Abstract
Purpose:
Women with a BRCA1 or BRCA2 mutation are at high risk for breast cancer and must make important decisions about breast cancer prevention and screening. In the current study, we report a multisite, randomized, controlled trial evaluating the effectiveness of a decision aid for breast cancer prevention in women with a BRCA mutation with no previous diagnosis of cancer.
Methods:
Within 1 month of receiving a positive BRCA result, women were randomized to receive either usual care (control group) or decision aid (intervention group). Participants were followed at 3, 6, and 12 months; were asked about preventive measures; and completed standardized questionnaires assessing decision making and psychosocial functioning.
Results:
One hundred fifty women were randomized. Mean cancer-related distress scores were significantly lower in the intervention group compared with the control group at 6 months (P = 0.01) and at 12 months postrandomization (P = 0.05). Decisional conflict scores declined over time for both groups and at no time were there statistical differences between the two groups.
Conclusion:
The decision aid for breast cancer prevention in women with a BRCA1 or BRCA2 mutation is effective in significantly decreasing cancer-related distress within the year following receipt of positive genetic test results.
Genet Med 19 3, 330–336.
Similar content being viewed by others
Introduction
For women who carry a mutation in BRCA1 or BRCA2, the risk of developing breast cancer is estimated to be as high as 80% by the age of 70 (ref. 1). Strategies to reduce the risk include prophylactic surgery (oophorectomy and/or mastectomy) and chemoprevention (tamoxifen). Each of these options has a different impact on breast cancer risk and a unique risk/benefit profile. As a result, decisions about breast cancer risk reduction can be difficult. No single choice will satisfy all of a woman’s personal objectives because no alternative is without residual risk of cancer and each has undesired outcomes. This situation is known as “choice dilemma” or “conflicted decision.”2
For women who receive a positive genetic test result, psychosocial functioning may be impaired and cancer-related distress may increase; these acute effects may exacerbate the difficulties of decision making. Nevertheless, professionals often encourage women to consider their cancer risk reduction options at the time of result disclosure when the women often experience distress and anxiety.3,4,5,6,7,8 After the genetic test result disclosure session, many women with a BRCA1 or BRCA2 mutation express the wish to have more information about cancer prevention options to help with decision making.9
Decision aids (DAs) have been shown to be effective for individuals facing decisions about health treatment and screening.10,11,12 They are interventions designed to help people make specific and deliberative choices among the available options that are relevant to health status.13 DAs are used to supplement, not replace, communication between professionals and patients. They differ from usual health education materials because of their detailed, specific, and personalized focus on options and outcomes for the purpose of preparing people for decision making.13 In general, DAs assist individuals in (i) understanding the range of options available, (ii) understanding the probable consequences of each option, (iii) considering the value they place on consequences, and (iv) participating actively with their professionals in deciding between options.13,14
In response to a needs assessment we conducted involving women with a BRCA mutation,9 we developed and pilot-tested a DA that was designed to support women with a BRCA1 or BRCA2 mutation regarding breast cancer prevention.15 Our pilot work suggested that our breast cancer prevention DA was effective at reducing decisional conflict and increasing knowledge. Decisional conflict is highly predictive of whether individuals make health-related decisions.16 Schwartz et al. reported that a DA for BRCA carriers (both affected and unaffected), which focused only on breast screening and prophylactic mastectomy (i.e., not including prophylactic oophorectomy and chemoprevention), was effective at reducing decisional conflict in women who remained undecided about breast cancer prevention.17 In the current study, we built on the study by Schwartz et al. and add prophylactic oophorectomy and chemoprevention as effective cancer prevention options. We report on a multisite, randomized, controlled trial comparing the effectiveness of a DA for breast cancer prevention that includes all risk-reducing options regarding decisional conflict, cancer-related distress, knowledge, and choice predisposition in women with a BRCA mutation with no previous diagnosis of cancer.
