Abstract
Lesions of the caruncle are uncommon. On account of the histological composition of the caruncle, which includes, in addition to conjunctiva, hair follicles, sebaceous glands, sweat glands, and accessory lacrimal tissue, the caruncle may develop lesions that may be similar to those found in the skin, conjunctiva, or lacrimal gland. Clinical preoperative diagnosis is very difficult and reached only in about half of the cases. The vast majority of lesions of the caruncle are benign, mainly nevi. Reported malignant lesions are very rare but can be potentially fatal. Although malignancy is clinically overestimated, any suspected malignant lesion should be excised and examined histopathologically by an experienced pathologist. This study presents the clinical and histological data of 42 consecutive caruncular lesions processed at our laboratory and reviews previously reported cases of caruncular lesions.
Similar content being viewed by others
Introduction
The caruncle (from Latin caro=flesh) is a soft, pink, ovoid body, about 5 mm high and 3 mm broad, situated in the lacus lacrimalis medial to the plica semilunaris.1 It is more prominent on lateral gaze and is retracted on medial gaze.
Lesions of the caruncle are uncommon. On account of the fact that the caruncle harbours skin elements, such as hair follicles, sebaceous glands, sweat glands, and accessory lacrimal tissue, the lesions developing from the caruncle are very diverse, making their clinical diagnosis very difficult. The vast majority of lesions of the caruncle is benign, although rare malignant lesions have been also reported.
This study aims to present the clinical and histological data of 42 consecutive caruncular lesions processed at our laboratory and to review the relevant literature of caruncular lesions.
Materials and methods
Records from the Ophthalmic Pathology Laboratory at the Hadassah-Hebrew University Medical Centre, Jerusalem, Israel, between the years 1990 and 2007 were retrospectively reviewed. The following data were extracted from patients’ files: age at the time of excision, gender, affected eye, suspected clinical diagnosis, gross appearance and tumour dimensions, light microscopic findings, and postoperative complications. Forty-two cases of caruncular lesions were found.
Paraffin sections stained with haematoxylin and eosin were extracted and examined in all cases.
Results
A total of 11 104 records from the Ophthalmic Pathology Laboratory, Hadassah-Hebrew University Medical Centre, Jerusalem, Israel, between the years 1990 and 2007 were reviewed. Forty-two cases of caruncular lesions were found (frequency of 1 : 264, 0.4%).
Age at the time of excision ranged from 13 to 93 years (mean 39.3 years, median 35.5 years). There were 21 male patients and 21 female patients. The left eye was involved in 27 cases (64%).
Most patients presented with a slowly growing caruncular lesion. In three cases, a history of rapid growth was referred. Clinically, pigmented lesions were observed in 29 cases (69%). All cases presented with solitary lesions. No concurrent disorders were observed.
Clinical suspected diagnosis included pigmented lesion (20 cases, 48%), naevus (10 cases), caruncular tumour (three cases), caruncular lesion (two cases), basal cell carcinoma (two cases), granuloma (two cases), papilloma (one case), cyst (one case), and malignant lesion (one case).
All the lesions were completely removed. There were no intraoperative or postoperative complications. The largest dimensions of the lesion varied from 12 × 8 × 8 mm to 2.5 × 1 × 1 mm. Histological findings allowed definitive diagnosis in all cases. There were 40 benign lesions (95%). Clinical suspected diagnosis was correct in 20 cases (48%).
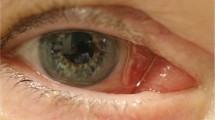
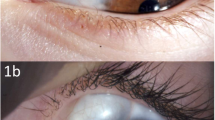
Nevi were the most frequent encountered group (25 cases, 60%). Ten of them (40%) were accurately diagnosed before biopsy. Incorrect or non-specific diagnoses included pigmented lesion (13 cases, 52%), caruncular lesion (one case), and basal cell carcinoma (one case). The mean age of the patients with nevi was 36.6 years (median of 35 years; range between 13–84 years) with a slightly male preponderance (15 cases, 60%). The left eye was affected in 18 cases (72%). The caruncular naevus characteristically appeared as a brown-pigmented mass (Figure 1a). Sometimes the lesion is non-pigmented (Figure 1b). Histopathologically, nests of benign melanocytic cells were found within the epithelium and susbtantia propria (compound naevus, 22 of 25 cases), or totally in the susbtantia propria (subepithelial naevus, 3 of 25 cases, Figure 1c). Other histological features included epithelial cyst formation (four cases), focal chronic inflammation (one case), marked chronic inflammation (one case), focal parakeratosis (one case), and focal area of primary acquired melanosis (PAM) with atypia (one case).
(a) Clinical appearance of a compound naevus in an 18-year-old patient with small surface cysts. (b) Clinical appearance of a non-pigmented large protruding naevus with overlying clear cysts in a 51-year-old patient. (c) Subepithelial naevus shown in Figure 1b. Nests of benign melanocytic cells (arrow), and cystic epithelial inclusions (asterisk) are detected at the substantia propria (haematoxylin and eosin, original magnification × 4).
In two cases, pigmentation of the basal layer of the epithelium without melanocytic hyperplasia or atypia, consistent with PAM without atypia, was detected (Figures 2a, b). In both cases, the suspected clinical diagnosis was a pigmented caruncular lesion. No cases of melanoma of the caruncle were detected in our laboratory.
Primary acquired melanosis without atypia. (a) Clinical appearance of the lesion in a 14-year-old patient. (b) Microscopic appearance of the same lesion. Increased number of melanocytes without melanocytic hyperplasia or atypia is detected at the basal layer of the epithelium (asterisk). Some melanophages (arrow) and chronic inflammation are found at the substantia propria (haematoxylin and eosin, original magnification × 20).
Three cases (7%) of squamous papilloma were found. From these three cases, a correct clinical diagnosis before the biopsy was made in one case; in the other two cases, a tumour and a pigmented lesion were suspected clinically. Patients’ age was 17, 29, and 54 years, respectively. Histopathologically, typical fibrovascular fronds with acanthotic epithelium were detected (Figure 3).
