Abstract
Aims
To compare intraocular pressure (IOP) reductions with fixed-combination (FC) latanoprost/timolol once daily in the evening vsFC dorzolamide/timolol twice daily.
Methods
This evaluator-masked, multicentre, controlled clinical trial randomized subjects with primary open-angle glaucoma or ocular hypertension with IOP insufficiently responsive to β-blocker therapy (screening IOP>21 and <37 mm Hg) to FC latanoprost–timolol (N=135) or FC dorzolamide/timolol (N=135). At screening, baseline, and after 4 and 12 weeks of therapy, IOP was measured three times at 0800, 1200, and 1600 hours. Adverse events were recorded at each visit. The primary efficacy end point was whether either FC could be shown to be inferior to the other with respect to change in mean daytime IOP from baseline to week 12.
Results
Mean daytime IOP levels were similar at baseline. Mean reductions in daytime IOP from baseline to week 12 were −9.7 mm Hg for FC latanoprost–timolol and −9.5 mm Hg for FC dorzolamide/timolol. The difference between FC latanoprost/timolol–FC dorzolamide–timolol was −0.2 mm Hg (95% confidence interval (CI), −0.8 to –0.4 mm Hg). The upper bound of the 95% CI was <1.5 mm Hg, indicating that neither FC is inferior to the other. However, a significantly greater percentage of subjects treated with FC latanoprost/timolol achieved IOP levels ⩽16 and ⩽15 mm Hg (P⩽0.01). Both treatments were well tolerated.
Conclusions
When β-blocker therapy is inadequate, either FC may achieve the desired IOP level, but FC latanoprost/timolol more oftenly achieves a pressure of ⩽16 mm Hg. Both FCs were well tolerated.
Similar content being viewed by others
Introduction
In many patients with glaucoma or ocular hypertension, targeted intraocular pressure (IOP) control is not obtained with a single topical ocular hypotensive agent;1, 2 multidrug regimens or fixed-combination (FC) therapies are often warranted. The β-adrenergic receptor antagonist timolol, which primarily acts by decreasing the rate of production of aqueous humour by the ciliary epithelium, commonly has been combined with other drugs to lower IOP in an additive or synergistic manner.3, 4, 5, 6, 7, 8 Latanoprost (Xalatan, Pfizer Inc, New York, NY, USA), a prostaglandin F2α analog that is effective and relatively safe in the treatment of glaucoma and ocular hypertension,9, 10, 11, 12, 13 acts by increasing the outflow,14, 15, 16 a mechanism possibly complementary to that of timolol. Studies have confirmed the additive effect of this combination in lowering IOP.17, 18, 19
Combining the two medications in an FC formulation is preferable to the administration of two individual agents to maximize patient medication adherence and quality of life.20, 21, 22, 23, 24 The FC of latanoprost 0.005% and timolol 0.5% (Xalacom, Pfizer Inc., NY, USA) was first approved in December 2000 by the Medical Products Agency in Sweden and since then has been registered and/or approved for marketing in 60 other countries.25 Recently, a trend towards a greater daytime reduction with nighttime dosing of FC latanoprost/timolol has been shown, whereas morning dosing tended to give lower nighttime pressures.26
Another available effective FC product combines timolol 0.5% and the topical anhydrase inhibitor dorzolamide 2.0%, which acts similarly to timolol in suppressing the production of aqueous humour27 but is dosed twice daily (Cosopt, Merck & Co., Inc., Blue Bell, PA, USA).
The purpose of this study was to compare IOP reductions after treatment with FC latanoprost/timolol administered once daily in the evening with reductions associated with twice-daily administration of FC dorzolamide/timolol over a 12-week period. The primary objective was to show the noninferiority of FC timolol/latanoprost; the experimental design also served to determine the converse, that is, whether FC dorzolamide/timolol is inferior to FC latanoprost/timolol. Considering the results of previous studies,9, 26, 28 a greater IOP reduction in daytime IOP levels was expected with an evening dosing of FC latanoprost/timolol.
Materials and methods
Study design
This 12-week, randomized, parallel-group, evaluator-masked study was conducted at 25 centres in Europe (Germany, 6; Italy, 6; France, 5; Greece, 4; and Sweden, 4; NCT00140049). The final protocol and informed consent documentation were reviewed and approved by the Independent Ethics Committees at each participating investigational centre. The study was conducted in compliance with the Declaration of Helsinki's principle and with all International Conference on Harmonization Good Clinical Practice guidelines. Written informed consent was obtained from all subjects before study enrollment. We certify that all applicable institutional and governmental regulations concerning the ethical use of human volunteers were followed during this research.