Materials and Methods
Participants
Women with a BRCA1 or BRCA2 mutation were recruited from four clinical cancer genetics clinics in Canada and through an online support network based in the United States (FORCE—Facing Our Risk of Cancer Empowered). Eligible women were those who (i) had a known BRCA1 or BRCA2 mutation, (ii) had received a positive genetic test result during a standard genetic counseling session within the previous month, (iii) had no previous diagnosis of cancer, (iv) were 25 to 60 years of age, and (v) understood written and spoken English. Women were excluded if they had a previous prophylactic mastectomy or prophylactic oophorectomy or had previously used tamoxifen.
Design and procedure
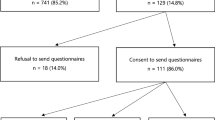
Ethics approval was obtained at all participating centers. We performed a multisite, randomized, controlled trial with stratification by site. Genetic counselors at each site obtained verbal consent from the women to be contacted by the study coordinator. Consenting women had baseline data (including date of genetic test result disclosure and age) provided by the genetic counselor, and further eligibility was assessed by the trial coordinator. If all eligibility criteria were met, then the women were randomized centrally with a secure Web-based randomization service (http://www.randomize.net). To limit the possibility of contamination, we enrolled only one woman per family.
Women allocated to the control group had access to standard care throughout the study period. Women in the intervention group had access to standard care in addition to the DA, which was mailed within 1 week of randomization. A follow-up telephone call with the study coordinator took place 4 weeks after randomization to ensure that the DA had been received. A research assistant blinded to group allocation telephoned all study participants at 3, 6, and 12 months postrandomization to determine trial outcomes. Each woman received a $10 gift card at completion of each follow-up questionnaire.
Intervention
The women allocated to the intervention group received standard care in addition to the intervention, which was a DA designed to provide decision support regarding breast cancer prevention in addition to standard genetic counseling to women with a BRCA1 or BRCA2 mutation. Development of the DA was guided by the Ottawa Decision Support Framework,18 an evidence-based, transdisciplinary, conceptual framework that can be used to guide clients in making decisions in clinical practice. The framework was developed for health decisions that (i) are stimulated by a new circumstance, diagnosis, or developmental transition; (ii) require careful deliberation because of the uncertain and/or value-sensitive nature of the benefits and risks; and (iii) require more effort during the deliberation phase than the implementation phase. The framework has three elements: assessing the needs/determinants of decision, providing decision support, and evaluating decision making and outcomes of decisions.
Construction of the DA was based on the following suggested components outlined by O’Connor and Edwards14: (i) information about options and outcomes; (ii) presentation of probability of outcomes; (iii) values clarification; (iv) coaching or guidance; and (v) delivery. The final version of the DA was based on feedback from cancer genetics specialists and women with a BRCA1 or BRCA2 mutation. The DA is a 15-page self-administered booklet that consists of key words and illustrative icons to summarize information and data regarding generic risk of breast cancer in BRCA1 and BRCA2 mutation carriers (risks presented using figures of 100 women, with number of affected women shaded in), breast cancer preventive options available to BRCA1 and BRCA2 mutation carriers (including prophylactic mastectomy, prophylactic bilateral salpingo-oophorectomy, and tamoxifen), types of studies evaluating breast cancer preventive strategies and guidelines for evaluating the evidence (four levels of evidence were used, denoted by colored ribbons), physical and psychological risks and benefits associated with each cancer preventive option, comparison of the options by profiling the pros and cons of each option, definitions of key words, and references for additional information and for supporting risk reduction estimates provided.
Description of usual care
Women allocated to the control group had access to standard genetic counseling provided to all women undergoing genetic testing for BRCA1 or BRCA2. This included both pretest genetic counseling and a standard 1-h result disclosure genetic counseling session and access to any follow-up care, which may have included referrals to specialists regarding breast cancer prevention, or follow-up with the genetic counselor.
