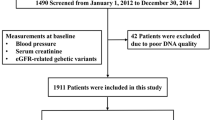
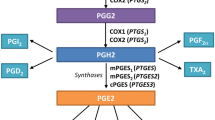
Abstract
Resistant hypertension (RH) is the maintenance of elevated blood pressure concurrent with the use of three different anti-hypertensive drugs, one of which is a diuretic. The Renin-Angiotensin-Aldosterone System plays a major role in volume-dependent hypertension. Therefore, its components are interesting targets for genetic association studies. This work focused on the −344 C/T polymorphism in the CYP11b2 gene, which encodes aldosterone synthase. This work evaluates the association between T allele and resistance to anti-hypertensive treatment. Genotyping analysis included 88 subjects with RH, 142 who were responsive to anti-hypertensive treatment and 110 subjects as a control group. Plasmatic concentrations of aldosterone, renin and cortisol, carotid intima-media thickness and carotid-femoral pulse wave velocity were assessed in a smaller subset of hypertensive patients. An association was found between T allele and hypertension (P<0.005), but there was no difference in allele frequencies between both hypertensive groups. There was no difference in plasmatic parameters either, in remodeling indicators between the genotypic groups.
Similar content being viewed by others
Introduction
Hypertension is one of the most important issues in public health care, and is associated with increased morbidity and mortality, mainly through its secondary consequences.
Resistant (or refractory) hypertension (RH) is defined as the maintenance of high blood pressure (140/80 mm Hg for systolic–diastolic arterial pressure, respectively; 130/80 in diabetics), concurrent with the use of three different anti-hypertensive drugs (one of which is a diuretic) in optimized doses, with a high compliance of the patient to treatment.1 One of the probable causes of resistance to anti-hypertensive treatment is the maintenance of an increased intravascular volume, even using diuretics, and, therefore, the Renin-Angiotensin-Aldosterone System may have a pivotal role to play in this phenomenon.2 Among the genes that participate in this system, the gene that encodes aldosterone synthase (CYP11b2) is an interesting target for genetic association studies, as this enzyme is responsible for the final step of aldosterone synthesis in justaglomerular cells.3 Several studies focused on the −344C/T polymorphism, which is located in the promoter of this gene, in a region where the transcription factor, steroidogenic factor-1, binds to the promoter.4 This polymorphism could affect CYP11b2 expression, and indirectly aldosterone release. Although there are some discordant reports, most of the studies link the T allele to detrimental effects in hypertensive subjects.3, 5, 6, 7 Moreover, there is an association between the T allele and higher plasma aldosterone levels in subjects with a high salt load.8
Higher levels of aldosterone are correlated to hazardous effects on the cardiovascular system: higher arterial stiffness, assessed through carotid-femoral pulse wave velocity (PWV),9 and higher carotid intima-media thickness (IMT),10 both parameters considered as predictive factors for cardiovascular outcomes.11, 12 Furthermore, two recent studies evaluating mineralocorticoid antagonists showed benefits that cannot be explained merely by the reduction in plasma volume through aldosterone blockade13, 14 It has been shown that aldosterone has a synergic effect with angiotensin II on vascular smooth muscle cells growth; therefore, it can act directly on cardiovascular remodeling in noncontrolled hypertensive patients.15
This study aims to assess the relationship between T allele and the pharmacological resistance to anti-hypertensive treatment. In addition, this study also investigates the possible physiological alterations associated with genotypic influence on aldosterone release, such as plasmatic aldosterone, renin and cortisol; carotid IMT and carotid-femoral PWV.
Methods
In this study, we included 340 subjects, 88 of whom had RH, 140 were responsive to anti-hypertensive treatment (RT) and 110 were healthy controls, using the JNC 7 criteria.1 To investigate the genetic influence on physiological parameters, we studied a smaller subset of patients, 36 of whom were RT and 42 RH, who were divided according to genotypes. Briefly, the inclusion criterion for the RH group was uncontrolled hypertension (systolic, SBP, and diastolic, DBP, blood pressures higher than 140 mm Hg and 80 mm Hg, respectively) concurrent with the use of three different anti-hypertensive drugs (among them is a diuretic) in optimal doses, with a high patient compliance to the treatment. The inclusion criterion for the RT group was controlled hypertension with up to three different anti-hypertensive drugs. The control group was defined as subjects with SBP and DBP below 140 mm Hg and 80 mm Hg, respectively, with no familial history of cardiovascular diseases. All patients had, at least 6 months of follow-up, were compliant to treatment, and had signed the informed consent form. The exclusion criteria were concurrent cardiovascular, hepatic or renal diseases, drug abuse and noncompliance of the patient to pharmacological treatment. This work was approved by the Human Research Ethics Committee at the State University of Campinas.