Subjects
See Table 1 for study inclusion and exclusion criteria. Note that according to the European Glaucoma Society Guidelines,20 if monotherapy is inadequately effective (or has no effect), the agent should be withdrawn and substituted before adding a second drug. However, if the first-choice agent effectively lowers the IOP but not to the target level, adjunctive therapy can be added. In cases in which two therapies are needed, an FC is preferable to individual drugs.20 Although investigators were expected to follow these guidelines, for practical reasons, data were not collected on IOP levels before therapy, on each of the two monotherapies, and on combination therapy. Therefore, the degree of nonresponsiveness to β-blocker therapy was not documented or analysed or may have varied among investigators, but should represent the usual practice within the regions represented by the investigators.
Treatments and assessments
Potentially eligible subjects were assessed at a screening visit 7 days to 4 weeks before study entry. Medical and ocular histories were recorded; visual acuity was measured; and visual field (if not performed within the previous year), gonioscopy (if not documented during the previous 5 years), lid and slit-lamp examination, and ophthalmoscopy were performed. Intraocular pressure levels were measured with a calibrated Goldmann applanation tonometer. All ocular measurements were performed in both eyes. Required washout periods before the baseline visit were 4 weeks for β-adrenergic antagonists and prostaglandin analogues, 2 weeks for adrenergic agonists, and 5 days for cholinergic agonists and carbonic anhydrase inhibitors. Subjects requiring a 4-week washout returned after 2 weeks for an IOP safety check.
Study visits occurred at baseline and at weeks 4 and 12. At the baseline visit, visual acuity measurement and lid and slit-lamp examinations were repeated, and masked evaluators measured and recorded IOP levels three times in each eye, starting with the right eye, at 0800, 1200, and 1600 hours. To be eligible for randomization, the mean of these IOP measurements must be ⩾24 and <37 mm Hg in the eye with the higher mean IOP. If both eyes of a subject met all inclusion and no exclusion criteria and had identical IOP levels, the right eye was used for randomization. Eligible subjects were assigned consecutively to one of the two treatment groups (1 : 1 ratio) using a randomized code generated by Pfizer Inc. and retained at Global Pharmacy Operations. Randomization was performed independently within each centre with a fixed block size of 4. Subjects assigned to latanoprost/timolol FC were instructed to instill one drop of study drug once daily in the evening; those assigned to dorzolamide/timolol FC were instructed to administer one drop of study drug in the morning and in the evening.
All study drugs were supplied in commercially labeled bottles. The study was evaluator masked, but subjects could not be masked because of differences in the frequency of administration of study medications. Subjects were cautioned not to reveal the study assignment or the frequency of administration to the masked evaluator, and bottles were packaged in small black cylinders to protect the evaluator masking. Each subject received two black cylinders at baseline and three black cylinders at week 4; each bottle was expected to last for 4 weeks. For subjects assigned to FC latanoprost/timolol, the first drop was instilled the evening after the baseline visit. Those assigned to FC dorzolamide/timolol instilled the first drop the morning after the baseline visit; at week 4 and 12 visits, to preserve masking, the morning dose was instilled after an IOP level measurement was performed without the investigator's presence. It was requested that the same examiner measure the IOP levels using the same calibrated tonometer at each time point and at each visit for a given subject. At weeks 4 and 12, visual acuity was measured and lid and slit-lamp examinations were repeated; refraction and ophthalmoscopy were performed at week 12.
Adverse events were monitored and recorded by investigators throughout the study. The severity of events and the investigator's opinion of the relationship with the study treatment were noted. An event was classified as serious if it was life threatening, required inpatient hospitalization or prolonged hospitalization, resulted in persistent or significant disability/incapacity, or resulted in a congenital anomaly/birth defect. Adverse events were followed until they resolved or stabilized.
