Abstract
The renin–angiotensin system (RAS) is involved in the pathological mechanisms of target organ damage, as well as in the induction of hypertension. RAS inhibition by angiotensin converting enzyme (ACE) inhibitors and angiotensin (Ang) II receptor blockers can prevent tissue damage by inhibition of Ang II type 1 receptor signaling. A beneficial effect of RAS inhibition on the heart, vasculature and kidney in cardiovascular disease has been reported. However, RAS inhibition can also prevent fibroproliferative diseases and damage of other tissues, such as brain, adipose tissue and muscle, because local RAS has an important role in tissue damage compared with circulating RAS. Moreover, other players, such as Ang II type 2 receptor signaling, aldosterone and ACE2 have been highlighted. Furthermore, there has also been a focus on the emerging concept of regulation of RAS, such as receptor-interacting proteins and receptor modifications, in the new discovery of therapeutic agents for tissue protection. The RAS has a pivotal role in various target organ damage, with complicated mechanisms; therefore, blockade of RAS may be therapeutically effective in preventing organ damage, as well as in having an antihypertensive effect.
Similar content being viewed by others
Introduction
Hypertension is one of the most common chronic diseases, being observed in one-fourth of the world’s population,1 and contributes substantially to the burden of cardiovascular (CV) disease and end organ damage. Although blood pressure lowering with antihypertensive agents prevents CV events, such as stroke, myocardial infarction, heart failure and kidney disease,2 accumulating evidence from large clinical trials suggests that blockade of the renin–angiotensin system (RAS) is more effective in the prevention of CV and target organ damage compared with other hypertensive agents. Many tissues are considered to be capable of local angiotensin (Ang) II productionthrough the tissue-specific local RAS. In pathological conditions, the local RAS is activated in various tissues, such as endothelium, vascular smooth muscle and renal mesangium, leading to organ damage. RAS is involved in all stages of the CV continuum,3 because the major effector of RAS, Ang II, has a direct pathobiological effect on the heart, brain, vessel wall, kidney and adipose tissue. Moreover, new evidence has recently accumulated showing the existence of several novel receptor-interacting proteins and various Ang II receptor activation mechanisms beyond the classical actions of receptors for Ang II. Ang II exerts its important physiological functions through two distinct receptor subtypes: type 1 (AT1) and type 2 (AT2) receptors. These associated proteins could contribute not only to Ang II receptors’ functions but also to influencing pathophysiological states. Moreover, other players in RAS have been highlighted in recent CV research. In this review, the major basic mechanisms of target organ damage induced by RAS in each organ and the effect of blockade of RAS, such as with angiotensin converting enzyme (ACE) inhibitors (ACEIs) and Ang II receptor blockers (ARBs), on target organ damage are discussed, together with the recent paradigm of RAS.
New paradigm shift of renin–angiotensin system
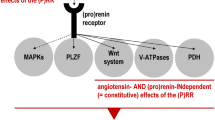
Ang II is the principal vasoactive substance of RAS, having a variety of physiological actions including vasoconstriction, aldosterone release and cell growth.4 Ang II binds two major receptors: the AT1 receptor and the AT2 receptor. The majority of well-known Ang II actions are mediated through AT1 receptor stimulation, and RAS inhibition by ACEIs and ARBs is expected to protect against CV disease. AT2 receptor stimulation by unbound Ang II could also be expected during treatment with ARBs. Recent accumulating evidence has suggested that the AT2 receptor not only opposes the AT1 receptor but also has unique effects beyond an interaction with AT1 receptor signaling. On the other hand, recent experimental studies have shown the existence of proteins interacting with Ang II receptors, screened by the yeast-based two-hybrid protein–protein interaction assay technique, and have also revealed their functions.5, 6, 7, 8, 9, 10, 11, 12 For the AT1 receptor, AT1 receptor-associated protein could act as a negative regulator in AT1 receptor-mediated cell proliferation and vascular remodeling, at least in part by the enhancement of AT1 receptor internalization.13, 14 On the other hand, the AT2 receptor-interacting protein seems to act as a novel early component of the growth inhibitory signaling cascade of the AT2 receptor.12 Moreover, the AT1 receptor is also reported to form homodimers or heterodimers, and undergo complex formation with the AT2 receptor15 and other GPCRs, such as the bradykinin B2 receptor in patients with preeclampsia,16 the EGF receptor,17 dopamine receptors,18, 19, 20, 21 AT1-endothelin receptor type B22 and AT1-Mas receptor.23 These dimerizations of Ang II receptors could possibly indicate unknown effects of Ang II receptors’ functional aspects in CV biology.
The ligand-independent activation of GPCRs has been highlighted, especially in the potential new discovery of drug targets.24 Mechanical stress activates the AT1 receptor independently of Ang II.25 This activation can be inhibited by an inverse agonist of the AT1 receptor; therefore, ARBs can be classified into competitive antagonists and inverse agonists.26 Moreover, agonistic antibodies against the second extracellular AT1 receptor loop have been shown in women with preeclampsia27 and in renal transplant recipients during an episode of rejection.28, 29
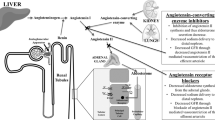
Moreover, another recent topic is new players in RAS (Figure 1). The counter-regulatory axis of the RAS, such as ACE2, Ang-(1–7) and its receptor, Mas, is potentially important for promoting vasoprotective effects. The balance between the ACE–Ang II–AT1 receptor and the ACE2–Ang-(1–-7)–Mas axis is considered to play an important role in organ damage, related directly to hypertension and associated diseases; therefore, the regulation of ACE2 offers a novel target for CVD therapeutics.30 On the other hand, brain Ang III, which is converted in vivo from Ang II by aminopeptidase A, controls vasopressin release and increases blood pressure. Although the true effector of Ang III is totally unknown, Ang III could constitute a putative central therapeutic target for the treatment of hypertension.31 Ang (1–12), an intermediate precursor derived directly from angiotensinogen, was identified recently by Nagata et al.32 Although Ang (1–12) may be an alternate precursor substrate for the formation of bioactive angiotensin peptides, its detailed function is an enigma. Furthermore, cross-talk of Ang II and aldosterone has also received attention. We earlier reported the interaction between Ang II and aldosterone on vascular smooth muscle cell proliferation, and the interaction between Ang II and Aldo on vascular smooth muscle cell proliferation33 and senescence.34 These results provide evidence that blockade of both Ang II and aldosterone could be of therapeutic benefit for vascular disorders.
Emerging concept of the renin–angiotensin system. Metabolism of angiotensinogen and major players in renin–angiotensin system. ACE, angiotensin converting enzyme; ACE2, angiotensin converting enzyme-2; AMP, aminopeptidase; D-Amp, dipeptidyl-aminopeptidase; IRAP, insulin-regulated aminopeptidase; NEP, neutral-endopeptidase; PCP, prolyl-carboxypeptidase; PEP, prolyl-endopeptidase.
Although the correlation between the emerging concept of RAS and pathophysiological conditions has not been elucidated in detail, further investigation of the functional regulation of Ang II receptor-interacting proteins, receptor modification and new players in RAS could be useful for new drug discovery for ameliorating the enhanced tissue RAS.