Outcome measures
The primary outcome was decisional conflict, which is highly predictive of whether individuals make health-related decisions.16 Decisional conflict was measured using the Decisional Conflict Scale.19 The purpose of this scale is to measure a person’s perception of the difficulty making a decision including their perceived uncertainty in choosing between options; modifiable factors contributing to uncertainty such as feeling uninformed, feeling unclear about personal values, and feeling unsupported in decision making; and quality of the choice selected, which is defined as informed (consistent with personal values) and that the person is satisfied with and expects to maintain. The questionnaire consists of 16 items, with scores ranging from 0 (no decisional conflict) to 100 (extremely high level of decisional conflict). Scores less than 25 are associated with making health-related decisions and scores exceeding 37.5 are associated with delay or feeling unsure about implementation.20 The scale has been used to study diverse health decisions, including immunization, cancer screening, prenatal testing, hormone replacement therapy, and treatments for lung cancer, heart disease, and atrial fibrillation. Test–retest reliability exceeded 0.78. For the current study, Cronbach’s α was 0.99.
Secondary outcomes included cancer-related distress, knowledge, and choice disposition. Cancer-related distress was measured using the Impact of Event Scale (IES),21 a self-report measure designed to measure current subjective distress in relation to a specific stressor. The scale consists of 15 items (7 intrusion items and 8 avoidance items). Participants rate the frequency of intrusive and avoidant behaviors using a 4-point frequency scale (0 = not at all, 1 = rarely, 3 = sometimes, 5 = often). The IES allows calculation of a total score (with a possible range of 0 to 75) and separate intrusion and avoidance subscale scores (with possible ranges of 0 to 35 for intrusion and 0 to 40 for avoidance). Cronbach’s α based on populations of patients with cancer, women with a family history of breast cancer, survivors of advanced Hodgkin disease, patients with malignant melanoma, individuals tested for Huntington disease, and patients experiencing bereavement are 0.78 for intrusion and 0.82 for avoidance. For the current study, Cronbach’s α was 0.98. The IES has been found to have good validity and reliability when measuring cancer-related distress in women at increased risk for developing breast cancer.22 Scores for the total IES can be divided into the subclinical range (0–8), mild range (9–25), moderate range (26–43), and severe range (≥44).
Knowledge of breast cancer risk and risk prevention options was assessed using a knowledge questionnaire that was developed and tested in the pilot study.15 This questionnaire contained 13 items pertaining to risk of breast cancer associated with having a BRCA1/2 mutation, risk reduction associated with preventive options, and knowledge questions regarding each of the preventive options (prophylactic mastectomy, chemoprevention, and screening). Risk estimates were presented in the form of a continuous scale from 0 to 100%.
The subjects’ decision predispositions were measured using a choice predisposition tool.23 The subjects were asked to rate on a 15-point scale: 1 = not leaning toward a breast cancer prevention option (surgery, chemoprevention, screening), 8 = unsure, and 15 = leaning toward a breast cancer prevention option (surgery, chemoprevention, screening). A total score of 6 to 10 was classified as undecided.24 The test–retest reliability coefficients of these measures exceed 0.90, are correlated with personal values and expectations, and are sensitive to change.11
Sample size
The primary outcome involved changes in decisional conflict scores between the intervention and control groups at 12 months postrandomization. The sample size calculations were based on a hypothesized mean value of 2.3 for the control group and 2.0 for the treatment groups, with an estimated standard deviation of 0.6 for both groups as obtained from pilot test results.15 A two-sample, two-sided t-test using these estimates required 63 subjects per group (126 total) to provide 80% power at α = 0.05 to detect a difference. Because we assumed that we would have a 15% loss to follow-up, we estimated that a total sample of 150 subjects (75 per group) was required.
