Abstract
Numerous in vitro and in vivo animal studies using the (pro)renin receptor (P)RR blocker handle region peptide have suggested an important role of (P)RR in the pathogenesis of end-stage organ damage in patients with diabetes and hypertension. In addition, a limited number of clinical studies have suggested an association between (P)RR gene polymorphisms and blood pressure levels and between (P)RR mRNA levels and angiotensin-converting enzyme mRNA levels in human arteries. However, recent studies have shown that the (P)RR is divided into its soluble form and a residual hydrophobic part, which includes ATPase 6 associated protein 2, within cells. Therefore, the (P)RR may have a more complex function than previously thought. In addition, the physiological roles of the (P)RR remain undetermined, because the construction of (P)RR null mice has not been successful. As a next step for research in this area, a method for determining the soluble (P)RR levels in plasma and urine and the construction of tissue-specific (P)RR-knockout mice are needed to elucidate the roles of the (P)RR in physiology and pathophysiology.
Similar content being viewed by others
Introduction
The pathophysiological roles of the (pro)renin receptor ((P)RR) are a growing concern because numerous experimental studies conducted since this receptor was first discovered in 20021 have suggested that the pro(renin) receptor has its own intracellular signaling pathways and is involved in the tissue renin–angiotensin system. However, the clinical relevance of the human (P)RR remains uncertain because only a few clinical studies examining the (P)RR have been performed. In this review article of previous studies and new findings, we attempt to elucidate the possible role of the (P)RR in humans.
Suggestions from in vitro studies
The (P)RR was first reported to be capable of binding both renin and prorenin in vitro.1 However, Batenburg et al.2 showed that prorenin, but not renin, was capable of binding to the (P)RR in cultured vascular smooth muscle cells, suggesting that prorenin is an endogenous agonist of the (P)RR. In addition, Nabi et al.3 provided clear evidence that receptor-bound prorenin gains ‘renin activity’ without undergoing the proteolytic cleavage of the prosegment of prorenin as a result of a conformational change, although the enzymatic activity of receptor-bound renin is similar to that of free renin. On the basis of these findings, renin may be an endogenous inhibitor for the binding of prorenin to the (P)RR.
Stimulation of the (P)RR by renin and prorenin reportedly results in the activation of intracellular signaling pathways, including MAP kinases, in mesangial cells,4, 5, 6 vascular smooth muscle cells,7 cardiomyocytes8 and renal tubular epithelial cells.9 However, the significance of the (P)RR-dependent intracellular signals in vivo remains undetermined.
Suggestions from animal models of diabetes
When a specific protein binds to the ‘handle region’ of the prosegment of prorenin, the protein-bound prorenin exerts ‘renin activity’ without changing the molecular weight of prorenin.10 On the basis of this finding, the ‘handle region’ of prorenin prosegment was thought to be a candidate of the prorenin site binding (P)RR. This concept was recently confirmed by the study using the BIACORE method showing that a peptide corresponding to the ‘handle region’ (HRP) binds to the (P)RR and that pretreatment with HRP inhibits the prorenin binding to the (P)RR.3, 11 Thus, HRP was thought to be a competitive inhibitor for prorenin binding to the (P)RR in vitro.
To elucidate in vivo its usefulness as a (P)RR blocker, HRP was administered to rats with streptozotocin-induced type I diabetes.12 The administration of HRP for 6 months significantly inhibited the increase in renal angiotensin II levels and the development of proteinuria and glomerulosclerosis, suggesting that the non-proteolytic activation of prorenin bound to the (P)RR has an important role in the development of nephropathy. Although the renal mRNA expression of the (P)RR in control and diabetic rats was similar, non-proteolytically activated prorenin increased in the kidneys of the diabetic rats, and this increase was inhibited by HRP. As the mRNA expression of cathepsin B, a processing enzyme contributing to the conversion of prorenin to renin, simultaneously decreased in the kidneys of the diabetic rats, prorenin may have accumulated in their kidneys. In addition, the release of prorenin into the circulation may have been elevated in the diabetic rats. Thus, receptor-bound prorenin may be elevated by an increase in prorenin levels and/or an increase in (P)RR levels,13 thereby contributing to the development of nephropathy in diabetic animals. These findings were recently confirmed by Matavelli et al.14 The direct administration of HRP to the renal cortical interstitium of diabetic rats significantly decreased urinary albumin excretion and the renal production of tumor necrosis factor-α and interleukin-1β. A similar improvement in nephropathy after HRP treatment was observed in streptozotocin-induced diabetic rats in which nephropathy had already developed15 and in angiotensin II-type Ia-receptor-deficient mice with streptozotocin-induced diabetes.16 These latter results indirectly suggested that (P)RR-dependent intracellular signals may also contribute to the development and progression of diabetic nephropathy.