Tissue renin–angiotensin system
Vascular remodeling, atherosclerosis and senescence
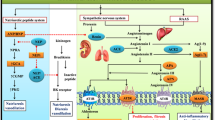
Ang II is generated by ACE secreted from endothelial cells, and constricts blood vessels through AT1 receptors that are expressed in them.35, 36 In blood vessels, RAS induces pathophysiological disorders after an increase in oxidative stress, mediated mainly by NAD(P)H oxidase.37, 38, 39 In endothelial cells, the NAD(P)H oxidase induces production of superoxide (·O2−), which oxidizes tetrahydrobiopterin (BH4), a co-factor of the enzyme endothelial nitric oxide (NO) synthase. In the presence of a high BH4 concentration, endothelial NO synthase is dimerized and produces NO. Reduced availability of BH4 causes uncoupling of endothelial NO synthase , leading to production of ·O2−, reduced availability of NO and generation of peroxynitrate (·ONOO−) as a result of the action of ·O2− on NO.40 Production of increased reactive oxygen species also leads to the activation of redox-sensitive pro-inflammatory transcription factors, such as NF (nuclear factor)-κB and Ets-1, which trigger and/or potentiate the inflammatory cascade.41, 42, 43 Reactive oxygen also promotes the expression of VCAM-1 (vascular cell adhesion molecule-1) and ICAM-1 (intercellular adhesion molecule-1) in endothelial cells, and that of VCAM-1, MCP-1 (monocyte chemotactic protein-1) and IL-6 (interleukin-1) in smooth muscle cells.44, 45 Therefore, AT1-receptor-induced oxidative stress may cause NO inactivation, lipid oxidation and activation of redox-sensitive genes, such as chemotaxis and adhesion molecules, pro-inflammatory cytokines and matrix metalloproteinases, all of which are involved in the initiation and progression of endothelial dysfunction and which manifest atherosclerosis. Although apolipoprotein E-deficient mice with a high-cholesterol diet show marked arteriosclerosis, administration of an ACEI or ARB to these mice suppresses the development of arteriosclerosis.46, 47 Moreover, activation of RAS is also related to the formation of thrombus, because Ang II activates plasminogen activator inhibitor type 1 (PAI-1) in endothelial cells.48 Thus, when the vascular RAS is activated by hypertension, not only the development of coronary artery plaque but also the formation of thrombus is accelerated, and this is considered to be involved in the destabilization of arteriosclerotic plaque. Therefore, the HOPE (Heart Outcomes Prevention Evaluation) study proved clinically that RAS inhibition not only decreases blood pressure but is also vasoprotective49 (Figure 2).
On the other hand, vascular senescence mediated by AT1 receptor stimulation has been highlighted recently,50 and ARBs have been shown to prevent vascular disorders associated with aging.51, 52 Recently, it was reported that the senescence of smooth muscle cells was increased by persistent Ang II stimulation.34 This senescence was suppressed by an ARB. A similar result was also obtained by the administration of aldosterone. Although senescence was not seen in smooth muscle cells treated with low-concentration Ang II or aldosterone added individually, senescence was induced by adding low-concentration Ang II and aldosterone simultaneously. This result suggests that Ang II and aldosterone have an interaction in vascular smooth muscle cells.
Heart
Although diuretics and cardiotonic agents were used mainly for the medical treatment of heart failure till 1980, they were not associated with a marked improvement in prognosis.53, 54, 55, 56, 57, 58 Entering the 1980s, research on neurohumoral factors, such as the sympathetic nerve RAS progressed, and the beneficial effects of ACEIs in heart failure were proved by large clinical trials, such as the CONSENSUS (Cooperative North Scandinavian Enalapril Survival Study)59 and the SOLVD (Studies of Left Ventricular Dysfunction),60 and they were used as the first-line drug. In the Valsartan Heart Failure Trial (Val-HeFT),61 together with the standard treatment, an ARB was proved to reduce CV events in heart failure patients. Moreover, the CHARM (Candesartan in Heart Failure Assessment of Reduction in Mortality and Morbidity) study also showed that the ARB candesartan was generally well tolerated and significantly reduced CV deaths and hospital admissions for heart failure.62
Ang II receptors are expressed in the human heart,63 and their expression is changed in the failing heart. Haywood et al.64 showed that AT1 receptor expression decreased in the failing human ventricle, whereas AT2 receptor expression was unaffected. Moreover, especially in human primary pulmonary hypertension hearts, the AT1 receptor was downregulated only in the failing right ventricle,65 suggesting that Ang II receptors may be regulated differentially in the failing heart. Basic research has also shown the role of RAS in the heart. The mice have two AT1 receptor subtypes: AT1a and AT1b. Ang II acts mainly through AT1a receptors. In AT1a receptor-deficient mice with myocardial infarction, cardiac muscle remodeling was less marked and the survival rate was higher compared with those in wild-type mice.66 In contrast, overexpression of the AT1 receptor in cardiomyocytes induced significant cardiac hypertrophy and remodeling, with increased expressions of ventricular atrial natriuretic factor and interstitial collagen deposition, and the mice died prematurely of heart failure67 showing upregulation of gene expression, such as c-Jun N-terminal kinase and c-fos.68 Upregulation of c-fos in cardiomyocytes by Ang II administration activates protein kinase C and extracellular signal-regulated kinase, and results in cardiac hypertrophy.69, 70 Moreover, cardiac myocytes have the ability to sense mechanical stretch and convert it into intracellular growth signals, resulting in cardiac hypertrophy. Mechanical stretch stimulates the rapid secretion of Ang II from neonatal rat cardiac myocytes.71 Furthermore, recently, mechanical stretch was reported to activate the AT1 receptor independently of Ang II.25 This activation can be inhibited by some ARBs, which are inverse agonists of the AT1 receptor, indicating a therapeutic effect of RAS inhibitionthrough multiple mechanisms dependent and independent of the AT1 receptor (Figure 2).
Aldosterone has recently been implicated as playing a major role in the progression of heart failure. Major clinical trials designed to analyze clinical outcomes of heart failure using an aldosterone antagonist, such as spironolactone or eplerenone, have been conducted. The first, the RALES (Randomized Aldactone Evaluation Study), showed that an aldosterone antagonist, spironolactone, significantly reduced mortality in symptomatic chronic advanced heart failure patients compared with that in placebo.72 The second was the EPHESUS (Eplerenone Post myocardial infarction Heart failure Efficacy and SUrvival Study), which showed a significant reduction in mortality and hospitalization in post-myocardial infarction patients with heart failure by a selective mineralocorticoid receptor blocker, eplerenone.73 These trials showed a beneficial effect of an aldosterone antagonist in chronic advanced heart failure patients, as well as post-myocardial infarction heart failure patients with reduced ejection fraction.
Kidney
The RAS has been developed for maintaining the sodium and electrolyte balance so that land animals can maintain body fluid. In recent times, however, the excess intake of sodium chloride has contributed to the development of hypertension, the metabolic syndrome and other lifestyle-related diseases.
All components of RAS are expressed in the kidney, and it appears that most renal AT1 receptors are exposed to locally generated Ang II rather than to Ang II from circulation.74 Ang II acts on the renal tubules, promotes the reabsorption of sodium, and has an effect that increases blood pressure. Gene-modification mice, which are double transgenic with human angiotensinogen and human renin in the proximal tubule, have significantly increased blood pressure, suggesting that activation of RAS in the kidney influences blood pressure. Moreover, as Ang II has a greater constrictive effect on the efferent arteriole than the afferent arteriole through AT1 receptor stimulation, excess pressure in the glomerular endothelial cells and the mesangial cells leads to nephropathy and renal dysfunction. Therefore, RAS inhibition increases renal blood flow beyond antihypertensive effects. Other beneficial roles of RAS inhibition in the kidney have been reported (Figure 2). For example, administration of an ARB in a diabetic nephropathy rat model prevents the development of nephropathy.75 Also, RAS inhibition prevents renal fibrosis.76, 77, 78 In clinical trials, the risk of onset of end-stage renal failure was inhibited by ARB treatment in the RENAL (Reduction of Endpoints in non-insulin-dependent diabetes mellitus (NIDDM) with the Angiotensin II Antagonist Losartan) and the IDNT (Irbesartan Diabetic Nephropathy Trial) studies.79, 80 Moreover, IRMA2 (IRbesartan in patients with type II diabetes and Micro-Albuminuria Study) showed that the ARB irbesartan exerts renal protection without a decrease in blood pressure.81
The renal protective effects of aldosterone blockade independent of Ang II blockade have been reported in animal models, and an additional effect of aldosterone blockade with Ang II inhibition has also been shown in clinical studies.82 For example, blockade of aldosterone, independent of RAS blockade, reduces proteinuria and nephrosclerosis in the SHRSP (spontaneously hypertensive, stroke-prone) rat.83 Clinically, co-administration of eplerenone with an ACEI, enalapril, significantly reduced albuminuria in patients with diabetes, compared with enalapril treatment alone.84 Moreover, the plasma concentration of aldosterone is reported to begin to rise after long-term RAS blockade in some patients.85 These ‘aldosterone breakthrough’ effects reflect incomplete blockade of RAS, and may promote renal injury even in patients with RAS blockade.
