Abstract
Intestinal ischemia-reperfusion (I/R) is an important event in the pathogenesis of multiple organ dysfunction syndrome (MODS). The aim of this study is to determine the effects of ginsenoside Rb1 on liver injury induced by intestinal I/R in rats. Adult male Wistar rats were randomly divided into four groups: (1) a control, sham-operated group (sham group); (2) an intestinal I/R group subjected to 1 h intestinal ischemia and 2 h reperfusion (I/R group); (3) a group treated with 20 mg/kg ginsenoside Rb1 before reperfusion (Rb1-20 group); and (4) a group treated with 40 mg/kg ginsenoside Rb1 before reperfusion (Rb1-40 group). Liver and intestinal histology was observed. Aspartate aminotransferase (AST), alanine aminotransferase (ALT) level in serum and malondialdehyde (MDA) level in intestinal tissues were measured. Myeloperoxidase (MPO), TNF-α, MDA level and immunohistochemical expression of NF-κB and intracellular adhesion molecale-1 (ICAM-1) in liver tissues was assayed. In addition, a western blot analysis of liver NF-κB expression was performed. Results indicated intestinal I/R induced intestinal and liver injury, which was characterized by increase of AST and ALT in serum, MDA level in intestine, MPO, TNF-α and MDA level and ICAM-1 and NF-κB expression in the liver tissues. Ginsenoside Rb1 (20, 40 mg/kg) ameliorated liver injury, decreased MPO, TNF-α and MDA level, NF-κB and ICAM-1 expression in liver tissues. In conclusion, ginsenoside Rb1 ablated liver injury induced by intestinal I/R by inhibiting NF-κB activation.
Similar content being viewed by others
Introduction
Intestinal ischemia-reperfusion (I/R) is an important event in the pathogenesis of multiple organ dysfunction syndrome (MODS) (Antonsson et al., 1991; Poggetti et al., 1992a; Turnage et al., 1996; Pierro et al., 2004). Although ischemia by itself induces little damage, reperfusion of the previously ischemic organ can yield to remote organ injury and life threatening multiple organ failure (Poggetti et al., 1992b; Amersi et al., 1999). The liver is the first organ injured and the important 'distance' organ affected by intestinal I/R because of the washout of toxic substances from the reperfused intestine (Horie et al., 1996; Horie et al., 2001; Leister et al., 2002). However, the mechanisms responsible for the liver injury caused by intestinal I/R are not clearly defined.
The pathogenesis of multiple organ failure after intestinal I/R is multifactorial, but the development of oxidative injury with a subsequent systemic inflammatory response appears to play a pivotal role (Cuzzocrea et al., 2000; Kalia et al., 2001). Oxidants and inflammatory mediators such as oxygen-derived free radicals, neutrophils and cytokines have been considered to exert their effects via a direct toxic action on target cells. However, recent studies have shown that these mediators are regulated by NF-κB family of transcription factors, which is a key regulator of inflammatory gene expression. It has been shown that NF-κB plays an important role in intestinal I/R (Yao et al., 2007).
Ginsenosides, which are glycosides containing an aglycone (protopanaxadiol or protopanaxatriol) with a dammarane skeleton, are the major effective components of ginseng and have been shown to have a wide variety of biological activities including immunomodulatory effects, antioxidant, anti-inflammatory and anti-tumor activity (Kenarova et al., 1990; Attele et al., 1999; Shibata, 2001; Park et al., 2003).
Ginsenosides are normally fractioned into two groups based on the types of aglycone, namely the panaxadiol group (e.g., Rb1 and Rc) and the panaxatriol group (e.g., Rg1 and Re). Ginsenoside Rb1 (Rb1), one of the panaxadiols, has a beneficial effects on lung, cerebral and cardiomyocyte I/R injury (Zeng et al., 2003; Geng et al., 2005; Li et al., 2005). But effect of Rb1 on intestinal I/R injury and liver injury induced by intestinal I/R has not been reported. In this paper, we used intestinal I/R model to investigate the influence of Rb1 on liver injury and NF-κB activity induced by intestinal I/R.