Furthermore, in streptozotocin-induced diabetic rats with a significant increase in the retinal expression of prorenin, the administration of HRP significantly suppressed retinal adherent leukocytes and inhibited the diabetes-induced retinal expression of vascular endothelial growth factor and ICAM-1.17 Similar results were also confirmed by Wilkinson-Berka et al. (personal communication). Thus, in animal studies, prorenin and the (P)RR appear to be significantly involved in the pathogenesis of diabetic microvascular complications.
Suggestions from animal models of hypertension
Elevated tissue levels of angiotensin I and II, glomerulosclerosis with proteinuria, and cardiac hypertrophy with left ventricular fibrosis have been observed in young hypertensive SHRsp rats fed a high-salt diet. The administration of HRP significantly attenuated, but did not completely suppress, these changes without affecting the development of hypertension.18, 19 These findings were recently confirmed by Susic et al.20 PRAM-1, which is identical to HRP, significantly decreased the serum creatinine level, left ventricular mass, left ventricular function and left ventricular fibrosis in SHR rats fed a high-salt diet. Interestingly, the beneficial effects of PRAM-1 were reduced in SHR rats fed a normal-salt diet. In addition, treatment with HRP had no effects under high plasma renin conditions.21, 22 On the basis of these findings, the possible explanation that high-salt diet-induced decrease in plasma renin levels might influence the effectiveness of the (P)RR blockers was raised, although there has been no direct evidence for the difference in binding of prorenin to the (P)RR between the high-salt diet and normal-salt diet. The affinities of renin and prorenin to bind to the (P)RR are similar; nevertheless, binding to the (P)RR makes prorenin non-proteolytically active but does not change the activity of renin.23 Thus, renin may be an endogenous inhibitor for prorenin's binding to the (P)RR, thereby reducing the benefit of HRP during a normal-salt diet compared with a high-salt diet.20 As renin is still active even in the presence of HRP, active renin in the plasma would have a pivotal role in pathogenesis under conditions with high plasma renin levels.21, 22 This concept was supported by recent studies showing that the renin inhibitor aliskiren, but not HRP, offered benefits to double transgenic rats overexpressing the human renin and angiotensinogen genes and with extremely high plasma renin levels,22 whereas the 14-day administration of HRP did not improve the acute nephropathy that occurred in the kidneys of Goldblatt hypertensive rats.21 Recent studies have shown that an increase in circulating prorenin level is not associated with organ damage.24, 25 As elevated levels of renin and prorenin downregulate the expression of the (P)RR through a negative feedback system,26, 27 organ damage would develop via a (P)RR-independent mechanism under conditions with a simple increase in circulating prorenin level. Thus, HRP would have no effect on animal models with a simple increase in circulating prorenin level. However, enhanced mRNA expression of the (P)RR was observed in animal models with hypertension18, 19, 28 and heart failure,29 despite their high levels of renin and prorenin. Under these conditions, the (P)RR may be upregulated, overwhelming its negative feedback control and contributing to the pathogenesis of end-stage organ damage. Taken together, these results suggest that the activation of tissue prorenin by the (P)RR may be involved in the pathogenesis of end-stage organ damage in hypertension and heart failure, whereas the contribution of angiotensin II-independent, (P)RR-dependent signals to these conditions remains uncertain.