Brain
Recently, there has been a focus on the local RAS in the brain.86 Although it is thought that Ang II does not cross the blood–brain barrier, it is reported that all components of RAS exist in the central nervous system, suggesting that Ang II is produced and functions in the central nervous system (Figure 3).
Recent large clinical trials, such as the LIFE (Losartan Intervention For Endpoint) reduction in hypertension87 and the MOSES (MOrbidity and mortality after Stroke, Eprosartan compared with nitrendipine for Secondary prevention)88 studies, indicated that the blockade of RAS is effective in preventing a first or recurrent stroke beyond its blood pressure-lowering effects. The ACCESS (Acute Candesartan Cilexetil Therapy in Stroke Survivors) study showed lower mortality at 12 months after stroke in the candesartan-treated group compared with that in the placebo group even with similar blood pressure in the 7 days after stroke in the two groups, suggesting that RAS inhibition in the acute phase of stroke leads to brain protection without a hypotensive effect.89 Moreover, the MOSES study showed that the primary end point, a composite of total mortality and all CV and cerebrovascular events, was significantly lower for treatment with an ARB, eprosartan without a change of blood pressure.88 An experimental brain injury model with middle cerebral artery occlusion, using genetically modified mice, revealed that AT1 receptor signaling enhances brain damage partly because of an increase in oxidative stress in the ischemic brain and a decrease in cerebral blood flow in the penumbral region of the middle cerebral artery territory. In contrast, the activation of the AT2 receptor-attenuated brain injury,90 with counter-regulatory effects on the AT1 receptor and the enhancement of neural differentiation and the repair of damaged DNA by the induction of a neural differentiating factor, MMS2, which is one of the ubiquitin conjugating enzyme variants.86 Recent studies have also shown the possibility that stimulation of AT2 receptors may promote cell differentiation and regeneration in neuronal tissue.4, 91 Li et al.92 reported that AT2 receptor stimulation supported neuronal survival and neurite outgrowth in response to ischemia-induced neuronal injury. Moreover, Gallo-Payet et al.93 showed that Ang II induces neural differentiation and neurite outgrowththrough mitogen-activated protein kinase or produces NO94 through AT2 receptor activation and is involved in brain development.95 This accumulating evidence indicates that AT2 receptor signaling acts as a crucial cerebroprotective factor after stroke.
Moreover, we also showed that a non-hypotensive dose of a mineralocorticoid receptor antagonist, eplerenone, reduced the stroke size after middle cerebral artery occlusion in mice.96 These inhibitory effects of eplerenone on stroke size in the brain were at least partly owing to an improvement in the early phase of cerebral blood flow in the peripheral region of the ischemic area and to the prevention of superoxide production in the injured brain. Furthermore, spironolactone improves the structure and increases the tone in the cerebral vasculature of male SHRSP,97 indicating that long-term administration of spironolactone is effective in the prevention of stroke onset. These results indicate that aldosterone is involved in stroke onset and in the expansion of brain damage after ischemic stroke.
Although an improvement of the cognitive function by RAS inhibition has not been confirmed clinically, RAS inhibition is expected to prevent a cognitive decline in Alzheimer's disease98 and in the metabolic syndrome,99 based on animal studies. Recently, it has been proven that RAS inhibition by an ARB is expected to prevent the onset of Alzheimer's disease. An ARB, valsartan, was able to attenuate oligomerization of amyloid β peptides into high-molecular-weight oligomeric peptides.100 Moreover, treatment with valsartan also attenuated the development of amyloid β-mediated cognitive impairment in Tg2576 mice, an Alzheimer's disease mouse model. On the other hand, ACE is concerned with the decomposition of amyloid β.101 In a clinical investigation of the relationship between antihypertensive medication use and the onset of Alzheimer's disease,102 the onset of Alzheimer's disease was attenuated by a diuretic agent or calcium channel blocker; however, an ACEI failed to prevent Alzheimer's disease, indicating the involvement of ACE in amyloid β deposition. However, amyloid β level in the brain was not changed in ACE-deficient mice, suggesting that further investigations are required to determine whether ACE is actually involved in the decomposition of amyloid β.103
Moreover, potassium-sparing diuretics, which include spironolactone and eplerenone, are associated with the reduced incidence of Alzheimer's disease according to the examination of the relationship of antihypertensive medication with Alzheimer's disease onset in the elderly population aged 65 years and older in Cache County, Utah, USA.102 Although further investigation is needed, these results suggest that aldosterone may affect the incidence of Alzheimer's disease.
Metabolic syndrome
The VALUE (Valsartan Antihypertensive Long-term Use Evaluation) study104 and other large clinical studies showed that a new onset of diabetes is suppressed by administration of an ARB compared with other antihypertensive agents, such as calcium channel blockers and β-blockers. Thus, local actions of RAS in adipose tissue,105 skeletal muscle and the pancreas have also been highlighted recently. Obesity is one of the major risks for the metabolic syndrome with hypertension and glucose intolerance. However, there have been inconsistent reports on the role of the adipose tissue RAS. There are at least two differentiation steps in adipogenesis involving RAS; from mesenchymal stem cell (MSC) to adipocytes and from preadipocytes to adipocytes. The inhibitory effects of Ang II seem to differ between MSC and preadipocyte differentiation. Janke et al.106 reported that Ang II inhibits differentiation of human adipocyte progenitor cells, and inhibiting this function by an ARB, thereby results in large insulin-resistant adipocytes with an increased storage of lipid.105 In contrast, blockade of RAS promotes the recruitment of preadipocytes, thereby increasing the number of small insulin-sensitive adipocytes. This hypothesis is supported by the observation by Shimamoto et al.107 that an ARB, olmesartan, significantly reduced adipocyte size in fructose-fed rats, with an improvement in glucose intolerance. In association with preadipocyte differentiation, an ARB increased well-differentiated adipocytes, which can secrete inflammatory adipocytokines, such as TNF-α, and more beneficial adipocytokines, such as adiponectin. Therefore, the effect of an ARB on preadipocyte differentiation is to increase ‘well-differentiated adipocytes’ rather than ‘poorly differentiated adipocytes’. On the other hand, in MSC differentiation, relative stimulation of AT2 receptors by an ARB increased less-differentiated adipocytes, such as progenitors with adipocyte characteristics, which secrete less adipocytokines and may have transdifferentiation potential.108 Thus, ARBs have two different possible beneficial effects on adipocyte differentiation, resulting in an improvement in the metabolic syndrome (Figure 4).
Moreover, we earlier reported that blockade of RAS by an ARB, valsartan, increased insulin uptake into skeletal muscle and attenuated the increase in plasma glucose concentration.109 Insulin-induced phosphorylation of insulin receptor substrate-1 (IRS-1), the association of IRS-1 with the p85 regulatory subunit of phosphoinositide 3 kinase (PI 3-K), PI 3-K activity and the translocation of glucose transporter type 4 (GLUT4) to the plasma membrane are exaggerated by valsartan treatment. Furthermore, Ang II receptors are expressed in the pancreatic tissue.110 An increase in Ang II suppressed the secretion of insulin dose-dependently in hyperglycemic mice.111 Moreover, administration of an ACEI or ARB attenuated inflammation and fibrosis in the pancreas.112, 113 These results indicate that RAS inhibition prevents the onset of diabetes and the metabolic syndrome.