Materials and Methods
Materials
Adult male Wistar rats, weighing 220-250g, were obtained from Experimental Animal Center of Tongji Medical College, Grade II, and Certificate No 19-050. This study complies with the European Community Guidelines for the Care and Use of Experimental Animals and was approved by the Animal Research Committee of Tongji Medical College of Huazhong University of Science and Technology (Wuhan, China). Rb1 (99.5%) were obtained from the Research Center of Traditional Chinese Medicine (Wuhan, China) and dissolved in saline. The aspartate aminotransferase (AST) and alanine aminotransferase (ALT) kits were obtained from AusBio Laboratories (Beijing, China). The malondialdehyde (MDA) and myeloperoxidase (MPO) assay kits were obtained from Nanjing Jiancheng Bioengineering Institute (Nanjing, China). TNF-α ELISA assay kit was obtained from R&D Systems, Inc (Minneapdis, MN). Antibodies for NF-κB and α-actin were purchased from Santa Cruz Biotechnology, Inc (Santa Cruz, CA). Nuclear Extract Kit was purchased from Active Motif, Inc (Carlsbad, CA). Antibody for ICAM-1 was purchased from Boster Biological Technology (Wuhan, China). All other chemicals used were of the highest grade available commercially. The molecule structure of Rb1 is shown in Figure 1.
Experimental protocol
The animals were anesthetized with sodium pentobarbital (50 mg/kg) intraperitoneally. The intestinal I/R model was established by SMA occlusion. Rats were assigned randomly into one of four experimental groups (n = 10 in each group) as follows: (1) a control, sham-operated group (sham group) that underwent isolation of the SMA without occlusion; (2) an intestinal I/R group (I/R group) subjected to 1 h intestinal ischemia and 2 h reperfusion after the SMA had been isolated and occluded (Megison et al., 1990) with administration of 10 ml/kg saline intraperitoneally before reperfusion; (3) a 20 mg/kg Ginsenoside Rb1 (2 mg/ml, dissolved in saline, 10ml/kg) treated group (Rb1-20 group), in which surgery was performed as in the intestinal I/R group with administration of 10 ml/kg 2% Ginsenoside Rb1 intraperitoneally before reperfusion; and (4) a 40 mg/kg Ginsenoside Rb1 (4 mg/ml, dissolved in saline, 10 ml/kg) treated group (Rb1-40 group), in which surgery was performed as in the intestinal I/R group with administration of 10 ml/kg 4% Ginsenoside Rb1 intraperitoneally before reperfusion. Liver and intestinal tissues, as well as blood samples, were obtained for analysis at the end of the 2 h reperfusion period.
Liver and intestinal histopathological assessment
The left lobe of the liver and isolated intestine were cut into sections and fixed in 40 g/L formaldehyde. After being embedded in paraffin, 4 µm sections were stained with haematoxylin and eosin for light microscopy. Intestinal damage was evaluated by a pathologist who scored the histology using the system described by Chiu et al. (1970) as follows: Grade 0, normal mucosa; Grade 1, subepithelial space developing at the tip of the villus; Grade 2, extension of the subepithelial space with moderate lifting of the epithelial layer from the lamina propria; Grade 3, some denuded tips of the villi and massive lifting of the epithelial layer; Grade 4, dilated and exposed capillaries and denuded villi; and Grade 5, haemorrhage, ulceration and disintegrated lamina propria.
Pathological scores of liver sections were evaluated as reported previously (Eckhoff et al., 2002). Briefly, liver biopsies were evaluated by a pointcounting method for the severity of hepatic injury with the use of the ordinal scale: Grade 0, minimal or no evidence of injury; Grade 1, mild injury consisting in cytoplasmic vacuolation and focal nuclear pyknosis; Grade 2, moderate to severe injury with extensive nuclear pyknosis, cytoplasmic hypereosinophilia, loss of intercellular borders and mild to moderate neutrophil infiltration; and Grade 3, severe injury with disintegration of hepatic cords, haemorrhage and severe polymorphonuclear leucocyte infiltration. On average, 100 adjacent points on a 1 mm2 grid were graded for each specimen (n = 4).
Measurement of serum AST, ALT
Serum levels of aspartate aminotransferase (AST), alanine aminotransferase (ALT), in U/L, were measured using an Olympus automatic analyzer (AU1000; Olympus Optical, Tokyo, Japan).
Intestinal and liver MDA assay
The intestinal and liver tissues were harvested and immediately homogenized on ice in 5 volumes of normal saline. The homogenates were centrifuged at 1200 g for 10 min. The MDA level in the supernatant was measured using an MDA assay kit according to the manufacturer's instructions.
Liver MPO and TNF-α assay
Neutrophil infiltration into the liver was assessed indirectly by measuring the MPO activity. The liver tissues were harvested and immediately homogenized on ice in 5 volumes of normal saline. The homogenates were centrifuged at 1,200 g for 10 min. The MPO and TNF-α level in the supernatant was measured using assay kits according to the manufacturer's instructions. One unit of MPO activity was defined as degrading 1 mmol hydrogen peroxide/g tissue at 37℃ and expressed as U/g.
