Abstract
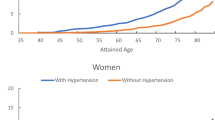
Family history and aging are independent risk factors for the development of hypertension as well as for the development of diabetes. However, it is unclear how the family histories influence the rate of age-associated increase in these diseases. Moreover, despite the fact that hypertension and diabetes often occur concomitantly, it is not known whether family history of hypertension increases the risk of diabetes or vice versa. To gain an insight into these questions, we investigated the cross-sectional prevalence and family history of hypertension and diabetes in 1,123 male subjects (mean age, 42.1±12 years; range, 20–60 years) who participated in annual medical check-ups. The data were analyzed by 10-year age groups (20s, 30s, 40s and 50s). The prevalence of hypertension increased with age group either in the absence (12% in the 20s and 39% in the 50s) or in the presence (21% in the 20s and 59% in the 50s) of family history of hypertension, and thus the increasing rate of prevalence with age was not affected by family history. The prevalence of diabetes in the absence of family history of diabetes was low until the 40s (<1.2%) but it jumped in the 50s (4.3%). On the other hand, in the presence of family history, the prevalence was 4% in the 20s and progressively increased to 20% in the 50s. The impact of family history on the risk of diabetes was strong and appeared to increase with age. Family history of hypertension did not increase the risk of diabetes, and family history of diabetes did not increase the risk of hypertension. These results suggest that family history of hypertension has an additive impact on the age-associated increase in the risk of hypertension, whereas family history of diabetes has an exponential impact on aging-associated increase in the risk of diabetes.
Similar content being viewed by others
Article PDF
References
Rebbeck TR, Turner ST, Sing CF : Probability of having hypertension: effects of sex, history of hypertension in parents, and other risk factors. J Clin Epidemiol 1996; 49: 727–734.
Burke GL, Savage PJ, Sprafka JM, et al: Relation of risk factor levels in young adulthood to parental history of disease. The CARDIA study. Circulation 1991; 84: 1176–1187.
Grill V, Persson G, Carlsson S, et al: Family history of diabetes in middle-aged Swedish men is a gender unrelated factor which associates with insulinopenia in newly diagnosed diabetic subjects. Diabetologia 1999; 42: 15–23.
Bao W, Srinivasan SR, Wattigney WA, Berenson GS : The relation of parental cardiovascular disease to risk factors in children and young adults: the Bogalusa Heart Study. Circulation 1995; 91: 365–371.
Tozawa M, Oshiro S, Iseki C, et al: Family history of hypertension and blood pressure in a screened cohort. Hypertens Res 2001; 24: 93–98.
Fujishima M, Kiyohara Y, Kato I, et al: Diabetes and cardiovascular disease in a prospective population survey in Japan: the Hisayama Study. Diabetes 1996; 45 ( Suppl 3): S14–S16.
Vlasakova Z, Pelikanova T, Karasova L, Skibova J : Insulin secretion, sensitivity, and metabolic profile of young healthy offspring of hypertensive parents. Metabolism 2004; 53: 469–475.
Hirose H, Saito I, Kawabe H, Saruta T : Insulin resistance and hypertension: seven-year follow-up study in middle-aged Japanese men (the KEIO study). Hypertens Res 2003; 26: 795–800.
Eckel RH, Grundy SM, Zimmet PZ : The metabolic syndrome. Lancet 2005; 365: 1415–1428.
Ishizaka N, Ishizaka Y, Toda E, Hashimoto H, Nagai R, Yamakado M : Hypertension is the most common component of metabolic syndrome and the greatest contributor to carotid arteriosclerosis in apparently healthy Japanese individuals. Hypertens Res 2005; 28: 27–34.
Kuzuya T, Nakagawa S, Satoh J, et al: Report of the Committee on the Classification and Diagnostic Criteria of Diabetes Mellitus. Diabetes Res Clin Pract 2002; 55: 65–85.
Stamler R, Stamler J, Riedlinger WF, Algera G, Roberts RH : Family (parental) history and prevalence of hypertension. Results of a nationwide screening program. JAMA 1979; 241: 43–46.
Sumino H, Ichikawa S, Kumakura H, et al: Effects of hormone replacement therapy on office and ambulatory blood pressure in Japanese hypertensive postmenopausal women. Hypertens Res 2003; 26: 369–376.
Kuzuya T : Prevalence of diabetes mellitus in Japan compiled from literature. Diabetes Res Clin Pract 1994; 24 ( Suppl): S15–S21.
Knowler WC, Pettitt DJ, Savage PJ, Bennett PH : Diabetes incidence in Pima indians: contributions of obesity and parental diabetes. Am J Epidemiol 1981; 113: 144–156.