Oncocytoma was detected in three cases (7%). Patients were older than the average age in the entire group (57, 58, and 93 years, respectively). There were two female patients and one male patient. Suspected clinical diagnosis before biopsy was pigmented lesion in two cases and caruncular tumour growing steadily in one case. Microscopically, oncocytomas were composed of benign epithelial cells with abundant eosinophilic granular cytoplasm (Figure 4a and b).
Oncocytoma. (a) A cystic structure lined by several layers of eosinophilic cells with granular cytoplasm is identified at the substantia propria (arrow). The cyst is filled with seromucinous material (asterisk; haematoxylin and eosin, original magnification × 4). (b) The tumour is composed of columnar cells with eosinophilic cytoplasm and benign nuclei. No mitotic figures are observed. The central lumen shows an eosinophilic acellular material (asterisk; haematoxylin and eosin, original magnification × 40).
Non-specific chronic inflammation was observed in two cases (Figure 5a and b). Patients were older than the average age group (55 and 63 years, respectively). Preoperatively, these lesions were diagnosed as naevus and pigmented lesion, respectively.
One case of sebaceous gland hyperplasia and one case of sebaceous adenoma were observed (Figures 6andFigures 7). The suspected clinical diagnosis before the biopsy was granuloma and caruncular lesion, respectively. There were no cases of sebaceous gland carcinoma in our series.
One case of moderate epithelial dysplasia was found in our series. Clinically, a caruncular tumour was suspected in a 46-year-old female patient. Dysplastic changes were observed in the lower and middle thirds of the conjunctival epithelial thickness (Figure 8a and b).
Moderate epithelial dysplasia. (a) Sharp demarcation (arrow) between normal (black asterisk) and acanthotic dysplastic epithelium (white asterisk; haematoxylin and eosin, original magnification × 10). (b) Dysplastic changes are observed in the lower and middle thirds of the conjunctival epithelial thickness (double arrow; haematoxylin and eosin, original magnification × 20).
There was one case of solitary fibrous tumour. This case was previously reported in a 29-year-old patient.2 The lesion existed for at least 1 year. On examination, an elliptical pink mobile mass was detected at the lower fornix and caruncle (Figure 9a). It was composed mostly of spindle cells arranged randomly in a ‘patternless pattern’ (Figure 9b and c). Tumour cells were stained positively with CD34, O13 (CD99), BCL2, and vimentin, and negatively with S100 and α-actin.
Solitary fibrous tumour. (a) A large pink elliptical lesion is observed at the lower fornix and caruncle. (b) The tumour is covered by conjunctival epithelium (arrow) and composed of spindle cells and collagen fibres (haematoxylin and eosin, original magnification × 4). (c) Higher magnification shows spindle cells arranged randomly in a ‘patternless pattern’ with collagen fibres between them (haematoxylin and eosin, original magnification × 20).
One lesion was diagnosed as reactive lymphoid hyperplasia. Clinically, a cyst was suspected in a 19-year-old female patient. Histopathologically, the lesion was composed of a mixture of mature lymphocytes, plasma cells, and eosinophils (Figure 10).
In three cases, a malignancy was suspected clinically but confirmed histologically in two cases. In the two cases with malignant histological lesion (‘so-called’ malignant fibrous histiocytoma and basosquamous carcinoma), a malignancy was suspected clinically (basal cell carcinoma and ‘malignant lesion,’ respectively). The third case, an intradermal naevus, was incorrectly clinically diagnosed as basal cell carcinoma. The ‘so-called’ malignant fibrous histiocytoma was composed of round and spindle cells, showing a storiform pattern, marked cellular pleiomorphism, and mitotic figures (Figure 11). Numerous foamy macrophages were detected. The atypical cells stained positively for vimentin and negatively for HMB-45, α-actin, and LCA. The patient with basosquamous carcinoma was 67-year old. The tumour presented histopathological features of both basal cell and squamous cell carcinomas (Figure 12).
‘So-called’ malignant fibrous histiocytoma. The tumour is composed of round and spindle cells, showing a storiform pattern, marked cellular pleiomorphism, and mitotic figures (black arrow). Numerous foamy macrophages (white arrow) are also present (haematoxylin and eosin, original magnification × 40).
Discussion
The caruncle is modified skin, bearing goblet cells, and lacrimal tissue, in addition to hairs, sebaceous, and sweat glands.1 The epithelium is non-keratinized, stratified squamous similar to the conjunctival epithelium, and the sebaceous glands are like those of the lids and the hairs. Modified lacrimal glands (of Krause), surrounded by a thin layer of fat, are often conspicuous in the centre of the caruncle. The caruncle is supplied by the superior medial palpebral arteries, its lymphatics drain into the submandibular lymph nodes, and it is innervated by the infratrochlear nerve.1 The function of the caruncle is poorly understood.3 All mammals possess a caruncle, and it is usually larger than that found in humans. In the camel, the caruncle may occupy the entire medial canthus, and in the dog, the caruncle is large and contains numerous accessory lacrimal glands.3 The embryology of the caruncle also is not well understood.3 It is formed at the end of the third month of gestation after the eyelids have fused. It is believed to develop either secondary to cutting off of a portion of the lower eyelid with its appendages by the ingrowth of the lower canaliculus, or it is formed independently of the canaliculus by a cellular proliferation of the epithelium on the posterior surface of the nasal lower eyelid. The average distance between the external surface of the caruncle and the common canaliculus has been reported to be 0.85 mm, whereas the shortest distance measured is of 0.50 mm.4 Consequently, caution should be exercised when operations are performed on or near the caruncle to avoid inadvertent damage to the canalicular system.