Variables and analyses
The primary end point was the mean change in daytime IOP from baseline to week 12 in the study eye. The daytime IOP for a given subject at any visit was calculated as the mean of IOP level measurements at 0800, 1200, and 1600 hours; if the IOP measurement at any time point was missing, daytime IOP was calculated as the mean of nonmissing IOP measurements. The analysis of covariance (ANCOVA) model was used to analyse the mean change in daytime IOP, with baseline daytime IOP as the covariate, and treatment and centre as factors. The treatment difference (FC latanoprost/timolol–FC dorzolamide/timolol) and a two-sided 95% confidence interval (CI) for the difference were calculated. FC latanoprost/timolol was considered to be noninferior to FC dorzolamide/timolol if the upper limit of the 95% CI of the difference was <1.5 mm Hg; FC latanoprost/timolol was considered to be superior if the upper limit of the 95% CI was <0 mm Hg.
Secondary efficacy end points included mean daytime IOP change from baseline to week 4; change from baseline in the mean IOP at weeks 4 and 12 at all measurement time points; the percentage of subjects reaching prespecified percentage reductions in IOP from baseline to weeks 4 and 12 (from ⩾5 to ⩾40% in 5% increments); and the percentage of subjects attaining prespecified IOP levels after 4 and 12 weeks of treatment (from ⩽22 to ⩽15 mm Hg in 1 mm Hg increments). An ANCOVA model was applied to the analysis of mean change in daytime IOP from baseline to week 4, with baseline IOP as the covariate and treatment and centre as factors; two-sided 95% CIs were calculated. Between-group differences in percentages were evaluated with the Cochran–Mantel–Haenszel test or the Fisher's exact test if the expected marginal size was <5. Adverse events were classified by body system and preferred term using the Medical Dictionary for Regulatory Activities coding system.
The intent-to-treat population (ITT) included all randomized subjects who had at least one postbaseline IOP measurement; the per protocol (PP) population included all those in the ITT population who had no major protocol violations, who completed IOP measurements within the allowed time frames, who completed ⩾75 days of treatment with the last dose administered before or on the day of the week 12 visit, and who did not take prohibited concurrent medication. Analyses using the ITT populations used the last observation carried-forward method; missing observations at weeks 4 or 12 were extrapolated by carrying forward the last postbaseline nonmissing observation. No imputation was applied to the PP population. The PP population was used to perform tests of noninferiority for daytime IOP levels and IOP levels at the three measurement time points at week 12. The ITT population was used to support tests of noninferiority at week 12, to evaluate noninferiority at week 4, and for analyses of between-group differences in percentages of subjects reaching prespecified percentage reductions in IOP and attaining prespecified IOP levels. Safety analyses included all randomized subjects. Statistical analyses were performed using SAS/UNIX Version 8.2 (SAS Institute, Cary, NC, USA).
The sample size was calculated using a t-test with a one-sided significance level of 2.5 and 80% power. Before the study it was determined that a sample of 113 evaluable subjects per treatment group was required to test a noninferiority margin of 1.5 mm Hg assuming a common standard deviation of the between-group difference of 4.0 mm Hg. Assuming an attrition rate of 5%, 238 subjects were targeted for enrollment. Sample size calculations were performed using the MTT0 program in nQuery, Version 4.0 (Statistical Solutions, Saugus, MA, USA).
Results
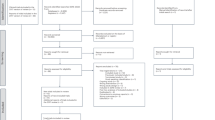
A total of 300 subjects entered the washout period, and 270 subjects were randomized, 135 to each treatment group. Most subjects completed the study (95%; 257 of 270), 128 in the FC latanoprost/timolol group and 129 in the FC dorzolamide/timolol group. The number of subjects withdrawing from the study was comparable across groups. The PP population included 121 subjects in the FC latanoprost/timolol group and 117 in the FC dorzolamide/timolol group; the ITT population included 133 subjects per treatment group.
At baseline, treatment groups generally were similar with regard to demographic and clinical characteristics (Table 2). Although the female to male ratio was higher in the FC dorzolamide/timolol group, the between-group difference was not statistically significant. The average spherical equivalent was close to plano for both treatment groups, with mean (SD) reported as −0.45 (3.07) in the FC latanoprost/timolol group and as −0.35 (2.68) in the FC dorzolamide/timolol group. In all, 134 of 135 (99.3%) subjects in the FC latanoprost/timolol group and 135 of 135 (100%) subjects in the FC dorzolamide/timolol group had been treated for the primary diagnosis before the start of the study. Systemic β-blockers were administered concomitantly during the study in 22 (18%) subjects in the FC latanoprost/timolol group and in 12 (10%) subjects in the FC dorzolamide/timolol group.
