Abstract
Background/Objectives:
Late preterm infants (born ⩾32 weeks of gestation) are at risk for developing iron deficiency and iron deficiency anaemia, and this may lead to impaired neurodevelopment. In the Netherlands, there is no guideline for standardised iron supplementation in these infants. Individualised iron supplementation has been suggested (that is, treating those infants with the highest risk), but risk factors for deprived iron stores in this specific group of infants are not well documented.
Subjects/Methods:
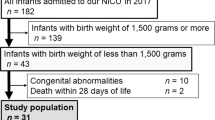
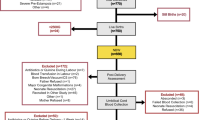
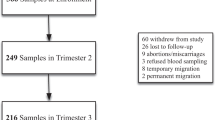
In this prospective multi-centre study, we analysed the iron status at the postnatal age of 6 weeks of 68 infants born between 32 and 35 weeks of gestation in the Netherlands. Serum ferritin (SF) <70 μg/l in the absence of infection (C-reactive protein <5 mg/l) was defined as iron depletion and whenever in combination with a haemoglobin level <110 mg/dl as iron-depleted anaemia. Medical charts were reviewed to identify risk factors.
Results:
Iron depletion and iron-depleted anaemia were present in 38.2% and 30.9% of the infants, respectively. Infants with a birth weight <1830 g and a SF <155 μg/l in the first week of life had a 26.4 times higher risk to develop iron depletion (95% confidence interval 3.1–227.0, P=0.003). Multivariate regression analyses also showed that iron depletion was associated with a higher number of blood draws.
Conclusions:
Iron depletion is common in late preterm infants at the age of 6 weeks in a setting without standardised iron supplementation. One should consider early individualised iron supplementation for late preterm infants with a low birth weight (<1830 g), and a low SF in the first week of life (<155 μg/l), as they have a high risk to develop iron depletion.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Domellof M, Braegger C, Campoy C, Colomb V, Decsi T, Fewtrell M et al. Iron requirements of infants and toddlers. J Pediatr Gastroenterol Nutr 2014; 58: 119–129.
Siddappa AM, Rao R, Long JD, Widness JA, Georgieff MK . The assessment of newborn iron stores at birth: a review of the literature and standards for ferritin concentrations. Neonatology 2007; 92: 73–82.
Andersson O, Lindquist B, Lindgren M, Stjernqvist K, Domellof M, Hellstrom-Westas L . Effect of delayed cord clamping on neurodevelopment at 4 years of age: a randomized clinical trial. JAMA Pediatr 2015; 169: 631–638.
Lozoff B . Iron deficiency and child development. Food Nutr Bull 2007; 28: S560–S571.
Rao R, Georgieff MK . Iron therapy for preterm infants. Clin Perinatol 2009; 36: 27–42.
Agostoni C, Buonocore G, Carnielli VP, De Curtis M, Darmaun D, Decsi T et al. Enteral nutrient supply for preterm infants: commentary from the European Society of Paediatric Gastroenterology, Hepatology and Nutrition Committee on Nutrition. J Pediatr Gastroenterol Nutr 2010; 50: 85–91.
Baker RD, Greer FR . Diagnosis and prevention of iron deficiency and iron-deficiency anemia in infants and young children (0-3 years of age). Pediatrics 2010; 126: 1040–1050.
Berglund S, Westrup B, Domellof M . Iron supplements reduce the risk of iron deficiency anemia in marginally low birth weight infants. Pediatrics 2010; 126: e874–e883.
Uijterschout L, Domellof M, Abbink M, Berglund S, van Veen I, Vos P et al. Iron deficiency in the first 6 months of age in infants born between 32 and 37 weeks of gestational age. Eur J Clin Nutr 2014; 69: 598–602.
World Health Organization Iron Deficiency Anaemia. Assessment, Prevention, and Control. A guide for programma managers. Publication date: 1 January 2001. Report No.: WHO/NHD/01.3. Accessed: 21 December 2015. Ref Type: Online Source.
TNO innovation for life. Groeidiagrammen in PDF-formaat (Dutch growth charts 2010). Accessed: 21 December 2015. Ref Type: Online Source.
Neu J . Necrotizing enterocolitis: the search for a unifying pathogenic theory leading to prevention. Pediatr Clin North Am 1996; 43: 409–432.
Glas BS, Rovekamp-Abels WW, van Zoeren-Grobben D . Content of feeding. In: Neonatology Division of the Dutch Association for Pediatrics, editor. Enteral and parenteral feeding for neonates, 3rd edn. VU University Press: Amsterdam, The Netherlands, 2012, pp 89–94.
Schiza V, Giapros V, Pantou K, Theocharis P, Challa A, Andronikou S . Serum transferrin receptor, ferritin, and reticulocyte maturity indices during the first year of life in 'large' preterm infants. Eur J Haematol 2007; 79: 439–446.
Ozdemir H, Akman I, Demirel U, Coskun S, Bilgen H, Ozek E . Iron deficiency anemia in late-preterm infants. Turk J Pediatr 2013; 55: 500–505.
Kohgo Y, Ikuta K, Ohtake T, Torimoto Y, Kato J . Body iron metabolism and pathophysiology of iron overload. Int J Hematol 2008; 88: 7–15.
Rabe H, Diaz-Rossello JL, Duley L, Dowswell T . Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Cochrane Database Syst Rev 2012; 8: CD003248.
McDonald SJ, Middleton P, Dowswell T, Morris PS . Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes. Cochrane Database Syst Rev 2013; 7: CD004074.
Mukhopadhyay K, Yadav RK, Kishore SS, Garewal G, Jain V, Narang A . Iron status at birth and at 4 weeks in preterm-SGA infants in comparison with preterm and term-AGA infants. J Matern Fetal Neonatal Med 2012; 25: 1474–1478.
Makela E, Takala TI, Suominen P, Matomaki J, Salmi TT, Rajamaki A et al. Hematological parameters in preterm infants from birth to 16 weeks of age with reference to iron balance. Clin Chem Lab Med 2008; 46: 551–557.
van de Lagemaat M, Amesz EM, Schaafsma A, Lafeber HN . Iron deficiency and anemia in iron-fortified formula and human milk-fed preterm infants until 6 months post-term. Eur J Nutr 2014; 53: 1263–1271.
Amin SB, Scholer L, Srivastava M . Pre-discharge iron status and its determinants in premature infants. J Matern Fetal Neonatal Med 2012; 25: 2265–2269.
Acknowledgements
This study was registered at the Dutch Trial Register (NTR) (www.trialregister.nl); NTR number: 2828.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
JBvG is director of the Dutch Human Milk Bank, member of the Dutch Health Council and received grant support/honoraria for lectures or consultancy from Danone Nutricia Research, Mead Johnson Nutritionals, Nestle Nutrition Institute, Hipp and Pharmaceutical United in the previous 3 years. The remaining authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Akkermans, M., Uijterschout, L., Abbink, M. et al. Predictive factors of iron depletion in late preterm infants at the postnatal age of 6 weeks. Eur J Clin Nutr 70, 941–946 (2016). https://doi.org/10.1038/ejcn.2016.34
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2016.34
This article is cited by
-
Rapid increase in the body mass index of very preterm infants is a risk factor for iron deficiency during infancy
Scientific Reports (2023)
-
Impact and interactions between risk factors on the iron status of at-risk neonates
Journal of Perinatology (2022)
-
The iron status at birth of neonates with risk factors for developing iron deficiency: a pilot study
Journal of Perinatology (2017)