Genetic analyses in population studies
The (P)RR gene is located on chromosome Xp11.4 in humans,1 and chromosome Xp11 has been linked with diastolic blood pressure in a genome-wide association study.30 However, no reported information has suggested a relationship between the (P)RR and hypertension in humans. Recently, a population study showed a significant association between (P)RR gene polymorphisms and blood pressure levels in 1112 Japanese subjects.31 Although further genetic studies in different ethnic groups, longitudinal surveillance and a functional analysis are needed to confirm these findings, (P)RR gene polymorphisms may have a role in the regulation of blood pressure in humans.
Arterial mRNA levels in patients with stage 5 chronic kidney diseases
We recently assessed the mRNA expression of the (P)RR in the arteries of 141 patients with stage 5 chronic kidney diseases.32 The plasma prorenin levels in diabetic patients were significantly higher than those in non-diabetic patients. Nevertheless, arterial (P)RR expression was similar in diabetic and non-diabetic patients, suggesting that the negative feedback mechanism of the (P)RR observed in cultured cells26, 27 does not work in diabetic patients. In addition, multiple regression analyses showed a significant association with a large coefficient between the arterial mRNA level of the (P)RR and the arterial mRNA level of angiotensin-converting enzyme; this significant association disappeared in patients who had been treated with inhibitors of the renin–angiotensin system. In addition, the arterial mRNA level of the (P)RR was not associated with the arterial mRNA level of other angiotensin I-processing enzymes such as angiotensin-converting enzyme-2 and neprilysin. Thus, in the arteries of patients with stage 5 chronic kidney diseases, synchronized expression of (P)RR and angiotensin-converting enzyme may promote the generation of angiotensin II from angiotensinogen.
New insights into the (P)RR
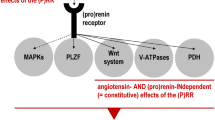
Cousin et al.33 recently showed that the (P)RR also exists as a soluble (P)RR. The truncated hydrophilic 28 kDa form is generated by furin cleavage in the trans-Golgi network and is secreted into the extracellular space. Although soluble (P)RR in the dialyzed human plasma containing a cocktail of protease inhibitors was precipitated with 100 nM His-tagged human renin,33 our preliminary study found soluble (P)RR in human urine but not in unmodified human plasma. In addition, an elevated circulating prorenin level did not cause organ damage in the rats overexpressing prorenin.24, 25 Thus, the majority of soluble (P)RRs may stay in the extracellular space, and only a few are present in the plasma probably because of digestion by plasma protease. If the prorenin-binding soluble (P)RR is enzymatically active, the presence of soluble (P)RR in renal extracellular space may explain why renal interstitial levels of angiotensin II are higher than plasma levels of angiotensin II. If soluble (P)RR in urine is derived from renal extracellular space, renal angiotensin II levels may be inferable by the determination of urinary soluble (P)RR levels in humans. Of interest, as shown in Figure 1, full-length (P)RR (39 kDa) is divided by furin cleavage to its soluble form (28 kDa) and the residual hydrophobic domains composed of ATPase accessory protein 2 (ATP6ap2, 8.9 kDa). Although the function of ATP6ap2 remains unknown, ATP6ap2 was reported to coprecipitate with the membrane sector of the vacuolar H+-ATPase (V-ATPase).34 As V-ATPase has an essential role in controlling the pH of secretory pathways,35 the (P)RR may have additional functions as ATP6ap2. Advani et al.9 recently showed that the (P)RR was co-localized with V-ATPase in α-intercalated cells of the distal nephron, and that the V-ATPase-specific inhibitor bafilomycin inhibited prorenin-induced ERK activation.
Processing of full-length (pro)renin receptor (fl(P)RR) to soluble (pro)renin receptor (soluble (P)RR) and ATPase 6 associated protein 2 (ATP6AP2), one of the proteins that binds vacuolar H+-ATPase (V-ATPase) in the trans-Golgi network. Both fl(P)RR and soluble (P)RR bind and activate prorenin, but only fl(P)RR is thought to exert its own intracellular signals.