Efficacy
In the PP population, mean daytime IOP levels at baseline were 26.6 mm Hg (SD, 2.8) and 27.3 mm Hg (SD, 3.2) in the FC latanoprost/timolol and dorzolamide/timolol groups, respectively (Table 3). Least square mean (standard error (SE)) changes in daytime IOP from baseline to week 12 (primary efficacy end point) were −9.7 mm Hg (0.2) in the FC latanoprost/timolol group and −9.5 mm Hg (0.2) in the FC dorzolamide/timolol group (Table 3). The treatment difference was −0.2 mm Hg (0.3) with a 95% CI of −0.8 to 0.4 mm Hg, favouring the latanoprost/timolol FC. The upper bound of 95% CI was <1.5 mm Hg, indicating that neither FC was inferior to the other (P=0.51). These results were only minimally impacted when the variable ‘gender’ was added to the ANCOVA model. The noninferiority of the agents at week 12 with regard to changes in daytime IOP levels was supported by results of a parallel analysis in the ITT population (P=0.08 for between-group difference).
Mean daytime IOP levels at weeks 4 and 12 were similar in the two treatment groups and were consistent in the PP and ITT populations (Figure 1). At week 12, treatment differences in IOP changes from baseline at 0800, 1200, and 1600 hours were small and not statistically significant in either PP (Table 3) or ITT populations (data not shown). No significant differences were noted with regard to percentages of subjects achieving prespecified percentages of mean daytime IOP reduction at the end of the treatment. Percentages of subjects reaching specific levels of daytime IOP at week 12 generally were similar with no statistically significant differences between treatment groups at levels of ⩾17 mm Hg (Figure 2). However, significantly greater percentages of those treated with FC latanoprost/timolol achieved IOP levels ⩽16 and ⩽15 mm Hg at week 12 (P⩽0.01; Figure 2).
Safety
Both FC agents were well tolerated. In all, 35 of 135 (25.9%) subjects in the FC latanoprost/timolol group and 41 of 135 (30.4%) in the FC dorzolamide/timolol group reported adverse events. The most frequently occurring adverse events were ocular, which affected similar numbers of subjects in the two groups (17 of 135 (12.6%) vs 20 of 135 (14.8%), respectively). The most commonly noted ocular adverse events in the FC latanoprost/timolol group were eye pruritus and ocular hyperaemia (each occurring in 3 of 135 subjects; 2.2%); most frequently reported ocular adverse events in the FC dorzolamide/timolol group were eye pain, blurred vision, and visual acuity reduction (each occurring in 4 of 135 subjects; 3.0%). Ocular events, which are considered to be treatment related, were reported in 8.9% (12 of 135) of subjects in both groups. With regard to systemic adverse events, nervous system disorders occurred in 2 of 135 (1.5%) subjects in the FC latanoprost/timolol group and in 6 of 135 (4.4%) subjects in the FC dorzolamide/timolol group; systemic adverse event profiles for all other nonocular body systems were similar (<2% between-group difference). Two subjects reported serious adverse events, one in each treatment group; neither event was considered to be related to study medication and both resolved. No deaths were reported.
Discussion
This 12-week, multicentre, randomized, evaluator-masked, parallel-group study, which included a 4-week washout period between screening and baseline, is the largest study to date comparing FC latanoprost/timolol administered once daily in the evening with FC dorzolamide/timolol instilled twice daily. There was no demonstrable difference in effectiveness between the two FC eye drops, neither being inferior to the other, when mean daytime IOP levels based on 0800, 1200, and 1600-hour measurements were compared after 4 and 12 weeks of treatment. Least square mean changes in daytime IOP levels from baseline to week 12 (primary efficacy end point) were −9.7 and −9.5 mm Hg in the latanoprost/timolol and dorzolamide/timolol FC groups, respectively.
The finding of equivalent effectiveness parallels the results of two previous studies in which FC latanoprost/timolol was administered in the evening.29, 30 A 3-month crossover study29 of second-line therapy in 31 patients insufficiently controlled on latanoprost monotherapy with open-angle glaucoma or exfoliative glaucoma found no statistical differences between the two FCs in mean 24-h IOP levels, maximum or minimum IOP levels, or IOP levels measured at six individual time points. Another crossover study30 of 32 newly diagnosed, open-angle glaucoma, treatment-naive patients found that both treatments significantly reduced the IOP levels (measured once in the morning) between baseline and month 1. Two additional studies31, 32 compared the outcomes in subjects treated with FC latanoprost/timolol administered in the morning vs FC dorzolamide/timolol instilled twice daily. A double-masked, 8-week, crossover study in 33 patients32 found mean daytime IOP levels to be statistically similar across treatments. In contrast, a 3-month, randomized, parallel-group, evaluator-masked study31 in 253 subjects found that FC latanoprost/timolol reduced the mean daytime IOP by 1 mm Hg more than the comparator (P=0.005) and that mean IOP levels after 3 months of treatment were significantly lower in the FC latanoprost/timolol group at 0800 and 1600 hours (P<0.01 for both comparisons).
