.84 A randomized, placebo-controlled, double-blind trial of 184 men with hypogonadism and metabolic syndrome showed that intramuscular administration of testosterone undecanoate decreased plasma levels of interleukin-1β, tumor necrosis factor-α and C-reactive protein in association with reductions in body mass index and waist circumference, while interleukin-6 and interleukin-10 did not change significantly.85
Taken together, testosterone administration, at least in hypogonadal men, may have a favorable vascular effect, including endothelium-dependent or -independent vasodilation and reduction of arterial stiffness and inflammatory markers. In contrast, the effects of testosterone replacement on the progression of carotid intima-media thickness or other atherosclerotic lesions, as well as on CVD risk,86 are unknown.
Direct effects of testosterone on vascular walls
Risk factors, such as metabolic syndrome, may partly explain the association of low testosterone with CVD. As the relationship between testosterone and metabolic syndrome has been extensively reviewed,87, 88 this section focuses on the direct effects of testosterone on the vascular wall and the underlying molecular mechanism.
As mentioned above, testosterone therapy can improve vascular function and several markers of atherosclerosis in men. Therefore, vascular ECs, VSMCs and macrophages may be targets of androgen’s actions. Indeed, androgen receptor (AR) has been shown to be expressed in these cells.89, 90, 91
Effects of testosterone on animal models of atherosclerosis and neointima formation
It has been demonstrated that the administration of testosterone in castrated male rabbits that were fed a high-cholesterol diet reduced aortic atherosclerosis, largely independent of plasma lipids.92, 93 In addition, neointima formation after coronary balloon injury in swine was increased by castration and was reversed by testosterone replacement.94 Regarding the role of AR, conflicting findings have been reported. Nathan et al.95 demonstrated the inhibitory effects of testosterone on fatty streak formation in castrated low-density lipoprotein receptor-deficient male mice, but the effects of testosterone were abrogated by treatment with an aromatase inhibitor, suggesting that estradiol converted from testosterone had a major role. Conversely, Qiu et al.91 showed that nonaromatizable dihydrotestosterone suppressed atherosclerosis formation in castrated male rabbits, indicating a role for AR. Exaggerated vascular remodeling in AR-deficient mice, in response to angiotensin II infusion, also suggests an important role for AR.96 A recent study by Bourghardt et al.97 may provide a hint in addressing this issue. They administered testosterone in AR-deficient mice with apolipoprotein E-deficient backgrounds and showed that testosterone reduced atherosclerotic lesions, both in AR-deficient and castrated wild-type male mice, but testosterone was less effective in AR-deficient mice, suggesting AR-dependent and -independent mechanisms.
Effects of testosterone on ECs
Several reports have implicated the effects of testosterone on endothelial regeneration. Cai et al.98 demonstrated that testosterone induced time- and dose-dependent proliferation of human aortic ECs via an AR-dependent pathway. In young hypogonadal men, low testosterone levels were associated with a small number of endothelial progenitor cells,99 and testosterone replacement was able to increase the number of progenitor cells.100 The synthesis and release of vasoactive substances by EC may have a role in these effects. Of the substances synthesized by EC, NO is a critical molecule that regulates vascular tone and atherosclerosis, and it is a major target of testosterone. It has been reported that testosterone-induced endothelium-dependent vasodilation is mediated in part by NO.101 We recently demonstrated that testosterone rapidly induces NO production via AR-mediated activation of eNOS in human aortic ECs.89 Furthermore, we showed that AR directly interacts with the p85 subunit of phosphatidylinositol 3-kinase, resulting in phosphorylation/activation of Akt/eNOS signaling. Taking together with our preliminary observation about the involvement of extracellular signal-regulated kinase 1/2 signaling and [Ca2+]i in AR-dependent eNOS activation, quite similar signaling pathways to those for estrogen can be proposed for testosterone (Figure 1), although some of these pathways should be verified in further studies. The genomic action of testosterone in ECs has not been studied extensively.
Signal transduction pathways of eNOS activation by estradiol and testosterone in vascular endothelial cells. AR, androgen receptor; E2, estradiol; eNOS, endothelial NO synthase; ERα, estrogen receptor α; ERK, extracellular signal-regulated kinase; NO, nitric oxide; PI3K, phosphatidylinositol 3-kinase; T, testosterone. Dotted curves indicate the plasma membrane. Dotted arrows indicate probable but undetermined pathways.
