Abstract
Purpose:
Population-based reflex testing of colorectal tumors can identify individuals with Lynch syndrome (LS), but there is debate regarding the type of patient discretion such a program warrants. We examined health-care providers’ views and experiences to inform the design of a reflex-testing program and their perspectives regarding an opt-out option.
Methods:
We interviewed providers managing LS or colorectal cancer patients, including surgeons, genetic counselors, oncologists, primary-care physicians, and gastroenterologists. Qualitative data were analyzed thematically using constant comparison techniques.
Results:
Providers supported a reflex-testing program because of the current lack of coordinated immunohistochemistry (IHC) testing and underascertainment of LS patients as well as the opportunity to standardize the increasing use of genomic tests in practice. Most supported an opt-out after reflex testing because they felt that IHC is akin to other pathology tests, which are not optional. Some favored an opt-out before testing because of concern for patients experiencing distress, insurance discrimination, or a diagnostic odyssey that may be inconclusive.
Conclusion:
Providers support a reflex-testing program to improve the identification and management of suspected LS patients. However, how to support meaningful information provision to enable an opt-out without jeopardizing testing uptake and the anticipated public health benefits remains a policy challenge.
Genet Med advance online publication 06 October 2016
Similar content being viewed by others
Introduction
Lynch syndrome (LS) is the most commonly inherited colon cancer syndrome, accounting for 3–5% of colorectal cancer (CRC) cases.1 LS is caused by inherited defects in DNA mismatch repair genes MLH1, MSH2, MSH6, and PMS2. LS mutation carriers are at increased lifetime risk for several cancers, including 12–48% risk of CRC and 15–54% risk of endometrial cancer, depending on the gene and mutation carried.2,3,4 When detected early, as stage I CRC, an estimated 90% of people with CRC will survive.5 Early detection and surveillance can reduce CRC incidence and all-cause mortality in gene mutation carriers.6,7 Guidelines recommend colonoscopies every 1–2 years starting at age 20–25.8 Reflex testing for LS in patients can benefit relatives; large-scale surveillance programs of affected families has led to a 62% reduction in the incidence of CRC and a 65–70% decrease in mortality.6
Traditionally, patients at risk for LS were identified by clinical criteria such as the Bethesda Guidelines or Amsterdam Criteria.9 These rely on clinicians obtaining a detailed family history but have been shown to have low sensitivity, are burdensome, and have been poorly implemented in clinical practice.9,10,11,12,13 In 2009, the Evaluation of Genomic Applications in Practice and Prevention (EGAPP) working group recommended that the surgical specimens of all newly diagnosed patients with CRC be reflexively tested for LS through microsatellite instability (MSI) testing or immunohistochemistry (IHC) (“reflex testing”), which, when coupled with mutation testing and surveillance in the index patient and relatives, is associated with reduced morbidity and mortality.14,15 EGAPP concluded that reflex testing for LS was clinically effective and cost-effective but acknowledged that the issue of informed consent remained unresolved.14,15,16
There has been significant controversy among providers and academics regarding the need for explicit consent for IHC or MSI testing in this context.14,17,18,19 Part of the debate hinges on the need to protect the autonomy of the few patients who would receive positive results and may suffer distress or insurance discrimination versus the need to avoid causing unnecessary anxiety to the majority who would have negative results. Also at issue are the significant resources and capacity required to obtain consent.19 Another part of the debate hinges on whether IHC testing is considered a “genetic test.” IHC is a proteomic test and may provide germ-line information, which supports the need for consent. However, IHC is not considered a diagnostic or confirmatory test, which suggests that informed consent may not be an ethical prerequisite.17 MSI constitutes discrete testing of tissue and does not provide germ-line information, which also suggests that no consent is needed.17
Despite the ongoing controversy, little is known about stakeholders’ perspectives, especially providers who would be impacted by the requirement to seek consent or provide an opt-out, i.e., the option to avoid receiving unsolicited testing. Commentators have called for empirical studies to assess stakeholders’ perceptions of an ethical requirement of informed consent for LS reflex testing.17 Understanding stakeholders’ values is crucial for informing the development of evidence-informed public health interventions and policy initiatives. Furthermore, recent controversies17,18,20 and growing interest in implementing reflex-testing programs for LS14,21,22,23 underscore the need to understand providers’ perspectives on these issues. We conducted a stakeholder engagement study to examine health-care providers’ views and experiences to inform the design of a population-based IHC reflex testing of CRC tissue program and the types of patient choices that such a program would warrant.
