Abstract
Purpose
To assess the vision-related quality of life and self-reported driving performance of patients with dry eye disease (DED).
Patients and methods
The study was performed in the eye centre of Peking University Third Hospital, China. In total, 87 dry eye patients and 42 controls were enroled, including 49 patients without any treatment (group A), 38 patients treated with artificial tears (group B) and 42 controls without DED (group C). The participants had no eye disease other than DED. Scores of a vision-related quality-of-life questionnaire (Ocular Surface Disease Index (OSDI)), a daily life-related visual function questionnaire and a questionnaire about performance during driving were collected. Data were compared among the groups and analysed.
Results
Significant differences in all clinical characteristics and OSDI scores were found between DED patients and normal controls (P<0.05). While subjects in group A felt more uncomfortable than those in group B, the functional limitations related to dry eye were significant in all DED patients, especially for daily work and using a computer. DED was correlated with unsafe driving habits and performance, which may increase the risk of dangerous driving (P<0.01). For patients with DED, the rate of accidents and near-accidents was 10.33%, and the rate of missed targets totalled 32.17%.
Conclusions
DED can lead to many inconveniences in daily life, including driving. The frequencies of unsafe driving habits and performance were increased in patients with DED.
Similar content being viewed by others
Introduction
Dry eye disease (DED) is a growing public health problem and is one of the most frequent reasons for seeking eye care. DED is estimated to affect from 5% to more than 30% of the population, depending on the diagnostic criteria.1 Increasing evidence shows that DED is a major cause of visual disturbances, which can degrade the quality of everyday life and impact health status.2 According to a recent review from the 2007 International Dry Eye Workshop, DED causes damage to the ocular surface and symptoms of ocular discomfort associated with impaired visual quality.3
Because driving is a task integral to daily life for many people around the world, research on the role of vision in driving is of great importance DED is one of the most common diseases leading to eye discomfort and vision loss. Patients with DED often report vision-related difficulties in performing daily activities, although no strong correlations have been found among clinical tests, optical and biological examinations, and patient-reported deterioration in quality of life in clinical practice.4, 5, 6 Research on eye disease and driving can serve as a basis for policies regarding who can be licensed to drive and for developing rehabilitation strategies that help visually impaired individuals acquire skills so that they can safely drive.
Materials and methods
Study participants
The study was performed in the eye centre of Peking University Third Hospital, China. Study participants were pre-screened for eligibility and were between 20 and 50 years of age. Patients were recruited between March 2014 and December 2015. The study adhered to the tenets of the Declaration of Helsinki, and informed consent was obtained from all participants.
All participants were in good general health and were licensed drivers with at least weekly driving practice. Three groups of drivers were included in the study. One group of patients (group A) had been diagnosed with DED for the first time without any prior treatment. The other patients (group B) included in the study were treated with tear substitutes only, without any anti-inflammatory or cyclosporine medication, and had not experienced changes in their condition within the last 3 months. Healthy subjects with no ocular pathology, treatment, or symptoms or signs of DED were included as controls (group C).
Only the subjects with a best-corrected visual acuity of at least 20/20 were included because this study was focused on decreases in visual function and fitness related to dry eye rather than extensive vision damage. The exclusion criteria included any ocular pathology other than DED, eyelid malpositioning or dynamic disorders, previous ocular or eyelid surgery, contact lens use, systemic disorders, pregnancy, and treatment changes within the last 3 months.
Clinical examination and questionnaires
DED was diagnosed by the association of ocular symptoms and tear film abnormalities (Schirmer I test <5 mm/5 min and/or tear break-up test <10 s), with or without ocular surface damage (corneal and conjunctival staining), according to the DEWS criteria from the modified Delphi Panel Report.4, 7 All patients presented mild-severity or moderate-severity DED according to the Delphi approach.5
The Ocular Surface Disease Index (OSDI) questionnaire was developed to quantify the specific effect of DED on vision-targeted, health-related quality of life.8 This disease-specific questionnaire includes three subscales: ocular symptoms (OSDI-symptoms), vision-related activities of daily living (OSDI-function), and environmental triggers. Each subscale (0–100) was calculated, as well as an overall averaged score (0–100). All subjects completed the questionnaire independently after researchers elaborated on the meaning of the questions. The subjects were allowed to ask questions while completing the questionnaire. The answers were scored as follows: 1=always, 2=mostly, 3=sometimes, 4=seldom, and 5=never.