It has been reported that testosterone increases the number of ECs secreting endothelin-1,102 although its contribution to the modulation of vascular tone and of CVD is unknown. Testosterone at physiological concentrations seems to have a beneficial influence on the hemostatic system through tissue plasminogen activator expression and inhibition of plasminogen activator inhibitor type 1 secretion by human umbilical vein ECs.103
Effects of testosterone on VSMCs
Most of the rapid vasodilator effects of testosterone are endothelium independent and thus are attributable to its action on VSMCs. In particular, vasodilator responses to pharmacological concentrations of testosterone seem to be AR independent. Yue et al.104 reported that the relaxing response of rabbit coronary arteries to testosterone was significantly inhibited by the potassium-channel inhibitor barium chloride but not by the inhibition of NO synthesis or by removal of the endothelium. Several groups have shown that testosterone inhibits the agonist-induced rise of [Ca2+]i in VSMCs, as has been documented for estrogen. Crews and Khalil28 reported that testosterone at supra-physiological doses (10–100 pmol l–1) significantly suppresses the vasoconstriction of porcine coronary artery strips induced by prostaglandin F2α or by KCl, in parallel with the inhibition of Ca2+ entry. Hall et al.105 demonstrated, using the A7r5 VSMC cell line, that testosterone and dihydrotestosterone selectively suppressed Ca2+ entry via L-type Ca2+ channels. Similar results have been reported in different experimental conditions by other groups.106, 107, 108
The involvement of potassium channels in testosterone-induced vasodilatation has also been studied by many researchers.109, 110, 111 Cairrao et al.112 reported that an AR antagonist, flutamide, and an adenosine triphosphate-sensitive potassium-channel inhibitor, glibenclamide, had no influence on the testosterone relaxant effect, whereas a voltage-sensitive potassium-channel inhibitor, 4-aminopyridine, decreased this effect of testosterone. Opening of voltage-sensitive potassium channels induces hyperpolarization of the plasma membrane, which in turn may lead to the closing of L-type Ca2+ channels. These pharmacological studies, most of which used chemical inhibitors, may be strengthened by studies employing molecular-targeting strategies.
Accumulation of VSMCs in damaged vascular layers is a critical process in the development of atherosclerosis and is closely related to hypertension and its complications. Many, but not all, of the previous studies indicated that testosterone might inhibit VSMC growth. Hanke et al.113 reported, using an ex vivo organ culture system, that testosterone at 10–100 ng ml–1 significantly inhibited neointima formation in association with increased expression of AR in endothelium-denuded rabbit aortic rings after 21 days of incubation. Somjen et al.114 demonstrated the dose-dependent inhibitory effects of dihydrotestosterone and membrane-impermeable testosterone on DNA synthesis in cultured VSMCs derived from the human umbilical artery, suggesting a role for membrane AR. The above-mentioned study by Tharp et al.94 showed that the expressions of protein kinase C delta and p27 (kip1) were increased in coronary artery sections of testosterone-treated swine.
Androgen-responsive genes directly regulated by AR in VSMCs have not been determined, except for AR itself. However, we recently found that growth arrest-specific gene 6 was transactivated by testosterone in human VSMCs via binding of AR to the promoter region of the growth arrest-specific gene 6.90 In this study, testosterone inhibited inorganic phosphate-induced VSMC apoptosis, leading to the suppression of VSMC calcification. To further elucidate the mechanism underlying the effects of testosterone on the cardiovascular system, identification of androgen-responsive genes in VSMCs, as well as in ECs, is required in future studies.
Natoli et al.115 investigated, using human aortic VMSCs, and found that testosterone significantly reduced collagen and fibrillin-1 deposition, while it had no effect on elastin. They also found that testosterone increased the expression of matrix metalloproteinase-3, which has an important role in vascular remodeling.
Possible harmful effects of testosterone on blood vessels
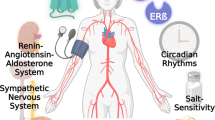
Although many studies have shown the beneficial effects of testosterone on the blood vessels, as mentioned above, other studies have suggested that long-term administration of testosterone may elicit harmful effects, especially vasoconstriction via upregulation of thromboxane A2,116 norepinephrine synthesis,117 angiotensin II118 and endothelin-1.102 It has been also reported that testosterone accelerates vascular remodeling119 and stimulates renal prohypertensive processes, including the renin–angiotensin–aldosterone system.120 Recent meta-analyses have revealed that CVD events were not different between testosterone and placebo groups,86, 121 indicating the complexity of testosterone therapy, as was shown for estrogen therapy in women.
Testosterone deficiency and CVD in women
An age-related reduction in circulating levels of androgens occurs in women as well.122 However, it is unclear whether this decline adversely affects vascular health in women. Higher serum testosterone concentrations, within the physiological range, have been associated with lower carotid intima-media thickness,123 suggesting potential protective effects of endogenous testosterone on cardiovascular health in pre- and postmenopausal women. Conversely, it is well known that women with polycystic ovary syndrome, who exhibit high androgen levels, are at a higher risk for CVD. Some studies have reported that high testosterone is associated with an adverse CVD risk factor profile in postmenopausal women, irrespective of polycystic ovary syndrome.3, 124 Polymorphism of the (CAG)n repeat of the AR gene was associated with CVD and risk factor profiles in postmenopausal women.125 Thus far, evidence is lacking for an association of testosterone with CVD events in women, and it is uncertain whether testosterone could be used as a postmenopausal hormone therapy.
Conclusion
In this review, we illustrated the sex hormones’ effects on the cardiovascular system, focusing on the action of testosterone on the blood vessels. Endogenous androgens, as well as estrogen, may display favorable effects on the vasculature, but whether HRT protects aging men and women from CVD is still unknown. Although testosterone administration seems to have diverse or contradictory effects in younger men and women, androgen therapy may provide hope for elderly hypogonadal men. This issue will remain unclear unless clinical trials of testosterone therapy are conducted. Also, progress in basic research on hormonal effects on blood vessels is essential to understanding the role of sex hormones in the development of CVD.
References
Sitigler LH, Tulgan J . Treatment of angina pectoris by testosterone propionate. NY State J Med 1943; 43: 1424–1428.