Statistical methods
All analyses were performed using SAS version 9.1 (SAS Institute, Cary, NC, USA). A two-sided significance level of 0.05 was used for the primary outcome. A significance level of 0.01 (two-sided) was used for secondary outcome and other outcomes to account for multiple comparisons. Descriptive statistics were calculated for all variables of interest. Continuous measures were summarized using means and standard deviations, whereas categorical measures were summarized using counts and percentages. To check the adequacy of the randomization, univariate analyses were performed to assess for differences between the two groups (treatment and control) on demographic variables. Continuous measures were assessed using two-sample, two-sided t-tests, whereas categorical measures were assessed using chi-square tests or Fisher’s exact tests when appropriate. The primary hypothesis was tested using a regression analysis to assess differences in the Decisional Conflict Scale between groups (treatment and control) at 12 months, controlling for baseline scores. The secondary outcome measures—the total IES score and the decision predisposition scale—werealso analyzed using regression analyses assessing differences between groups (treatment and control) at 12 months, controlling for baseline scores. The distribution of all outcome measures was assessed for normality prior to analysis. When required, normalizing transformations were sought and applied to the data. Missing data were handled using multiple imputation. Analyses were performed on an intent-to-treat basis.
Results
Participant characteristics
The 150 study participants were recruited between September 2008 and June 2011. The intervention and control groups were similar regarding baseline demographic and clinical variables ( Table 1 ). Study participants were contacted at 3, 6, and 12 months postrandomization to complete study questionnaires. Response rates were 94% at 3 months, 94% at 6 months, and 93% at 12 months. There was no difference in the response rate by group allocation.
Outcomes
Table 1 shows mean scores related to trial outcomes, including decisional conflict, cancer-related distress, and knowledge.
Decisional conflict
At baseline, the mean score for decisional conflict was 32.5 (SD = 14.1) for women in the intervention group and was 36.4 (SD = 17.1) for the control group (P = 0.13). Overall, 65 women (43.3%) had scores higher than 37 on the decisional conflict score. There were no statistical differences in mean decisional conflict scores between the DA group compared with the control group at any of the three follow-up times ( Table 2 ). Decisional conflict scores declined with time for both groups.
Cancer-related distress
At 3 months postrandomization, there were no differences in mean IES scores between the two groups. However, at 6 months, mean IES scores were significantly lower in the DA group than in the control group (19.3 (SD 13.2) vs. 25.2 (SD 14.5); t = −2.51, P = 0.01). This difference was also observed at 12 months postrandomization during the univariate analysis (17.7 (SD 14.7) vs. 22.4 (SD 15.5); t = −1.94; P = 0.05) ( Table 2 ), but it did not reach statistical significance when controlling for baseline scores ( Table 3 ).
BRCA knowledge
Knowledge scores were higher than 87% for both groups at all time points. There were no statistical differences in mean knowledge scores between the two groups at any of the three follow-up time points ( Table 2 ).
Choice predisposition
A minority of women were undecided about breast cancer prevention at the time of randomization regarding prophylactic mastectomy (25.3% undecided), prophylactic oophorectomy (12.0% undecided), and tamoxifen (26.7% undecided). Table 4 presents the frequencies of subjects reporting as undecided for each cancer prevention option at each of the three follow-up time points. For prophylactic mastectomy, the change in the proportion of women undecided decreased by 11.5% in the intervention group and by 5.3% in the control group. For prophylactic oophorectomy, the change in the proportion of women undecided decreased by 2.2% in the intervention group and increased by 8.6% in the control group.
Among those undecided about prophylactic mastectomy or tamoxifen (too few subjects undecided about prophylactic oophorectomy), mean scores for decisional conflict and cancer-related distress were compared between subjects who received the intervention and those who received usual care (control group) ( Table 5 ). Among women who were undecided about prophylactic mastectomy, mean cancer-related distress scores were significantly lower at 12 months for those in the intervention group than for those in the control group (P = 0.02). Among women who were undecided about tamoxifen, cancer-related distress was lower at all three follow-up time points for women in the intervention group than for women in the control group ( Table 5 ).
Discussion
This multisite, randomized, controlled trial was designed to evaluate the effectiveness of a DA for breast cancer prevention on decisional conflict, cancer-related distress, knowledge, and choice predisposition in women with a BRCA mutation with no previous diagnosis of cancer. We found that a DA for breast cancer prevention in women with a BRCA1 or BRCA2 mutation did not reduce decisional conflict, but it was effective in decreasing cancer-related distress in the year following receipt of positive genetic test results, especially for those who were undecided about cancer prevention within 1 month after receiving positive BRCA genetic test results.