The vision-related activities of daily living (OSDI-function) portion was combined with the 25-item National Eye Institute Visual Function Questionnaire to produce questions about daily life designed to evaluate the impact of DED, including the effects on reading, computer use, watching TV, driving, walking, emotion, sleep, and interpersonal relationships. The dry eye-related functional limitations of all drivers in the study were evaluated by autognosis. The answers were scored as follows: 1=always, 2=mostly, 3=sometimes, 4=seldom, and 5=never.
Questionnaires about performance during driving were collected to measure the safety of driving. Drivers evaluated their on-road driving performance by autognosis using the same method as the OSDI questionnaire. Dangerous activities that may increase the risk of danger during driving, such as increasing blink times and missed signals on the road and traffic lights, were assessed and given scores of 1–5 (1=completely agree, 2=mostly agree, 3=sometimes agree, 4=mostly disagree, and 5=completely disagree). The environmental triggers and treatments were also recorded in the questionnaire. The detailed questionnaires are provided in the appendix.
Statistical analysis
All data are presented as the mean±SD. Data were assessed for normality, homogeneity of variance, and sphericity to perform the appropriate tests.
Results
Study participants
The study population was composed of 89 dry eye patients and 44 normal controls (Table 1). No significant differences were observed among the three groups regarding gender, number, age, and years of driving (P>0.05).
Characteristics of dry eye disease
The OSDI scores of each group are detailed in Table 1. Significant differences in all clinical characteristics and OSDI scores were found between DED patients and normal controls (ANOVA, P<0.05 for each). Subjects in group A were more uncomfortable than those in group B. Multiple comparisons were also performed among the three groups according to the OSDI scale.
Functional limitations in activities of daily life
The functional limitations related to DED were significant in DED patients. Most DED patients said that DED limited their quality of daily life at most times. The patients with no treatment (group A) suffered more functional limitations than the patients receiving treatment with artificial tears (group B), especially during daily work and when using a computer (P<0.01, shown in Table 2).
All DED patients, both groups A and B, complained about daily life-related vision limitations. The degree of functional limitations presented the same trend in the two groups, and some patients were suffering for approximately half of the time (score 2.5). The trend of functional limitations is shown in Figure 1.
Driving performance
In all three groups, the sum of the dry eye symptom scores was correlated with the functional limitations, according to vision-related quality-of-life questionnaires (P<0.001, r=0.835, correlation was significant at the 0.01 level (two-tailed)).9, 10
In the three groups, the sum of dry eye symptom scores was correlated with driving habits and performance, which may increase the risk of dangerous driving (P<0.01, r=0.069, correlation is significant at the 0.01 level (two-tailed)). The years of driving showed no correlation with driving habits and performance (P=0.971).
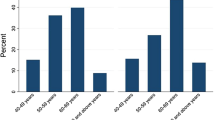
The scores of dangerous activities during driving were evaluated by self-assessment, as shown in Table 3. The environmental triggers and treatments are also shown in the table.
Effects on driving safety
In the study, ~40% of DED patients had dangerous driving experiences, and one driver had an accident due to visual disturbances related to DED. The rate of accidents and near-accidents was 10.33%. The rate of missing targets, including vehicles, pedestrians, traffic lights, and signals, was 32.17% (Table 4).
Discussion
In this study, we used a detailed daily life and driving questionnaire to compare the driving habits and driving adaptations in a sample of patients with DED. Our study found functional limitations that primarily included using a computer, reading, watching TV, daily work, and driving. The effect of DED on driving was more serious than the effect on emotion, walking, sleep, and interpersonal relationships. DED was correlated with unsafe driving habits and performance, which may increase the risk of danger. Our finding suggests that more attention should be focused on the effect of DED on driving performance.