Liver NF-κB and ICAM-1 immunohistochemical assays
Paraffin-embedded liver sections were stained using the streptavidin peroxidase (SP) immunohistochemistry technique for intercellular adhesion molecule-1 (ICAM-1) and NF-κB detection. After being dewaxed or washed in PBS, 4 µm sections were immersed in 3% hydrogen peroxide to eliminate intrinsic peroxidase, quenched in normal goat serum for 30 min, and the sections were incubated overnight at 4℃ with polyclonal rabbit anti-rat NF-κB p65 and ICAM-1 antibody, against purified recombinant NF-κB or ICAM-1. Then, anti-rabbit immunoglobulin and streptavidin conjugated to HRP were added. Finally, 3, 3'-diaminobenzidine (DAB) was used for colour development and haematoxylin was used for counterstaining. Brown staining in the cytoplasm and/or nucleus was considered an indicator of positive expression. With the Medical Image Analysis System HMIAS-2000 (Qianping Image Co., Wuhan, China), results were evaluated semiquantitatively according to optical density values of positive expression.
Liver NF-κB western blot analysis
Cellular nuclear proteins were extracted from frozen liver tissue with a nuclear extract kit according to the manufacturer's instructions. An equal amount of protein was loaded onto 10% SDS-PAGE at 100 V for 3 h. After electrophoresis, proteins were transferred onto nitrocellulose membranes at 200 mA for 2 h. The transferred membranes were incubated overnight at 4℃ with mouse polyclonal antibodies NF-κB p65 (1:1,000 dilution) against rat in PBS-T containing 5% skim milk. After washing three times in Tris phosphate-buffered sodium (TBS-T), membranes were incubated with antimouse IgG conjugated to HRP at a dilution of 1:2,000 in PBS-T containing 5% skim milk for 1 h at room temperature. The immunoreactive bands were visualized with enhanced chemiluminescence (ECL) and captured on X-ray film. Optical density of the bands was measured with a Gel imaging analysis system.
Statistical analysis
Mean ± S.D. values were calculated to summarize all outcome measurements. One-way analysis of variance (ANOVA) was used to compare the means of four groups and P < 0.05 was chosen to indicate statistical significance.
Results
Effects of Rb1 on intestinal injury induced by intestinal I/R
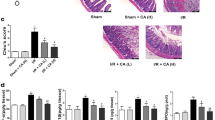
Occluded small intestine showed a dark color and mild swelling after 1 h intestinal ischemia and 2 h reperfusion. H-E staining was carried out to determine the histological changes in the intestinal tissue. Histological evaluation was performed according to the Chiu scoring method. As expected, no mucosal injury was observed in the sham group. The oedema, bleeding and villi irregularities could be found in the intestinal mucosa and submucosa in the I/R group. Treatment of rats with 20 mg/kg and 40 mg/kg Rb1 resulted in marked amelioration of intestinal injury compared with the I/R group (Figure 2).
Effects of Rb1 on intestinal injury after intestinal I/R. Representative hematoxylin and eosin-stained high magnification (original magnification ×200) of intestinal tissue from different groups. The sham group showed normal appearance of intestinal mucosa. The oedema, bleeding and villi irregularities could be found in the intestinal mucosa and submucosa in the I/R group. Treatment of rats with 20 and 40 mg/kg Rb1 resulted in a marked amelioration of intestinal injury compared with the I/R group. Pathological scores of liver sections were evaluated. Data represent means ± S.D. *P < 0.01 versus sham group; #P < 0.01 versus I/R group.
Effects of Rb1 on MDA level in intestinal and liver tissue
MDA is a kind of metabolism product of lipid superoxidation reaction, whose content reflects that of free radicals in tissue. Following 1 h of intestinal ischemia, reperfusion significantly increased intestinal tissue MDA levels in the I/R group compared with sham group. Administration of 20 mg/kg and 40 mg/kg Rb1 markedly decreased intestinal MDA level compared with the I/R group (Figure 3A). The data suggested that Rb1 markedly relieved intestinal mucosa damage and decreased MDA level in intestinal tissue with increasing dose of Rb1.
We also examined the effects of Rb1 on MDA levels in liver tissue. At 2 h after intestinal I/R, liver tissue MDA levels was increased significantly in I/R group compared with sham group. Administration of 20 mg/kg and 40 mg/kg Rb1 significantly reduced MDA levels (Figure 3B). Results indicate that Rb1 ablated the liver injury induced by intestinal I/R in a dose-dependent manner.