Cancer-related distress has been reported to be elevated in women who receive positive BRCA1 and BRCA2 genetic test results, but it decreases over time.5,7 In the current study, we observed lower levels of long-term cancer-related distress in women who used the DA compared with those who received usual care. Hooker and colleagues25 have previously reported that decision support impacts the trajectory of distress among BRCA1 and BRCA2 mutation carriers. In their trial of a DA for women with and without a previous diagnosis of breast cancer, they observed an initial increase in distress at 1 month in the women with the DA; however, at 12 months, distress was lower in the DA group compared with the control group. The authors suggested that this may reflect short-term ongoing cognitive processing and extended deliberation about management options. In the current study, we did not observe elevated levels of distress at 3 months; however, levels were similar in those who used the DA and those with usual care. It was only later, at 6 and 12 months, when we observed significantly lower levels of distress in those using the DA compared with women receiving usual care, especially for those undecided about cancer prevention.
We found no significant difference in decisional conflict at any time point when comparing women who received the DA to women who received usual care. Interestingly, at randomization within 1 month after women received positive genetic test results, the mean levels of decisional conflict were lower than the cut-off score of 37.5; any score higher than 37.5 represents the point at which decisional conflict impairs the deliberation process. This suggests that most women in this trial were not experiencing decisional conflict related to their choices for breast cancer prevention at the time when they were randomized into the study. These baseline scores may provide an explanation for why there was no effect of the DA on decisional conflict. Furthermore, very few women reported being undecided about their choices for breast cancer prevention at randomization. In addition, knowledge scores were very high at baseline, suggesting that women had an excellent understanding of cancer risks and risk reduction strategies. This highlights the importance of both pre- and posttest genetic counseling in the clinical setting. As a component of standard genetic counseling, women who receive positive genetic test results typically receive intensive pretest counseling, during which options are discussed, and posttest counseling, during which options and recommendations for cancer prevention are discussed in detail. As a result, many women had made decisions about cancer prevention prior to being randomized in the current study. After testing of a CD-ROM DA for women with a BRCA mutation that focused on breast screening and prophylactic mastectomy (for women with and without a previous diagnosis of breast cancer), Schwartz et al.17 reported that, overall, there were no differences in decisional conflict scores at 12 months between those in the DA group and those in the usual care group. However, for the 52% of women who reported being undecided at baseline, the DA was effective at reducing decisional conflict compared with usual care. They proposed that because DA are essentially designed for those individuals experiencing heightened decisional conflict, women who have successfully formulated their decision prior to using the DA may have derived limited, if any, benefit. In our study, there were far fewer women undecided at baseline than in this previous study, which may explain the nonsignificant difference in decisional conflict between those in the DA group and those in the usual care group.
As previously mentioned, there were very few women undecided about each preventive option at baseline; therefore, we were unable to detect any significant change in the frequency of women being undecided about an option. At randomization, few women were undecided about each breast cancer prevention option (25% for prophylactic mastectomy, 12% for prophylactic oophorectomy, and 26% for tamoxifen). Interestingly, from 3 months to 12 months postrandomization, 11.5% fewer women were undecided about prophylactic mastectomy in the DA arm and 5.3% fewer women were undecided in the usual care arm. For prophylactic oophorectomy, there was a decrease of 2.2% being undecided in the DA arm but an increase of 8.6% being undecided in the usual care arm. This provides further evidence that DA may be most appropriate for those women who are undecided about their cancer prevention options.
Our trial adds to the understanding of the effects of DA for women with a BRCA mutation. Unlike other studies, in the current study, only women without a previous diagnosis of breast or ovarian cancer were included, and all breast cancer risk reduction options were included. Other trials have included women with a previous diagnosis of cancer, and prevention options may differ for these women. Interestingly, van Roosmalen et al.26 reported that their decision-making intervention, which included two value assessment sessions followed by individualized treatment information, was beneficial for unaffected women and detrimental for women with a previous cancer diagnosis.