Materials and Methods
Study design
We conducted a qualitative study, the methodology best suited for exploring the views and experiences of CRC and LS providers, in order to elucidate key ethical issues related to an opt-out and notification of reflex-testing results as well as genetic testing and counseling of LS patients and their families. This qualitative study is part of a mixed methods study to design, plan, and implement a population-based reflex-testing program for LS in Ontario, Canada. The research ethics boards at St. Michael’s Hospital, Sunnybrook Health Sciences Centre, and Mount Sinai Hospital approved the study.
Study population
Our population of interest comprised providers within the circle of care of CRC and LS patients who have the potential to be involved in making patients aware of the reflex-testing program, notifying patients of results, referring them to genetic services, and providing genetic counseling and testing. They included surgeons, geneticists, genetic counselors, family physicians, gastroenterologists, and medical oncologists from both academic and community hospitals. Eligible participants included providers in Ontario in independent practice for at least 1 year with experience managing LS patients or with an interest in CRC screening. We also interviewed representatives of the newborn-screening program because they have similar features and can reflect on the analogous ethical issues related to an opt-out, notification of positive screen results, genetic testing and counseling of families of screen-positive infants.
Sample recruitment
We used purposeful maximum variation sampling24 to capture as broad a range of views and experiences as possible across age, sex, discipline, length of time in practice, institutional setting, and geographic location. Participants constituted a convenience sample recruited through referrals from the research team supplemented by snowball sampling. An initial list of potential participants was compiled by study-team members drawing on their professional networks. This was supplemented by snowball sampling and a search of the Canadian Society of Colon and Rectal Surgeons directory. An invitation including detailed study information was e-mailed to prospective participants by the principal investigator. Nonresponders received a follow-up e-mail. Affirmative replies were forwarded by the study coordinator to the qualitative researcher for follow-up and scheduling.
Data collection
We conducted in-depth telephone interviews of 40–60 min in length using a semistructured discussion guide based on literature review25,26,27,28 and clinical consultation. Interviews explored participants’ experiences with IHC testing and notification of results, counseling of LS patients and their families, as well as their vision for the design and delivery of a reflex-testing program focusing on information provision, opt-out, result notification, and support for subsequent options (Interview Guide, Supplementary Information 1 online). Demographic data were collected before the interviews using standardized questions.
Data analysis
Interview data were digitally recorded for verbatim transcription. All transcripts were checked by the researcher against sound files for accuracy and corrected when necessary. Corrected transcripts were entered into HyperResearch software and coded for both anticipated and emergent themes using a coding framework developed in consultation with the study team. We analyzed the data using a qualitative descriptive approach,29,30 incorporating techniques from grounded theory, specifically, the constant comparative method and searches for disconfirming evidence (negative cases).31 Analyses were validated through peer debriefing, in which developing themes were identified and discussed with the study team. We also conducted descriptive statistical analysis of the participants’ demographics.
Results
Participants’ demographics characteristics
Twenty-seven providers participated in the interviews. Participants included colorectal surgeons (n = 6), general surgeons (n = 5), genetic counselors (n = 7), primary-care providers (n = 3), medical oncologists (n = 2), newborn-screening providers (n = 3), and a gastroenterologist. A majority practiced in academic centers (63%), for an average of 17 years ( Table 1 ).