Blood pressure was assessed by a calibrated sphygmomanometer with a mercury column, in a calm and quiet room, after 15 min of resting time in sitting position. Patients were instructed to abstain from nicotine and caffeine for at least 60 min before blood pressure measurements; and at least 12 h before IMT and PWV exams. All subjects with high blood pressure had the diagnosis confirmed by 24 h ambulatory blood pressure monitoring. Blood samples were collected after a 12 h fasting period between 0800 and 0900 h for laboratory examinations and for DNA extraction. Patient compliance was assessed by counting the tablets,16 and 0.8 was the minimum value accepted for the administered/prescription tablets rate. IMT was assessed by a high-resolution ultra-sound using the Powervision 6000 (Toshiba, Japan) equipment, and PWV was determined using the Complior SP (Artech Medical, France) equipment, both following the manufacturer's protocols. DNA was extracted using the salting-out method.
Genotyping of CYP11b2 −344C/T polymorphism was carried out using the restriction fragment length polymorphism method. Polymerase chain reaction (PCR) was carried out with primers forward (5′- AGG CGT GGG GTC TGG ACT – 3′) and reverse (5′- GTG TCA GGG CAG GGG GTA – 3′), using the following steps: initial denaturation of 3 min at 94 °C, 30 cycles of denaturation (1 min at 93 °C), annealing (1 min at 68 °C) and extension (1 min at 72 °C) and a final extension step of 7 min at 72 °C. The amplified PCR product (228 pb) was then digested with an HaeIII endonuclease (New England Biolabs, USA) for 2 h at 37 °C. The digestion product was separated finally by electrophoresis using a 3% METAPHOR agarose gel (Lonza, USA). The C allele of −344C/T polymorphism creates a new restriction site, hence C homozygous (CC) individuals will generate three fragments (106, 69 and 53 pb), T homozygous (TT) individuals will generate two fragments (175 and 53 pb), and heterozygous (CT) individuals will generate four fragments (175, 106, 69 and 53 pb). Figure 1 shows a digestion example.
Restriction fragment length polymorphism of the CYP11b2 gene. High-resolution agarose gel (3% w/v) stained with ethidium bromide. Column A: ladder (50 pb). Column B: polymerase chain reaction (PCR) product not digested. Columns D and G: digested product; TT homozygous. Columns C, E, F and H: digested product, CT heterozygous. The sizes of the fragments are indicated on both sides of the gel.
Statistical analysis was performed as follows: Allelic and genotypic distributions were expressed as frequencies, and were compared using the chi-squared method. Numerical parameters were expressed as mean±s.d.; when comparing three groups, the test used was one-way ANOVA with Tukey's post test; when comparing two groups, the Student's t-test was used. P<0.005 was considered as statistically significant.
Results
The characteristics of the groups are shown in Table 1.
Genotypic and allelic frequencies are presented in Figures 2 and 3, respectively. All genotypic distributions were in the Hardy–Weinberg equilibrium (P=1 for the control group; P=0.7370 for RT group and P=0.7919 for RH group).
Genotypic frequencies of −344C/T polymorphism on the CYP11b2 gene in control, responsive to anti-hypertensive treatment (RT) and resistant hypertension (RH) groups. There is statistical difference between control and RT (P=0.0221) and between control and RH (P=0.0448) groups. There is no difference between RT and RH groups (P=0.3079).
Allelic frequencies of −344C/T polymorphism on the CP11b2 gene in control, responsive to anti-hypertensive treatment (RT) and resistant hypertension (RH) groups. There is statistical difference between control and RT (P=0.0094) and between control and RH (P=0.0174) groups. There is no difference between RT and RH groups (P=0.9272).
