Abstract
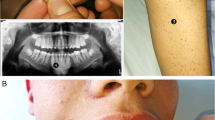
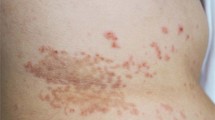
Scurvy is one of the oldest diseases in human history. Nowadays, although scurvy tends to become a forgotten disease in developed country, rare cases still occur, especially in people undergoing extreme diet, old people or children with poor diet and patients with malabsorption. We describe three cases of scurvy. The first case is a patient diagnosed with Crohn’s disease, the second one is in a context of anorexia nervosa and drug addiction, and the third case is in a context of social isolation. Early recognition of scurvy can be difficult because symptoms may appear nonspecific and can mimic more common conditions. In any patient with spontaneous hematoma and purpura, in the context of nutritional disorder, scurvy should be systematically considered. As this disease can lead to severe complications, such as bone pain, heart failure or gastrointestinal symptoms, nothing should delay vitamin C supplementation, which is a simple and rapidly effective treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Magiorkinis E, Beloukas A, Diamantis A, Scurvy . Past, present and future. Eur J Int Med 2011; 22: 147–152.
Olmedo JM, Yiannias JA, Windgassen EB, Gornet MK . Scurvy: a disease almost forgotten. Int J Dermatol 2006; 45: 909–913.
Hodges RE, Hood J, Canham JE, Sauberlich HE, Baker EM . Clinical manifestations of ascorbic acid deficiency in man. Am J Clin Nutr 1971; 24: 432–443.
Léger D . Scurvy: reemergence of nutritional deficiencies. Can Fam Physician 2008; 54: 1403–1406.
Hansen E, Metzsche C, Henningsen E, Toft P . Severe scurvy after gastric bypass surgery and a poor postoperative diet. J Clin Med Res 2012; 4: 135–137.
Khonsari H, Grandière-Perez L, Caumes E . Le scorbut n’a pas disparu: histoire d’une maladie réémergente. Rev Med Interne 2005; 26: 885–890.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Levavasseur, M., Becquart, C., Pape, E. et al. Severe scurvy: an underestimated disease. Eur J Clin Nutr 69, 1076–1077 (2015). https://doi.org/10.1038/ejcn.2015.99
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2015.99
This article is cited by
-
No longer a historical ailment: two cases of childhood scurvy with recommendations for bone health providers
Osteoporosis International (2020)
-
Adding an orange to the banana bag: vitamin C deficiency is common in alcohol use disorders
Critical Care (2019)
-
Ein seltener Fall von alimentärem Skorbut
Monatsschrift Kinderheilkunde (2019)