In conclusion, numerous in vitro and in vivo studies have suggested possible roles of the (P)RR in diabetes and hypertension. Although genetic studies have also suggested a significant role of the (P)RR in patients, the (P)RR was recently shown to be cleaved into a soluble (P)RR and ATP6ap2 at the trans-Golgi network. Therefore, the complex functions of soluble (P)RR/ATP6ap2 must be analyzed at the protein level. In addition, the physiological roles of the (P)RR remain undetermined. As the construction of (P)RR null mice has not been successful, tissue-specific (pro)renin-receptor-knockout mice are required to elucidate the physiological roles of the full-length (P)RR, the soluble (P)RR and ATP6ap2.
Conflict of interest
The authors declare no conflict of interest.
References
Nguyen G, Delarue F, Burckle C, Bouzhir L, Giller T, Sraer J-D . Pivotal role of the renin/prorenin receptor in angiotensin II production and cellular responses to renin. J Clin Invest 2002; 109: 1417–1427.
Batenburg WW, Krop MK, Garrelds IM, deVries R, deBruin RJA, Burckle CA, Muller DN, Bader M, Nguyen G, Danser AHJ . Prorenin is the endogenous agonist of the (pro)renin receptor. Binding kinetics of renin and prorenin in rat vascular smooth muscle cells overexpressing the human (pro)renin receptor. J Hypertens 2007; 25: 2441–2453.
Nabi AHMN, Uddin M, Nakagawa T, Iwata H, Ichihara A, Inagami T, Suzuki F . Role of ‘handle’ region of prorenin prosegment in the non-proteolytic activation of prorenin by binding to membrane anchored (pro)renin receptor. Front Biosci 2007; 12: 4810–4817.
Huang Y, Noble N, Zhang J, Xu C, Border W . Renin-stimulated TGF-beta1 expression is regulated by a mitogen-activated protein kinase in mesangial cells. Kidney Int 2007; 72: 42–52.
Huang Y, Wongamorntham S, Kasting J, McQuillan D, Owens RT, Yu L, Noble NA, Border W . Renin increases mesangial cell transforming growth factor-b1 and matrix proteins through receptor-mediated, angiotensin II-independent mechanisms. Kidney Int 2006; 69: 105–113.
He M, Zhang L, Shao Y, Wang X, Huang Y, Yao T, Lu L . Inhibition of renin/prorenin receptor attenuated mesangial cell proliferation and reduced associated fibrotic factor release. Eur J Pharmacol 2009; 606: 155–161.
Sakoda M, Ichihara A, Kaneshiro Y, Takemitsu T, Nakazato Y, Migita T, Nabi AHMN, Nakagawa T, Suzuki F, Inagami T, Itoh H . The (pro)renin receptor-mediated activation of mitogen-activated protein kinases in human vascular smooth muscle cells. Hypertens Res 2007; 30: 1139–1146.
Saris J, ‘tHoen P, Garrelds I, Dekkers D, denDunnen J, Lamers J, JanDanser A . Prorenin induces intracellular signaling in cardiomyocytes independently of angiotensin II. Hypertension 2006; 48: 564–571.
Advani A, Kelly DJ, Cox AJ, White KE, Advani SL, Thai K, Connelly KA, Yuen D, Trogadis J, Herzenberg AM, Kuliszewski MA, Leong-Poi H, Gilbert RE . The (pro)renin receptor: site-specific and functional linkage to the vacuolar H+-ATPase in the kidney. Hypertension 2009; 54: 261–269.
Suzuki F, Hayakawa M, Nakagawa T, Nasir UM, Ebihara A, Iwasawa A, Ishida Y, Nakamura Y, Murakami K . Human prorenin has ‘gate and handle’ regions for its non-proteolytic activation. J Biol Chem 2003; 278: 22217–22222.
Nabi AHMN, Biswas KB, Nakagawa T, Ichihara A, Inagami T, Suzuki F . ‘Decoy peptide’ region (RIFLKRMPSI) of prorenin prosegment plays a crucial role in prorenin binding to the (pro)renin receptor. Int J Mol Med 2009; 24: 83–89.
Ichihara A, Hayashi M, Kaneshiro Y, Suzuki F, Nakagawa T, Tada Y, Koura Y, Nishiyama A, Okada H, Uddin MN, Nabi AHMN, Ishida Y, Inagami T, Saruta T . Inhibition of diabetic nephropathy by a decoy peptide corresponding to the ‘handle’ region for non-proteolytic activation of prorenin. J Clin Invest 2004; 114: 1128–1135.