A smaller subset of the hypertensive patients (36 RT and 42 RH) was divided as CC, CT and TT genotype carriers to assess the genetic influence on plasmatic aldosterone, renin, cortisol and in remodeling indicators PWV and IMT (Table 2).
Discussion
Two important findings reported here are the following: T allele of −344C/T polymorphism in the CYP11b2 gene is more frequent in both hypertensive groups when compared with control groups, thus suggesting that this allele is associated with hypertension. The second important result is that there is no difference in T allele frequency when hypertensives that respond to treatment and those that are resistant are compared, thus suggesting that this allele is not linked to resistance to anti-hypertensive treatment.
Besides the association with hypertension phenotype, we found no alteration in plasmatic aldosterone in T allele carriers (CT and TT genotypes) compared with that in noncarriers. Low salt load in alimentation was used as one of the nonpharmacological approaches to the treatment of all hypertensive subjects. As the maintenance of high salt load stimulates aldosterone release, this may obscure the genetic influence of the T allele on plasmatic aldosterone in the studied subjects. Iwai and colleagues8 found increased plasmatic aldosterone in T carriers with a high salt intake,which strengthens this hypothesis.
Once the aldosterone concentration was not augmented in T allele carriers, no subsequent alteration was expected to appear in PWV and IMT in CT and TT genotypic groups, as it indeed happened. It is interesting to observe that there is a clear association between RH and increases in IMT, as our group has earlier reported.17 However, the T allele of aldosterone synthase did not affect this parameter, as we have reported here. Probably this allele influences acute aldosterone release; thus not reflecting the maintenance of high plasmatic aldosterone levels in the absence of a high salt load.
This study did not reproduce the results reported by Freel and colleagues.3 They hypothesized that the T allele of the CYP11b2 gene would be in linkage disequilibrium with another unknown genetic factor in CYP11b1, which controls cortisol production. In that study, the T allele in CYP11b2 was linked to higher plasmatic cortisol concentrations, thus leading to a higher adrenocorticotropic hormone (ACTH) drive, and indirectly to augmented aldosterone plasmatic concentrations. In this study, however, neither aldosterone nor cortisol was augmented in CT and TT groups. The biochemical mechanism behind the influence of T allele of the studied polymorphism on hypertension has yet to be elucidated, especially in individuals with controlled salt load.
An important feature of this study is that resistant hypertensive subjects have been extensively well characterized. All confounding factors such as heavy smoking, alcohol abuse, noncompliance to the pharmacological treatment and secondary causes of hypertension have been thoroughly investigated. The three genotyped groups had similar characteristics, and although there were some differences in black and white frequencies in the RT group, our control group matched the RH group adequately. In addition, the subset of patients who were used to assess the genetic influence on physiological parameters showed, between groups, differences only in those parameters that were really expected to show differences, such as blood pressure, IMT and the number of anti-hypertensive drugs used (not shown).
As a limitation of this study, we should mention the small number of subjects in the RH group, both for genotyping, and for physiological assessment. The difficulty in achieving a larger group of RH subjects is the long duration of follow-up that is required for a reliable diagnosis. Moreover, we had some differences in the body mass index (BMI) on RT and RH groups. However, these differences have been neutralized in the smaller subset of patients used for physiological study.
Conflict of interest
None.
References
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo Jr JL, Jones DW, Materson BJ, Oparil S, Wright Jr JT, Roccella EJ . The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA 2003; 289: 2560–2572.
Gaddam KK, Nishizaka MK, Pratt-Ubunama MN, Pimenta E, Aban I, Oparil S, Calhoun DA . Characterization of resistant hypertension: association between resistant hypertension, aldosterone, and persistent intravascular volume expansion. Arch Intern Med 2008; 168: 1159–1164.
Freel EM, Ingram M, Friel EC, Fraser R, Brown M, Samani NJ, Caulfield M, Munroe P, Farrall M, Webster J, Clayton D, Dominiczak AF, Davies E, Connell JM . Phenotypic consequences of variation across the aldosterone synthase and 11-beta hydroxylase locus in a hypertensive cohort: data from the MRC BRIGHT Study. Clin Endocrinol (Oxf) 2007; 67: 832–838.