Lesser MA . Testosterone propionate therapy in one hundred cases of angina pectoris. J Clin Endocrinol Metab 1946; 6: 549–557.
Barrett-Connor E . Sex differences in coronary heart disease. Why are women so superior? The 1995 Ancel Keys Lecture. Circulation 1997; 95: 252–264.
Reckelhoff JF . Gender differences in the regulation of blood pressure. Hypertension 2001; 37: 1199–1208.
Mendelsohn ME, Karas RH . Molecular and cellular basis of cardiovascular gender differences. Science 2005; 308: 1583–1587.
Hulley S, Grady D, Bush T, Furberg C, Herrington D, Riggs B, Vittinghoff E . Randomized trial of estrogen plus progestin for secondary prevention of coronary heart disease in postmenopausal women. Heart and Estrogen/progestin Replacement Study (HERS) Research Group. JAMA 1998; 280: 605–613.
Rossouw JE, Anderson GL, Prentice RL, LaCroix AZ, Kooperberg C, Stefanick ML, Jackson RD, Beresford SA, Howard BV, Johnson KC, Kotchen JM, Ockene J . Risks and benefits of estrogen plus progestin in healthy postmenopausal women: principal results From the Women's Health Initiative randomized controlled trial. JAMA 2002; 288: 321–333.
Phillips GB, Pinkerbell BH, Jing TY . The association of hypotestosteronemia with coronary artery disease in men. Arterioscler Thromb 1994; 14: 701–706.
English KM, Mandour O, Steeds RP, Diver MJ, Jones TH, Channer KS . Men with coronary artery disease have lower levels of androgens than men with normal coronary angiograms. Eur Heart J 2000; 2: 890–894.
Rosano GM, Sheiban I, Massaro R, Pagnotta P, Marazzi G, Vitale C, Mercuro G, Volterrani M, Aversa A, Fini M . Low testosterone levels are associated with coronary artery disease in male patients with angina. Int J Impot Res 2007; 19: 176–182.
Mendelsohn ME, Karas RH . The protective effects of estrogen on the cardiovascular system. N Engl J Med 1999; 340: 1801–1811.
Klouche M . Estrogens in human vascular diseases. Ann NY Acad Sci 2006; 1089: 431–443.
Yang XP, Reckelhoff JF . Estrogen, hormonal replacement therapy and cardiovascular disease. Curr Opin Nephrol Hypertens 2011; 20: 133–138.
Mendelsohn ME, Karas RH . Rapid progress for non-nuclear estrogen receptor signaling. J Clin Invest 2010; 120: 2277–2279.
Yamakawa-Kobayashi K, Somekawa Y, Fujimura M, Tomura S, Arinami T, Hamaguchi H . Relation of the -514C/T polymorphism in the hepatic lipase gene to serum HDL and LDL cholesterol levels in postmenopausal women under hormone replacement therapy. Atherosclerosis 2002; 162: 17–21.
Kuohung W, Shwaery GT, Keaney Jr JF . Tamoxifen, esterified estradiol, and physiologic concentrations of estradiol inhibit oxidation of low-density lipoprotein by endothelial cells. Am J Obstet Gynecol 2001; 184: 1060–1063.
Santanam N, Shern-Brewer R, McClatchey R, Castellano PZ, Murphy AA, Voelkel S, Parthasarathy S . Estradiol as an antioxidant: incompatible with its physiological concentrations and function. J Lipid Res 1998; 39: 2111–2118.
Liang YQ, Akishita M, Kim S, Ako J, Hashimoto M, Iijima K, Ohike Y, Watanabe T, Sudoh N, Toba K, Yoshizumi M, Ouchi Y . Estrogen receptor beta is involved in the anorectic action of estrogen. Int J Obes Relat Metab Disord 2002; 26: 1103–1109.
Lijnen HR . Murine models of obesity and hormonal therapy. Thromb Res 2011; 127 (Suppl 3): S17–S20.
Kauser K, Rubanyi GM . Potential cellular signaling mechanisms mediating upregulation of endothelial nitric oxide production by estrogen. J Vasc Res 1997; 34: 229–236.
Hashimoto M, Akishita M, Eto M, Ishikawa M, Kozaki K, Toba K, Sagara Y, Taketani Y, Orimo H, Ouchi Y . Modulation of endothelium-dependent flow-mediated dilatation of the brachial artery by sex and menstrual cycle. Circulation 1995; 92: 3431–3435.
Geary GG, Krause DN, Duckles SP . Estrogen reduces mouse cerebral artery tone through endothelial NOS- and cyclooxygenase-dependent mechanisms. Am J Physiol Heart Circ Physiol 2000; 279: H511–H519.
Liu MY, Hattori Y, Fukao M, Sato A, Sakuma I, Kanno M . Alterations in EDHF-mediated hyperpolarization and relaxation in mesenteric arteries of female rats in long-term deficiency of oestrogen and during oestrus cycle. Br J Pharmacol 2001; 132: 1035–1046.
Jun SS, Chen Z, Pace MC, Shaul PW . Estrogen upregulates cyclooxygenase-1 gene expression in ovine fetal pulmonary artery endothelium. J Clin Invest 1998; 102: 176–183.
Sherman TS, Chambliss KL, Gibson LL, Pace MC, Mendelsohn ME, Pfister SL, Shaul PW . Estrogen acutely activates prostacyclin synthesis in ovine fetal pulmonary artery endothelium. Am J Respir Cell Mol Biol 2002; 26: 610–616.