Other tissues
Fibroproliferative diseases, including liver cirrhosis, pulmonary fibrosis, aortic aneurysm and macular degeneration, are also target-organ diseases and are the leading causes of morbidity and mortality. CV disease and progressive kidney disease also involve these pathological disorders. Fibrosis is characterized by the accumulation of matrix molecules, such as collagen and fibronectin, owing to overexpression and decreased clearance and degradation of these matrix components. Epithelial–mesenchymal transition, a process through which an epithelial cell changes its phenotype to become more like a mesenchymal cell, activates local tissue fibroblasts. Ang II induces an epithelial–mesenchymal transition through increased expression of vimentin and α-smooth muscle actin and downregulation of E-cadherin, followed by phosphorylation of Smad2/3 by TGF-β (transforming growth factor-β) activation.114 Recently, an association of fibroproliferative diseases with upregulation of TGF-β by Ang II has been reported.
Hepatocytes are the main source of angiotensinogen.115, 116 Recently, the hepatic RAS has been reported to be related to the pathogenesis of chronic liver disease. Hepatic RAS is upregulated in chronic liver injury, and contributes to oxidative stress,117 recruitment of inflammatory cells and the development of fibrosis. In AT1a-deficient mice, inflammation and fibrosis were attenuated after treatment with either CCl4 or bile duct ligation.118, 119 Although large randomized clinical trials have not been conducted to date, on the basis of the results of clinical120 and experimental studies in vivo121, 122 and in vitro,123 RAS inhibition has been expected to become a potential new therapeutic strategy against the progression of chronic liver disease, for preventing liver fibrosis.
An elevated ACE concentration in bronchoalveolar lavage fluid and/or serum has been reported in many potentially fibrotic lung diseases, including sarcoidosis,124 idiopathic pulmonary fibrosis125 and in the acute respiratory distress syndrome.126 Ang II has been identified as a proapoptotic and profibrotic factor in experimental lung fibrosis models, and patients with the insertion/deletion (ID)/deletion/deletion (DD) polymorphism of ACE, which confers higher levels of ACE, are predisposed to pulmonary fibrosis.127 ACEI and ARB prevented experimental lung fibrosisthrough inhibition of the angiotensin/TGF-β ‘autocrine loop’,128 indicating that RAS inhibition may prevent the fibrotic change in the lung.
On the other hand, excessive TGF-β signaling enlarges the aortic root and results in aortic aneurysm. Treatment with an ARB attenuated aortic root dilatation in a mouse model129 and in patients with Marfan's syndrome.130 Marfan's syndrome is a disorder of connective tissue resulting from mutations in the gene for fibrillin-1, which leads to skeletal muscle weakness and CV abnormalities. A similar group also reported that treatment with the ARB losartan normalized muscle architecture observed in fibrillin-1 deficient mice, a mouse model of Marfan’s syndrome.131 Interestingly, losartan treatment improved the muscle function in a dystrophin-deficient mouse model of Duchenne's muscular dystrophy.131
Further clinical investigation should be carried out to prove the actual beneficial effect of RAS inhibition in such fibroproliferative diseases in the future.
Conclusions
Recent clinical studies indicate multiple preventive effects of the blockade of RAS on target organ damage. As the TROPHY (Trial Of Preventing Hypertension) showed recently that the treatment of prehypertension with an ARB, candesartan, reduced the incidence of hypertension even after the cessation of ARB administration,132 RAS inhibition may have to be initiated as soon as possible for resetting RAS. Moreover, in some patients, long-term treatment with an ACEI or ARB induces an increase in serum aldosterone level, which is called ‘aldosterone breakthrough’.133 Therefore, in the next stage, further investigation is necessary to determine when to start and what doses of ACEI and ARB and other RAS inhibition agents to use through a comparison of the long-term therapeutic effects of RAS inhibition with single and combined agents for the optimal prevention of target organ damage.
References
Kearney PM, Whelton M, Reynolds K, Muntner P, Whelton PK, He J . Global burden of hypertension: analysis of worldwide data. Lancet 2005; 365: 217–223.
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo Jr JL, Jones DW, Materson BJ, Oparil S, Wright Jr JT, Roccella EJ, National Heart, Lung, and Blood Institute Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure; National High Blood Pressure Education Program Coordinating Committee. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA 2003; 289: 2560–2572.
Dzau V, Braunwald E . Resolved and unresolved issues in the prevention and treatment of coronary artery disease: a workshop consensus statement. Am Heart J 1991; 121: 1244–1263.
de Gasparo M, Catt KJ, Inagami T, Wright JW, Unger T . International Union of Pharmacology. XXIII. The angiotensin II receptors. Pharmacol Rev 2000; 52: 415–472.
Shivakumar BR, Wang Z, Hammond TG, Harris RC . EP24.15 interacts with the angiotensin II type I receptor and bradykinin B2 receptor. Cell Biochem Funct 2005; 23: 195–204.
Seachrist JL, Laporte SA, Dale LB, Babwah AV, Caron MG, Anborgh PH, Ferguson SS . Rab5 association with the angiotensin II type 1A receptor promotes Rab5 GTP binding and vesicular fusion. J Biol Chem 2002; 277: 679–685.
Scott MG, Pierotti V, Storez H, Lindberg E, Thuret A, Muntaner O, Labbé-Jullié C, Pitcher JA, Marullo S . Cooperative regulation of extracellular signal-regulated kinase activation and cell shape change by filamin A and beta-arrestins. Mol Cell Biol 2006; 26: 3432–3445.
Pulakat L, Gray A, Johnson J, Knowle D, Burns V, Gavini N . Role of C-terminal cytoplasmic domain of the AT2 receptor in ligand binding and signaling. FEBS Lett 2002; 524: 73–78.
Pulakat L, Cooper S, Knowle D, Mandavia C, Bruhl S, Hetrick M, Gavini N . Ligand-dependent complex formation between the angiotensin II receptor subtype AT2 and Na+/H+ exchanger NHE6 in mammalian cells. Peptides 2005; 26: 863–873.
Fessart D, Simaan M, Laporte SA . c-Src regulates clathrin adapter protein 2 interaction with beta-arrestin and the angiotensin II type 1 receptor during clathrin-mediated internalization. Mol Endocrinol 2005; 19: 491–503.
Daviet L, Lehtonen JY, Tamura K, Griese DP, Horiuchi M, Dzau VJ . Cloning and characterization of ATRAP, a novel protein that interacts with the angiotensin II type 1 receptor. J Biol Chem 1999; 274: 17058–17062.
Nouet S, Amzallag N, Li JM, Louis S, Seitz I, Cui TX, Alleaume AM, Di Benedetto M, Boden C, Masson M, Strosberg AD, Horiuchi M, Couraud PO, Nahmias C . Trans-inactivation of receptor tyrosine kinases by novel angiotensin II AT2 receptor-interacting protein, ATIP. J Biol Chem 2004; 279: 28989–28997.
Lopez-Ilasaca M, Liu X, Tamura K, Dzau VJ . The angiotensin II type I receptor-associated protein, ATRAP, is a transmembrane protein and a modulator of angiotensin II signaling. Mol Biol Cell 2003; 14: 5038–5050.
Cui T, Nakagami H, Iwai M, Takeda Y, Shiuchi T, Tamura K, Daviet L, Horiuchi M . ATRAP, novel AT1 receptor associated protein, enhances internalization of AT1 receptor and inhibits vascular smooth muscle cell growth. Biochem Biophys Res Commun 2000; 279: 938–941.
AbdAlla S, Lother H, Abdel-tawab AM, Quitterer U . The angiotensin II AT2 receptor is an AT1 receptor antagonist. J Biol Chem 2001; 276: 39721–39726.
AbdAlla S, Lother H, Quitterer U . AT1-receptor heterodimers show enhanced G-protein activation and altered receptor sequestration. Nature 2000; 407: 94–98.
Olivares-Reyes JA, Shah BH, Hernandez-Aranda J, García-Caballero A, Farshori MP, García-Sáinz JA, Catt KJ . Agonist-induced interactions between angiotensin AT1 and epidermal growth factor receptors. Mol Pharmacol 2005; 68: 356–364.
Zeng C, Asico LD, Wang X, Hopfer U, Eisner GM, Felder RA, Jose PA . Angiotensin II regulation of AT1 and D3 dopamine receptors in renal proximal tubule cells of SHR. Hypertension 2003; 41: 724–729.