The caruncle may develop a tumour or cyst that may be similar to one found in the skin, conjunctiva, or lacrimal gland. Lesions of the caruncle are reported to be uncommon. Since 1854, when von Graefe5 reported the first series of lesions of the caruncle, only a few reviews have been published, the majority of them reported more than 15 years ago.3, 6, 7, 8, 9, 10, 11, 12, 13 In our series, caruncular lesions represented only 0.4% of all surgical specimens submitted to our Ophthalmic Pathology Laboratory during the 18 years of the study. This incidence is in agreement with the incidences previously reported (0.3–1.1%).9, 10, 11, 13
Thirteen different histopathological types of lesions were identified in our series. This diversity is explained based on all the different tissues forming the caruncle. Table 1 shows the relative frequency of caruncular lesions in this study and in previously reported large series. In the majority of studies,9, 11, 13 as in this study, nevi constituted the largest group of caruncular lesions (average of 45.8%, range: 33.7–59.5% of lesions). However, other authors found a preponderance of papillomas6, 7, 10 or epithelial cysts8 in lesions removed from the caruncle. The majority of the lesions is benign. Except for the studies published before 1940, where a very high frequency of malignant lesions of up to 27% was found,6, 7 the rest of studies show that malignant caruncular lesions are very rare (average of 4.15% of total lesions; range: 2.7–5.4%). Preoperative clinical diagnosis is reported to be correct in only about half of cases (range: 37–52%),10, 11, 13 which is in concordance with our figures (48%). Coming up next, we present a detailed description of the reported lesions of the caruncle.
Congenital and developmental lesions
A number of developmental anomalies of the caruncle can seldom occur. Absence or hypoplasia and cleavage of the caruncle are almost always associated with other congenital anomalies.14 Hyperplasia of the caruncle is frequently associated with hyperplasia of the plica semilunaris, but a supernumerary caruncle seems to be invariably an isolated developmental anomaly, with only a few reports in the literature.14 It may be found in the lower or upper eyelid, and may be singular or multiple.15, 16 Supernumerary lacrimal punctum on the caruncle has also been reported.17 A supernumerary punctum connected to a supernumerary canaliculus and ending in a blind supernumerary sac is extremely rare.18 Caruncular abnormalities, including bilobed caruncles and ectopic caruncles, have been described in patients with Goldenhar syndrome,19 which is a congenital disorder believed to be caused by the defective development of the first and second brachial arches and the first brachial cleft during the fourth through eighth weeks of embryologic development.
Dermoid and epidermoid cysts can occur in the caruncle.20 Dermoid cysts are usually ovoid and yellowish.11 Both cysts are lined by squamous stratified epithelium, with skin appendages (sebaceous glands and hair follicles) in the case of dermoid cysts. Histopathologically, epidermoid cysts are indistinguishable from the epithelial inclusion cysts of squamous origin.
Inflammatory process
Several types of inflammatory processes have been described in the caruncle. Among them, the most frequent reported in the large series of caruncle lesions are chronic non-granulomatous inflammation, lipogranulomatous inflammation, and foreign body granuloma.6, 7, 9, 10, 11 Other exceptional inflammatory process described are methicillin-resistant Staphylococcus aureus caruncle abscess,21 inflammatory pseudotumor,22 involvement of the caruncle in ocular cicatricial pemphigoid,23 cytomegalovirus infection,24 molluscum contagiosum,25 spherulocystosis,26 and Armillifer armillatus infection.27
Secondary caruncular pigmentation
Silver deposits (argyrosis) on the eyelids, conjunctiva, and caruncle have been described after long-term application of readily available cosmetic eyelash tints.28 Similarly, patients receiving long-term topical eyedrops containing epinephrine compounds can develop pigmented deposits on the conjunctiva and caruncle.29
Epithelial lesions
Frequent benign skin lesions, such as seborrhoeic keratosis and actinic keratosis have been also reported in the caruncle.9, 10 A squamous caruncular horn with gradual enlargment in a 3-month infant has been described.30 On the basis of the similarities between this case and the tusks of elephants, the authors suggested that the caruncle can be a vestigial remnant of the upper incisor of lower animals.
Squamous papillomas are one of the three most frequent lesions of the caruncle and in some series, constitute the largest group of caruncular lesions.6, 7, 10 In our series, papillomas accounted for the second most frequent caruncular lesion, together with oncocytomas. A previous study found a strong association between conjunctival papillomas and certain types of human papilloma virus, mainly types 6 and 11.31 Viral aetiology has been proposed as a possible explanation for the variation in frequency between different series.12 Papillomas are usually described as a frond-like mass with fine vascular tufts visible clinically in the central core of each frond. They can be removed to rule out malignancy.10 Reported recurrence rates of conjunctival papillomas vary from 6 to 27%.32 Topical α-interferon has been used successfully for some recalcitrant cases.33 Inverted papillomas have been reported in the caruncular area, and they have a higher incidence of local invasion.34 They consist of fold of papillomatous epithelium that invaginate into the underlying stroma rather than growing in the pure exophytic fashion characteristic of the common squamous papilloma.34
Only one case of caruncular and a few cases of conjunctival keratoacanthoma have been described previously.13 Cutaneous keratoacanthoma typically shows rapid growth before undergoing spontaneous regression. The natural history of their conjunctival counterparts is unknown because of early excision.13 Some pathologists consider keratoacanthoma as a subtype of squamous cell carcinoma,35 so complete excision of the lesion is recommended.
Epithelial premalignant lesions, such as conjunctival epithelial dysplasia and carcinoma in situ in the caruncle are rarer than in the conjunctiva. We found only one case of moderate epithelial dysplasia, in which dysplastic changes were observed in the lower and middle thirds of the conjunctival epithelial thickness.