In this study, the decrease in IOP was somewhat less marked than expected in view of the results of previous studies showing increased efficacy with nighttime dosing of latanoprost.17, 28 In the present research, both combination therapies showed a mean IOP-reducing effect from baseline of about 35%. As far as FC latanoprost/timolol is concerned, this level of reduction is toward the high end of the range of decreases found in previous studies31, 33, 34, 35, 36, 37, 38, 39 with morning dosing and no timolol run-in (range, 31.5–36.0%). With regard to the FC dorzolamide/timolol; however, the percentage daytime IOP reduction found herein is considerably larger than those reported in five of six previously published studies (range, 25.2–31.2%). Although systemic β-blockers are known to potentially interfere with the reduction of IOP induced by timolol,40 use of systemic β-blockers was not an exclusion criterion in this study if the subject and dosage were stable for 3 months before screening and if the dosage was not expected to change during the study. Use of systemic β-blockers occurred in 22 (18%) of the FC latanoprost/timolol group and in 12 (10%) subjects in the FC dorzolamide/timolol group.
At 12 weeks, similar numbers of subjects in each treatment group achieved prespecified percent IOP reductions from baseline, but a significantly greater percentage of subjects achieved IOP levels of ⩽16 mm Hg with FC latanoprost/timolol (36 vs 21%; P=0.001). This finding may reflect differences in the mechanisms of action of the individual agents.41 Both timolol and dorzolamide lower the rate of aqueous humour formation affecting the inflow pathway, whereas latanoprost facilitates the outflow pathways.
In general, both treatments were well tolerated and safe. Overall, there was no specific trend in occurrence of either ocular or systemic adverse events, and the number of subjects withdrawn because of an adverse event was low in both treatment groups.
In patients in whom a given monotherapy does not sufficiently reduce IOP levels, the practitioner may first consider a trial with alternative monotherapy. In those patients for whom individual ocular hypotensive therapy provides a response but does not reduce the IOP to the target level (insufficient response), European Glaucoma Society Guidelines20 advise that adjunctive therapy can be initiated and that combination therapy is preferable to individual therapies. Topical treatment with multiple agents should be avoided where possible to enhance compliance.20
This study had several strengths and limitations. For example, we used an evaluator-masked approach to reduce bias in clinical assessments, and investigator masking was maintained by packaging the treatments into small black cylinders to protect the identity of the bottles within. Generally, treatment groups were well balanced in terms of baseline demographic and clinical characteristics, including baseline IOP; the potential impact of the nonstatistically significant between-group imbalance in the male to female ratio was tested in the ANCOVA model for the primary analysis and was found to impact the results only minimally. This study was limited by its relatively short time frame, as 12 weeks is not sufficiently long enough to evaluate long-term efficacy or safety, changes in visual acuity, visual field, or cup-to-disc ratio.
In conclusion, the study showed that, when β-blocker therapy is inadequate, both FC treatments result in clinically and statistically significant decreases in post-baseline IOP levels and are well tolerated.

References
Collaborative Normal-Tension Glaucoma Study Group. Comparison of glaucomatous progression between untreated patients with normal-tension glaucoma and patients with therapeutically reduced intraocular pressures. Am J Ophthalmol 1998; 126: 487–497.
Kass MA, Heuer DK, Higginbotham EJ, Johnson CA, Keltner JL, Miller JP et al. The Ocular Hypertension Treatment Study: a randomized trial determines that topical ocular hypotensive medication delays or prevents the onset of primary open-angle glaucoma. Arch Ophthalmol 2002; 120: 701–713.
Bucci MG . Intraocular pressure-lowering effects of latanoprost monotherapy versus latanoprost or pilocarpine in combination with timolol: a randomized, observer-masked multicenter study in patients with open-angle glaucoma. Italian Latanoprost Study Group. J Glaucoma 1999; 8: 24–30.