Zeng C, Liu Y, Wang Z, He D, Huang L, Yu P, Zheng S, Jones JE, Asico LD, Hopfer U, Eisner GM, Felder RA, Jose PA . Activation of D3 dopamine receptor decreases angiotensin II type 1 receptor expression in rat renal proximal tubule cells. Circ Res 2006; 99: 494–500.
Zeng C, Luo Y, Asico LD, Hopfer U, Eisner GM, Felder RA, Jose PA . Perturbation of D1 dopamine and AT1 receptor interaction in spontaneously hypertensive rats. Hypertension 2003; 42: 787–792.
Zeng C, Yang Z, Wang Z, Jones J, Wang X, Altea J, Mangrum AJ, Hopfer U, Sibley DR, Eisner GM, Felder RA, Jose PA . Interaction of angiotensin II type 1 and D5 dopamine receptors in renal proximal tubule cells. Hypertension 2005; 45: 804–810.
Zeng C, Wang Z, Asico LD, Hopfer U, Eisner GM, Felder RA, Jose PA . Aberrant ETB receptor regulation of AT receptors in immortalized renal proximal tubule cells of spontaneously hypertensive rats. Kidney Int 2005; 68: 623–631.
Von Bohlen und Halbach O, Walther T, Bader M, Albrecht D . Interaction between Mas and the angiotensin AT1 receptor in the amygdala. J Neurophysiol 2000; 83: 2012–2021.
Bond RA, Ijzerman AP . Recent developments in constitutive receptor activity and inverse agonism, and their potential for GPCR drug discovery. Trends Pharmacol Sci 2006; 27: 92–96.
Zou Y, Akazawa H, Qin Y, Sano M, Takano H, Minamino T, Makita N, Iwanaga K, Zhu W, Kudoh S, Toko H, Tamura K, Kihara M, Nagai T, Fukamizu A, Umemura S, Iiri T, Fujita T, Komuro I . Mechanical stress activates angiotensin II type 1 receptor without the involvement of angiotensin II. Nat Cell Biol 2004; 6: 499–506.
Komuro I . New mechanism of heart protection by angiotensin receptor blockers. Drugs Today (Barc) 2006; 42 (Suppl C): 25–28.
Wallukat G, Homuth V, Fischer T, Lindschau C, Horstkamp B, Jüpner A, Baur E, Nissen E, Vetter K, Neichel D, Dudenhausen JW, Haller H, Luft FC . Patients with preeclampsia develop agonistic autoantibodies against the angiotensin AT1 receptor. J Clin Invest 1999; 103: 945–952.
Dragun D, Brasen JH, Schonemann C, Fritsche L, Budde K, Neumayer HH, Luft FC, Wallukat G . Patients with steroid refractory acute vascular rejection develop agonistic antibodies targeting angiotensin II type 1 receptor. Transplant Proc 2003; 35: 2104–2105.
Dragun D, Muller DN, Brasen JH, Fritsche L, Nieminen-Kelhä M, Dechend R, Kintscher U, Rudolph B, Hoebeke J, Eckert D, Mazak I, Plehm R, Schönemann C, Unger T, Budde K, Neumayer HH, Luft FC, Wallukat G . Angiotensin II type 1-receptor activating antibodies in renal-allograft rejection. N Engl J Med 2005; 352: 558–569.
Ferreira AJ, Raizada MK . Are we poised to target ACE2 for the next generation of antihypertensives? J Mol Med 2008; 86: 685–690.
Reaux A, Fournie-Zaluski MC, Llorens-Cortes C . Angiotensin III: a central regulator of vasopressin release and blood pressure. Trends Endocrinol Metab 2001; 12: 157–162.
Nagata S, Kato J, Sasaki K, Minamino N, Eto T, Kitamura K . Isolation and identification of proangiotensin-12, a possible component of the renin-angiotensin system. Biochem Biophys Res Commun 2006; 350: 1026–1031.
Min LJ, Mogi M, Li JM, Iwanami J, Iwai M, Horiuchi M . Aldosterone and angiotensin II synergistically induce mitogenic response in vascular smooth muscle cells. Circ Res 2005; 97: 434–442.
Min LJ, Mogi M, Iwanami J, Li JM, Sakata A, Fujita T, Tsukuda K, Iwai M, Horiuchi M . Cross-talk between aldosterone and angiotensin II in vascular smooth muscle cell senescence. Cardiovasc Res 2007; 76: 506–516.
Suzuki H, Motley ED, Frank GD, Utsunomiya H, Eguchi S . Recent progress in signal transduction research of the angiotensin II type-1 receptor: protein kinases, vascular dysfunction and structural requirement. Curr Med Chem Cardiovasc Hematol Agents 2005; 3: 305–322.
Hilgers KF, Hilgenfeldt U, Veelken R, Muley T, Ganten D, Luft FC, Mann JF . Angiotensinogen is cleaved to angiotensin in isolated rat blood vessels. Hypertension 1993; 21: 1030–1034.
Wei Y, Whaley-Connell AT, Chen K, Habibi J, Uptergrove GM, Clark SE, Stump CS, Ferrario CM, Sowers JR . NADPH oxidase contributes to vascular inflammation, insulin resistance, and remodeling in the transgenic (mRen2) rat. Hypertension 2007; 50: 384–391.
Griendling KK, Minieri CA, Ollerenshaw JD, Alexander RW . Angiotensin II stimulates NADH and NADPH oxidase activity in cultured vascular smooth muscle cells. Circ Res 1994; 74: 1141–1148.
Fukui T, Ishizaka N, Rajagopalan S, Laursen JB, Capers IV Q, Taylor WR, Harrison DG, de Leon H, Wilcox JN, Griendling KK . p22phox mRNA expression and NADPH oxidase activity are increased in aortas from hypertensive rats. Circ Res 1997; 80: 45–51.
Vasquez-Vivar J, Martasek P, Whitsett J, Joseph J, Kalyanaraman B . The ratio between tetrahydrobiopterin and oxidized tetrahydrobiopterin analogues controls superoxide release from endothelial nitric oxide synthase: an EPR spin trapping study. Biochem J 2002; 362: 733–739.
Bubici C, Papa S, Dean K, Franzoso G . Mutual cross-talk between reactive oxygen species and nuclear factor-kappa B: molecular basis and biological significance. Oncogene 2006; 25: 6731–6748.
Ni W, Zhan Y, He H, Maynard E, Balschi JA, Oettgen P . Ets-1 is a critical transcriptional regulator of reactive oxygen species and p47(phox) gene expression in response to angiotensin II. Circ Res 2007; 101: 985–994.
Adachi T, Yamamoto M, Suematsu M . Targeting NAD(P)H oxidase: Ets-1 regulates p47(phox). Circ Res 2007; 101: 962–964.
Griendling KK, Sorescu D, Lassegue B, Ushio-Fukai M . Modulation of protein kinase activity and gene expression by reactive oxygen species and their role in vascular physiology and pathophysiology. Arterioscler Thromb Vasc Biol 2000; 20: 2175–2183.
Schrader LI, Kinzenbaw DA, Johnson AW, Faraci FM, Didion SP . IL-6 deficiency protects against angiotensin II induced endothelial dysfunction and hypertrophy. Arterioscler Thromb Vasc Biol 2007; 27: 2576–2581.
Keidar S, Attias J, Smith J, Breslow JL, Hayek T . The angiotensin-II receptor antagonist, losartan, inhibits LDL lipid peroxidation and atherosclerosis in apolipoprotein E-deficient mice. Biochem Biophys Res Commun 1997; 236: 622–625.
Hayek T, Attias J, Coleman R, Brodsky S, Smith J, Breslow JL, Keidar S . The angiotensin-converting enzyme inhibitor, fosinopril, and the angiotensin II receptor antagonist, losartan, inhibit LDL oxidation and attenuate atherosclerosis independent of lowering blood pressure in apolipoprotein E deficient mice. Cardiovasc Res 1999; 44: 579–587.