Basal cell carcinoma has been reported to affect the caruncle.13, 36, 37, 38, 39, 40 About 90% of the eyelid cancers are basal cell carcinomas and the conjunctiva is usually invaded secondarily from an eyelid tumour, with only very few cases of primary developing tumour at the caruncle, as it is a sun-exposed area. In our series, we found one case of basosquamous carcinoma in an old patient; the tumour presented histopathological features of both basal cell and squamous cell carcinomas. Basal cell carcinoma of the caruncle may originate from basal cells of the epithelium or infundibular cells of the hair follicles, or from pluripotent stem cells.37 Surgical removal of caruncular basal cell carcinoma with clear surgical margins can be sometimes difficult. Mohs’ micrographic surgery in selected cases may preserve more normal tissue than conventional surgery with less reported rates of recurrence.41 Radiation can be used as an adjuvant therapy to help reduce the chance of tumour recurrence or orbital invasion.36 Recurrences have been described even after complete excision, making long-term follow-up mandatory. Rare cases of squamous cell carcinoma,10, 42 adenosquamous carcinoma,43 mucoepidermoid carcinoma,44 and undifferentiated carcinoma45 of the caruncle have been also reported.
Cysts
Epithelial cysts are lesions frequently encountered at the caruncle,8, 11 and in one large series were the most frequent lesion removed from the caruncle.8 Other rare epithelial cysts described in the caruncle are apocrine hidrocystoma9 and steatocystoma.46, 47 In the former, the cyst is lined by an inner layer of low cuboidal secretory cells and an outer row of slightly flattened myoepithelial cells. The steatocystoma consists of a cyst lined by stratified squamous epithelium and containing sebaceous glands in its wall. Treatment consists of simple excision with removal of the cyst wall intact to reduce the risk of recurrence.
Melanocytic lesions
The majority of melanocytic lesions encountered at the caruncle are nevi. Nevi are the most frequent reported caruncular lesion in the majority of large series in the literature, as in ours, with frequency rates ranging between 33.7 and 59.5%.9, 11, 13 Classically, nevi appear near puberty and may show slight change in size or colour with time.10 Preoperative clinical diagnosis was accurate in 40% of our cases, but as suggested by Shields et al,10 in most instances, the lesions are removed for cosmetic reasons or to exclude the possibility of melanoma. If progressive changes in size, colour, or vascularity are noted, excision is recommended to rule out malignant transformation.
Simple caruncular freckles are rarely reported. The freckles are rarely subjected to biopsy because they are not usually confused with melanoma and they are not a cosmetic problem.10 Complexion-associated pigmentation (a better descriptive term for racial pigmentation) is also reported in the caruncle. Norn48 noted pigmentation of the plica semilunaris and/or lacrimal caruncle in 2% of 380 white north Europeans, in 4% of 189 Mongols, and in 45% of 257 Eskimos. In Eskimos, the phenomenon was found to be bilateral in 60% and confluent with pigmentation of the bulbar conjunctiva in 18%. The author concluded that caruncular pigmentation, like other pigmentation, is racially influenced. As in our series, the majority of reported nevi are of the compound type.49, 50, 51 Other less frequent types are subepithelial, combined, and blue nevi. At clinical examination, cysts are recognized in up to 65% of conjunctival nevi.49 In contrast, conjunctival melanoma rarely, if ever, displays intralesional cysts.49
PAM is less frequent encountered at the caruncle than nevi. In our series, we found two cases of PAM without atypia. PAM without atypia shows no progression to melanoma, whereas PAM with severe atypia shows progression to melanoma in up to 13% of cases.52, 53 Specifically, PAM recurrence is 3.53 times more frequent to occur in lesions affecting the caruncle than in cases without caruncular involvement.53 Lesions suspected clinically to be PAM at the caruncle should be excised.
Malignant melanoma has been reported to be the most prevalent malignant lesion of the caruncle. However, its occurrence on the caruncle is rare compared with its occurrence in the conjunctiva.13 It has been reported to occur in up to 17.5% of caruncular series in Evans’ series,7 although the majority of series show a rate of less than 4%.8, 9, 11, 13 This difference can be explained by the bias in collection of Evans’ cases, which came from many sources. Reported treatments for malignant melanoma of the caruncle include wide excision, adjuvant cryotherapy, and radiotherapy, or orbital exenteration for tumours with conjunctival, skin, and orbital extensions.13, 54 The caruncle is considered an ‘unfavourable’ location for conjunctival melanoma (together with palpebral, plica, and forniceal involvement, and opposed to ‘favourable’ location of bulbar conjunctiva and limbus), with an associated higher risk for melanoma recurrence and associated mortality.55, 56, 57, 58 The conjunctiva at the limbus is constituted of dense collagen preventing the penetration of the tumour. At the caruncle, the melanoma can more easily penetrate in depth and consequently cause lymphatic dissemination.59, 60
Sebaceous tumours
Sebaceous gland hyperplasia and adenoma are seldom reported at the caruncle.6, 7, 10, 11, 13, 61 Clinically, both lesions are similar and characterized by their yellow, nodular appearance, but they are distinguishable histopathologically. Sebaceous gland hyperplasia is characterized by hyperplastic lobules situated around a single duct; a normal cellular maturation sequence is observed.10 In the sebaceous gland adenoma, there is a loss of this maturation sequence.10
Sebaceous carcinoma rarely arises in the sebaceous glands of the caruncle.62, 63 It develops most often in the eyelids, usually from the meibomian glands of the tarsus and less often from the Zeis glands of the cilia. A recent study of 60 cases from a tertiary centre revealed a single case arising from the sebaceous glands of the caruncle.63 However, the caruncle may be affected in up to 25% of cases of eyelid sebaceous carcinoma.64 The clinical differential diagnosis of sebaceous carcinoma of the caruncle is different from those of the eyelids and includes sebaceous hyperplasia and adenoma, oncocytma, squamous cell carcinoma, naevus, and papilloma.63 The tumour should be removed with clear margins as wide as possible. Extensive cryotherapy, conjunctival reconstruction, and map biopsies to rule out subclinical pagetoid spread should be performed.63, 65
