Abstract
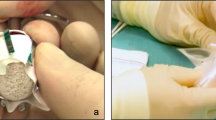
Purpose The hydroxyapatite orbital implant has been introduced as a buried, integrated implant for use in the anophthalmic patient. The second stage of the procedure involves drilling the implant and inserting a motility peg that allows direct coupling of the artificial eye to the implant. Other authors have advocated an assessment of implant vascularity by imaging prior to drilling. We aimed to see whether our practice of drilling after a predetermined time interval without assessment of implant vascularity would result in a higher complication rate. We also aimed to determine how successful the drilling procedure was in improving both the motility and the stability of the artificial eye.
Methods The notes of 41 consecutive patients who underwent drilling were studied to determine the time interval between implantation with a hydroxyapatite sphere and drilling the nature of any complications and any further surgical procedures undertaken. A postal questionnaire was sent to all patients asking them to grade the motility of their implant before and after drilling, and to state whether or not there had been any improvement in the stability of their artificial eye.
Results The most frequent complication encountered was extrusion of the motility peg, which occurred in 3 patients. A total of 5 patients required redrilling. There was an 80% response rate to the questionnaire. Ninety-one per cent of patients felt that there had been an improvement in the motility of their artificial eye and 76% felt that the stability of their artificial eye had been improved.
Conclusion Pegging of the hydroxyapatite implant improves both the motility and the stability of the artificial eye in the majority of cases. Complications are infrequent and minor. If sufficient time is allowed after implantation for full implant vascularity to occur, it is not necessary to perform imaging studies. This practice does not result in an increase in complications, and significantly reduces the expense of the procedure.
Similar content being viewed by others
Article PDF
References
Shields CL, Shields JA, De Potter P, Singh AD . Problems with the hydroxyapatite orbital implant: experience with 250 consecutive cases. Br J Ophthalmol 1994;78:702–6.
Ashworth JL, Rhatighan M, Sampath R, Brammar R, Sunderland S, Leatherbarrow B . The hydroxyapatite orbital implant: a prospective study. Eye 1996;10:29–37.
Perry AC . Advances in enucleation. Ophthalmic Clin North Am 1991;1:173–82.
Ferrone PJ, Dutton JJ . Rate of vascularisation of coralline hydroxyapatite ocular implants. Ophthalmology 1992;99:376–9.
De Potter P, Shields CL, Shields JA . The role of magnetic resonance imaging in the evaluation of the hydroxyapatite orbital implant. Ophthalmology 1992;99:824–30.
Dutton JJ . Coralline hydroxyapatite as an ocular implant. Ophthalmology 1991;98:370–7.
De Potter, Shields CL, Shields JA, Singh AD . Use of the hydroxyapatite ocular implant in the pediatric population. Arch Ophthalmol 1994;112:208–12.
Shields CL, Shields JA, De Potter P . Hydroxyapatite orbital implant after enucleation. Arch Ophthalmol 1992;110:333–8.
Shields JA, Shields CL, De Potter P . Hydroxyapatite orbital implant after enucleation: experience with 200 cases. Mayo Clin Proc 1993;68:1191–5.
Goldberg RA, Holds JB, Ebrahimpour J . Exposed hydroxyapatite orbital implants: a report of six cases. Ophthalmology 1992;99:831–6.
Kim Y-D, Goldberg RA, Shorr N, Steinsapir KD . Management of exposed hydroxyapatite orbital implants. Ophthalmology 1994;101:1709–15.
Buettner H, Bartley GB . Tissue breakdown and exposure associated with orbital hydroxyapatite implants. Am J Ophthalmol 1992;113:669–73.
Leatherbarrow B, Kwartz J, Sunderland S, Brammar R, Nichol E . The ‘baseball’ orbital implant: a prospective study. Eye 1994;8:569–76.
Tyers AG, Collin JRO . Baseball orbital implants: a review of 39 patients. Br J Ophthalmol 1985;69:438–42.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Ashworth, J., Brammar, R., Inkster, C. et al. A study of the hydroxyapatite orbital implant drilling procedure. Eye 12, 37–42 (1998). https://doi.org/10.1038/eye.1998.6
Issue Date:
DOI: https://doi.org/10.1038/eye.1998.6