In the study, information from three groups of individuals was collected to assess the effect of DED on driving. According to the OSDI scores, significant differences were present between group A (dry eye patients without any treatment) and group C (normal controls) for OSDI-symptoms scores, functional scores, and environmental factors. The DED patients without any treatment suffered more discomfort than patients treated with artificial tears (group B), but no significant differences were found between group A and group B. The results also indicated that artificial tears were one of the most important treatments for DED because the complicated precorneal tear film plays an important role in ocular optical quality, as it is the most anterior refractive surface of the eye.11, 12
DED patients commonly complain of difficulties in performing vision-related daily activities, as previously reported using quality-of-life questionnaires.9 We found that driving is greatly influenced by DED. In this study, the 25-item National Eye Institute Visual Function Questionnaire was combined with another questionnaire about driving and traffic safety. According to the questionnaire scores, the limitations on driving ranked in the first half, indicating it was more greatly affected than other daily life activities, such as sleeping, walking, emotion, and interpersonal relationships. However, driving is a dangerous activity and requires increased attention and skill. In this study, the sum of dry eye symptom scores was correlated with functional limitations and negative experiences on the road. Therefore, the effect of DED on driving should be emphasised. Drivers should at least receive treatments, such as eye drops, to relieve the uncomfortable symptoms of DED.
Negative driving activities, which may be dangerous, were scored by self-assessment in the three groups. Significant differences were found between DED patients and normal controls for bad driving habits, such as inattention; missing vehicles, pedestrians, traffic lights, and other signals; reduced concern about the surroundings; tension; dysphoria; delayed cognition; and fatigue. Deschampset al13 also reported that DED patients more commonly missed targets at crossroad entrances than targets appearing straight ahead. Therefore, drivers with DED will experience more dangerous conditions than drivers without DED. In this study, the effects on the safety of driving were evaluated by self-assessments. Approximately 40% of DED patients in the study had dangerous driving experiences, and one driver had an accident due to visual disturbances related to DED. The rate of accidents and near-accidents was 10.33%. The rate of missed targets, including vehicles, pedestrians, traffic lights, and signals, was 32.17%. Difficulty in viewing lighted targets may be related to a disability in identifying external signals, such as lights or traffic signs as well as pedestrians or other vehicles when driving. Although DED patients may have more difficulty while driving, this does not necessarily mean that they cannot drive safely. Future studies should evaluate the correlation between accident rates and DED. The reaction time was also delayed in DED patients, which could be linked to discomfort when driving regularly. This could explain the feeling of insecurity and loss of confidence in patients with ocular dryness.
Despite the novel and important findings of our study, there are some limitations. First, all information that we collected was self-reported, and therefore subjectivity and recall bias cannot be avoided. As an example, according to the results of the self-assessment, DED patients reported no increase in blink frequency, which may not be true according to the combination of answers of other questions and the results of previous studies. Second, the driving situation that we evaluated was limited. Considering that the environment significantly influences driving performance, and insecurity is enhanced when driving at night, it would be interesting to perform such a simulation in dark conditions. In addition, a future study using artificial tears during driving may be helpful to determine whether a driving simulator could be useful for the evaluation of treatments.14
In summary, our study investigated the self-reported driving performance of drivers with DED as compared with drivers with normal vision. The results indicated that drivers with DED may experience greater driving skill limitations and therefore be more dangerous than healthy drivers, and these factors may be underestimated by drivers with DED. Using eye drops or avoiding difficult driving conditions may be safe choices for drivers with DED.15, 16, 17, 18, 19, 20

References
The epidemiology of dry eye disease: report of the Epidemiology Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 2007; 5 (2): 93–107.
Baudouin C, Creuzot-Garcher C, Hoang-Xuan T, Rigeade MC, Brouquet Y, Bassols A et al. Severe impairment of health-related quality of life in patients suffering from ocular surface diseases. J Fr Ophtalmol 2008; 31 (4): 369–378.