Effects of Rb1 on liver injury induced by intestinal I/R
Serum ALT and AST levels were measured in order to evaluate the effects of Rb1 on intestinal I/R-induced liver injury. Following 1 h of intestinal ischemia, reperfusion significantly increased serum ALT and AST levels in the I/R group in comparison with the sham group. Treatment with 20 mg/kg and 40 mg/kg Rb1 markedly decreased serum ALT and AST levels compared with the I/R group (Figure 4).
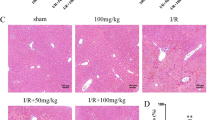
Similar to the effects on serum ALT and AST levels, Rb1 could alleviate liver histology injury at 2 h after intestinal reperfusion. In Figure 5, the liver lobes in the I/R group show pathological changes, including oedema, haemorrhage and PMN infiltration. And the pathological score of liver was higher than sham group. Significant amelioration of histological oedema, haemorrhage and inflammatory cell infiltration was seen in the 20 and 40 mg/kg Rb1 treated groups and the pathological score was lower than that of the I/R group.
Effects of Rb1 on liver injury after intestinal I/R. Representative hematoxylin and eosin-stained high magnification (original magnification ×400) of liver tissue from different groups. The sham group showed normal appearance of hepatocytes and sinusoids. The I/R group showed oedema, haemorrhage, nuclear pyknosis, partial exfoliation of blood vessel endothelium and infiltration by inflammatory cells. Significant amelioration of histological oedema, haemorrhage and inflammatory cell infiltration was seen in the 20 and 40 mg/kg Rb1 treated groups. Pathological scores of liver sections were evaluated. Data represent means ± S.D. *P < 0.01 versus sham group; #P < 0.01 versus I/R group.
Effects of Rb1 on TNF-α level in liver tissue
In order to investigate the mechanism of Rb1 protective role on liver injury, we studied the effects of Rb1 on the TNF-α level in liver tissue. Compared with the sham group, liver tissue TNF-α level increased significantly in I/R group. Administration of 20 mg/kg and 40 mg/kg Rb1 significantly reduced TNF-α level compared with I/R group. The data suggested that Rb1 decreased TNF-α level in a dose-dependent manner (Figure 6).
Effects of Rb1 on MPO activity in liver tissue
Neutrophils infiltration in liver tissue played an important role in liver injury induced by intestinal tissue. MPO assay is widely used to quantify the number of neutrophils in a tissue and serves as an index of inflammation, because MPO is an enzyme that is released mainly from Neutrophils (Krawisz et al., 1984). Compared with the sham group, the liver MPO activity was increased in I/R group. Treatment of rats with 20 mg/kg and 40 mg/kg of Rb1 significantly decreased MPO activity compared with the I/R group (Figure 7).
Effects of Rb1 on ICAM-1 expression in liver tissue by immunohistochemical analysis
Histological examination and MPO assay in liver tissue showed more extensive neutrophils infiltration in the I/R group. We therefore determined the effects of Rb1 on expression of the ICAM-1 required for neutrophils recruitment. ICAM-1 expression immunohistochemical analysis showed light brown immunostainging in the sham group. The significant positive expression of ICAM-1 with strong brown staining was observed in the I/R group. The expression of ICAM-1 was decreased in Rb1-20 and Rb1-40 group compared with I/R group. The data suggested that Rb1 markedly inhibited ICAM-1 expression in a dose-dependent manner (Figure 8).
Effects of Rb1 on ICAM-1 expression of liver tissue after intestinal I/R. Immunohistochemical staining of liver ICAM-1 expression (original magnification ×400). There was little staining for ICAM-1 in the sham group. Strong positive expression ICAM-1 as brown staining was observed in the I/R group. Compared with I/R group, the ICAM-1 expression was markedly reduced in the Rb1 treated groups. Data represent means ± S.D. *P < 0.01 versus sham group; #P < 0.01 versus I/R group.
Effects of Rb1 on NF-κB p65 expression in liver tissue
NF-κB is an important nuclear transcription factor which regulates TNF-α and ICAM-1 gene expression. Above data suggested that Rb1 could decrease TNF-α level and ICAM-1 expression and ablate liver injury induced by intestinal I/R. To elucidate the mechanism by which Rb1 decreased TNF-α level and ICAM-1 expression, we examined the effects of Rb1 on NF-κB p65 expression in liver tissue. Immunohistochemical analysis showed light brown immunostainging in the cytoplasm and no staining in the nucleus in the sham group. The significant positive expression of NF-κB p65 with strong brown staining in the cytoplasm and nucleus was observed in the I/R group. Administration of 20 mg/kg and 40 mg/kg Rb1 inhibited the expression of NF-κB p65 in liver tissue compared with I/R group (Figure 9).