Mogielnicki A, Chabielska E, Pawlak R, Szemraj J, Buczko W . Angiotensin II enhances thrombosis development in renovascular hypertensive rats. Thromb Haemost 2005; 93: 1069–1076.
Yusuf S, Sleight P, Pogue J, Bosch J, Davies R, Dagenais G . Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular events in high-risk patients. The Heart Outcomes Prevention Evaluation Study Investigators. N Engl J Med 2000; 342: 145–153.
Kunieda T, Minamino T, Nishi J, Tateno K, Oyama T, Katsuno T, Miyauchi H, Orimo M, Okada S, Takamura M, Nagai T, Kaneko S, Komuro I . Angiotensin II induces premature senescence of vascular smooth muscle cells and accelerates the development of atherosclerosis via a p21-dependent pathway. Circulation 2006; 114: 953–960.
de Cavanagh EM, Piotrkowski B, Fraga CG . Concerted action of the renin-angiotensin system, mitochondria, and antioxidant defenses in aging. Mol Aspects Med 2004; 25: 27–36.
Basso N, Paglia N, Stella I, de Cavanagh EM, Ferder L, del Rosario Lores Arnaiz M, Inserra F . Protective effect of the inhibition of the renin-angiotensin system on aging. Regul Pept 2005; 128: 247–252.
Massie B, Bourassa M, DiBianco R, Hess M, Konstam M, Likoff M, Packer M . Long-term oral administration of amrinone for congestive heart failure: lack of efficacy in a multicenter controlled trial. Circulation 1985; 71: 963–971.
DiBianco R, Shabetai R, Kostuk W, Moran J, Schlant RC, Wright R . A comparison of oral milrinone, digoxin, and their combination in the treatment of patients with chronic heart failure. N Engl J Med 1989; 320: 677–683.
Uretsky BF, Jessup M, Konstam MA, Dec GW, Leier CV, Benotti J, Murali S, Herrmann HC, Sandberg JA . Multicenter trial of oral enoximone in patients with moderate to moderately severe congestive heart failure. Lack of benefit compared with placebo. Enoximone Multicenter Trial Group. Circulation 1990; 82: 774–780.
Packer M, Carver JR, Rodeheffer RJ, Ivanhoe RJ, DiBianco R, Zeldis SM, Hendrix GH, Bommer WJ, Elkayam U, Kukin ML . Effect of oral milrinone on mortality in severe chronic heart failure. The PROMISE Study Research Group. N Engl J Med 1991; 325: 1468–1475.
Lubsen J, Just H, Hjalmarsson AC, La Framboise D, Remme WJ, Heinrich-Nols J, Dumont JM, Seed P . Effect of pimobendan on exercise capacity in patients with heart failure: main results from the Pimobendan in Congestive Heart Failure (PICO) trial. Heart 1996; 76: 223–231.
Hauptman PJ, Kelly RA . Digitalis. Circulation 1999; 99: 1265–1270.
Kjekshus J, Swedberg K, Snapinn S . Effects of enalapril on long-term mortality in severe congestive heart failure. CONSENSUS Trial Group. Am J Cardiol 1992; 69: 103–107.
Effect of enalapril on mortality and the development of heart failure in asymptomatic patients with reduced left ventricular ejection fractions. The SOLVD Investigators. N Engl J Med 1992; 327: 685–691.
Cohn JN, Tognoni G . A randomized trial of the angiotensin-receptor blocker valsartan in chronic heart failure. N Engl J Med 2001; 345: 1667–1675.
Pfeffer MA, Swedberg K, Granger CB, Held P, McMurray JJ, Michelson EL, Olofsson B, Ostergren J, Yusuf S, Pocock S, CHARM Investigators and Committees. Effects of candesartan on mortality and morbidity in patients with chronic heart failure: the CHARM-Overall programme. Lancet 2003; 362: 759–766.
Regitz-Zagrosek V, Friedel N, Heymann A, Bauer P, Neuss M, Rolfs A, Steffen C, Hildebrandt A, Hetzer R, Fleck E . Regulation, chamber localization, and subtype distribution of angiotensin II receptors in human hearts. Circulation 1995; 91: 1461–1471.
Haywood GA, Gullestad L, Katsuya T, Hutchinson HG, Pratt RE, Horiuchi M, Fowler MB . AT1 and AT2 angiotensin receptor gene expression in human heart failure. Circulation 1997; 95: 1201–1206.
Zisman LS, Asano K, Dutcher DL, Ferdensi A, Robertson AD, Jenkin M, Bush EW, Bohlmeyer T, Perryman MB, Bristow MR . Differential regulation of cardiac angiotensin converting enzyme binding sites and AT1 receptor density in the failing human heart. Circulation 1998; 98: 1735–1741.
Harada K, Sugaya T, Murakami K, Yazaki Y, Komuro I . Angiotensin II type 1A receptor knockout mice display less left ventricular remodeling and improved survival after myocardial infarction. Circulation 1999; 100: 2093–2099.
Paradis P, Dali-Youcef N, Paradis FW, Thibault G, Nemer M . Overexpression of angiotensin II type I receptor in cardiomyocytes induces cardiac hypertrophy and remodeling. Proc Natl Acad Sci USA 2000; 97: 931–936.
Kim S, Iwao H . Molecular and cellular mechanisms of angiotensin II-mediated cardiovascular and renal diseases. Pharmacol Rev 2000; 52: 11–34.
Zou Y, Komuro I, Yamazaki T, Aikawa R, Kudoh S, Shiojima I, Hiroi Y, Mizuno T, Yazaki Y . Protein kinase C, but not tyrosine kinases or Ras, plays a critical role in angiotensin II-induced activation of Raf-1 kinase and extracellular signal-regulated protein kinases in cardiac myocytes. J Biol Chem 1996; 271: 33592–33597.
Yamazaki T, Komuro I, Shiojima I, Yazaki Y . Angiotensin II mediates mechanical stress-induced cardiac hypertrophy. Diabetes Res Clin Pract 1996; 30 (Suppl): 107–111.
Sadoshima J, Izumo S . The cellular and molecular response of cardiac myocytes to mechanical stress. Annu Rev Physiol 1997; 59: 551–571.
Pitt B, Zannad F, Remme WJ, Cody R, Castaigne A, Perez A, Palensky J, Wittes J . The effect of spironolactone on morbidity and mortality in patients with severe heart failure. Randomized Aldactone Evaluation Study Investigators. N Engl J Med 1999; 341: 709–717.
Pitt B, Remme W, Zannad F, Neaton J, Martinez F, Roniker B, Bittman R, Hurley S, Kleiman J, Gatlin M, Eplerenone Post-Acute Myocardial Infarction Heart Failure Efficacy and Survival Study Investigators. Eplerenone, a selective aldosterone blocker, in patients with left ventricular dysfunction after myocardial infarction. N Engl J Med 2003; 348: 1309–1321.
van Kats JP, Schalekamp MA, Verdouw PD, Duncker DJ, Danser AH . Intrarenal angiotensin II: interstitial and cellular levels and site of production. Kidney Int 2001; 60: 2311–2317.
Nagai Y, Yao L, Kobori H, Miyata K, Ozawa Y, Miyatake A, Yukimura T, Shokoji T, Kimura S, Kiyomoto H, Kohno M, Abe Y, Nishiyama A . Temporary angiotensin II blockade at the prediabetic stage attenuates the development of renal injury in type 2 diabetic rats. J Am Soc Nephrol 2005; 16: 703–711.
Mezzano SA, Ruiz-Ortega M, Egido J . Angiotensin II and renal fibrosis. Hypertension 2001; 38: 635–638.
Nakamura S, Nakamura I, Ma L, Vaughan DE, Fogo AB . Plasminogen activator inhibitor-1 expression is regulated by the angiotensin type 1 receptor in vivo. Kidney Int 2000; 58: 251–259.
Nangaku M . Chronic hypoxia and tubulointerstitial injury: a final common pathway to end-stage renal failure. J Am Soc Nephrol 2006; 17: 17–25.