The definition and classification of dry eye disease: report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 2007; 5 (2): 75–92.
Schein OD, Tielsch JM, Munoz B, Bandeen-Roche K, West S . Relation between signs and symptoms of dry eye in the elderly. A population-based perspective. Ophthalmology 1997; 104 (9): 1395–1401.
Begley CG, Chalmers RL, Abetz L, Venkataraman K, Mertzanis P, Caffery BA et al. The relationship between habitual patient-reported symptoms and clinical signs among patients with dry eye of varying severity. Invest Ophthalmol Vis Sci 2003; 44 (11): 4753–4761.
Nichols KK, Nichols JJ, Mitchell GL . The lack of association between signs and symptoms in patients with dry eye disease. Cornea 2004; 23 (8): 762–770.
Behrens A, Doyle JJ, Stern L, Chuck RS, McDonnell PJ, Azar DT et al. Dysfunctional tear syndrome: a Delphi approach to treatment recommendations. Cornea 2006; 25 (8): 900–907.
Dougherty BE, Nichols JJ, Nichols KK . Rasch analysis of the Ocular Surface Disease Index (OSDI). Invest Ophthalmol Vis Sci 2011; 52 (12): 8630–8635.
Tong L, Waduthantri S, Wong TY, Saw SM, Wang JJ, Rosman M et al. Impact of symptomatic dry eye on vision-related daily activities: the Singapore Malay Eye Study. Eye 2010; 24 (9): 1486–1491.
Miljanovic B, Dana R, Sullivan DA, Schaumberg DA . Impact of dry eye syndrome on vision-related quality of life. Am J Ophthalmol 2007; 143 (3): 409–415.
Rieger G . The importance of the precorneal tear film for the quality of optical imaging. Br J Ophthalmol 1992; 76 (3): 157–158.
Koh S, Maeda N, Kuroda T, Hori Y, Watanabe H, Fujikado T et al. Effect of tear film break-up on higher-order aberrations measured with wavefront sensor. Am J Ophthalmol 2002; 134 (1): 115–117.
Deschamps N, Ricaud X, Rabut G, Labbe A, Baudouin C, Denoyer A . The impact of dry eye disease on visual performance while driving. Am J Ophthalmol 2013; 156 (1): 184–189 e3.
Huang FC, Tseng SH, Shih MH, Chen FK . Effect of artificial tears on corneal surface regularity, contrast sensitivity, and glare disability in dry eyes. Ophthalmology 2002; 109 (10): 1934–1940.
Mangione CM, Lee PP, Gutierrez PR, Spritzer K, Berry S, Hays RD et al. Development of the 25-item National Eye Institute Visual Function Questionnaire. Arch Ophthalmol 2001; 119 (7): 1050–1058.
Freeman EE, Gange SJ, Munoz B, West SK . Driving status and risk of entry into long-term care in older adults. Am J Public Health 2006; 96 (7): 1254–1259.
Goto E, Yagi Y, Matsumoto Y, Tsubota K . Impaired functional visual acuity of dry eye patients. Am J Ophthalmol 2002; 133 (2): 181–186.
Ferrer-Blasco T, Garcia-Lazaro S, Montes-Mico R, Cervino A, Gonzalez-Meijome JM . Dynamic changes in the air-tear film interface modulation transfer function. Graefes Arch Clin Exp Ophthalmol 2010; 248 (1): 127–132.
Montes-Mico R, Alio JL, Charman WN . Dynamic changes in the tear film in dry eyes. Invest Ophthalmol Vis Sci 2005; 46 (5): 1615–1619.
Montes-Mico R, Caliz A, Alio JL . Wavefront analysis of higher order aberrations in dry eye patients. J Refract Surg 2004; 20 (3): 243–247.
Acknowledgements
The research was supported by National Natural Science Foundation of China (No. 7250204).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Wang, Y., Lv, H., Liu, Y. et al. Characteristics of symptoms experienced by persons with dry eye disease while driving in China. Eye 31, 1550–1555 (2017). https://doi.org/10.1038/eye.2017.88
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2017.88