Abstract
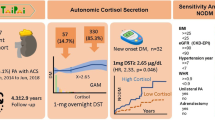
The present prospective observational study was designed to assess the prevalence of hemodialysis in type 2 diabetic patients with an impairment of plasma aldosterone responsiveness to adrenocorticotropic hormone (ACTH). Sixty seven patients (43 men and 24 women) were selected. The inclusion criteria were age <65 years; presence of normoalbuminemia (serum albumin>3.6 g/dl); and absence of azotemia (serum creatinine≤1.2 mg/dl in males, and ≤1.0 mg/dl in females). Soluble α1–24-ACTH was injected intramuscularly in a single dose of 0.25 mg after overnight recumbency. The area under the aldosterone curve (aldosterone AUC) was calculated. The diabetic patients were divided into two groups according to the levels of aldosterone AUC. Patients with an aldosterone AUC in the range of 0–381 were considered poor responders (n=31) and those with an AUC of 397–1,007 were considered good responders (n=36). The follow-up was performed during a 144-month period. The end point of the study was the introduction of hemodialysis. A total of 14 patients (12 poor responders and 2 good responders; p<0.001) were introduced to hemodialysis. The prevalence of hemodialysis in the poor responders (5.74 per 100 patient-years) was significantly higher (p<0.001, log-rank test) than that in the good responders (0.68 per 100 patient-years). One possible explanation is that an inappropriate level of salt intake relative to the impaired plasma aldosterone control may have contributed to the high prevalence of risks and hemodialysis in the poor responders.
Similar content being viewed by others
Article PDF
References
DeChatel R, Weidmann P, Flammer J, et al : Sidium, renin, aldosterone, catecholamines, and blood pressure in diabetes mellitus. Kidney Int 1977; 12: 412– 421.
Beretta-Piccoli C, Weidmann P, Keusch G : Responsiveness of plasma renin and aldosteronein diabetes mellitus. Kidney Int 1981; 20: 259– 266.
Tuck ML, Mayes DM : Mineralocorticoid biosynthesis in patients with hyporeninemic hypoaldosteronism. J Clin Endocrinol Metab 1980; 50: 341– 347.
Perez GO, Lespier L, Jacobi J, Oster JR, Katz FH : Hyporeninemia and hypoaldosteronism in diabetes mellitus. Arch Intern Med 1977; 137: 852– 855.
DeFronzo RA : Hyperkaremia and hyporeninemic hypoaldosteronism. Kidney Int 1980; 17: 118– 134.
Iwasaki R, Kigoshi T, Uchida K, Morimoto S : Plasma 18-hydroxycorticosterone and aldosterone responses to angiotensin II and corticotropin in diabetic patients with hyporeninemic and normoreninemic hypoaldosteronism. Acta Endocrinol (Copenh) 1989; 121: 83– 89.
Kigoshi T, Morimoto S, Uchida K, et al : Unresponsiveness of plasma mineralocorticoids to angiotensin II in diabetic patients with asymptomatic normoreninemic hypoaldosteronism. J Lab Clin Med 1985; 105: 195– 200.
Muller J : Regulation of Aldosterone Biosynthesis. Heidelberg, Springer-Verlag, 1988, pp 110– 112.
Kigoshi T, Iwasaki R, Kaneko M, et al : Lack of enhanced responsiveness of plasma 18-hydroxycorticosterone and aldosterone to adrenocorticotropin as well as to angiotensin-II during moderate sodium depletion in type II diabetic subjects with normoreninemia. J Clin Endocrinol Metab 1991; 72: 1200– 1205.
Allison DB, Paultre F, Maggio C, Mezzitis N, Pi-Sunyer FX : The use of area under curves in diabetes research. Diabetes Care 1995; 18: 245– 250.
Messerli FH, Weidmann P, DeChatel R, Maxwell MH : Responsiveness of plasma aldosterone dependency upon basal secretory activity. Klin Wochenschr 1978; 56: 719– 726.
Morimoto S, Takeda R, Uchida K, et al : Reduced aldosterone secretory response to acute ACTH stimulation in sodium restricted elderly subjects. J Am Geriatr Soc 1980; 28: 361– 366.
Walker WG : Hypertension-related renal injury: a major contributor to end-stage renal disease. Am J Kidney Dis 1993; 22: 164– 173.
Ibrahim HN, Rosenberg ME, Hostetter TH : Role of the renin-angiotensin-aldosterone system in the progression of renal disease: a critical review. Semin Nephrol 1997; 17: 431– 440.
Damsgaard EM, Floland A, Jorgensen OD, Mogensen CE : Prognostic value of urinary albumin excretion rate and other risk factors in elderly diabetic patients and non-diabetic control subjects surviving the first 5 years after assessment. Diabetologia 1993; 36: 1030– 1036.
Zimpelmann J, Kumar D, Levine DZ, et al : Early diabetes mellitus stimulates proximal tubule renin mRNA expression in the rat. Kidney Int 2000; 58: 2320– 2330.
Tojo A, Onozato ML, Kurihara H, Sakai T, Goto A, Fujita T : Angiotensin II blockade restores albumin reabsorption in the proximal tubules of diabetic rats. Hypertens Res 2003; 26: 413– 419.
Sato A, Saruta T : Aldosterone-induced organ damage: plasma aldosterone level and inappropriate salt status. Hypertens Res 2004; 27: 303– 310.
Wakisaka M, Spiro MJ, Spiro RG : Synthesis of type VI collagen by cultured glomerular cells and comparison of its regulation by glucose and other factors with that of type IV collagen. Diabetes 1994; 43: 95– 103.
Hironaka K, Makino H, Ota Z : Renal basement membranes by ultrahigh resolution scanning electron microscopy. Kidney Int 1993; 43: 334– 345.
Makino H, Shikata K, Hironaka K, et al : Ultrastructure of nonenzymatically glycated mesangial matrix in diabetic nephropathy. Kidney Int 1995; 48: 517– 526.
Jin DK, Fish AJ, Wayner EA, et al : Distribution of integrin subunits in human diabetic kidneys. J Am Soc Nephrol 1996; 7: 2636– 2645.
Rocha R, Stier CT Jr, Kifor I, et al : Aldosterone: a mediator of myocardial necrosis and renal arteriopathy. Endocrinology 2000; 141: 3871– 3878.
Brilla CG, Weber KT : Reactive and reparative myocardial fibrosis in arterial hypertension in the rat. Cardiovasc Res 1992; 26: 671– 677.
Schlaich MP, Schobel HP, Hilgers K, et al : Impact of aldosterone on left ventricular structure and function in young normotensive and mild hypertensive subjects. Am J Cardiol 2000; 85: 1199– 1206.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kigoshi, T., Uehara, K., Furuya, K. et al. Relationship between Impaired Aldosterone Response to Adrenocorticotropic Hormone and Prevalence of Hemodialysis in Type 2 Diabetic Patients without Azotemia. Hypertens Res 28, 21–26 (2005). https://doi.org/10.1291/hypres.28.21
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1291/hypres.28.21