Effects of Rb1 on NF-κB expression of liver tissue after intestinal I/R. Immunohistochemical staining of liver NF-κB expression (original magnification ×400). There was no staining in the nucleus for NF-κB p65 expression in the sham group. Strong positive expression NF-κB p65 expression in the nucleus as brown staining was observed in the I/R group. Compared with I/R group, the NF-κB p65 expression was markedly reduced in the Rb1 treated groups. Data represent means ± S.D. *P < 0.01 versus sham group; #P < 0.01 versus I/R group.
Western blot analysis showed weak NF-κB p65 positive signals in the liver of sham group. In contrast, significant increase of the NF-κB p65 protein expression was found in the I/R group. Compared with I/R group, the signals were weakened in the Rb1-20 and Rb1-40 group. The data suggested that Rb1 markedly inhibited NF-κB activation with increasing dose of Rb1 (Figure 10). Thus, Rb1 inhibited the NF-κB activation in a dosedependent manner. These findings suggested the importance of NF-κB pathway in protective effects of Rb1 on liver injury induced by intestinal I/R.
Discussion
Intestinal I/R occurs not only in mesentery and intestinal diseases, but also in many clinical situations such as shock, hemorrhage, liver resection and transplantation, which is considered to be a critical and triggering event in the development of distant organ dysfunction.
The liver is the first injured 'distance' organ affected by intestinal I/R because of the washout of toxic substances from the reperfused intestine. Traditionally, the mechanism of liver injury induced by intestinal I/R focused on the direct effect of toxic substances, including oxygen free radical, neutrophils, pro-inflammatory cytokines and adhesion molecules (Yao et al., 2007). Many studies have demonstrated that inflammatory mediators are regulated by NF-κB, which is a key regulator of inflammatory gene expression in liver injury. In addition, Tian et al. have shown in a recent study that NF-κB plays an important role in the process of liver injury caused by intestinal I/R (Tian et al., 2006).
Ginsenosides have been shown to have a wide variety of biological activities including immunomodulatory effects, antioxidant, anti-inflammatory and anti-tumor activity (Kenarova et al., 1990; Attele et al., 1999; Shibata 2001; Park et al., 2003). A series of studies have demonstrated that Ginsenoside Rb1 effectively protects against cerebral, heart and lung ischemia/reperfusion injuries (Zeng et al., 2003; Geng et al., 2005; Li et al., 2005). However, few reports have been published about the effects of Ginsenoside Rb1 on liver injury induced by intestinal I/R. In this study, we attempted to explore the possible protective role of Rb1 on intestinal I/R induced liver injury and its molecular events. So we focused the effects of Rb1 not only on the direct effect of toxic substances, including oxygen free radical (MDA), neutrophils (MPO), pro-inflammatory cytokines (TNF-α) and adhesion molecules (ICAM-1), but also on the NF-kB expression in liver tissue.
In this research, we used superior mesenteric artery occlusion method to establish intestinal I/R. After 1 h intestinal ischemia and 2 h reperfusion, Rb1 markedly ablated intestinal mucosa damage (Figure 2). The liver is the first injured distance organ affected by intestinal I/R. In this study, 1 h intestinal ischemia followed by 2 h reperfusion induced liver injury. ALT and AST levels of serum markers of liver function, as well as the liver histological scores was increased significantly in I/R group but improved in the Rb1-20 and Rb1-40 treated group (Figure 4). These data suggested that Rb1 alleviated liver injury induced by intestinal I/R in a dose-dependent manner. The mechanism underlying the attenuation of intestinal I/R induced liver injury by Rb1 is the emphasis of this study.
Oxidative stress is one proposed mechanism for the development of I/R-induced damage. Lipidic peroxidation is frequently used to prove the involvement of free radicals in cell damage. MDA is one of the final products of lipidic peroxidation and several methods have been proposed for its determination. MDA can be dosed in both tissue and blood and its concentration is directly proportional to the cell damage caused by free radicals (Gutteridge et al., 1990). So the MDA level indirectly reflects tissue or cell damage caused by free radicals. In the present study, MDA level was significantly increased in intestinal and liver tissue in I/R group. Treatment with 20 mg/kg and 40 mg/kg Rb1 decreased MDA level in intestinal and liver tissue (Figure 3). Results indicated that there existed free radical damage in liver and intestinal tissue and Rb1 could attenuate liver and intestinal damage caused by free radical.