Siragy HM, Huang J . Renal (pro)renin receptor upregulation in diabetic rats through enhanced angiotensin AT1 receptor and NADPH oxidase activity. Exp Physiol 2008; 93: 709–714.
Matavelli LC, Huang J, Siragy HM . (Pro)renin receptor contributes to diabetic nephropathy through enhancing renal inflammation. Clin Exp Pharmacol Physiol 2009 (e-pub ahead of print 21 September 2009; PMID: 19769609).
Takahashi H, Ichihara A, Kaneshiro Y, Inomata K, Sakoda M, Takemitsu T, Nishiyama A, Itoh H . Regression of nephropathy developed in diabetes by (pro)renin receptor blockade. J Am Soc Nephrol 2007; 18: 2054–2061.
Ichihara A, Suzuki F, Nakagawa T, Kaneshiro Y, Takemitsu T, Sakoda M, Nabi AHMN, Nishiyama A, Sugaya T, Hayashi M, Inagami T . Prorenin receptor blockade inhibits development of glomerulosclerosis in diabetic angiotensin II type 1a receptor deficient mice. J Am Soc Nephrol 2006; 17: 1950–1961.
Satofuka S, Ichihara A, Nagai N, Noda K, Ozawa Y, Fukamizu A, Tsubota K, Itoh H, Oike Y, Ishida S . (Pro)renin receptor-mediated signal transduction and tissue renin-angiotensin system contribute to diabetes-induced retinal inflammation. Diabetes 2009; 58: 1625–1633.
Ichihara A, Kaneshiro Y, Takemitsu T, Sakoda M, Nakagawa T, Nishiyama A, Kawachi H, Shimizu F, Inagami T . Contribution of non-proteolytically activated prorenin in glomeruli to hypertensive renal damage. J Am Soc Nephrol 2006; 17: 2495–2503.
Ichihara A, Kaneshiro Y, Takemitsu T, Sakoda M, Suzuki F, Nakagawa T, Nishiyama A, Inagami T, Hayashi M . Non-proteolytic activation of prorenin contributes to development of cardiac fibrosis in genetic hypertension. Hypertension 2006; 47: 894–900.
Susic D, Zhou X, Frohlich ED, Lippton H, Knight M . Cardiovascular effects of prorenin blockade in genetically hypertensive rats (SHR) on normal and high salt diet. Am J Physiol Heart Circ Physiol 2008; 295: H1117–H1121.
Muller DN, Klanke B, Feldt S, Cordasic N, Hartner A, Schmieder RE, Luft FC, Hilgers KF . (Pro)renin receptor peptide inhibitor ‘handle-region’ peptide does not affect hypertensive nephrosclerosis in Goldblatt rats. Hypertension 2008; 51: 676–681.
Feldt S, Maschke U, Dechend R, Luft FC, Muller DN . The putative (pro)renin receptor blocker HRP fails to prevent (pro)renin signaling. J Am Soc Nephrol 2008; 19: 743–748.
Nabi AHMN, Kageshima A, Uddin M, Nakagawa T, Park E, Suzuki F . Binding properties of rat prorenin and renin to the recombinant rat renin/prorenin receptor prepared by a baculovirus expression system. Int J Mol Med 2006; 18: 483–488.
Peters B, Grisk O, Becher B, Wanka H, Kuttler B, Ludemann J, Lorenz G, Rettig R, Mullins JJ, Peters J . Dose-dependent titration of prorenin and blood pressure in Cyp1a1ren-2 transgenic rats: absence of prorenin-induced glomerulosclerosis. J Hypertens 2008; 26: 102–109.
Mercure C, Prescott G, Lacombe M-J, Silversides DW, Reudelhuber TL . Chronic increases in circulating prorenin are not associated with renal or cardiac pathologies. Hypertension 2009; 53: 1062–1069.