Current reflex-testing practice
Providers’ experiences and perceptions of current practice revealed inconsistent identification and management of suspected LS patients. There was significant variation in IHC testing practice, where testing was ad hoc and ordered by a variety of providers, usually by geneticists or genetic counselors. In addition, medical oncologists often ordered MSI testing to support chemotherapy decisions, frequently without patients’ awareness. Pathologists also often initiated IHC testing at their discretion, without consulting either the patient or the surgeon. Given these scenarios, several expressed concern about the potential for patients to be blindsided by the results:
We are getting more and more of the stage 2c colon cancers where the oncologist is ordering the MSI ... and I don’t know that they’re being counselled at that point about the fact that they could be identified as having a hereditary cancer syndrome ... they order that testing to determine the chemotherapy plan but, then, “Surprise! You’re positive and being referred to genetics.” They don’t really understand why they are coming in. (Lynch 02 GC)
Once suspected LS patients were identified, providers worried about significant challenges in genetics service delivery. Providers noted concerns about long wait times, a lack of integrated genetics services in hospitals, geographic distance, patients actively undergoing cancer treatment, and complex family-history questionnaires. These barriers also led providers to question health-service capacity once reflex testing is scaled up:
My main concern is that it’s inadequately resourced in the province and so the waits are too long. People aren’t being seen for months, if not longer. (Lynch 22 Surg Onc)
These practice variations and delivery challenges led to a perceived underascertainment of LS patients and a lack of coordinated care. Providers noted that some patients “fell through the cracks” when months or years passed before referring providers became aware that their patient had not been seen by a genetics service. For these reasons, the prospect of a coordinated, population-based reflex-testing program was generally welcomed.
Perceptions of a population-based reflex-testing program
Providers expressed a high degree of support for a population-based reflex-testing program as an approach to addressing the underascertainment of LS patients and lack of coordinated care as well as standardizing the increasing use of genomic tests in practice.
The underascertainment of LS was frequently attributed to inadequate family-history taking and limited awareness of LS in the wider medical community.
I think, overall, there is a general lack of understanding of the spectrum of Lynch-associated tumors, which can explain why the referrals aren’t getting to us. (Lynch 01 GC)
There was broad agreement that more consistency and a more systematic approach to identifying and managing LS carriers are needed.
It just might be able to catch a proportion that are missed by our current criteria which are not 100% sensitive. It may improve sensitivity, specificity of selection and make it more cost-effective that way. (Lynch 11 Med Onc)
Many felt that, ultimately, implementation of a reflex-testing program for LS would improve care for LS patients only as part of a comprehensive approach. This would include improved awareness of the syndrome in the wider medical community, adequate funding and robust planning for downstream needs such as additional genetics capacity, ongoing surveillance, and coordination of care to ensure that LS patients or their unaffected relatives did not lapse into inadequate surveillance routines because they had been discharged from specialist care.
It has to do with all the other health delivery systems that have to be brought in line too if you’re going to increase the amount of screening ... Who’s going to do all the follow-up? (Lynch 09 CRC Surg)
I can imagine in many centres there would be a need for more genetic counsellors, which would obviously be a resource issue. Probably some places would need more clinicians who are familiar with the management of Lynch syndrome. So there are a lot of downstream implications. (Lynch 26 Med Onc)
Participants from the newborn-screening program echoed the need to budget for downstream costs and to plan for indeterminate results and provide information to patients as early as possible.
Introducing the screen right before someone is rolled into surgery isn’t the most ideal time for them to hear about that for the first time and be able to think about the implications ... Considering how much they’re dealing with and maybe even able to hear or not ... offers a better chance of success. (Lynch 24 NBS)
As someone who works in the downstream, I would encourage lots of discussion about what the follow-up is projected to be. What those models of care are going to look like ... What’s the projected ... increase in volume, given it’s ad hoc now ... And not only thinking about human resources but also from a data management and information perspective as well ... not only from a clinical perspective but, eventually, from an evaluation and research perspective as well. (Lynch 20 NBS)
One of the most consistent factors in support of a reflex-testing program for LS was the rapid evolution of new genetic technologies and their impact on patient care. Providers saw the program as providing an opportunity to standardize what they felt to be increasingly complex and evolving genetic tests in routine care:
In the 1980’s, I could do it ... basic family history ... and they had those 1, 2, 3, Amsterdam kind of things. I could sort that out. But now, it’s all kinds of different tests ... and different kinds of situations with different levels of sensitivity and certainty. And I can’t keep track ... I’m overwhelmed by the world of genetic testing.” (CRC surg 23)
On the other hand, providers highlighted the challenge of introducing a new program, where there was a need to emphasize the value of this information to patients rather than exceptionalizing genetic information by requiring formal consent:
“I think it’s just going to get more complicated as advanced molecular genetics [technologies] are going to be used more often [we need to] move forward in a, kind of, future-proof manner, having some type of discussion [with] enough information that people aren’t blindsided when they find out about [hereditary risks]. But at the same time, not so over-inclusive that it’s going to overwhelm them.” (Gen Surg, 26)
Positions on an opt-out for a reflex-testing program
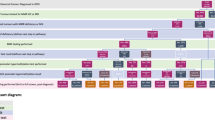
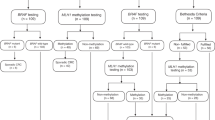
Discussion of whether patients should have the right to opt out of IHC testing elicited a wide range of nuanced, complex, and sometimes contradictory views. Broadly speaking, two positions emerged regarding when to provide an opt-out ( Figure 1 ).