Oncocytoma
Oncocytoma (oxyphil cell adenoma) is a rare but typical caruncular tumour with a reported frequency of about 3.5% of caruncular lesions.9, 10, 13 In our series, we found three cases of caruncular oncocytoma (7.1% of cases). Benign oncocytomas arising in the ocular adnexa have been described in the lacrimal gland, lacrimal sac, plica semilunaris, bulbar conjunctiva, upper and lower fornices, mucocutaneous junction, and caruncle.66, 67, 68, 69, 70 Of these, the caruncular oncocytoma is by far the commonest, but it is still a rare lesion. Oncocytomas of the caruncle are more frequent in elderly women, as in our series. Its natural history is of a slowly growing painless mass. In spite of its rarity, the diagnosis should be considered when there is a caruncular swelling, particularly if the lesion appears cystic or has a bright cherry red colour. Microscopically, oncocytomas are composed of benign epithelial cells with abundant eosinophilic granular cytoplasm, which is found on ultrastructural examination to be composed of altered mitochondria. The histogenesis of caruncular oncocytomas has been reviewed by Rennie66 who believed that the lesion arises from glands or their secretory ducts. Clinically, aggressive behaviour has not been documented in oncocytomas arising in the caruncle, whereas in other locations have indeed behaved aggressively.70
Sweat gland tumours
Benign sweat gland tumours (for example, hidrocystoma) have been already described. A very rare case of malignant apocrine sweat gland carcinoma of the caruncle in a young patient who underwent exenteration has been reported.71
Myeloproliferative disorders
Myeloproliferative disorders have been extensively described in the ocular adnexa72, 73, 74 and rarely affect the caruncle. In some series of caruncular lesions, the most common lesion was benign lymphoid hyperplasia,9, 11 with a reported frequency of about 3% of all caruncular lesions, similar to our experience. However, in large series of conjunctival lymphoid lesions, lymphoma was detected in 56% of 117 cases and benign lymphoid hyperplasia in 17% of cases. Only 7% of the 117 cases of conjunctival lymphoid lesions occurred at the caruncle.72
Typical clinical presentation is of a slow growing salmon coloured lesion, but definite diagnosis requires always tissue biopsy. Isolated case reports of caruncular myeloproliferative lesions include benign lymphoid hyperplasia,75, 76, 77 lymphoma,78 Langerhans cell histiocytosis,79, 80 and granulocytic sarcoma.81
Lymphoid tumours of the conjunctiva are reported to be associated with systemic lymphoma in 31% of patients. Systemic lymphoma is found more often in those patients with forniceal or midbulbar conjunctival involvement, and in those with multiple conjunctival tumours.72 The authors advised the long-term systemic follow-up, because related systemic lymphoma can manifest many years later.72
Vascular lesions
Pyogenic granuloma is the most frequent vascular lesion with a reported rate ranging between 1.7 and 8.8% of caruncular lesions.8, 10, 11, 13 Pyogenic granuloma of the caruncle appears as a fleshy vascular mass usually after surgical or accidental trauma.10 It may resolve on its own or after application of steroid drops. Shields et al10 described two cases occurring after medial rectus muscle surgery for strabismus. Medial rectus muscle surgery may lead to granulation tissue in the caruncle because the medial rectus sheath has fibres that penetrate the deep structures of the caruncle.
Other reported vascular lesions at the caruncle are capillary hemangioma,9, 13 cavernous hemangioma,9, 11, 13 lymphangiectasia,10 lymphangioma,82 and Kaposi sarcoma.83
Neural tumours
Exceptional cases of neurofibroma,7, 84 neurilemoma (schwannoma), either isolated85 or as part as Carney complex86 (myxomas, spotty pigmentation, endocrine overactivity, and conjunctival schwannomas), and granular cell tumour9, 87 have been reported in the literature.
Myogenic tumours
Only one case of primary leiomyoma affecting the caruncle has been reported in the literature.88 The authors suggested that the origin of the lesion was either from pericytes or from the medial part of the capsulo–palpebral muscle of Hesser.
Fibrous and fibrohistiocytic tumours
Rare cases of fibroma,6, 7, 8, 11 fibrolipoma,8, 11 solitary fibrous tumour,2 and ‘so-called’ malignant fibrous histiocytoma89 have been reported in the caruncle. These lesions are much less frequent that their counterparts affecting the eyelids, orbit, or conjunctiva. Interestingly, and in spite of their rarity, we found one case of solitary fibrous tumour (previously reported),2 and one case of ‘so-called’ malignant fibrous histiocytoma in our series.
Metastatic tumours
Only one case of caruncle tumour as presenting metastatic carcinoid tumour90 and other case of caruncle tumour as the first sign of metastatic lung carcinoma91 have been reported previously. The presence of a conjunctival mass in patients with known prior malignancy and associated ocular and systemic metastases is suggestive of a metastatic lesion.92 Conjunctival metastases represent a very bad prognostic sign for the patient; in addition to the high incidence of metastatic disease in other organs, the mean survival time from diagnosis is reported to be only about 9 months.92
Conclusion
Lesions of the caruncle are uncommon and very diverse, which makes clinical diagnosis very difficult. Reported preoperative diagnosis is correct only in about half of the cases, which is explained by the large pathologic variety of lesions encountered at the caruncle. Nevi are the most frequent reported lesions. Malignant lesions are very uncommon. Although there is a reported clinical overestimation of malignancy, malignant lesions can be fatal. Any change in colour, size, or vascularization of a caruncular lesion should be excised. Pathological examination should be mandatory. On account of the enormous variety of reported cases, close collaboration between eye pathologists, dermatopathologists, surgical pathologists, and soft tissue pathologists may be needed in selected difficult cases.
Method of literature search
A search of the PubMed database 1966–2007 was conducted using various combinations of the key words such as caruncle, caruncular, lesion, tumour, and conjunctiva. Articles in all languages were considered, provided that the non-English articles included English abstracts. Relevant articles that were cited in the reference lists of the retrieved articles were also included.