Schefe J, Menk M, Reinemund J, Effertz K, Hobbs R, Pandolfi P, Ruiz P, Unger T, Funke-Kaiser H . A novel signal transduction cascade involving direct physical interaction of the renin/prorenin receptor with the transcription factor promyelocytic zinc finger protein. Circ Res 2006; 99: 1355–1366.
Schefe JH, Neumann C, Goebel M, Danser J, Kirsch S, Gust R, Kintscher U, Unger T, Funke-Kaiser H . Prorenin engages the (pro)renin receptor like renin and both ligand activities are unopposed by aliskiren. J Hypertens 2008; 26: 1787–1795.
Krebs C, Hamming I, Sadaghiani S, Steinmetz OM, Meyer-Schwesinger C, Fehr S, Stahl RAK, Garrelds IM, Danser AHJ, Goor Hv, Contrepas A, Nguyen G, Wenzel U . Antihypertensive therapy upregulates renin and (pro)renin receptor in the clipped kidney of Goldblatt hypertensive rats. Kidney Int 2007; 72: 725–730.
Hirose T, Mori N, Totsune K, Morimoto R, Maejima T, Kawamura T, Metoki H, Asayama K, Kikuya M, Ohkubo T, Kohzuki M, Takahashi K, Imai Y . Gene expression of (pro)renin receptor is upregulated in hearts and kidneys of rats with congestive heart failure. Peptides 2009; 30: 2316–2322.
Perola M, Kainulainen K, Pajukanta P, Terwilliger JD, Hiekkalinna T, Ellonen P, Kaprio J, Koskenvuo M, Kontula K, Peltonen L . Genome-wide scan of predisposing loci for increased diastolic blood pressure in Finnish siblings. J Hypertens 2000; 18: 1579–1585.
Hirose T, Hashimoto M, Totsune K, Metoki H, Asayama K, Kikuya M, Sugimoto K, Katsuya T, Ohkubo T, Hashimoto J, Rakugi H, Takahashi K, Imai Y . Association of (pro)renin receptor gene polymorphism with blood pressure in Japanese men: the Ohasama study. Am J Hypertens 2009; 22: 294–299.
Takemitsu T, Ichihara A, Kaneshiro Y, Sakoda M, Kurauchi-Mito A, Narita T, Kinouchi K, Yamashita N, Itoh H . Association of (pro)renin receptor mRNA expression with angiotensin-converting enzyme mRNA expression in human artery. Am J Nephrol 2009; 30: 361–370.
Cousin C, Bracquart D, Contrepas A, Corvol P, Muller L, Nguyen F . Soluble form of the (pro)renin receptor generated by intracellular cleavage by furin is secreted in plasma. Hypertension 2009; 53: 1077–1082.
Ludwig J, Kerscher S, Brandt U, Pfeiffer K, Getlawi F, Apps DK, Schagger H . Identification and characterization of a novel 9.2-kDa membrane sector-associated protein of vacuolar proton-ATPase from chromaffin granules. J Biol Chem 1998; 273: 10939–10947.
Paroutis P, Touret N, Grinstein S . The pH of the secretory pathway: measurement, determinants, and regulation. Physiology 2004; 19: 207–215.
Acknowledgements
We thank Ms Miki Chika for her skilful secretarial assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ichihara, A., Sakoda, M., Kurauchi-Mito, A. et al. Possible roles of human (pro)renin receptor suggested by recent clinical and experimental findings. Hypertens Res 33, 177–180 (2010). https://doi.org/10.1038/hr.2009.214
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2009.214
Keywords
This article is cited by
-
Atp6ap2 ablation in adult mice impairs viability through multiple organ deficiencies
Scientific Reports (2017)
-
Significant roles of the (pro)renin receptor in integrity of vascular smooth muscle cells
Hypertension Research (2014)
-
The (pro)renin receptor. A decade of research: what have we learned?
Pflügers Archiv - European Journal of Physiology (2013)
-
Potential cross-talk between (pro)renin receptors and Wnt/frizzled receptors in cardiovascular and renal disorders
Hypertension Research (2011)
-
Antihypertensive Therapy in Diabetes: The Legacy Effect and RAAS Blockade
Current Hypertension Reports (2011)