Brenner BM, Cooper ME, de Zeeuw D, Keane WF, Mitch WE, Parving HH, Remuzzi G, Snapinn SM, Zhang Z, Shahinfar S, RENAAL Study Investigators. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001; 345: 861–869.
Lewis EJ, Hunsicker LG, Clarke WR, Berl T, Pohl MA, Lewis JB, Ritz E, Atkins RC, Rohde R, Raz I, Collaborative Study Group. Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 2001; 345: 851–860.
Parving HH, Lehnert H, Brochner-Mortensen J, Gomis R, Andersen S, Arner P . The effect of irbesartan on the development of diabetic nephropathy in patients with type 2 diabetes. N Engl J Med 2001; 345: 870–878.
Epstein M . Aldosterone blockade: an emerging strategy for abrogating progressive renal disease. Am J Med 2006; 119: 912–919.
Rocha R, Chander PN, Khanna K, Zuckerman A, Stier Jr CT . Mineralocorticoid blockade reduces vascular injury in stroke-prone hypertensive rats. Hypertension 1998; 31: 451–458.
Epstein M, Williams GH, Weinberger M, Lewin A, Krause S, Mukherjee R, Patni R, Beckerman B . Selective aldosterone blockade with eplerenone reduces albuminuria in patients with type 2 diabetes. Clin J Am Soc Nephrol 2006; 1: 940–951.
Staessen J, Lijnen P, Fagard R, Verschueren LJ, Amery A . Rise in plasma concentration of aldosterone during long-term angiotensin II suppression. J Endocrinol 1981; 91: 457–465.
Mogi M, Li JM, Iwanami J, Min LJ, Tsukuda K, Iwai M, Horiuchi M . Angiotensin II type-2 receptor stimulation prevents neural damage by transcriptional activation of methyl methanesulfonate sensitive 2. Hypertension 2006; 48: 141–148.
Dahlof B, Devereux RB, Kjeldsen SE, Julius S, Beevers G, de Faire U, Fyhrquist F, Ibsen H, Kristiansson K, Lederballe-Pedersen O, Lindholm LH, Nieminen MS, Omvik P, Oparil S, Wedel H, LIFE Study Group. Cardiovascular morbidity and mortality in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomised trial against atenolol. Lancet 2002; 359: 995–1003.
Schrader J, Luders S, Kulschewski A, Hammersen F, Plate K, Berger J, Zidek W, Dominiak P, Diener HC, MOSES Study Group. Morbidity and Mortality After Stroke, Eprosartan Compared with Nitrendipine for Secondary Prevention: principal results of a prospective randomized controlled study (MOSES). Stroke 2005; 36: 1218–1226.
Schrader J, Luders S, Kulschewski A, Berger J, Zidek W, Treib J, Einhäupl K, Diener HC, Dominiak P, Acute Candesartan Cilexetil Therapy in Stroke Survivors Study Group. The ACCESS Study: evaluation of Acute Candesartan Cilexetil Therapy in Stroke Survivors. Stroke 2003; 34: 1699–1703.
Iwai M, Liu HW, Chen R, Ide A, Okamoto S, Hata R, Sakanaka M, Shiuchi T, Horiuchi M . Possible inhibition of focal cerebral ischemia by angiotensin II type 2 receptor stimulation. Circulation 2004; 110: 843–848.
Reinecke K, Lucius R, Reinecke A, Rickert U, Herdegen T, Unger T . Angiotensin II accelerates functional recovery in the rat sciatic nerve in vivo: role of the AT2 receptor and the transcription factor NF-kappaB. FASEB J 2003; 17: 2094–2096.
Li J, Culman J, Hortnagl H, Zhao Y, Gerova N, Timm M, Blume A, Zimmermann M, Seidel K, Dirnagl U, Unger T . Angiotensin AT2 receptor protects against cerebral ischemia-induced neuronal injury. FASEB J 2005; 19: 617–619.
Gendron L, Laflamme L, Rivard N, Asselin C, Payet MD, Gallo-Payet N . Signals from the AT2 (angiotensin type 2) receptor of angiotensin II inhibit p21ras and activate MAPK (mitogen-activated protein kinase) to induce morphological neuronal differentiation in NG108-15 cells. Mol Endocrinol 1999; 13: 1615–1626.
Cote F, Laflamme L, Payet MD, Gallo-Payet N . Nitric oxide, a new second messenger involved in the action of angiotensin II on neuronal differentiation of NG108-15 cells. Endocr Res 1998; 24: 403–407.
Cote F, Do TH, Laflamme L, Gallo JM, Gallo-Payet N . Activation of the AT(2) receptor of angiotensin II induces neurite outgrowth and cell migration in microexplant cultures of the cerebellum. J Biol Chem 1999; 274: 31686–31692.
Iwanami J, Mogi M, Okamoto S, Gao XY, Li JM, Min LJ, Ide A, Tsukuda K, Iwai M, Horiuchi M . Pretreatment with eplerenone reduces stroke volume in mouse middle cerebral artery occlusion model. Eur J Pharmacol 2007; 566: 153–159.
Rigsby CS, Pollock DM, Dorrance AM . Spironolactone improves structure and increases tone in the cerebral vasculature of male spontaneously hypertensive stroke-prone rats. Microvasc Res 2007; 73: 198–205.
Mogi M, Li JM, Tsukuda K, Iwanami J, Min LJ, Sakata A, Fujita T, Iwai M, Horiuchi M . Telmisartan prevented cognitive decline partly due to PPAR-gamma activation. Biochem Biophys Res Commun 2008; 375: 446–449.
Tsukuda K, Mogi M, Li JM, Iwanami J, Min LJ, Sakata A, Fujita T, Iwai M, Horiuchi M . Amelioration of cognitive impairment in the type-2 diabetic mouse by the angiotensin II type-1 receptor blocker candesartan. Hypertension 2007; 50: 1099–1105.
Wang J, Ho L, Chen L, Zhao Z, Zhao W, Qian X, Humala N, Seror I, Bartholomew S, Rosendorff C, Pasinetti GM . Valsartan lowers brain beta-amyloid protein levels and improves spatial learning in a mouse model of Alzheimer disease. J Clin Invest 2007; 117: 3393–3402.
Hu J, Igarashi A, Kamata M, Nakagawa H . Angiotensin-converting enzyme degrades Alzheimer amyloid beta-peptide (A beta); retards A beta aggregation, deposition, fibril formation; and inhibits cytotoxicity. J Biol Chem 2001; 276: 47863–47868.
Khachaturian AS, Zandi PP, Lyketsos CG, Hayden KM, Skoog I, Norton MC, Tschanz JT, Mayer LS, Welsh-Bohmer KA, Breitner JC . Antihypertensive medication use and incident Alzheimer disease: the Cache County Study. Arch Neurol 2006; 63: 686–692.
Kehoe PG, Wilcock GK . Is inhibition of the renin-angiotensin system a new treatment option for Alzheimer's disease? Lancet Neurol 2007; 6: 373–378.
Julius S, Kjeldsen SE, Weber M, Brunner HR, Ekman S, Hansson L, Hua T, Laragh J, McInnes GT, Mitchell L, Plat F, Schork A, Smith B, Zanchetti A, VALUE trial group. Outcomes in hypertensive patients at high cardiovascular risk treated with regimens based on valsartan or amlodipine: the VALUE randomised trial. Lancet 2004; 363: 2022–2031.
Sharma AM, Janke J, Gorzelniak K, Engeli S, Luft FC . Angiotensin blockade prevents type 2 diabetes by formation of fat cells. Hypertension 2002; 40: 609–611.
Janke J, Engeli S, Gorzelniak K, Luft FC, Sharma AM . Mature adipocytes inhibit in vitro differentiation of human preadipocytes via angiotensin type 1 receptors. Diabetes 2002; 51: 1699–1707.
Furuhashi M, Ura N, Takizawa H, Yoshida D, Moniwa N, Murakami H, Higashiura K, Shimamoto K . Blockade of the renin-angiotensin system decreases adipocyte size with improvement in insulin sensitivity. J Hypertens 2004; 22: 1977–1982.
