Abstract
Background/Objectives:
The body mass index (BMI) of breakfast eaters is frequently reported to be lower compared with that of breakfast skippers. This is not explained by differences in energy intakes, indicating there may be other mechanisms serving to drive this paradoxical association between breakfast and BMI. This study aimed to investigate the effect of eating breakfast versus morning fasting on measures predominantly of metabolism in lean and overweight participants who habitually eat or skip breakfast.
Subjects/Methods:
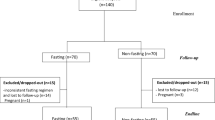
Participants (n=37) were recruited into four groups on the basis of BMI (lean and overweight) and breakfast habit (breakfast eater and breakfast skipper). Participants were randomly assigned to a breakfast experimental condition, breakfast eating or no breakfast, for 7 days and then completed the alternative condition. At the end of each breakfast experimental condition, measurements were made before and after a high carbohydrate breakfast of 2274±777 kJ or a rest period. Resting metabolic rate, thermic effect of food (TEF), blood glucose, insulin and leptin levels were recorded. Hunger and ‘morningness’ were assessed and pedometers worn.
Results:
Lean participants had lower fasting insulin levels (P=0.045) and higher insulin concentrations following breakfast (P=0.001). BMI and breakfast habit did not interact with the experimental breakfast condition, with the exception of hunger ratings; breakfast eaters were hungrier in the mornings compared with breakfast skippers in the no breakfast condition (P=0.001).
Conclusions:
There is little evidence from this study for a metabolic-based mechanism to explain lower BMIs in breakfast eaters.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Cho S, Dietrich M, Brown CJ, Clark CA, Block G . The effect of breakfast type on macronutrient intakes and body mass index (BMI) of Americans. J Am Coll Nutr 2003; 22: 296–302.
Barton BA, Eldridge AL, Thompson D, Affenito SG, Striegel-Moore RH, Franko DL et al. The relationship of breakfast and cereal consumption to nutrient intake and body mass index: the National Heart, Lung, and Blood Institute Growth and Health Study. J Am Diet Assoc 2005; 105: 1383–1389.
Keski-Rahkonen A, Kaprio J, Rissanen A, Virkkunen M, Rose RJ . Breakfast skipping and health-compromising behaviors in adolescents and adults. Eur J Clin Nutr 2003; 57: 842–853.
Casazza K, Fontaine KR, Astrup A, Birch L, Brown AW, Bohan Brown MM et al. Myths, presumptions, and facts about obesity. N Engl J Med 2003; 368: 446–454.
Song WO, Chun OK, Obayashi S, Cho S, Chung CE . Is consumption of breakfast associated with body mass index in US adults? J Am Diet Assoc 2005; 105: 1373–1382.
Brown AW, Bohan Brown MM, Allison DB . Belief beyond the evidence: using the proposed effect of breakfast on obesity to show 2 practices that distort scientific evidence. Am J Clin Nutr 2013; 98: 1298–1308.
Stanton JL, Keast DR . Serum cholesterol, fat intake and breakfast consumption in the United States population. J Am Coll Nutr 1989; 8: 567–572.
Timlin MT, Pereira MA . Breakfast frequency and quality in the etiology of adult obesity and chronic diseases. Nutr Rev 2007; 65: 268–281.
Levitsky DA, Pacanowski CR . Effects of skipping breakfast on subsequent energy intakes. Physiol Behav 2013; 11: 9–16.
Reeves S, Huber JW, Halsey LG, Horabady-Farahani Y, Ijadi M, Smith T . Experimental manipulation of breakfast in normal and overweight/obese participants is associated with changes to nutrient intake and energy consumption patterns. Phys Behav 2014; 133: 130–135.
Kobayashi F, Ogata H, Omi N, Nagasaka S, Yamaguchi S, Hibi M et al. Effect of breakfast skipping on diurnal variation of energy metabolism and blood glucose. Obes Res Clin Pract 2014; 8: e201–e298.
Bonifacio LA, Ikuno MR, HCCE Villar, Carvalho PE, Rubira CJ . Leptin for overweight and obesity (protocol). Cochrane Library 2010; 12.
Farshchi HR, Taylor MA, Macdonald IA . Decreased thermic effect of food after irregular compared with regular meal pattern in healthy lean women. Int J Obes 2004; 28: 653–660.