Opt-out: after reflex testing. Many participants reflected on the feasibility of an opt-out for current delivery of care. Most took the view that IHC should be treated in the same way as other aspects of pathology testing and therefore should not be optional. “When women have their breast cancer out they don’t ask them whether they want their ER and PR testing” (Lynch 03 Gen Surg). Several participants argued that IHC testing is standard of care and part of routine pathology, leading some to ask “Do you have to consent to the pathology report then?” (Lynch 26 Med Onc). Those supporting this approach felt that if patients wished to opt out of a genetics referral, then that was a more reasonable point in their journey to provide detailed information and an opt-out:
Patients get fairly overwhelmed with discussions about cancer to begin with…when you... introduce a concept like IHC, where it’s not a black or white issue…I think it’s too much to try to explain that to everybody up front…. (Lynch 26 Med Onc)
However, providers also stressed the need for transparency about the possibility that the routine pathology tests could have genetic implications, to avoid blindsiding patients who screen positive. This position was bolstered by the argument that IHC is a proteomic test and may provide germ-line information:
I do feel that patients need to be aware that some testing is being done ... that may indicate there’s a greater hereditary component to their cancer that may have implications for further testing and ... if the red flag goes up, will be discussed in detail. And they would be able to consent [to] or decline that testing because patients then still have the option. (Lynch 05 GC)
Opt-out: before reflex testing. Although most participants were in favor of an opt-out after reflex testing, some preferred the opt-out before because of the concern that patients would experience distress, insurance discrimination, or a diagnostic odyssey that may be inconclusive. The emotionally burdensome information generated by the testing journey drew some providers toward the right not to know:
If, at the end of testing you have a diagnosis that suddenly puts patients into a pathway that may not have been of their choosing ... you have to imagine that group that wouldn’t want to know ... their rights to live their life without the information that some would consider critical, others might consider debilitating. (Lynch 21 Gen Surg)
Some providers supported an opt-out before reflex testing because of the concern about insurance discrimination if patients are found to have a LS mutation. Others justified an opt-out before reflex testing because of the possibility that the test may subject patients to a diagnostic process that yielded inconclusive findings: “If whatever is being introduced might open a can of worms on the path of the patients, then they need to be consented” (Lynch 21 Gen Surg).
That said, there was also recognition that offering an opt-out—at any point—raised a host of practical questions about who would do this and what information should be provided to patients to allow them to make a meaningful decision.
I think I would [favor opt-out], but I guess it would have to be within feeling really confident that they’re opting out in an informed way ... that they understand the implications... We just want to make sure that they’re doing it in an informed fashion. [Lynch 13 CRC Surg]
Many felt that genetic counselors were the best providers for detailed discussion about LS, but they also worried that there would not be sufficient capacity to engage in such discussions with all presurgical patients. Finally, there was considerable concern that patients undergoing treatment would be overwhelmed by the complex implications of a LS diagnosis that ultimately might not even be relevant in their case.
Discussion
Amid growing interest in implementing reflex-testing programs for LS,14,21,22,23 our study provides timely insight into ways to design and deliver this program. Our stakeholder study demonstrated that current practice supports the need for a population-based reflex-testing program, which could improve the identification and management of patients with suspected LS. Providers supported such a program because of the current lack of coordinated IHC testing and underascertainment of LS patients as well as for the opportunity to standardize the increasing use of genomic tests in clinical care. Most supported an opt-out after reflex testing because they felt that IHC testing is similar to other pathology tests, which are not optional. However, some preferred the opt-out before IHC testing out of concern for the possibility that patients would experience distress, the potential for insurance discrimination, or a diagnostic odyssey that might turn out to be inconclusive.