Matsushita K, Wu Y, Okamoto Y, Pratt RE, Dzau VJ . Local renin angiotensin expression regulates human mesenchymal stem cell differentiation to adipocytes. Hypertension 2006; 48: 1095–1102.
Shiuchi T, Iwai M, Li HS, Wu L, Min LJ, Li JM, Okumura M, Cui TX, Horiuchi M . Angiotensin II type-1 receptor blocker valsartan enhances insulin sensitivity in skeletal muscles of diabetic mice. Hypertension 2004; 43: 1003–1010.
Tahmasebi M, Puddefoot JR, Inwang ER, Vinson GP . The tissue renin-angiotensin system in human pancreas. J Endocrinol 1999; 161: 317–322.
Lau T, Carlsson PO, Leung PS . Evidence for a local angiotensin-generating system and dose-dependent inhibition of glucose-stimulated insulin release by angiotensin II in isolated pancreatic islets. Diabetologia 2004; 47: 240–248.
Kuno A, Yamada T, Masuda K, Ogawa K, Sogawa M, Nakamura S, Nakazawa T, Ohara H, Nomura T, Joh T, Shirai T, Itoh M . Angiotensin-converting enzyme inhibitor attenuates pancreatic inflammation and fibrosis in male Wistar Bonn/Kobori rats. Gastroenterology 2003; 124: 1010–1019.
Yamada T, Kuno A, Masuda K, Ogawa K, Sogawa M, Nakamura S, Ando T, Sano H, Nakazawa T, Ohara H, Nomura T, Joh T, Itoh M . Candesartan, an angiotensin II receptor antagonist, suppresses pancreatic inflammation and fibrosis in rats. J Pharmacol Exp Ther 2003; 307: 17–23.
Daniel C . Blocking of angiotensin II is more than blocking of transforming growth factor-beta. Kidney Int 2008; 74: 551–553.
Paizis G, Cooper ME, Schembri JM, Tikellis C, Burrell LM, Angus PW . Up-regulation of components of the renin-angiotensin system in the bile duct-ligated rat liver. Gastroenterology 2002; 123: 1667–1676.
Morris BJ, Iwamoto HS, Reid IA . Localization of angiotensinogen in rat liver by immunocytochemistry. Endocrinology 1979; 105: 796–800.
Bataller R, Schwabe RF, Choi YH, Yang L, Paik YH, Lindquist J, Qian T, Schoonhoven R, Hagedorn CH, Lemasters JJ, Brenner DA . NADPH oxidase signal transduces angiotensin II in hepatic stellate cells and is critical in hepatic fibrosis. J Clin Invest 2003; 112: 1383–1394.
Kanno K, Tazuma S, Chayama K . AT1A-deficient mice show less severe progression of liver fibrosis induced by CCl(4). Biochem Biophys Res Commun 2003; 308: 177–183.
Yang L, Bataller R, Dulyx J, Coffman TM, Ginès P, Rippe RA, Brenner DA . Attenuated hepatic inflammation and fibrosis in angiotensin type 1a receptor deficient mice. J Hepatol 2005; 43: 317–323.
Yoshiji H, Noguchi R, Fukui H . Combined effect of an ACE inhibitor, perindopril, and interferon on liver fibrosis markers in patients with chronic hepatitis C. J Gastroenterol 2005; 40: 215–216.
Wei YH, Jun L, Qiang CJ . Effect of losartan, an angiotensin II antagonist, on hepatic fibrosis induced by CCl4 in rats. Dig Dis Sci 2004; 49: 1589–1594.
Nabeshima Y, Tazuma S, Kanno K, Hyogo H, Iwai M, Horiuchi M, Chayama K . Anti-fibrogenic function of angiotensin II type 2 receptor in CCl4-induced liver fibrosis. Biochem Biophys Res Commun 2006; 346: 658–664.
Kurikawa N, Suga M, Kuroda S, Yamada K, Ishikawa H . An angiotensin II type 1 receptor antagonist, olmesartan medoxomil, improves experimental liver fibrosis by suppression of proliferation and collagen synthesis in activated hepatic stellate cells. Br J Pharmacol 2003; 139: 1085–1094.
Lieberman J . Elevation of serum angiotensin-converting-enzyme (ACE) level in sarcoidosis. Am J Med 1975; 59: 365–372.
Specks U, Martin II WJ, Rohrbach MS . Bronchoalveolar lavage fluid angiotensin-converting enzyme in interstitial lung diseases. Am Rev Respir Dis 1990; 141: 117–123.
Fourrier F, Chopin C, Wallaert B, Mazurier C, Mangalaboyi J, Durocher A . Compared evolution of plasma fibronectin and angiotensin-converting enzyme levels in septic ARDS. Chest 1985; 87: 191–195.
Morrison CD, Papp AC, Hejmanowski AQ, Addis VM, Prior TW . Increased D allele frequency of the angiotensin-converting enzyme gene in pulmonary fibrosis. Hum Pathol 2001; 32: 521–528.
Uhal BD, Kim JK, Li X, Molina-Molina M . Angiotensin-TGF-beta 1 crosstalk in human idiopathic pulmonary fibrosis: autocrine mechanisms in myofibroblasts and macrophages. Curr Pharm Des 2007; 13: 1247–1256.
Habashi JP, Judge DP, Holm TM, Cohn RD, Loeys BL, Cooper TK, Myers L, Klein EC, Liu G, Calvi C, Podowski M, Neptune ER, Halushka MK, Bedja D, Gabrielson K, Rifkin DB, Carta L, Ramirez F, Huso DL, Dietz HC . Losartan, an AT1 antagonist, prevents aortic aneurysm in a mouse model of Marfan syndrome. Science 2006; 312: 117–121.
Brooke BS, Habashi JP, Judge DP, Patel N, Loeys B, Dietz III HC . Angiotensin II blockade and aortic-root dilation in Marfan's syndrome. N Engl J Med 2008; 358: 2787–2795.
Cohn RD, van Erp C, Habashi JP, Soleimani AA, Klein EC, Lisi MT, Gamradt M, ap Rhys CM, Holm TM, Loeys BL, Ramirez F, Judge DP, Ward CW, Dietz HC . Angiotensin II type 1 receptor blockade attenuates TGF-beta-induced failure of muscle regeneration in multiple myopathic states. Nat Med 2007; 13: 204–210.
Julius S, Nesbitt SD, Egan BM, Weber MA, Michelson EL, Kaciroti N, Black HR, Grimm Jr RH, Messerli FH, Oparil S, Schork MA, Trial of Preventing Hypertension (TROPHY) Study Investigators. Feasibility of treating prehypertension with an angiotensin-receptor blocker. N Engl J Med 2006; 354: 1685–1697.
Bomback AS, Klemmer PJ . The incidence and implications of aldosterone breakthrough. Nat Clin Pract Nephrol 2007; 3: 486–492.
Acknowledgements
This study was supported by grants from the Ministry of Education, Science, Sports, and Culture of Japan to MH and MM and from the Takeda Science Foundation to MM.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Iwanami, J., Mogi, M., Iwai, M. et al. Inhibition of the renin–angiotensin system and target organ protection. Hypertens Res 32, 229–237 (2009). https://doi.org/10.1038/hr.2009.5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2009.5
Keywords
This article is cited by
-
Clarification of hypertension mechanisms provided by the research of central circulatory regulation
Hypertension Research (2023)
-
Reversal of deleterious effect of hypertension on the liver by inhibition of endoplasmic reticulum stress
Molecular Biology Reports (2020)
-
Novel RAAS agonists and antagonists: clinical applications and controversies
Nature Reviews Endocrinology (2015)
-
Programming of Essential Hypertension: What Pediatric Cardiologists Need to Know
Pediatric Cardiology (2015)
-
Azilsartan Decreases Renal and Cardiovascular Injury in the Spontaneously Hypertensive Obese Rat
Cardiovascular Drugs and Therapy (2014)