Choudhri S, Wand M, Shields MB . A comparison of dorzolamide–timolol combination versus the concomitant drugs. Am J Ophthalmol 2000; 130: 832–833.
Holló G, Chiselita D, Petkova N, Cvenkel B, Liehneova I, Izgi B et al. The efficacy and safety of timolol maleate versus brinzolamide each given twice daily added to travoprost in patients with ocular hypertension or primary open-angle glaucoma. Eur J Ophthalmol 2006; 16: 816–823.
Hommer A, Kapik B, Shams N, The Unoprostone Adjunctive Therapy Study Group. Unoprostone as adjunctive therapy to timolol: a double masked randomised study versus brimonidine and dorzolamide. Br J Ophthalmol 2003; 87: 592–598.
Strahlman ER, Vogel R, Tipping R, Clineschmidt CM . The use of dorzolamide and pilocarpine as adjunctive therapy to timolol in patients with elevated intraocular pressure. The Dorzolamide Additivity Study Group. Ophthalmology 1996; 103: 1283–1293.
Wang RF, Serle JB, Gagliuso DJ, Podos SM . Comparison of the ocular hypotensive effect of brimonidine, dorzolamide, latanoprost, or artificial tears added to timolol in glaucomatous monkey eyes. J Glaucoma 2000; 9: 458–462.
Alm A, Stjernschantz J . Effects on intraocular pressure and side effects of 0.005% latanoprost applied once daily, evening or morning. A comparison with timolol. Scandinavian Latanoprost Study Group. Ophthalmology 1995; 102: 1743–1752.
Camras CB, Alm A, Watson P, Stjernschantz J . Latanoprost, a prostaglandin analog, for glaucoma therapy. Efficacy and safety after 1 year of treatment in 198 patients. Latanoprost Study Groups. Ophthalmology 1996; 103: 1916–1924.
Camras CB . Comparison of latanoprost and timolol in patients with ocular hypertension and glaucoma: a six-month masked, multicenter trial in the United States. The United States Latanoprost Study Group. Ophthalmology 1996; 103: 138–147.
Parrish RK, Palmberg P, Sheu WP, XLT Study Group. A comparison of latanoprost, bimatoprost, and travoprost in patients with elevated intraocular pressure: a 12-week, randomized, masked-evaluator multicenter study. Am J Ophthalmol 2003; 135: 688–703.
Watson P, Stjernschantz J . A six-month, randomized, double-masked study comparing latanoprost with timolol in open-angle glaucoma and ocular hypertension. The Latanoprost Study Group. Ophthalmology 1996; 103: 126–137.
Toris CB, Camras CB, Yablonski ME . Effects of PhXA41, a new prostaglandin F2α analog, on aqueous humor dynamics in human eyes. Ophthalmology 1993; 100: 1297–1304.
Weinreb RN, Toris CB, Gabelt BT, Lindey JD, Kaufman PL . Effects of prostaglandins on the aqueous humor outflow pathways. Surv Ophthalmol 2002; 47 (Suppl 1): S53–S64.
Ziai N, Dolan JW, Kacere RD, Brubaker RF . The effects on aqueous dynamics of PhXA41, a new prostaglandin F2α analogue, after topical application in normal and ocular hypertensive human eyes. Arch Ophthalmol 1993; 111: 1351–1358.
Alm A, Widengård I, Kjellgren D, Söderström M, Friström B, Heijl A et al. Latanoprost administered once daily caused a maintained reduction of intraocular pressure in glaucoma patients treated concomitantly with timolol. Br J Ophthalmol 1995; 79: 12–16.
Lee PY, Shao H, Camras CB, Podos SM . Additivity of prostaglandin F2 alpha-1-isopropyl ester to timolol in glaucoma patients. Ophthalmology 1991; 98: 1079–1082.
Rulo AH, Greve EL, Hoyng PF . Additive effect of latanoprost, a prostaglandin F2 alpha analogue, and timolol in patients with elevated intraocular pressure. Br J Ophthalmol 1994; 78: 899–902.
European Glaucoma Society. Terminology and Guidelines for Glaucoma, 3rd edn. DOGMA, Srl: Savona, Italy, 2008.
Gurwitz JH, Glynn RJ, Monane M, Everitt DE, Gilden D, Smith N et al. Treatment for glaucoma: adherence by the elderly. Am J Public Health 1993; 83: 711–716.