Staessen JA, Celis H, Fagard R : The epidemiology of the association between hypertension and menopause. J Hum Hypertens 1998; 12: 587–592.
Pyke DA, Nelson PG : Diabetes mellitus in identical twins, in Creutzfeldt W ( ed): The Genetics of Diabetes Mellitus. Berlin, Springer-Verlag, 1976, pp 194–205.
Pimenta W, Korytkowski M, Mitrakou A, et al: Pancreatic beta-cell dysfunction as the primary genetic lesion in NIDDM. Evidence from studies in normal glucose-tolerant individuals with a first-degree NIDDM relative. JAMA 1995; 273: 1855–1861.
Nakanishi N, Suzuki K, Tatara K : Serum γ-glutamyltransferase and risk of metabolic syndrome and type 2 diabetes in middle-aged Japanese men. Diabetes Care 2004; 27: 1427–1432.
Kubo M, Kiyohara Y, Kato I, et al: Trends in the incidence, mortality, and survival rate of cardiovascular disease in a Japanese community: the Hisayama Study. Stroke 2003; 34: 2349–2354.
Wang Z, Wu Y, Zhao L, Li Y, Yang J, Zhou B : Trends in prevalence, awareness, treatment and control of hypertension in the middle-aged population of China, 1992–1998. Hypertens Res 2004; 27: 703–709.
Burt VL, Whelton P, Roccella EJ, et al: Prevalence of hypertension in the US adult population: results from the Third National Health and Nutrition Examination Survey, 1988–1991. Hypertension 1995; 25: 305–313.
Ohkubo T, Obara T, Funahashi J, et al: Control of blood pressure as measured at home and office, and comparison with physicians' assessment of control among treated hypertensive patients in Japan: first report of the Japan Home versus Office Blood Pressure Measurement Evaluation (J-HOME) study. Hypertens Res 2004; 27: 755–763.
Society for Cardiovascular Disease Prevention, Ministry of Health, Labour, and Welfare, Japan : Dai 5ji Junkanki Shikkan Kiso Kenkyu Kekka (Summary of the Fifth National Survey on Cardiovascular Disease: Full Coverage of the Results of Fifth National Survey of Cardiovascular Survey), Tokyo, Chuo-Hoki Shuppan, 2002, pp 291–295 ( in Japanese).
Sekikawa A, Eguchi H, Tominaga M, et al: Prevalence of type 2 diabetes mellitus and impaired glucose tolerance in a rural area of Japan: the Funagata diabetes study. J Diabetes Complicat 2000; 14: 78–83.
The Diabetes Prevention Program Research Group: Strategies to identify adults at high risk for type 2 diabetes: the Diabetes Prevention Program. Diabetes Care 2005; 28: 138–144.
Iseki K, Oshiro S, Tozawa M, Ikemiya Y, Fukiyama K, Takishita S : Prevalence and correlates of diabetes mellitus in a screened cohort in Okinawa, Japan. Hypertens Res 2002; 25: 185–190.
Ohmura T, Ueda K, Kiyohara Y, et al: Prevalence of type-2 (non-insulin-dependent) diabetes-mellitus and impaired glucose-tolerance in the Japanese general-population—the Hisayama Study. Diabetologia 1993; 36: 1198–1203.
Health and Welfare Statistics Association, Japan : Kokumin-Eisei No Doukou. J Health Welfare Stat 2005; 52 ( Suppl 9): 142 ( in Japanese).
Cruz ML, Weigensberg MJ, Huang TTK, Ball G, Shaibi GQ, Goran MI : The metabolic syndrome in overweight Hispanic youth and the role of insulin sensitivity. J Clin Endocrinol Metab 2004; 89: 108–113.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shirakawa, T., Ozono, R., Kasagi, F. et al. Differential Impact of Family History on Age-Associated Increase in the Prevalence of Hypertension and Diabetes in Male Japanese Workers. Hypertens Res 29, 81–87 (2006). https://doi.org/10.1291/hypres.29.81
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1291/hypres.29.81
Keywords
This article is cited by
-
Comparison of the effects of sibling and parental history of type 2 diabetes on metabolic syndrome
Scientific Reports (2020)
-
BMI better explains hypertension in Chinese senior adults and the relationship declines with age
Aging Clinical and Experimental Research (2015)
-
Central obesity is important but not essential component of the metabolic syndrome for predicting diabetes mellitus in a hypertensive family-based cohort. Results from the Stanford Asia-pacific program for hypertension and insulin resistance (SAPPHIRe) Taiwan follow-up study
Cardiovascular Diabetology (2012)
-
Analysis of various etiologies of hypertension in patients hospitalized in the endocrinology division
Endocrine (2012)