The support for an opt-out for reflex testing for LS is consistent with findings of other studies. Studies indicated that consent is unnecessary because IHC is one of several tests performed as part of the pathological examination,32 which often identifies lesions specific to genetic disorders with germ-line mutations.18 Study results also demonstrated the difficulty of incorporating genetic counseling before IHC testing given the burden to both doctor and patient at a time when the patient’s attention is focused on concerns of “self-preservation.”32 Other programs have come to similar conclusions, maintaining that an opt-out should be made available, as long as genetic counselors meet with all screen-positive patients to discuss results and provide informed consent for confirmatory mutation testing.18,33,34 This position is also consistent with current practice across North American laboratories,28 genetic counselors,33,35 and US cancer programs.18,36 A recent survey of 29 National Cancer Institute–designated cancer centers found that none required written consent for reflex testing and most (23/29, 79%) did not routinely include preoperative educational brochures; only 4 (14%) offered an opt-out from reflex testing.36 Furthermore, few genetic counselors or laboratories reported obtaining written or verbal consent to perform or report LS reflex testing, citing consent as a barrier to implementing tumor screening or the position that IHC testing was unlike germ-line testing and required no consent.28,35 However, when provided the opportunity to opt out of germ-line testing or learning its results, nearly 50% of high-risk patients either declined to be tested or declined to receive the test results.37 An estimated 30% of those who declined would have had germ-line mutations that would be missed,37 which raises questions about the value of screening and heightens the need for effective and scalable approaches to facilitating informed decision-making and education strategies.38
Beyond informing the ethical debate on patient choice, our study also provides novel insights into optimal ways to design and deliver a population-based reflex-testing program. Participants emphasized that the introduction of a reflex-testing program alone would not necessarily improve care overall for LS patients and their families. They felt that a comprehensive approach was needed to increase awareness of LS in the wider medical community and that substantial change would be needed to improve coordinated care, ensure adequate resourcing for genetics services, and facilitate ongoing surveillance. Finally, participants with experience with other screening programs strongly emphasized the need for early information provision and downstream planning, taking into account local differences in service structure. A comprehensive reflex-testing program for LS will need to include sufficient resources for genetic counseling coupled with provider awareness and education of LS and coordination of care.
There are several limitations of our study. Not all of the participants had substantial experience dealing with LS patients. Most of the participants were based at academic centers, and many were surgeons specializing in CRC rather than general surgeons. It is possible that more input from additional gastroenterologists and general surgeons, especially those based at community hospitals and outside large urban centers, would have yielded additional insights. Further research with patients is also warranted to ensure that their views and preferences regarding reflex testing are incorporated into the design of the program.
Despite these limitations, our study is the first to report a broad range of expert stakeholders’ perspectives on population-based reflex testing and to elucidate views on patient choice. The results demonstrate providers’ strong support for a population-based reflex-testing program for LS and delineate ways to plan, design, and organize the delivery of this service. Importantly, providers endorsed an opt-out after reflex testing as an appropriate governance mechanism for a population-based tumor testing program, which was based on feasibility and delivery constraints, provided that sufficient transparency and information were provided to patients prior to surgery. Our findings highlight the need to develop well-designed methods of patient education to support a meaningful information provision to enable an opt-out without jeopardizing uptake of screening and public health benefits for relatives of LS patients.
Disclosure
The authors declare no conflict of interest.
References
Matloff J, Lucas A, Polydorides AD, Itzkowitz SH. Molecular tumor testing for Lynch syndrome in patients with colorectal cancer. J Natl Compr Canc Netw 2013;11:1380–1385.
Bonadona V, Bonaïti B, Olschwang S, et al.; French Cancer Genetics Network. Cancer risks associated with germline mutations in MLH1, MSH2, and MSH6 genes in Lynch syndrome. JAMA 2011;305:2304–2310.
Dowty JG, Win AK, Buchanan DD, et al. Cancer risks for MLH1 and MSH2 mutation carriers. Hum Mutat 2013;34:490–497.