Akishita M, Kozaki K, Eto M, Yoshizumi M, Ishikawa M, Toba K, Orimo H, Ouchi Y . Estrogen attenuates endothelin-1 production by bovine endothelial cells via estrogen receptor. Biochem Biophys Res Commun 1998; 251: 17–21.
Han SZ, Karaki H, Ouchi Y, Akishita M, Orimo H . 17 Beta-estradiol inhibits Ca2+ influx and Ca2+ release induced by thromboxane A2 in porcine coronary artery. Circulation 1995; 91: 2619–2626.
Crews JK, Khalil RA . Antagonistic effects of 17 beta-estradiol, progesterone, and testosterone on Ca2+ entry mechanisms of coronary vasoconstriction. Arterioscler Thromb Vasc Biol 1999; 19: 1034–1040.
Prakash YS, Togaibayeva AA, Kannan MS, Miller VM, Fitzpatrick LA, Sieck GC . Estrogen increases Ca2+ efflux from female porcine coronary arterial smooth muscle. Am J Physiol 1999; 276: H926–H934.
Chen SJ, Li H, Durand J, Oparil S, Chen YF . Estrogen reduces myointimal proliferation after balloon injury of rat carotid artery. Circulation 1996; 93: 577–584.
Krom YD, Pires NM, Jukema JW, de Vries MR, Frants RR, Havekes LM, van Dijk KW, Quax PH . Inhibition of neointima formation by local delivery of estrogen receptor alpha and beta specific agonists. Cardiovasc Res 2007; 73: 217–226.
Akishita M, Ouchi Y, Miyoshi H, Kozaki K, Inoue S, Ishikawa M, Eto M, Toba K, Orimo H . Estrogen inhibits cuff-induced intimal thickening of rat femoral artery: effects on migration and proliferation of vascular smooth muscle cells. Atherosclerosis 1997; 130: 1–10.
Krasinski K, Spyridopoulos I, Asahara T, van der Zee R, Isner JM, Losordo DW . Estradiol accelerates functional endothelial recovery after arterial injury. Circulation 1997; 95: 1768–1772.
Sudoh N, Toba K, Akishita M, Ako J, Hashimoto M, Iijima K, Kim S, Liang YQ, Ohike Y, Watanabe T, Yamazaki I, Yoshizumi M, Eto M, Ouchi Y . Estrogen prevents oxidative stress-induced endothelial cell apoptosis in rats. Circulation 2001; 103: 724–729.
Simoncini T, Hafezi-Moghadam A, Brazil DP, Ley K, Chin WW, Liao JK . Interaction of oestrogen receptor with the regulatory subunit of phosphatidylinositol-3-OH kinase. Nature 2000; 407: 538–541.
Haas E, Meyer MR, Schurr U, Bhattacharya I, Minotti R, Nguyen HH, Heigl A, Lachat M, Genoni M, Barton M . Differential effects of 17beta-estradiol on function and expression of estrogen receptor alpha, estrogen receptor beta, and GPR30 in arteries and veins of patients with atherosclerosis. Hypertension 2007; 49: 1358–1363.
Haas E, Bhattacharya I, Brailoiu E, Damjanović M, Brailoiu GC, Gao X, Mueller-Guerre L, Marjon NA, Gut A, Minotti R, Meyer MR, Amann K, Ammann E, Perez-Dominguez A, Genoni M, Clegg DJ, Dun NJ, Resta TC, Prossnitz ER, Barton M . Regulatory role of G protein-coupled estrogen receptor for vascular function and obesity. Circ Res 2009; 104: 288–291.
Meyer MR, Prossnitz ER, Barton M . The G protein-coupled estrogen receptor GPER/GPR30 as a regulator of cardiovascular function. Vascul Pharmacol 2011; 55: 17–25.
Broughton BR, Miller AA, Sobey CG . Endothelium-dependent relaxation by G protein-coupled receptor 30 agonists in rat carotid arteries. Am J Physiol Heart Circ Physiol 2010; 298: H1055–H1061.
Lindsey SH, Carver KA, Prossnitz ER, Chappell MC . Vasodilation in response to the GPR30 agonist G-1 is not different from estradiol in the mRen2. Lewis female rat. J Cardiovasc Pharmacol 2011; 57: 598–603.
Meyer MR, Baretella O, Prossnitz ER, Barton M . Dilation of epicardial coronary arteries by the G protein-coupled estrogen receptor agonists G-1 and ICI 182,780. Pharmacology 2010; 86: 58–64.
Takahashi K, Ohmichi M, Yoshida M, Hisamoto K, Mabuchi S, Arimoto-Ishida E, Mori A, Tsutsumi S, Tasaka K, Murata Y, Kurachi H . Both estrogen and raloxifene cause G1 arrest of vascular smooth muscle cells. J Endocrinol 2003; 178: 319–329.
Rowlands DJ, Chapple S, Siow RC, Mann GE . Equol-stimulated mitochondrial reactive oxygen species activate endothelial nitric oxide synthase and redox signaling in endothelial cells: roles for F-actin and GPR30. Hypertension 2011; 57: 833–840.
