Abstract
Background/Objectives:
The objective of this study was to determine the postprandial change in free fatty acid (FFA) profiles in subjects with impaired fasting glucose (IFG), and to evaluate the effect of low glycemic index (GI) load on postprandial FFA profiles and inflammation.
Subjects/Methods:
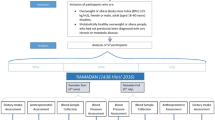
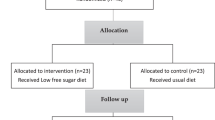
First, 50 IFG and 50 healthy subjects were recruited; and 2 -h postprandial changes in FFA profiles were determined. Second, the 50 IFG subjects then received three different loads: glucose load (GL), high glycemic index (HGI) load and low glycemic index (LGI) load, respectively. FFA profile, glucose, insulin, glucagon-like peptide 1 (GLP-1) and inflammatory biomarkers were assayed at 0, 30, 60, 90 and 120 min.
Results:
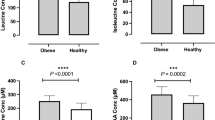
Postprandial stearic acid (C18:0) increased compared with baseline in all subjects, whereas the change in postprandial C18:0 was more marked in IFG subjects than in healthy subjects. Compared with subjects who received the GL and HGI load, the area under the curve for insulin, GLP-1, C18:0 and tumor necrosis factor-alpha significantly decreased and adiponectin increased in subjects who received the LGI load.
Conclusions:
The rise in postprandial C18:0 in IFG subjects was inhibited by LGI load.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Konukoglu D, Firtina S, Serin O . The relationship between plasma asymmetrical dimethyl-L-arginine and inflammation and adhesion molecule levels in subjects with normal, impaired, and diabetic glucose tolerance. Metabolism 2008; 57: 110–115.
Carlson OD, David JD, Schrieder JM, Muller DC, Jang HJ, Kim BJ et al. Contribution of nonesterified fatty acids to insulin resistance in the elderly with normal fasting but diabetic 2- hour postchallenge plasma glucose levels: the Baltimore Longitudinal Study of Aging. Metabolism 2007; 56: 1444–1451.
Bays H, Mandarino L, DeFronzo RA . Role of the adipocyte, free fatty acids, and ectopic fat in pathogenesis of type 2 diabetes mellitus: peroxisomal proliferator-activated receptor agonists provide a rational therapeutic approach. J Clin Endocrinol Metab 2004; 89: 463–478.
Schalch DS, Kipnis DM . Abnormalities in carbohydrate tolerance associated with elevated plasma nonesterified fatty acids. J Clin Invest 1965; 44: 2010–2020.
Reaven GM . The fourth musketeer—from Alexandre Dumas to Claude Bernard. Diabetologia 1995; 38: 3–13.
Frangioudakis G, Garrard J, Raddatz K, Nadler JL, Mitchell TW, Schmitz-Peiffer C . Saturated- and n-6 polyunsaturated-fat diets each induce ceramide accumulation in mouse skeletal muscle: reversal and improvement of glucose tolerance by lipid metabolism inhibitors. Endocrinology 2010; 151: 4187–4196.
Fedor D, Kelley DS . Prevention of insulin resistance by n-3 polyunsaturated fatty acids. Curr Opin Clin Nutr Metab Care 2009; 12: 138–146.
Jula A, Marniemi J, Ronnemaa T, Virtanen A, Huupponen R . Effects of diet and simvastatin on fatty acid composition in hypercholesterolemic men: a randomized controlled trial. Arterioscler Thromb Vasc Biol 2005; 25: 1952–1959.
Chu X, Liu L, Na L, Lu H, Li S, Li Y et al. Sterol regulatory element-binding protein-1c mediates increase of postprandial stearic acid, a potential target for improving insulin resistance, in hyperlipidemia. Diabetes 2013; 62: 561–571.
Abdul-Ghani MA, Tripathy D, DeFronzo RA . Contributions of beta-cell dysfunction and insulin resistance to the pathogenesis of impaired glucose tolerance and impaired fasting glucose. Diabetes Care 2006; 29: 1130–1139.
Tapola N, Karvonen H, Niskanen L, Mikola M, Sarkkinen E . Glycemic responses of oat bran products in type 2 diabetic patients. Nutr Metab Cardiovasc Dis 2005; 15: 255–261.
Sakuma M, Yamanaka-Okumura H, Naniwa Y, Matsumoto D, Tsunematsu M, Yamamoto H et al. Dose-dependent effects of barley cooked with white rice on postprandial glucose and desacyl ghrelin levels. J Clin Biochem Nutr 2009; 44: 151–159.
Laaksonen DE, Toppinen LK, Juntunen KS, Autio K, Liukkonen KH, Poutanen KS et al. Dietary carbohydrate modification enhances insulin secretion in persons with the metabolic syndrome. Am J Clin Nutr 2005; 82: 1218–1227.
Brand-Miller J, Hayne S, Petocz P, Colagiuri S . Low-glycemic index diets in the management of diabetes: a meta-analysis of randomized controlled trials. Diabetes Care 2003; 26: 2261–2267.
Murakami K, Sasaki S, Takahashi Y, Okubo H, Hosoi Y, Horiguchi H et al. Dietary glycemic index and load in relation to metabolic risk factors in Japanese female farmers with traditional dietary habits. Am J Clin Nutr 2006; 83: 1161–1169.