Senter L, Clendenning M, Sotamaa K, et al. The clinical phenotype of Lynch syndrome due to germ-line PMS2 mutations. Gastroenterology 2008;135:419–428.
Ries LAG, Melbert D, Krapcho M, et al. SEER Cancer Statistics Review, 1975–2004. National Cancer Institute, 2007. http://seer.cancer.gov/archive/csr/1975_2004/.
de Vos tot Nederveen Cappel WH, Järvinen HJ, Lynch PM, Engel C, Mecklin JP, Vasen HF. Colorectal surveillance in Lynch syndrome families. Fam Cancer 2013;12:261–265.
de Jong AE, Hendriks YM, Kleibeuker JH, et al. Decrease in mortality in Lynch syndrome families because of surveillance. Gastroenterology 2006;130:665–671.
Rubenstein JH, Enns R, Heidelbaugh J, Barkun A ; Clinical Guidelines Committee American gastroenterological association institute guideline on the diagnosis and management of Lynch syndrome. Gastroenterology 2015;149:777–782; quiz, e716-777.
Lynch HT, Lynch PM. Molecular screening for the Lynch syndrome–better than family history? N Engl J Med 2005;352:1920–1922.
Pérez-Carbonell L, Ruiz-Ponte C, Guarinos C, et al. Comparison between universal molecular screening for Lynch syndrome and revised Bethesda guidelines in a large population-based cohort of patients with colorectal cancer. Gut 2012;61:865–872.
Morrison J, Bronner M, Leach BH, Downs-Kelly E, Goldblum JR, Liu X. Lynch syndrome screening in newly diagnosed colorectal cancer in general pathology practice: from the revised Bethesda guidelines to a universal approach. Scand J Gastroenterol 2011;46:1340–1348.
Moreira L, Balaguer F, Lindor N, et al.; EPICOLON Consortium. Identification of Lynch syndrome among patients with colorectal cancer. JAMA 2012;308:1555–1565.
van Lier MG, Leenen CH, Wagner A, et al.; LIMO Study Group. Yield of routine molecular analyses in colorectal cancer patients ≤70 years to detect underlying Lynch syndrome. J Pathol 2012;226:764–774.
Evaluation of Genomic Applications in Practice and Prevention (EGAPP) Working Group. Recommendations from the EGAPP Working Group: genetic testing strategies in newly diagnosed individuals with colorectal cancer aimed at reducing morbidity and mortality from Lynch syndrome in relatives. Genet Med 2009;11:35–41.
Palomaki GE, McClain MR, Melillo S, Hampel HL, Thibodeau SN. EGAPP supplementary evidence review: DNA testing strategies aimed at reducing morbidity and mortality from Lynch syndrome. Genet Med 2009;11:42–65.
Bombard Y, Bach PB, Offit K. Translating genomics in cancer care. J Natl Compr Canc Netw 2013;11:1343–1353.
Chubak B, Heald B, Sharp RR. Informed consent to microsatellite instability and immunohistochemistry screening for Lynch syndrome. Genet Med 2011;13:356–360.
Williams JL, Williams MS. Informed consent and immunohistochemistry screening for Lynch syndrome. Genet Med 2011;13:848–849.
Zeps N, Iacopetta BJ, Schofield L, George JM, Goldblatt J. Waiver of individual patient consent in research: when do potential benefits to the community outweigh private rights? Med J Aust 2007;186:88–90.
Hall MJ. Counterpoint: implementing population genetic screening for Lynch Syndrome among newly diagnosed colorectal cancer patients–will the ends justify the means? J Natl Compr Canc Netw 2010;8:606–611.
Ngeow J, Eng C. Population-based universal screening for Lynch syndrome: ready, set. How? J Clin Oncol 2013;31:2527–2529.
Kastrinos F, Syngal S. Screening patients with colorectal cancer for Lynch syndrome: what are we waiting for? J Clin Oncol 2012;30:1024–1027.
Tomiak E, Samson A, Spector N, et al. Reflex testing for Lynch syndrome: if we build it, will they come? Lessons learned from the uptake of clinical genetics services by individuals with newly diagnosed colorectal cancer (CRC). Fam Cancer 2014;13:75–82.