White PC, Slutsker L . Haplotype analysis of CYP11B2. Endocr Res 1995; 21: 437–442.
Freitas SR, Cabello PH, Moura-Neto RS, Dolinsky LC, Lima AB, Barros M, Bittencourt I, Cordovil IL . Analysis of renin-angiotensin-aldosterone system gene polymorphisms in resistant hypertension. Braz J Med Biol Res 2007; 40: 309–316.
Hilgers KF, Schmidt BM . Gene variants of aldosterone synthase and hypertension. J Hypertens 2005; 23: 1957–1959.
Davies E, Holloway CD, Ingram MC, Inglis GC, Friel EC, Morrison C, Anderson NH, Fraser R, Connell JM . Aldosterone excretion rate and blood pressure in essential hypertension are related to polymorphic differences in the aldosterone synthase gene CYP11B2. Hypertension 1999; 33: 703–707.
Iwai N, Kajimoto K, Tomoike H, Takashima N . Polymorphism of CYP11B2 determines salt sensitivity in Japanese. Hypertension 2007; 49: 825–831.
Park S, Kim JB, Shim CY, Ko YG, Choi D, Jang Y, Chung N . The influence of serum aldosterone and the aldosterone-renin ratio on pulse wave velocity in hypertensive patients. J Hypertens 2007; 25: 1279–1283.
Holaj R, Zelinka T, Wichterle D, Petrak O, Strauch B, Widimsky Jr J . Increased intima-media thickness of the common carotid artery in primary aldosteronism in comparison with essential hypertension. J Hypertens 2007; 25: 1451–1457.
Boutouyrie P, Tropeano AI, Asmar R, Gautier I, Benetos A, Lacolley P, Laurent S . Aortic stiffness is an independent predictor of primary coronary events in hypertensive patients: a longitudinal study. Hypertension 2002; 39: 10–15.
Laurent S, Cockcroft J, Van Bortel L, Boutouyrie P, Giannattasio C, Hayoz D, Pannier B, Vlachopoulos C, Wilkinson I, Struijker-Boudier H . Expert consensus document on arterial stiffness: methodological issues and clinical applications. Eur Heart J 2006; 27: 2588–2605.
Pitt B, Zannad F, Remme WJ, Cody R, Castaigne A, Perez A, Palensky J, Wittes J . The effect of spironolactone on morbidity and mortality in patients with severe heart failure. Randomized Aldactone Evaluation Study Investigators. N Engl J Med 1999; 341: 709–717.
Pitt B, Remme W, Zannad F, Neaton J, Martinez F, Roniker B, Bittman R, Hurley S, Kleiman J, Gatlin M . Eplerenone, a selective aldosterone blocker, in patients with left ventricular dysfunction after myocardial infarction. N Engl J Med 2003; 348: 1309–1321.
Schiffrin EL . Effects of aldosterone on the vasculature. Hypertension 2006; 47: 312–318.
Taylor DW, Sackett DL, Haynes RB, Johnson AL, Gibson ES, Roberts RS . Compliance with antihypertensive drug therapy. Ann NY Acad Sci 1978; 304: 390–403.
Cittadino M, Goncalves de Sousa M, Ugar-Toledo JC, Rocha JC, Tanus-Santos JE, Moreno Jr H . Biochemical endothelial markers and cardiovascular remodeling in refractory arterial hypertension. Clin Exp Hypertens 2003; 25: 25–33.
Acknowledgements
We would like to sincerely thank Leoní Adriana de Souza and Samira Ubaid Girioli for their inestimable contribution to the studied patient's health care. Financial Support: Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP), Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), and Coordenadoria de Aperfeiçoamento de Pessoal de Nível Superior (CAPES).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lacchini, R., Sabha, M., Coeli, F. et al. T allele of −344C/T polymorphism in aldosterone synthase gene is not associated with resistant hypertension. Hypertens Res 32, 159–162 (2009). https://doi.org/10.1038/hr.2008.36
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2008.36
Keywords
This article is cited by
-
Controlled Versus Uncontrolled Resistant Hypertension: Are They in the Same Bag?
Current Hypertension Reports (2018)