Deschamps AM, Murphy E, Sun J . Estrogen receptor activation and cardioprotection in ischemia reperfusion injury. Trends Cardiovasc Med 2010; 20: 73–78.
Filice E, Recchia AG, Pellegrino D, Angelone T, Maggiolini M, Cerra MC . A new membrane G protein-coupled receptor (GPR30) is involved in the cardiac effects of 17beta-estradiol in the male rat. J Physiol Pharmacol 2009; 60: 3–10.
Prossnitz ER, Maggiolini M . Mechanisms of estrogen signaling and gene expression via GPR30. Mol Cell Endocrinol 2009; 308: 32–38.
Prossnitz ER, Barton M . The G-protein-coupled estrogen receptor GPER in health and disease. Nat Rev Endocrinol 2011; 7: 715–726.
Grodstein F, Stampfer MJ, Colditz GA, Willett WC, Manson JE, Joffe M, Rosner B, Fuchs C, Hankinson SE, Hunter DJ, Hennekens CH, Speizer FE . Postmenopausal hormone therapy and mortality. N Engl J Med 1997; 336: 1769–1775.
Grodstein F, Manson JE, Colditz GA, Willett WC, Speizer FE, Stampfer MJ . A prospective, observational study of postmenopausal hormone therapy and primary prevention of cardiovascular disease. Ann Intern Med 2000; 133: 933–941.
Rossouw JE, Prentice RL, Manson JE, Wu L, Barad D, Barnabei VM, Ko M, LaCroix AZ, Margolis KL, Stefanick ML . Postmenopausal hormone therapy and risk of cardiovascular disease by age and years since menopause. JAMA 2007; 297: 1465–1477.
Salpeter SR, Cheng J, Thabane L, Buckley NS, Salpeter EE . Bayesian meta-analysis of hormone therapy and mortality in younger postmenopausal women. Am J Med 2009; 122: 1016–1022.
Manson JE, Allison MA, Rossouw JE, Carr JJ, Langer RD, Hsia J, Kuller LH, Cochrane BB, Hunt JR, Ludlam SE, Pettinger MB, Gass M, Margolis KL, Nathan L, Ockene JK, Prentice RL, Robbins J, Stefanick ML . Estrogen therapy and coronary-artery calcification. N Engl J Med 2007; 356: 2591–2602.
Miller VM, Black DM, Brinton EA, Budoff MJ, Cedars MI, Hodis HN, Lobo RA, Manson JE, Merriam GR, Naftolin F, Santoro N, Taylor HS, Harman SM . Using basic science to design a clinical trial: baseline characteristics of women enrolled in the Kronos Early Estrogen Prevention Study (KEEPS). J Cardiovasc Transl Res 2009; 2: 228–239.
Harman SM, Metter EJ, Tobin JD, Pearson J, Blackman MR . Longitudinal effects of aging on serum total and free testosterone levels in healthy men: Baltimore Longitudinal Study of Aging. J Clin Endocrinol Metab 2001; 86: 724–731.
Feldman HA, Longcope C, Derby CA, Johannes CB, Araujo AB, Coviello AD, Bremner WJ, McKinlay JB . Age trends in the level of serum testosterone and other hormones in middle-aged men: longitudinal results from the Massachusetts Male Aging Study. J Clin Endocrinol Metab 2002; 87: 589–598.
Lamberts SW, van den Beld AW, van der Lely AJ . The endocrinology of aging. Science 1997; 278: 419–424.
Kaufman JM, Vermeulen A . The decline of androgen levels in elderly men and its clinical and therapeutic implications. Endocr Rev 2005; 26: 833–876.
Sewdarsen M, Vythilingum S, Jialal I, Desai RK, Becker P . Abnormalities in sex hormones are a risk factor for premature manifestation of coronary artery disease in South African Indian men. Atherosclerosis 1990; 83: 111–117.
Mohamad MJ, Mohammad MA, Karayyem M, Hairi A, Hader AA . Serum levels of sex hormones in men with acute myocardial infarction. Neuro Endocrinol Lett 2007; 28: 182–186.
Feldman HA, Johannes CB, McKinlay JB, Longcope C . Low dehydroepiandrosterone sulfate and heart disease in middle-aged men: cross-sectional results from the Massachusetts Male Aging Study. Ann Epidemiol 1998; 8: 217–228.
Khaw KT, Dowsett M, Folkerd E, Bingham S, Wareham N, Luben R, Welch A, Day N . Endogenous testosterone and mortality due to all causes, cardiovascular disease, and cancer in men: European prospective investigation into cancer in Norfolk (EPIC-Norfolk) Prospective Population Study. Circulation 2007; 116: 2694–2701.
Laughlin GA, Barrett-Connor E, Bergstrom J . Low serum testosterone and mortality in older men. J Clin Endocrinol Metab 2008; 93: 68–75.
Vikan T, Schirmer H, Njølstad I, Svartberg J . Endogenous sex hormones and the prospective association with cardiovascular disease and mortality in men: the Tromsø Study. Eur J Endocrinol 2009; 161: 435–442.
Akishita M, Hashimoto M, Ohike Y, Ogawa S, Iijima K, Eto M, Ouchi Y . Low testosterone level as a predictor of cardiovascular events in Japanese men with coronary risk factors. Atherosclerosis 2010; 210: 232–236.