Coyne IT. Sampling in qualitative research. Purposeful and theoretical sampling; merging or clear boundaries? J Adv Nurs 1997;26:623–630.
Cragun D, DeBate RD, Vadaparampil ST, Baldwin J, Hampel H, Pal T. Comparing universal Lynch syndrome tumor-screening programs to evaluate associations between implementation strategies and patient follow-through. Genet Med 2014;16:773–782.
Hunter JE, Zepp JM, Gilmore MJ, et al. Universal tumor screening for Lynch syndrome: Assessment of the perspectives of patients with colorectal cancer regarding benefits and barriers. Cancer 2015;121:3281–3289.
Schneider JL, Davis J, Kauffman TL, et al. Stakeholder perspectives on implementing a universal Lynch syndrome screening program: a qualitative study of early barriers and facilitators. Genet Med 2016;18:152–161.
Kalloger SE, Allo G, Mulligan AM, et al. Use of mismatch repair immunohistochemistry and microsatellite instability testing: exploring Canadian practices. Am J Surg Pathol 2012;36:560–569.
Sandelowski M. Whatever happened to qualitative description? Res Nurs Health 2000;23:334–340.
Sandelowski M. What’s in a name? Qualitative description revisited. Res Nurs Health 2010;33:77–84.
Strauss A, Corbin J. Basics of Qualitative Research: Techniques and Procedures for Developing Grounded Theory, 2nd edn. Sage Publications: Thousand Oaks, CA, 1998.
Southey MC, Jenkins MA, Mead L, et al. Use of molecular tumor characteristics to prioritize mismatch repair gene testing in early-onset colorectal cancer. J Clin Oncol 2005;23:6524–6532.
Gaff CL, Rogers MT, Frayling IM. Genetic counselling and consent for tumour testing in HNPCC. Clin Genet 2007;71:400–405.
Lynch Syndrome Screening Network. Best Practices. 2016. http://www.lynchscreening.net/best-practices.
Cohen SA. Current Lynch syndrome tumor screening practices: a survey of genetic counselors. J Genet Couns 2014;23:38–47.
Beamer LC, Grant ML, Espenschied CR, et al. Reflex immunohistochemistry and microsatellite instability testing of colorectal tumors for Lynch syndrome among US cancer programs and follow-up of abnormal results. J Clin Oncol 2012;30:1058–1063.
Ward RL, Hicks S, Hawkins NJ. Population-based molecular screening for Lynch syndrome: implications for personalized medicine. J Clin Oncol 2013;31:2554–2562.
Manne SL, Meropol NJ, Weinberg DS, et al. Facilitating informed decisions regarding microsatellite instability testing among high-risk individuals diagnosed with colorectal cancer. J Clin Oncol 2010;28:1366–1372.
Acknowledgements
We thank the providers who participated in this study and generously shared their experiences and views with us. This study was conducted with the support of Cancer Care Ontario and the Ontario Institute for Cancer Research through funding provided by the Government of Ontario. Y.B. is a Canadian Institutes of Health Research New Investigator. Results of this work have been presented at the following conferences: the American Society of Human Genetics, Health Technology Assessment International, the Canadian Agency for Drugs and Technologies in Health, Cancer Care Ontario, the Canadian Centre for Applied Research in Cancer Control, and the Ontario Institute for Cancer Research Health Services Research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bombard, Y., Rozmovits, L., Sorvari, A. et al. Universal tumor screening for Lynch syndrome: health-care providers’ perspectives. Genet Med 19, 568–574 (2017). https://doi.org/10.1038/gim.2016.150
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/gim.2016.150
Keywords
This article is cited by
-
When guidelines face reality — Lynch syndrome screening in the setting of public health system in a developing country
Journal of Community Genetics (2022)
-
Worldwide variation in lynch syndrome screening: case for universal screening in low colorectal cancer prevalence areas
Familial Cancer (2021)
-
Universal tumor screening for Lynch syndrome: perspectives of Canadian pathologists and genetic counselors
Journal of Community Genetics (2019)
-
Barriers to Lynch Syndrome Testing and Preoperative Result Availability in Earlyonset Colorectal Cancer: A National Physician Survey Study
Clinical and Translational Gastroenterology (2018)