References
Bron AJ, Tripathi RC, Tripathi BJ . Wolff's Anatomy of the Eye and Orbit, 18th edn. Chapman and Hall Medical: Spain, 1997 pp 70–71.
Pe’er J, Maly A, Deckel Y, Frenkel S . Solitary fibrous tumor of the conjunctiva. Arch Ophthalmol 2007; 125: 423–426.
Shields CL, Shields JA . Tumors of the caruncle. Int Ophthalmol Clin 1993; 33: 31–36.
Kathuria SS, Howarth D, Hurwitz JJ, Oestreicher J . An anatomic and histologic study of the caruncle. Ophthal Plast Reconstr Surg 1999; 15: 407–411.
von Graefe A . Geschwülste der Tränenkarunkel. Arch Ophthalmol 1854; 1: 289–291.
Serra GM . Tumori della caruncola lacrimale. Studio clinico ed anatomo patologico-casistica. Boll Ocul 1928; 7: 783–802.
Evans WH . Tumors of the lacrimal caruncle. A study of 200 collected cases. Arch Ophthalmol 1940; 24: 83–106.
Wilson RP . Tumours and cysts of the lacrimal caruncle. Trans Ophthalmol Soc N Z 1959; 11: 23–32.
Luthra CL, Doxanas MT, Green WR . Lesions of the caruncle: a clinicohistopathologic study. Surv Ophthalmol 1978; 23: 183–195.
Shields CL, Shields JA, White D, Augsburger JJ . Types and frequency of lesions of the caruncle. Am J Ophthalmol 1986; 102: 771–778.
Santos A, Gómez-Leal A . Lesions of the lacrimal caruncle. Clinicopathologic features. Ophthalmology 1994; 101: 943–949.
Østergard J, Prause JU, Heegaard S . Caruncular lesions in Denmark 1978–2002: a histopatholgical study with correlation to clinical referral diagnosis. Acta Ophthalmol Scand 2006; 84: 130–136.
Kaeser PF, Uffer S, Zografos L, Hamédani M . Tumors of the caruncle: a clinicopathologic correlation. Am J Ophthalmol 2006; 142: 448–455.
Mansour K, van Bijsterveld OP . Supernumerary caruncle: report of a case. Ann Ophthalmol 1984; 16: 677–678.
Duke-Elder S . Congenital anomalies of the ocular adnexa: the eyelids. In: Duke-Elder S (ed). System of Ophthalmology. Henry Kimpton: London, England, 1964; 861–862.
Zamir E, Banin E, Chowers I, Arnon N, Pe’er J . Ectopic caruncle. Arch Ophthalmol 1999; 117: 1446–1447.
Nirankari MS, Chaddah MR . Supernumerary punctum on the caruncle. Br J Ophthalmol 1962; 46: 380–381.
Mansour K, Versteegh M, Janssen A, Blanksma L . Epiphora due to compression of the lacrimal sac by a supernumerary blind sac. Orbit 2002; 21: 43–47.
Nijhawan N, Morad Y, Seigel-Bartelt J, Levin AV . Caruncle abnormalities in the oculo-auriculo-vertebral spectrum. Am J Med Genet 2002; 113: 320–325.
Ghafouri A, Rodgers IR, Perry HD . A caruncular dermoid with contiguous eyelid involvement: embryologic implications. Ophthal Plast Reconstr Surg 1998; 14: 375–377.
Koo L, Chang EL . Methicillin-resistant Staphylococcus aureus caruncle abscess. Ophthal Plast Reconstr Surg 2007; 23: 160–161.
D’Hermies F, Validire P, Meyer A, Morel X, Halhal M, Elmaleh C et al. Inflammatory pseudotumor of the caruncle. J Fr Ophtalmol 2003; 26: 204–207.
Murube J, Chenzhuo L, Murube E, Rivas L, Shalaby O . Measuring the lacunar sulci as a new indicator of shrinkage of the ocular surface. Eur J Ophthalmol 2001; 11: 227–232.
España-Gregori E, Vera-Sempere FJ, Cano-Parra J, Ramos-Fernandez V, Navea-Tejerina A, Díaz-Llopis M . Cytomegalovirus infection of the caruncle in the acquired immunodeficiency syndrome. Am J Ophthalmol 1994; 117: 406–407.
Vannas S, Lapinleimu K . Molluscum contagiosum in the skin, caruncle, and conjunctiva: detection of a cytopathic agent in tissue culture. Acta Ophthalmol (Copenh) 1967; 45: 314–321.
Kini U, Babu MK . Ocular spherulocystosis. J Clin Pathol 1996; 49: 857–858.
Polderman AM, Manschot WA . Armillifer armillatus located within the lacrimal caruncle. Acta Leiden 1979; 47: 71–77.
Gallardo MJ, Randleman JB, Price KM, Johnson DA, Acosta S, Grossniklaus HE et al. Ocular argyrosis after long-term self-application of eyelash tint. Am J Ophthalmol 2006; 141: 198–200.
Spencer WH . Conjunctiva. In: Spencer WH (ed). Ophthalmic Pathology: An Atlas and Textbook. WB Saunders: Philadelphia, 1996; 97.
Dhir SP, Shishku MN, Krewi A . Ocular horn. Br J Ophthalmol 1989; 73: 317–318.
Sjö NC, Heegaard S, Prause JU, von Buchald C, Lindeberg H . Human papillomavirus in conjunctival papilloma. Br J Ophthalmol 2001; 85: 785–787.
Sjö NC, Heegaard S, Prause JU . Conjunctival papilloma. A histopathologically based retrospective study. Acta Ophthalmol Scand 2000; 78: 663–666.
de Keizer RJW, de Wolff-Rouendaal D . Topical α-interferon in recurrent conjunctival papilloma. Acta Ophthalmol Scand 2003; 81: 193–196.
Streeten BW, Carrillo R, Jamison R, Brownstein S, Font RL, Zimmerman LE . Inverted papilloma of the conjunctiva. Am J Ophthalmol 1979; 88: 1062–1066.