Muller M, van de Beld AW, Bots ML, Grobbee DE, Lamberts SWJ, van der Schouw YT . Endogenous sex hormones and progression of carotid atherosclerosis in elderly men. Circulation 2004; 109: 2074–2079.
Van de Beld AW, Bots ML, Janssen JAMLL, Pols HAP, Lamberts SWJ, Grobbee DE . Endogenous hormones and carotid atherosclerosis in elderly men. Am J Epidemiol 2003; 157: 25–31.
Makinen J, Jarvisalo MJ, Pollanen P, Perheentupa A, Irjala K, Koskenvuo M, Makinen J, Huhtaniemi I, Raitakari OT . Increased carotid atherosclerosis in andropausal middle-aged men. J Am Coll Cardiol 2005; 45: 1603–1608.
Demirbag R, Yilmaz R, Ulucay A, Unlu D . The inverse relationship between thoracic aortic intima media thickness and testosterone level. Endocr Res 2005; 31: 335–344.
Hak AE, Witteman JC, de Jong FH, Geerlings MI, Hofman A, Pols HA . Low levels of endogenous androgens increase the risk of atherosclerosis in elderly men: the Rotterdam study. J Clin Endocrinol Metab 2002; 87: 3632–3639.
Vlachopoulos C, Aznaouridis K, Stefanadis C . Prediction of cardiovascular events and all-cause mortality with arterial stiffness: a systematic review and meta-analysis. J Am Coll Cardiol 2010; 55: 1318–1327.
Yaron M, Greenman Y, Rosenfeld JB, Izkhakov E, Limor R, Osher E, Shenkerman G, Tordjman K, Stern N . Effect of testosterone replacement therapy on arterial stiffness in older hypogonadal men. Eur J Endocrinol 2009; 160: 839–846.
Kyriazis J, Tzanakis I, Stylianou K, Katsipi I, Moisiadis D, Papadaki A, Mavroeidi V, Kagia S, Karkavitsas N, Daphnis E . Low serum testosterone, arterial stiffness and mortality in male haemodialysis patients. Nephrol Dial Transplant 2011; 26: 2971–2977.
Akishita M, Hashimoto M, Ohike Y, Ogawa S, Iijima K, Eto M, Ouchi Y . Low testosterone level is an independent determinant of endothelial dysfunction in men. Hypertens Res 2007; 30: 1029–1034.
Mäkinen JI, Perheentupa A, Irjala K, Pöllänen P, Mäkinen J, Huhtaniemi I, Raitakari OT . Endogenous testosterone and brachial artery endothelial function in middle-aged men with symptoms of late-onset hypogonadism. Aging Male 2011; 14: 237–242.
Yilmaz MI, Sonmez A, Qureshi AR, Saglam M, Stenvinkel P, Yaman H, Eyileten T, Caglar K, Oguz Y, Taslipinar A, Vural A, Gok M, Unal HU, Yenicesu M, Carrero JJ . Endogenous testosterone, endothelial dysfunction, and cardiovascular events in men with nondialysis chronic kidney disease. Clin J Am Soc Nephrol 2011; 6: 1617–1625.
Webb CM, McNeill JG, Hayward CS, de Zeigler D, Collins P . Effects of testosterone on coronary vasomotor regulation in men with coronary heart disease. Circulation 1999; 100: 1690–1696.
Rosano GM, Leonardo F, Pagnotta P, Pelliccia F, Panina G, Cerquetani E, della Monica PL, Bonfigli B, Volpe M, Chierchia SL . Acute anti-ischemic effect of testosterone in men with coronary artery disease. Circulation 1999; 99: 1666–1670.
Webb CM, Adamson DL, de Zeigler D, Collins P . Effect of acute testosterone on myocardial ischemia in men with coronary artery disease. Am J Cardiol 1999; 83: 437–439.
Pugh PJ, Jones TH, Channer KS . Acute haemodynamic effects of testosterone in men with chronic heart failure. Eur Heart J 2003; 24: 909–915.
Malkin CJ, Pugh PJ, West JN, van Beek EJ, Jones TH, Channer KS . Testosterone therapy in men with moderate severity heart failure: a double-blind randomized placebo controlled trial. Eur Heart J 2006; 27: 57–64.
Webb CM, Elkington AG, Kraidly MM, Keenan N, Pennell DJ, Collins P . Effects of oral testosterone treatment on myocardial perfusion and vascular function in men with low plasma testosterone and coronary heart disease. Am J Cardiol 2008; 101: 618–624.
Ong PJ, Patrizi G, Chong WC, Webb CM, Hayward CS, Collins P . Testosterone enhances flow-mediated brachial artery reactivity in men with coronary artery disease. Am J Cardiol 2000; 85: 269–272.
Kang SM, Jang Y, Kim JY, Chung N, Cho SY, Chae JS, Lee JH . Effect of oral administration of testosterone on brachial arterial vasoreactivity in men with coronary artery disease. Am J Cardiol 2002; 89: 862–864.
Corrales JJ, Almeida M, Burgo R, Mories MT, Miralles JM, Orfao A . Androgen-replacement therapy depresses the ex vivo production of inflammatory cytokines by circulating antigen-presenting cells in aging type-2 diabetic men with partial androgen deficiency. J Endocrinol 2006; 189: 595–604.