Patel SC, Spaeth GL . Compliance in patients prescribed eyedrops for glaucoma. Ophthalmic Surg 1995; 26: 233–236.
Robin AL, Novack GD, Covert DW, Crockett RS, Marcic TS . Adherence in glaucoma: objective measurements of once-daily and adjunctive medication use. Am J Ophthalmol 2007; 144: 533–540.
Tsai JC, McClure CA, Ramos SE, Schundt DG, Pichert JW . Compliance barriers in glaucoma: a systematic classification. J Glaucoma 2003; 12: 393–398.
Latanoprost/Timolol Fixed Combination Investigator's Brochure (Pfizer internal document, New York, NY). June 2004, p 100.
Konstas AG, Nakos E, Tersis I, Lallos NA, Leech JN, Stewart WC . A comparison of once-daily morning vs evening dosing of concomitant latanoprost/timolol. Am J Ophthalmol 2002; 133: 753–757.
Wayman L, Larsson LI, Maus T, Brubaker R . Comparison of dorzolamide and timolol as suppressors of aqueous humor flow in humans. Arch Ophthalmol 1997; 115: 1368–1371.
Konstas AG, Maltezos AC, Gandi S, Hudgins AC, Stewart WC . Comparison of 24-hour intraocular pressure reduction with two dosing regimens of latanoprost and timolol maleate in patients with primary open-angle glaucoma. Am J Ophthalmol 1999; 128: 15–20.
Konstas AGP, Mikropoulos D, Dimopoulos AT, Moumtzis G, Nelson LA, Stewart WC . Second-line therapy with dorzolamide/timolol or latanoprost/timolol fixed combination versus adding dorzolamide/timolol fixed combination to latanoprost monotherapy. Br J Ophthalmol 2008; 92: 1498–1502.
Martinez A, Sanchez M . Retrobulbar haemodynamic effects of the latanoprost/timolol and the dorzolamide/timolol fixed combinations in newly diagnosed glaucoma patients. Int J Clin Prac 2007; 61: 815–825.
Shin DH, Feldman RM, Sheu WP, Fixed Combination Latanoprost/Timolol Study Group. Efficacy and safety of the fixed combinations latanoprost/timolol versus dorzolamide/timolol in patients with elevated intraocular pressure. Ophthalmology 2004; 111: 276–282.
Konstas AG, Kozobolis VP, Lallos N, Christodoulakis E, Stewart JA, Stewart WC . Daytime diurnal curve comparison between the fixed combinations of latanoprost 0.005%/timolol maleate 0.5% and dorzolamide 2%/timolol maleate 0.5%. Eye 2004; 18: 1264–1269.
Garcia-Sanchez J, Rouland JF, Spiegel D, Pajic B, Cunliffe I, Traverso C et al. A comparison of the fixed combination of latanoprost and timolol with the unfixed combination of brimonidine and timolol in patients with elevated intraocular pressure. A six month, evaluator masked, multicentre study in Europe. Br J Ophthalmol 2004; 88: 877–883.
Stewart WC, Stewart JA, Day DG, Sharpe ED, Jenkins JN . Efficacy and safety of the latanoprost/timolol maleate fixed combination vs the concomitant brimonidine and latanoprost therapy. Eye 2004; 18: 990–995.
Diestelhorst M, Larsson LI, European–Canadian Latanoprost Fixed Combination Study Group. A 12-week, randomized, double-masked, multicenter study of the fixed combination of latanoprost and timolol in the evening versus the individual components. Ophthalmology 2006; 113: 70–76.
Konstas AG, Papapanos P, Tersis I, Houliara D, Stewart WC . Twenty-four hour diurnal curve comparison of commercially available latanoprost 0.005% versus timolol and dorzolamide fixed combination. Ophthalmology 2003; 110: 1357–1360.
Orzalesi N, Rossetti L, Bottoli A, Fumagalli E, Fogagnolo P . The effect of latanoprost, brimonidine, and a fixed combination of timolol and dorzolamide on circadian intraocular pressure in patients with glaucoma or ocular hypertension. Arch Ophthalmol 2003; 121: 453–457.
Fechtner RD, Airaksinen PJ, Getson AJ, Lines CR, Adamsons IA, COSOPT versus XALATAN Study Groups. Efficacy and tolerability of the dorzolamide 2%/timolol 0.5% combination (COSOPT) versus 0.005% (XALATAN) in the treatment of ocular hypertension or glaucoma: results from two randomized clinical trials. Acta Ophthalmol Scand 2004; 82: 42–48.