Hodak E, Jones RE, Ackerman AB . Solitary keratoacanthoma is a squamous-cell carcinoma: three examples with metastases. Am J Dermatopathol 1993; 15: 332–342; discussion 343–352.
Rossman D, Arthurs B, Odashiro A, Saraiva V, Burnier Jr M . Basal cell carcinoma of the caruncle. Ophthal Plast Reconstr Surg 2006; 22: 313–314.
stergaard J, Boberg-Ans J, Prause JU, Heegaard S . Primary basal cell carcinoma of the caruncle with seeding to the conjunctiva. Graefes Arch Clin Exp Ophthalmol 2005; 243: 615–618.
Meier P, Sterker I, Meier T . Primary basal cell carcinoma of the caruncle. Arch Ophthalmol 1998; 116: 1373–1374.
Poon A, Sloan B, McKelvie P, Davies R . Primary basal cell carcinoma of the caruncle. Arch Ophthalmol 1997; 115: 1585–1587.
Mencía-Gutiérrez E, Gutiérrez-Díaz E, Pérez-Martín ME . Lacrimal caruncle primary basal cell carcinoma: case report and review. J Cutan Pathol 2005; 32: 502–505.
Lindgren G, Lindblom B, Larkö O . Mohs’ micrographic surgery for basal cell carcinomas on the eyelids and medical canthal area. II. Reconstruction and follow-up. Acta Ophthalmol Scand 2000; 78: 430–436.
Dithmar S, Schütt F, Völcker HE . Papillary plica/caruncle tumor. Squamous epithelial carcinoma of the conjunctiva associated with human papillomavirus type 16. Ophthalmologe 2002; 99: 118–119.
Nylander AG, Atta HR . Adenosquamous carcinoma of the lacrimal caruncle: a case report. Br J Ophthalmol 1986; 70: 864–866.
Rodman RC, Frueh BR, Elner VM . Mucoepidermoid carcinoma of the caruncle. Am J Ophthalmol 1997; 123: 564–565.
Lam DS, To KF, Fan DS, Cheuk W . An uncommon malignant neoplasm of the caruncle: report of a case of undifferentiated carcinoma. Arch Ophthalmol 1998; 116: 374–376.
Bowyer J, Sullivan T, Whitehead K . Steatocystoma simplex of the caruncle. Br J Ophthalmol 2003; 87: 240–241.
Kim NJ, Moon KC, Khwarg SI . Steatocystoma simplex of the caruncle. Can J Ophthalmol 2006; 41: 83–85.
Norn M . Pigmentation of plica and lacrymal caruncle. Prevalence among Caucasians, Eskimos, and Japanese. Acta Ophthalmol (Copenh) 1984; 62: 939–943.
Shields CL, Fasiuddin AF, Mashayekhi A, Shields JA . Conjunctival nevi: clinical features and natural course in 410 consecutive patients. Arch Ophthalmol 2004; 122: 167–175.
Gerner N, Nørregaard JC, Jensen OA, Prause JU . Conjunctival naevi in Denmark 1960–1980. A 21-year follow-up study. Acta Ophthalmol Scand 1996; 74: 334–337.
Shields CL, Demirci H, Karatza E, Shields JA . Clinical survey of 1643 melanocytic and nonmelanocytic conjunctival tumors. Ophthalmology 2004; 111: 1747–1754.
Jakobiec FA, Folberg R, Iwamoto T . Clinicopathologic characteristics of premalignant and malignant melanocytic lesions of the conjunctiva. Ophthalmology 1989; 96: 147–166.
Shields JA, Shields CL, Mashayekhi A, Marr BP, Benavides R, Thangappan A et al. Primary acquired melanosis of the conjunctiva: risks for progression to melanoma in 311 eyes. The 2006 Lorenz E. Zimmerman lecture. Ophthalmology 2008; 115: 511–519.
Hamilton RS . Two cases of malignant melanoma of the lids, conjunctiva, and caruncle. Trans Am Ophthalmol Soc 1968; 66: 394–415.
Paridaens AD, Minassian DC, McCartney AC, Hungerford JL . Prognostic factors in primary malignant melanoma of the conjunctiva: a clinicopathological study of 256 cases. Br J Ophthalmol 1994; 78: 252–259.
Anastassiou G, Heiligenhaus A, Bechrakis N, Bader E, Bornfeld N, Steuhl KP . Prognostic value of clinical and histopathological parameters in conjunctival melanomas: a retrospective study. Br J Ophthalmol 2002; 86: 163–167.
Shields CL . Conjunctival melanoma. Br J Ophthalmol 2002; 86: 127.
Shields CL, Shields JA, Gündüz K, Cater J, Mercado GV, Gross N et al. Conjunctival melanoma: risk factors for recurrence, exenteration, metastasis, and death in 150 consecutive patients. Arch Ophthalmol 2000; 118: 1497–1507.
Zimmerman LE, Maumenee AE, Reese AB . Discussion of pigmented tumors of the conjunctiva. In: Boniuk M (ed). Ocular and Adnexal Tumors. C.V. Mosby Company: St Louis, 1964.
Kodjikian L, Devouassoux M, Grange JD . Pigmented tumors of the caruncle. Review of the literature. J Fr Ophtalmol 1999; 22: 688–699.
Massry GG, Holds JB, Kincaid MC, Patrinely JR . Sebaceous gland hyperplasia of the caruncle. Ophthal Plast Reconstr Surg 1995; 11: 32–36.
Shields JA, Shields CL, Marr BP, Eagle Jr RC . Sebaceous carcinoma of the caruncle. Cornea 2006; 25: 858–859.
Shields JA, Demirci H, Marr BP, Eagle Jr RC, Shields CL . Sebaceous carcinoma of the eyelids: personal experience with 60 cases. Ophthalmology 2004; 111: 2151–2157.