This study has several limitations. Our findings have limited generalizability given the highly educated and well-informed nature of our study participants. In future studies, it will be important to assess our DA within a more diverse context, as measured across various demographic features, including culture, education, and socioeconomic status. Additionally, within our study we did not capture utilization of our DA tool. Evaluating the uptake of our intervention as well as the frequency of use would enable a more meaningful analysis of its impact across the various outcome measures we included. Furthermore, the majority of our respondents were decided about cancer prevention options at the time of randomization, and as a result we were underpowered to evaluate whether there were statistical differences between groups when limiting analyses to only those who were undecided. Furthermore, we did not confirm uptake of preventive options with medical records. Future studies that are targeted at women who are undecided would provide further evidence of the effectiveness of the DA.
We previously reported that the DA was very acceptable to women who recently received positive BRCA1 and BRCA2 genetic test results.15 The current study has demonstrated that the DA is effective at reducing cancer-related distress when compared with usual care, especially for women undecided about cancer prevention within the first month after receiving positive BRCA genetic test results. This DA was developed to be used in addition to usual care for women with a BRCA1 and BRCA2 mutation and requires no extra resources for health-care providers, unlike other previous DA for this population. This DA is a feasible15 and effective tool for women with a BRCA mutation and adds to the resources available for these women at high risk.
Disclosure
The authors declare no conflict of interest.
References
Ford D, Easton DF, Bishop DT, Narod SA, Goldgar DA. Risks of cancer in BRCA1 mutation carriers. Lancet 1994;343:692–695.
Sjoberg L. To smoke or not to smoke: conflict or lack of differentiation? In: Humphreys P, Sevenson O, Vari A (eds). Analysing and Aiding Decision Processes. Elsevier: New York, 1983.
Croyle RT, Smith KR, Botkin JR, Baty B, Nash J. Psychological responses to BRCA1 mutation testing: preliminary findings. Health Psychol 1997;16:63–72.
Lerman C, Narod S, Schulman K, et al. BRCA1 testing in families with hereditary breast-ovarian cancer. A prospective study of patient decision making and outcomes. JAMA 1996;275:1885–1892.
Schwartz MD, Peshkin BN, Hughes C, Main D, Isaacs C, Lerman C. Impact of BRCA1/BRCA2 mutation testing on psychologic distress in a clinic-based sample. J Clin Oncol 2002;20:514–520.
Lodder L, Frets PG, Trijsburg RW, et al. Psychological impact of receiving a BRCA1/BRCA2 test result. Am J Med Genet 2001;98:15–24.
Metcalfe KA, Mian N, Enmore M, et al. Long-term follow-up of Jewish women with a BRCA1 and BRCA2 mutation who underwent population genetic screening. Breast Cancer Res Treat 2012;133:735–740.
Bjørnslett M, Dahl AA, Sørebø Ø, Dørum A. Psychological distress related to BRCA testing in ovarian cancer patients. Fam Cancer 2015;14:495–504.
Metcalfe KA, Liede A, Hoodfar E, Scott A, Foulkes WD, Narod SA. An evaluation of needs of female BRCA1 and BRCA2 carriers undergoing genetic counselling. J Med Genet 2000;37:866–874.
Goel V, Sawka CA, Thiel EC, Gort EH, O’Connor AM. Randomized trial of a patient decision aid for choice of surgical treatment for breast cancer. Med Decis Making 2001;21:1–6.
O’Connor AM, Tugwell P, Wells GA, et al. A decision aid for women considering hormone therapy after menopause: decision support framework and evaluation. Patient Educ Couns 1998;33:267–279.
Dolan JG, Frisina S. Randomized controlled trial of a patient decision aid for colorectal cancer screening. Med Decis Making 2002;22:125–139.
O’Connor AM, Stacey D, Rovner DR, et al. Decision aids for people facing health treatment or screening decisions (Cochrane Review). Cochrane Library. Update Software: Oxford, UK, 2002.