Kalinchenko SY, Tishova YA, Mskhalaya GJ, Gooren LJ, Giltay EJ, Saad F . Effects of testosterone supplementation on markers of the metabolic syndrome and inflammation in hypogonadal men with the metabolic syndrome: the double-blinded placebo-controlled Moscow study. Clin Endocrinol (Oxf) 2010; 73: 602–612.
Haddad RM, Kennedy CC, Caples SM, Tracz MJ, Boloña ER, Sideras K, Uraga MV, Erwin PJ, Montori VM . Testosterone and cardiovascular risk in men: a systematic review and meta-analysis of randomized placebo-controlled trials. Mayo Clin Proc 2007; 82: 29–39.
Traish AM, Miner MM, Morgentaler A, Zitzmann M . Testosterone deficiency. Am J Med 2011; 124: 578–587.
Corona G, Rastrelli G, Vignozzi L, Mannucci E, Maggi M . Testosterone, cardiovascular disease and the metabolic syndrome. Best Pract Res Clin Endocrinol Metab 2011; 25: 337–353.
Yu J, Akishita M, Eto M, Ogawa S, Son BK, Kato S, Ouchi Y, Okabe T . Androgen receptor-dependent activation of endothelial nitric oxide synthase in vascular endothelial cells: role of phosphatidylinositol 3-kinase/AKT pathway. Endocrinology 2010; 151: 1822–1828.
Son BK, Akishita M, Iijima K, Ogawa S, Maemura K, Yu J, Takeyama K, Kato S, Eto M, Ouchi Y . Androgen receptor-dependent transactivation of growth arrest-specific gene 6 mediates inhibitory effects of testosterone on vascular calcification. J Biol Chem 2010; 285: 7537–7544.
Qiu Y, Yanase T, Hu H, Tanaka T, Nishi Y, Liu M, Sueishi K, Sawamura T, Nawata H . Dihydrotestosterone suppresses foam cell formation and attenuates atherosclerosis development. Endocrinology 2010; 151: 3307–3316.
Bruck B, Brehme U, Gugel N, Hanke S, Finking G, Lutz C, Benda N, Schmahl FW, Haasis R, Hanke H . Gender-specific differences in the effects of testosterone and estrogen on the development of atherosclerosis in rabbits. Arterioscler Thromb Vasc Biol 1997; 17: 2192–2199.
Alexandersen P, Haarbo J, Byrjalsen I, Lawaetz H, Christiansen C . Natural androgens inhibit male atherosclerosis: a study in castrated, cholesterol-fed rabbits. Circ Res 1999; 84: 813–819.
Tharp DL, Masseau I, Ivey J, Ganjam VK, Bowles DK . Endogenous testosterone attenuates neointima formation after moderate coronary balloon injury in male swine. Cardiovasc Res 2009; 82: 152–160.
Nathan L, Shi W, Dinh H, Mukherjee TK, Wang X, Lusis AJ, Chaudhuri G . Testosterone inhibits early atherogenesis by conversion to estradiol: critical role of aromatase. Proc Natl Acad Sci 2001; 98: 3589–3593.
Ikeda Y, Aihara K, Yoshida S, Sato T, Yagi S, Iwase T, Sumitomo Y, Ise T, Ishikawa K, Azuma H, Akaike M, Kato S, Matsumoto T . Androgen-androgen receptor system protects against angiotensin II-induced vascular remodeling. Endocrinology 2009; 150: 2857–2864.
Bourghardt J, Wilhelmson AS, Alexanderson C, De Gendt K, Verhoeven G, Krettek A, Ohlsson C, Tivesten A . Androgen receptor-dependent and independent atheroprotection by testosterone in male mice. Endocrinology 2010; 151: 5428–5437.
Cai J, Hong Y, Weng C, Tan C, Imperato-McGinley J, Zhu YS . Androgen stimulates endothelial cell proliferation via an androgen receptor/VEGF/cyclin A-mediated mechanism. Am J Physiol Heart Circ Physiol 2011; 300: H1210–H1221.
Foresta C, Caretta N, Lana A, De Toni L, Biagioli A, Ferlin A, Garolla A . Reduced number of circulating endothelial progenitor cells in hypogonadal men. J Clin Endocrinol Metab 2006; 91: 4599–4602.
Foresta C, Zuccarello D, De Toni L, Garolla A, Caretta N, Ferlin A . Androgens stimulate endothelial progenitor cells through an androgen-mediated pathway. Clin Endo 2008; 68: 284–289.
Costarella CE, Stallone JN, Rutecki GW, Whittier FC . Testosterone causes direct relaxation of rat thoracic aorta. J Pharmacol Exp Ther 1996; 277: 34–39.
Pearson LJ, Yandle TG, Nicholls MG, Evans JJ . Regulation of endothelin-1 release from human endothelial cells by sex steroids and angiotensin-II. Peptides 2008; 9: 1057–1061.
Jin H, Lin J, Fu L, Mei YF, Peng G, Tan X, Wang DM, Wang W, Li YG . Physiological testosterone stimulates tissue plasminogen activator and tissue factor pathway inhibitor and inhibits plasminogen activator inhibitor type 1 release in endothelial cells. Biochem Cell Biol 2007; 85: 246–251.
Yue P, Chatterjee K, Beale C, Poole-Wilson PA, Collins P . Testosterone relaxes rabbit coronary arteries and aorta. Circulation 1995; 91: 1154–1160.