Shields JA, Demirci H, Marr BP, Eagle Jr RC, Stefanyszyn M, Shields CL . Conjunctival epithelial involvement by eyelid sebaceous carcinoma. The 2003 J. Howard Stokes lecture. Ophthal Plast Reconstr Surg 2005; 21: 92–96.
Shields JA, Demirci H, Marr BP, Eagle Jr RC, Shields CL . Sebaceous carcinoma of the ocular region: a review. Surv Ophthalmol 2005; 50: 103–122.
Rennie IG . Oncocytomas (oxyphil adenomas) of the lacrimal caruncle. Br J Ophthalmol 1980; 64: 935–939.
Shields CL, Shields JA, Arbizo V, Augsburger JJ . Oncocytoma of the caruncle. Am J Ophthalmol 1986; 102: 315–319.
Morgan MB, Truitt CA, Romer C, Somach S, Pitha JV . Ocular adnexal oncocytoma: a case series and clinicopathologic review of the literature. Am J Dermatopathol 1998; 20: 487–490.
Rodgers IR, Jakobiec FA, Krebs W, Hornblass A, Gingold MP . Papillary oncocytoma of the eyelid. A previously undescribed tumor of apocrine gland origin. Ophthalmology 1988; 95: 1071–1076.
George E, Swanson PE, Newman BK, Wick MR . Oculocutaneous oncocytic tumors: clinicopathologic and immunohistochemical study of 2 cases with literature review. Am J Dermatopathol 2007; 29: 279–285.
Duke TG, Fahy GT, Brown LJ . Malignant apocrine sweat gland carcinoma of the caruncle. Orbit 2000; 19: 7–11.
Shields CL, Shields JA, Carvalho C, Rundle P, Smith AF . Conjunctival lymphoid tumors: clinical analysis of 117 cases and relationship to systemic lymphoma. Ophthalmology 2001; 108: 979–984.
Cockerham GC, Jakobiec FA . Lymphoproliferative disorders of the ocular adnexa. Int Ophthalmol Clin 1997; 37: 39–59.
Coupland SE, Krause L, Delecluse HJ, Anagnostopoulos I, Foss HD, Hummel M et al. Lymphoproliferative lesions of the ocular adnexa. Analysis of 112 cases. Ophthalmology 1998; 105: 1430–1441.
Tang J, Rodgers IR, Basham KL, Goh J . Rare case of exuberant benign lymphoid hyperplasia involving the conjunctiva, caruncle, and plica in a child with tonsilar enlargement. J AAPOS 2003; 7: 293–294.
Telander DG, Lee TZ, Pambuccian SE, Huang AJ . Subconjunctival corticosteroids for benign lymphoid hyperplasia. Br J Ophthalmol 2005; 89: 770–771.
Reddy S, Finger PT, Chynn EW, Iacob CE . Reactive lymphoid hyperplasia 1 month after LASIK surgery. Graefes Arch Clin Exp Ophthalmol 2006; 244: 262–264.
Chang YC, Chang CH, Liu YT, Tsai KB, Liu TC, Lin YN . Spontaneous regression of a large-cell lymphoma in the conjunctiva and orbit. Ophthal Plast Reconstr Surg 2004; 20: 461–463.
Kiratli H, Kocabeyoğlu S, Sağlam A, Söylemezoğlu F . Langerhans cell histiocytosis of the caruncle. Clin Experiment Ophthalmol 2007; 35: 661–663.
Stanowsky A, Krey HF, Wagner T . Histiocytosis X (eosinophilic granuloma) of the caruncle. Klin Monatsbl Augenheilkd 1991; 199: 359–361.
Yaghouti F, Nouri M, Mannor GE . Ocular adnexal granulocytic sarcoma as the first sign of acute myelogenous leukemia relapse. Am J Ophthalmol 1999; 127: 361–363.
Kafil-Hussain N, Khooshabeh R, Graham C . Superficial adnexal lymphangioma. Orbit 2005; 24: 141–143.
Hirsch C, Holz FG, Tetz M, Völcker HE . Clinical aspects and histopathology of caruncular tumors. Klin Monatsbl Augenheilkd 1997; 210: 153–157.
Freedman KA, Tran RM . Neurofibroma involving the caruncle. Arch Ophthalmol 2004; 122: 294–295.
Rennie IG, Parsons MA, Benson MT . Neurilemoma of the caruncle: a clinicopathological report. Br J Ophthalmol 1991; 75: 749–751.
Carney JA . Carney complex: the complex of myxomas, spotty pigmentation, endocrine overactivity, and schwannomas. Semin Dermatol 1995; 14: 90–98.
Evans M, Chang E, Yu DL, Rao NA . Granular cell tumour: a rare caruncle lesion. Br J Ophthalmol 2006; 90: 246–247.
Heegaard S, Prause JU . Leiomyoma of the caruncle. Acta Ophthalmol Scand 1998; 76: 731–733.
Allaire GS, Corriveau C, Teboul N . Malignant fibrous histiocytoma of the conjunctiva. Arch Ophthalmol 1999; 117: 685–687.
Gritz DC, Rao NA . Metastatic carcinoid tumor diagnosis from a caruncular mass. Am J Ophthalmol 1991; 112: 470–472.
Lie A, Mooy C, van den Bosch W, Paridaens D . Caruncle tumor as the first sign of metastatic lung carcinoma. Am J Ophthalmol 2002; 134: 438–439.
Kiratli H, Shields CL, Shields JA, DePotter P . Metastatic tumours to the conjunctiva: report of 10 cases. Br J Ophthalmol 1996; 80: 5–8.
Acknowledgements
We thank Mr Israel Barzel for the clinical pictures of the patients.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Levy, J., Ilsar, M., Deckel, Y. et al. Lesions of the caruncle: a description of 42 cases and a review of the literature. Eye 23, 1004–1018 (2009). https://doi.org/10.1038/eye.2008.316
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/eye.2008.316