There is a growing body of evidence that incriminates PMNs in the pathophysiological progress of I/R injury. Neutrophils activation leads to remote organ injury due to adherence of circulating neutrophils to microvasculature in susceptible organs, especially liver (Horie et al., 1996; Kalia et al., 2003). PMNs can cause tissue damage in several ways including secretion of proteolytic enzymes such as elastase from cytoplasmic granules, production of free radicals via a respiratory burst, and physical impairment of the microcirculation and thereby extension of ischemia. Neutrophils infiltration into tissues is commonly assessed by changes in activity of MPO, an enzyme found almost exclusively in neutrophils. The increased MPO activity in the liver tissue after intestinal I/R injury suggested activation of an inflammatory response. Furthermore, intestine-and/or liver-derived mediators, such as TNF-α, have been implicated as participants in the intestinal I/R-induced leucocytemediated liver response (Yao et al., 1995). Previous work has shown that liver injury associated with intestinal I/R appears to be dependent on leucocyte adhesion and activation (Giakoustidis et al., 2006). ICAM-1 play a key role in neutrophil chemoattraction, adhesion, and emigration from the vascularture to the tissue, contributing the systemic inflammatory response and organ injury. Adhesion molecule-specific monoclonal antibody treatment can attenuate intestinal I/R-induced leucocyte recruitment and hepatocellular dysfunction in animals (Horie et al., 1997). In this study, we found the MPO activity, TNF-α level and ICAM-1 expression was increased in I/R group. Treatment with 20 mg/kg and 40 mg/kg Rb1 markedly decreased MPO activity, TNF-α level and ICAM-1 expression in liver tissue compared with I/R group (Figure 6-8). These data suggested that Rb1 attenuated liver injury by decreasing MPO activity, ICAM-1 expression and TNF-α level in liver tissue.
NF-κB is a rapid response transcription factor in the cytoplasm and consists of two subunits of 50kDa and 65kDa that are bound to an inhibitor protein termed IkB. Because NF-κB activation can lead to enhanced expression of proinflammatory cytokines, chemokines and adhesion molecules, modulation of NF-κB activation may provide a direct way of inhibiting inflammatory mediators (Cong et al., 2002). For that reason, control of NF-κB activation is a potential therapeutic strategy to reduce the untoward tissue damage. Directing drug discovery efforts towards NF-κB activation rather than towards any one of its many target genes could produce a much greater therapeutic benefit by inhibiting expression of the constellation of NF-κB-induced pro-inflammatory genes (Emery et al., 2001). In our study, 1 h intestinal ischemia followed by 2 h reperfusion induced liver injury that paralleled the increased levles of serum markers of liver function, as well as the expression of NF-κB. This suggests that NF-κB activation is involved in the pathogenesis of liver injury induced by intestinal I/R. And Rb1 could attenuate liver injury by inhibiting NF-κB activation in a dose-dependent manner (Figure 9, 10). So Rb1 decreased TNF-α level and ICAM-1 expression by inhibiting NF-κB activation. In the early stage of intestinal ischemia/reperfusion, the gut barrier function is progressively damaged, and bacteria, endogenous endotoxin, bacteriotoxin and reactive oxygen species (ROS) invade into the circulation, and the low levels of ROS and inflammatory mediators can activate the expression of NF-κB (Xu et al., 2003). In this research, Rb1 decreased MDA level in intestinal tissue and TNF-α level in liver tissue in a dose-dependent manner. So the possible mechanism of inhibitory effects of Rb1 on NF-κB activation might be related to antioxidant and anti-inflammatory role of Rb1.
Taken together, the present study delivers important new insights to the molecular mechanisms of protective effect of Rb1 on liver injury induced by intestinal I/R. Our results indicated that Rb1 markedly attenuated liver injury by inhibiting NF-κB activation in liver tissue. The inhibition of NF-κB pathway may be involved in the protective effect. Although the precise mechanism by which Rb1 attenuates liver injury induced by intestinal I/R remains to be further clarified, understanding the pharmacological actins of Rb1 on liver injury may allow the development of novel therapeutic strategies for intestinal I/R induced remote organ injury. The next steps we need to take care to investigate the other mediators and other organ injury induced by intestinal I/R.