Hall J, Jones RD, Jones TH, Channer KS, Peers C . Selective inhibition of L-type Ca2+ channels in A7r5 cells by physiological levels of testosterone. Endocrinology 2006; 147: 2675–2680.
Jones RD, English KM, Jones TH, Channer KS . Testosterone-induced coronary vasodilatation occurs via a non-genomic mechanism: evidence of a direct calcium antagonism action. Clin Sci (Lond) 2004; 107: 149–158.
Alvarez E, Cairrão E, Morgado M, Morais C, Verde I . Testosterone and cholesterol vasodilation of rat aorta involves L-type calcium channel inhibition. Adv Pharmacol Sci 2010; 2010: 534184.
Scragg JL, Jones RD, Channer KS, Jones TH, Peers C . Testosterone is a potent inhibitor of L-type Ca(2+) channels. Biochem Biophys Res Commun 2004; 318: 503–506.
Honda H, Unemoto T, Kogo H . Different mechanisms for testosterone-induced relaxation of aorta between normotensive and spontaneously hypertensive rats. Hypertension 1999; 34: 1232–1236.
Tep-areenan P, Kendall DA, Randall MD . Testosterone-induced vasorelaxation in the rat mesenteric arterial bed is mediated predominantly via potassium channels. Br J Pharmacol 2002; 135: 735–740.
Yildiz O, Seyrek M, Gul H, Un I, Yildirim V, Ozal E, Uzun M, Bolu E . Testosterone relaxes human internal mammary artery in vitro. J Cardiovasc Pharmacol 2005; 45: 580–585.
Cairrão E, Alvarez E, Santos-Silva AJ, Verde I . Potassium channels are involved in testosterone-induced vasorelaxation of human umbilical artery. Naunyn Schmiedebergs Arch Pharmacol 2008; 376: 375–383.
Hanke H, Lenz C, Hess B, Spindler KD, Weidemann W . Effect of testosterone on plaque development and androgen receptor expression in the arterial vessel wall. Circulation 2001; 103: 1382–1385.
Somjen D, Kohen F, Gayer B, Kulik T, Knoll E, Stern N . Role of putative membrane receptors in the effect of androgens on human vascular cell growth. J Endocrinol 2004; 180: 97–106.
Natoli AK, Medley TL, Ahimastos AA, Drew BG, Thearle DJ, Dilley RJ, Kingwell BA . Sex steroids modulate human aortic smooth muscle cell matrix protein deposition and matrix metalloproteinase expression. Hypertension 2005; 46: 1129–1134.
Masuda A, Mathur R, Halushka PV . Testosterone increases thromboxane A2 receptors in cultured rat aortic smooth muscle cells. Circ Res 1991; 69: 638–643.
Kumai T, Tanaka M, Watanabe M, Nakura H, Kobayashi S . Influence of androgen on tyrosine hydroxylase mRNA in adrenal medulla of spontaneously hypertensive rats. Hypertension 1995; 26: 208–212.
Reckelhoff JF, Zhang H, Granger JP . Testosterone exacerbates hypertension and reduces pressure-natriuresis in male spontaneously hypertensive rats. Hypertension 1998; 31: 435–439.
Kienitz T, Quinkler M . Testosterone and blood pressure regulation. Kidney Blood Press Res 2008; 31: 71–79.
Yanes LL, Sartori-Valinotti JC, Iliescu R, Romero DG, Racusen LC, Zhang H, Reckelhoff JF . Testosterone-dependent hypertension and upregulation of intrarenal angiotensinogen in Dahl salt-sensitive rats. Am J Physiol Renal Physiol 2009; 296: F771–F779.
Fernández-Balsells MM, Murad MH, Lane M, Lampropulos JF, Albuquerque F, Mullan RJ, Agrwal N, Elamin MB, Gallegos-Orozco JF, Wang AT, Erwin PJ, Bhasin S, Montori VM . Clinical review 1: adverse effects of testosterone therapy in adult men: a systematic review and meta-analysis. J Clin Endocrinol Metab 2010; 95: 2560–2575.
Longcope C, Franz C, Morello C, Baker R, Johnston Jr CC . Steroid and gonadotropin levels in women during the peri-menopausal years. Maturitas 1986; 8: 189–196.
Bernini GP, Sgró M, Moretti A, Argenio GF, Barlascini CO, Cristofani R, Salvetti A . Endogenous androgens and carotid intimal-medial thickness in women. J Clin Endocrinol Metab 1999; 84: 2008–2012.
Brand JS, van der Schouw YT . Testosterone, SHBG and cardiovascular health in postmenopausal women. Int J Impot Res 2010; 22: 91–104.
Saltiki K, Cimponeriu A, Garofalaki M, Sarika L, Papathoma A, Stamatelopoulos K, Alevizaki M . Severity of coronary artery disease in postmenopausal women: association with the androgen receptor gene (CAG)n repeat polymorphism. Menopause 2011; 18: 1225–1231.
Acknowledgements
This work was supported by grants received from Grants-in-Aid for Scientific Research from the Ministry of Education, Science, Culture and Sports of Japan (21390220, 20249041).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Akishita, M., Yu, J. Hormonal effects on blood vessels. Hypertens Res 35, 363–369 (2012). https://doi.org/10.1038/hr.2012.4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2012.4