O’Connor AM, Edwards A. The role of decision aids in promoting evidence-based patient choice. In: Edwards A, Elwyn G (eds). Evidence-Based Patient Choice: Inevitable or Impossible? Oxford University Press: New York, 2001:220–242.
Metcalfe KA, Poll A, O’Connor A, et al. Development and testing of a decision aid for breast cancer prevention for women with a BRCA1 or BRCA2 mutation. Clin Genet 2007;72:208–217.
O’Connor A, Sun Q, Laupacis A, et al. Predicting downstream effects of decisional conflict: meta-analysis of the decisional conflict scale. 3rd International Shared Decision Making Conference, Ottawa, ON, Canada, 14–16 June 2005.
Schwartz MD, Valdimarsdottir HB, DeMarco TA, et al. Randomized trial of a decision aid for BRCA1/BRCA2 mutation carriers: impact on measures of decision making and satisfaction. Health Psychol 2009;28:11–19.
O’Connor AM, Tugwell P, Wells GA, et al. Randomized trial of a portable, self-administered decision aid for postmenopausal women considering long-term preventive hormone therapy. Med Decis Making 1998;18:295–303.
O’Connor AM. Validation of a decisional conflict scale. Med Decis Making 1995;15:25–30.
O’Connor A. User Manual: Decisional Conflict Scale. Ottawa Health Research Institute, 1993 (updated 2010). http://decisionaid.ohri.ca/docs/develop/User_Manuals/UM_decisional_conflict.pdf.
Horowitz M, Wilner N, Alvarez W. Impact of Event Scale: a measure of subjective stress. Psychosom Med 1979;41:209–218.
Thewes B, Meiser B, Hickie IB. Psychometric properties of the Impact of Event Scale amongst women at increased risk for hereditary breast cancer. Psychooncology 2001;10:459–468.
O’Connor A, Jacobsen MJ, Stacey D. Ottawa Personal Decision Guide. 2002. http://www.ohri.ca/programs/clinical_epidemiology/OHDEC/Ottawa_5Step_020909_wData.pdf.
O’Connor A. User Manual: Measures of Decision/Choice Predisposition. Ottawa Hospital Research Institute. 1996. http://decisionaid.ohri.ca/docs/develop/User_Manuals/UM_ChoicePredisposition_Decision.pdf.
Hooker GW, Leventhal KG, DeMarco T, et al. Longitudinal changes in patient distress following interactive decision aid use among BRCA1/2 carriers: a randomized trial. Med Decis Making 2011;31:412–421.
van Roosmalen MS, Stalmeier PF, Verhoef LC, et al. Randomized trial of a shared decision-making intervention consisting of trade-offs and individualized treatment information for BRCA1/2 mutation carriers. J Clin Oncol 2004;22:3293–3301.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Metcalfe, K., Dennis, CL., Poll, A. et al. Effect of decision aid for breast cancer prevention on decisional conflict in women with a BRCA1 or BRCA2 mutation: a multisite, randomized, controlled trial. Genet Med 19, 330–336 (2017). https://doi.org/10.1038/gim.2016.108
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/gim.2016.108
Keywords
This article is cited by
-
Risk-management decision-making data from a community-based sample of racially diverse women at high risk of breast cancer: rationale, methods, and sample characteristics of the Daughter Sister Mother Project survey
Breast Cancer Research (2024)
-
Effectiveness of evidence-based decision aids for women with pathogenic BRCA1 or BRCA2 variants in the german health care context: results from a randomized controlled trial
BMC Medical Informatics and Decision Making (2023)
-
Impact of shared decision making on healthcare in recent literature: a scoping review using a novel taxonomy
Journal of Public Health (2023)
-
Evaluation of two evidence-based decision aids for female BRCA1/2 mutation carriers in Germany: study protocol for a randomised controlled parallel-group trial
Trials (2022)
-
Patient-provider communication while using a clinical decision support tool: explaining satisfaction with shared decision making for mammography screening
BMC Medical Informatics and Decision Making (2022)