Abbreviations
- ALT:
-
alanine aminotransferase
- AST:
-
aspartate aminotransferase
- I/R:
-
ischemia-reperfusion
- ICAM-1:
-
intercellular adhesion molecule-1
- MDA:
-
malondialdehyde
- MODS:
-
multiple organ dysfunction syndrome
- MPO:
-
myeloperoxidase
- Rb1:
-
ginsenoside Rb1
References
Amersi F, Buelow R, Kato H, Ke B, Coito AJ, Shen XD, Zhao D, Zaky J, Melinek J, Lassman CR, Kolls JK, Alam J, Ritter T, Volk HD, Farmer DG, Ghobrial RM, Busuttil RW, Kupiec-Weglinski JW . Upregulation of heme oxygenase-1 protects genetically fat Zucker rat livers from ischemia/reperfusion injury . J Clin Invest 1999 ; 104 : 1631 - 1639
Antonsson JB, Fiddian-Green RG . The role of the gut in shock and multiple system organ failure . Eur J Surg 1991 ; 157 : 3 - 12
Attele AS, Wu JA, Yuan CS . Ginseng pharmacology: multiple constituents and multiple actions . Biochem Pharmacol 1999 ; 58 : 1685 - 1693
Chiu CJ, McArdle AH, Brown R, Scott HJ, Gurd FN . Intestinal mucosal lesion in low flow states . Arch Surg 1970 ; 101 : 478 - 483
Cong B, Li SJ, Yao YX, Zhu GJ, Ling YL . Effect of cholecystokinin octapeptide on tumor necrosis factor a transcription and nuclear factor-kB activity induced by lipopolysaccharide in rat pulmonary interstitial macrophages . World J Gastroenterol 2002 ; 8 : 718 - 723
Cuzzocrea S, Misko TP, Costantino G, Mazzon E, Micali A, Caputi AP, MacArthur H, Salvemini D . Beneficial effects of peroxynitrite decomposition catalyst in a rat model of splanchnic artery occlusion and reperfusion . FASEB J 2000 ; 14 : 1061 - 1072
Eckhoff DE, Bilbao G, Frenette L, Thompson JA, Contreras JL . 17-Beta-estradiol protects the liver against warm ischemia/reperfusion injury and is associated with increased serum nitric oxide and decreased tumor necrosis factor-alpha . Surgery 2002 ; 132 : 302 - 309
Emery JG, Ohlstein EH, Jaye M . Therapeutic modulation of transcription factor activity . Trends Pharmacol Sci 2001 ; 22 : 233 - 240
Geng Q, Wu D, Xie YC, Zhang BG, Wu H, Yin WH . Effects of ginsenoside Rb1 on apoptosis and Bcl-2, Bax gene expression in rabbits with lung ischemia/reperfusion injury . Chin J TCM WM Crit Care 2005 ; 12 : 159 - 161
Giakoustidis AE, Giakoustidis DE, Iliadis S, Papageorgiou G, Koliakou K, Kontos N, Taitzoglou I, Botsoglou E, Papanikolaou V, Atmatzidis K, Takoudas D, Antoniadis A . Attenuation of intestinal ischemia/reperfusion induced liver and lung injury by intraperitoneal administration of (-)-epigallocatechin-3-gallate . Free Radic Res 2006 ; 40 : 103 - 110
Gutteridge JMC, Halliwell B . The measurement and mechanism of lipid peroxidation in biological systems . Tibs 1990 ; 15 : 129 - 135
Horie Y, Wolf R, Miyasaka M, Anderson DC, Granger DN . Leukocyte adhesion and hepatic microvascular responses to intestinal ischemia/reperfusion in rats . Gastroenterology 1996 ; 111 : 666 - 673
Horie Y, Wolf R, Anderson DC, Granger DN . Hepatic leukostasis and hypoxic stress in adhesion molecule-deficient mice after gut ischemia/reperfusion . J Clin Invest 1997 ; 99 : 781 - 788
Horie Y, Ishii H . Liver dysfunction elicited by gut ischemia-reperfusion . Pathophysiology 2001 ; 8 : 11 - 20
Kalia N, Pockley AG, Wood RFM, Brown NJ . Effects of FK409 on intestinal ischemia-reperfusion injury and ischemia-induced changes in the rat mucosal villus microcirculation . Transplantation 2001 ; 72 : 1875 - 1880
Kalia N, Brown NJ, Wood RF, Hopkinson K, Fairburn B, Pockley AG . Effects of intestinal ischemia-reperfusion injury on rat peripheral blood neutrophil activation . Dig Dis Sci 2003 ; 48 : 1677 - 1684
Kenarova B, Neychev H, Hadjiivanova C, Petkov VD . Immunomodulating activity of ginsenoside Rg1 from Panax ginseng . Jpn J Pharmacol 1990 ; 54 : 447 - 454
Krawisz JE, Sharon P, Stenson WF . Quantitative assay for acute intestinal inflammation based on myeloperoxidase activity. Assessment of inflammation in rat and hamster models . Gastroenterology 1984 ; : 1344 - 1350