Report of the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 1997; 20: 1183–1197.
Liu L, Li Y, Guan C, Li K, Wang C, Feng R et al. Free fatty acid metabolic profile and biomarkers of isolated post-challenge diabetes and type 2 diabetes mellitus based on GC-MS and multivariate statistical analysis. J Chromatogr B Analyt Technol Biomed Life Sci 2010; 878: 2817–2825.
Yue KT, Davis JW, Phillips PE, Graham BA . Effect of glucose on plasma concentrations of individual non-esterified fatty acids of non-diabetic and insulin-independent diabetic men. Postgrad Med J 1981; 57: 622–626.
Louheranta AM, Turpeinen AK, Schwab US, Vidgren HM, Parviainen MT, Uusitupa MI . A high-stearic acid diet does not impair glucose tolerance and insulin sensitivity in healthy women. Metabolism 1998; 47: 529–534.
Sampath H, Ntambi JM . The fate and intermediary metabolism of stearic acid. Lipids 2005; 40: 1187–1191.
Emken EA . Metabolism of dietary stearic acid relative to other fatty acids in human subjects. Am J Clin Nutr 1994; 60: 1023S–1028S.
van den Berg SA, Guigas B, Bijland S, Ouwens M, Voshol PJ, Frants RR et al. High levels of dietary stearate promote adiposity and deteriorate hepatic insulin sensitivity. Nutr Metab (Lond) 2010; 7: 24.
Makelainen H, Anttila H, Sihvonen J, Hietanen RM, Tahvonen R, Salminen E et al. The effect of beta-glucan on the glycemic and insulin index. Eur J Clin Nutr 2007; 61: 779–785.
Kim H, Behall KM, Vinyard B . Short-term satiety and glycemic response after consumption of whole grains with various amounts of b-glucan. Cereal Foods World 2006; 51: 29–33.
Orskov C, Wettergren A, Holst JJ . Secretion of the incretin hormones glucagon-like peptide-1 and gastric inhibitory polypeptide correlates with insulin secretion in normal man throughout the day. Scand J Gastroenterol 1996; 31: 665–670.
Salehi M, Gastaldelli A, D'Alessio DA . Evidence from a single individual that increased plasma GLP-1 and GLP-1-stimulated insulin secretion after gastric bypass are independent of foregut exclusion. Diabetologia 2014; 57: 1495–1499.
Li J, Zhang N, Hu L, Li Z, Li R, Li C et al. Improvement in chewing activity reduces energy intake in one meal and modulates plasma gut hormone concentrations in obese and lean young Chinese men. Am J Clin Nutr 2011; 94: 709–716.
Jelic K, Hallgreen CE, Colding-Jorgensen M . A model of NEFA dynamics with focus on the postprandial state. Ann Biomed Eng 2009; 37: 1897–1909.
Nazare JA, Normand S, Oste Triantafyllou A, Brac de la Perriere A, Desage M, Laville M . Modulation of the postprandial phase by beta-glucan in overweight subjects: effects on glucose and insulin kinetics. Mol Nutr Food Res 2009; 53: 361–369.
Christensen KL, Hedemann MS, Laerke HN, Jorgensen H, Mutt SJ, Herzig KH et al. Concentrated arabinoxylan but not concentrated beta-glucan in wheat bread has similar effects on postprandial insulin as whole-grain rye in porto-arterial catheterized pigs. J Agric Food Chem 2013; 61: 7760–7768.
Korkmazer E, Solak N . Correlation between inflammatory markers and insulin resistance in pregnancy. J Obstet Gynaecol 2015; 35: 142–145.
Lou Y, Wu C, Wu M, Xie C, Ren L . The changes of neutrophil gelatinase-associated lipocalin in plasma and its expression in adipose tissue in pregnant women with gestational diabetes. Diabetes Res Clin Pract 2014; 104: 136–142.
Iida KT, Shimano H, Kawakami Y, Sone H, Toyoshima H, Suzuki S et al. Insulin up-regulates tumor necrosis factor-alpha production in macrophages through an extracellular-regulated kinase-dependent pathway. J Biol Chem 2001; 276: 32531–32537.
Suganami T, Nishida J, Ogawa Y . A paracrine loop between adipocytes and macrophages aggravates inflammatory changes: role of free fatty acids and tumor necrosis factor alpha. Arterioscler Thromb Vasc Biol 2005; 25: 2062–2068.
Acknowledgements
Funding was provided by Program for New Century Excellent Talents In Heilongjiang Provincial University (No. 1254-NCET-013), Postdoctoral Science Foundation of China (No. 2014M551280) and Natural Science Foundation of China Key Project (No. 81130049). The trial registry number is ChiCTR-TRC-12002630.
Author contributions
CS is the guarantor of this work and had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. LL, YL and CS contributed to the conception and design. LL, XC and LN wrote the manuscript and researched data. All authors contributed to the drafting of the article and gave final approval of the version to be published.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on European Journal of Clinical Nutrition website
Supplementary information
Rights and permissions
About this article
Cite this article
Liu, L., Chu, X., Na, L. et al. Decreasing high postprandial stearic acid in impaired fasting glucose by dietary regulation. Eur J Clin Nutr 70, 795–801 (2016). https://doi.org/10.1038/ejcn.2015.208
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2015.208