Konstas AG, Kozobolis VP, Tsironi S, Makridaki I, Efremova R, Stewart WC . Comparison of the 24-hour intraocular pressure-lowering effects of latanoprost and dorzolamide/timolol fixed combination after 2 and 6 months of treatment. Ophthalmology 2008; 115: 99–103.
Lama PJ . Systemic adverse effects of beta-adrenergic blockers: an evidence-based assessment. Am J Ophthalmol 2002; 134: 749–760.
Brubaker RF . Targeting outflow facility in glaucoma management. Surv Ophthalmol 2003; 48 (Suppl 1): S17–S20.
Acknowledgements
Editorial support, including revising the paper based on author feedback and styling the paper for journal submission, was provided by Jane G Murphy, PhD, of Zola Associates. Gerald Bean, BS, an independent consultant and former employee of Pharmacia, Inc., critically reviewed the manuscript. Support for these activities was funded by Pfizer Inc., New York, NY, USA.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
Dr Grunden and Mr Kwok are employees of Pfizer Inc. Dr Miglior declares no conflict of interest.
Appendix A
Appendix A
Members of the Xalacom/Cosopt European Study Group
France: Dr med Philippe Denis, Hôpital Edouard Heriot, Lyon; Dr med Frederic Mouriaux, Hôpital Côte de Nacre, Caen; Dr med Guillaume Peigne, Polyclinique de Atlantique, Saint Herblain; Dr med Bernard Ridings, Hôpital De La Timme, Marseille; Dr med Daniele Rigal, Hôpital Gabriel Montpied, Clermont-ferrand.
Germany: Dr med Thomas Christ, Ophthalmology practice, Schorndorf; Dr med Heinrich Deuker, Ophthalmology practice, Darmstadt; Dr med Thomas Hamacher, Ophthalmology practice, Starnberg; Dr med Martin Hoffmann, Ophthalmology practice, Landau/Pfalz; Dr med Christoph Jelinek, Ophthalmology practice, Darmstadt; Dr med Maria-Luise Scherzer, Ophthalmology practice, Regenstauf.
Greece: Dr Konstandinos Karabatsas, University Hospital of Larisa, Larisa; Dr Anastassios Konstas, Ahepa General Hospital, Thessaloniki, Macedonia; Dr Vasilios Kozombolis, University Hospital of Alexandroupoli, Alexandroupoli; Dr Miltiadis Tsilimbaris, University Hospital of Heraklion, Heraklion, Crete.
Italy: Professor Roberto Carassa, Instituto S Raffaele/Clinica Oculistica Universitaria, Milano; Professor Nicola Delle Noci, Univerita de Foggia, Ospedali Riuniti, Foggia; Professor Michele Iester, Universita’ di Genova, Genova; Dr Leonardo Mastropasqua, Ospedale Clinicizzato Univeritaria i Chieti, Chieti; Professor Stefano Miglior, Universitaria Milano Biocca, Monza; Dr Marco Nardi, Ospedale S Chiaro A.O. Universitaria Pisana, Pisa.
Sweden: Dr Adnan Chatila, University Hospital, Ebro; Dr Anders Heijl, Malmö University Hospital, Malmö; Dr Bertil Lindblom, Sahlgren University Hospital, Molndal; Dr Lucian Vancea, Lanssjukhuset, Sundsvall.
Rights and permissions
About this article
Cite this article
Miglior, S., Grunden, J., Kwok, K. et al. Efficacy and safety of fixed combinations of latanoprost/timolol and dorzolamide/timolol in open-angle glaucoma or ocular hypertension. Eye 24, 1234–1242 (2010). https://doi.org/10.1038/eye.2009.307
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2009.307
Keywords
This article is cited by
-
Dorzolamide/Timolol Fixed Combination: Learning from the Past and Looking Toward the Future
Advances in Therapy (2021)
-
Repurposing Ophthalmologic Timolol for Dermatologic Use: Caveats and Historical Review of Adverse Events
American Journal of Clinical Dermatology (2021)
-
Twenty-four hour efficacy with the dorzolamide/timolol-fixed combination compared with the brimonidine/timolol-fixed combination in primary open-angle glaucoma
Eye (2012)