Leister I, Mbachu EM, Post S, Samel ST, Stojanovic T, Gutt CN, Becker H, Markus PM . Vasoactive intestinal polypeptide and gastrin-releasing peptide attenuate hepatic microvasculatory disturbances following intestinal ischemia and reperfusion . Digestion 2002 ; 66 : 186 - 192
Li FC, Tao ZY, Liu AM, Li JL, Wu ZH, Lin JH . Effect of ginsenoside Rb1 on the expression of GLUT1 in penumbra area after cerebral ischemia/reperfusion injury in rats . Chin J Exp Surg 2005 ; 22 : 196 - 197
Megison SM, Horton JW, Chao H, Walker PB . A new model for intestinal ischemia in the rat . J Surg Res 1990 ; 49 : 168 - 173
Park EK, Choo MK, Kim EJ, Han MJ, Kim DH . Antiallergic activity of ginsenoside Rh2 . Biol Pharm Bull 2003 ; 26 : 1581 - 1584
Pierro A, Eaton S . Intestinal ischemia reperfusion injury and multisystem organ failure . Semin Pediatr Surg 2004 ; 13 : 11 - 17
Poggetti RS, Moore EE, Moore FA, Koike K, Banerjee A . Gut ischemia/reperfusion-induced liver dysfunction occurs despite sustained oxygen consumption . J Surg Res 1992a ; 52 : 436 - 442
Poggetti RS, Moore FA, Moore EE, Koeike K, Banerjee A . Simultaneous liver and lung injury following gut ischemia is mediated by xanthine oxidase . J Trauma 1992b ; 32 : 723 - 727
Shibata S . Chemistry and cancer preventing activities of ginseng saponins and some related triterpenoid compounds . J Korean Med Sci 2001 ; 16 : S28 - S37
Tian XF, Yao JH, Li YH . Protective effect of pyrrolidine dithiocarbamate on liver injury induced by intestinal ischemia-reperfusion in rats . Hepatobiliary Pancreat Dis Int 2006 ; 5 : 90 - 95
Turnage RH, Kadesky KM, Myers SI, Guice KS, Oldham KT . Hepatic hypoperfusion after intestinal reperfusion . Surgery 1996 ; 119 : 151 - 160
Xu J, Xie J, Bao M, Li Z, Yang Z . NF-kappa B / I-kappa B pathway during ischemia reperfusion injury of rat liver . Chin Med J 2003 ; 116 : 1146 - 1149
Yao JH, Li YH, Wang ZZ, Zhang XS, Wang YZ, Yuan JC, Zhou Q, Liu KX, Tian XF . Proteasome inhibitor lactacystin ablates liver injury induced by intestinal ischaemia-reperfusion . Clin Exp Pharmacol Physiol 2007 ; 34 : 1102 - 1108
Yao YM, Sheng ZY, Yu Y, Tian HM, Wang YP, Lu LR, Xu SH . The potential etiologic role of tumor necrosis factor in mediating multiple organ dysfunction in rats following intestinal ischemia-reperfusion injury . Resuscitation 1995 ; 29 : 157 - 168
Zeng HS, Liu ZX, Liu XC . Effect of ginsenoside-Rb1 and Re against cardiomyocyte apoptosis and expression of the related gene proteins in the experimental cardiac ischemia-reperfusion in rats . Chin J Phys Med Rehabil 2003 ; 25 : 402 - 405
Acknowledgements
This work was supported by grant 2003AA301C51 from Hubei Province Science and Technique Foundation of China. The authors express their thanks to Dr. Wang Ni and Shixin Chen in Laboratory of Respiratory Medicine.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Wang, J., Qiao, L., Li, Y. et al. Ginsenoside Rb1 attenuates intestinal ischemia-reperfusion-induced liver injury by inhibiting NF-κB activation. Exp Mol Med 40, 686–698 (2008). https://doi.org/10.3858/emm.2008.40.6.686
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.3858/emm.2008.40.6.686
Keywords
This article is cited by
-
Effect of ginseng extract on the TGF-β1 signaling pathway in CCl4-induced liver fibrosis in rats
BMC Complementary and Alternative Medicine (2017)
-
Effect of two administration routes of Shenmai Injection (参麦注射液) on pulmonary gas exchange function after tourniquet-induced ischemia-reperfusion
Chinese Journal of Integrative Medicine (2017)
-
A comprehensive overview of hepatoprotective natural compounds: mechanism of action and clinical perspectives
Archives of Toxicology (2016)
-
Ginseng extract and ginsenoside Rb1 attenuate carbon tetrachloride-induced liver fibrosis in rats
BMC Complementary and Alternative Medicine (2014)
-
The effects of ginsenoside Rb1 on JNK in oxidative injury in cardiomyocytes
Archives of Pharmacal Research (2012)