Farshchi HR, Taylor MA, Macdonald IA . Beneficial metabolic effects of regular meal frequency on dietary thermogenesis, insulin sensitivity and fasting lipid profiles in healthy obese women. Am J Clin Nutr 2005; 1: 16–24.
Farshchi HR, Taylor MA, Macdonald IA . Deleterious effects of omitting breakfast on insulin sensitivity and fasting lipid profiles in healthy lean women. Am J Clin Nutr 2005; 81: 88–396.
Farshchi HR, Farschi HR, Taylor MA, Macdonald IA . Regular meal frequency creates more appropriate insulin sensitivity and lipid profiles compared with irregular meal frequency in healthy lean women. Eur J Clin Nutr 2004; 58: 1071–1077.
Halsey L, Huber J, Low T, Ibeawuchi C, Woodruff P, Reeves S . Does breakfasting affect activity levels? An experiment into the effect of breakfast consumption on eating habits and energy expenditure. Public Health Nutr 2011; 15: 238–245.
Barton J, Costa G, Smith L, Spelten E, Totterdell P, Folkard S . The Standard Shift work Index: a battery of questionnaires for assessing shift work-related problems. Work Stress 1995; 9: 4–30.
Mitchell PJ, Redman JR . The relationship between morningness-eveningness, personality and habitual caffeine consumption. Person Indiv Diff 1993; 5: 105–108.
Penolazzi B, Natale V, Leone L, Russo PM . Individual differences affecting caffeine intake. Analysis of consumption behaviours for different times of day and caffeine sources. Appetite 2012; 58: 971–977.
Glade MJ . Caffeine – not just a stimulant. Nutrition 2010; 26: 932–938.
Belza A, Toubro S, Astrup A . The effect of caffeine, green tea and tyrosine on thermogenesis and energy intake. Eur J Clin Nutr 2009; 63: 57–64.
Schlundt DG, Hill JO, Sbrocco T, Pope-Cordle J, Sharp T . The role of breakfast in the treatment of obesity. Am J Clin Nutr 1992; 55: 645–651.
Dhurandhar E, Dawson J, Alcorn A, Larson LH, Thomas EA, Cardel M et al. The effectiveness of breakfast recommendations on weight loss: a randomized controlled trial. Am J Clin Nutr 2014; 100: 507–513.
Martin A, Normand S, Sothier M, Peyrat J, Louche-Pelissier C, Laville M . Is dietary advice for breakfast consumption justified? Results from a short-term dietary and metabolic experiment in young health men. Br J Nutr 2000; 84: 337–344.
Faul F, Erdfelder E, Buchner A, Lang A-G . Statistical power analyses using G*Power 3.1: Tests for correlation and regression analyses. Behav Res Method 2009; 4: 1149–1160.
Food Standards Agency Food Standards Agency Survey of Caffeine Levels in Hot Beverages. Information sheet 53/04, HMSO: London, 2004.
Weir JB . New methods for calculating metabolic rate with special references to protein metabolism. J Physiol 1949; 109: 1–9.
Reed GW, Hill JO . Measuring the thermic effect of food. Am J Clin Nutr 1996; 63: 164–169.
Allison DB, Paultre F, Maggio C, Mezzitis N, Pi-Sunyer FX . The use of areas under curves in diabetes research. Diabetes Care 1995; 18: 245–250.
Matthews D, Hosker J, Rudenski A, Naylor B, Treacher D, Turner R . Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 1985; 28: 412–419.
Stubbs RJ, Hughes DS, Johnston AM, Rowley E, Reid C, Elia M et al. The use of visual analogue scales to assess motivation to eat in human subjects: a review of their reliability and validity with an evaluation of new hand held computerised systems for temporal tracking of appetite ratings. Br J Nutr 2000; 84: 405–415.
Fisher RA . Statistical Methods for Research Workers. Oliver and Boyd Pub: London, UK, 1950.
Lew MJ . Bad statistical practice in pharmacology (and other basic biomedical disciplines): you probably don’t know P. Br J Pharmacol 2012; 166: 1559–1567.
Tudor-Locke C . A preliminary study to determine instrument responsiveness to change with a walking program: Physical activity logs versus pedometers. Res Q Exerc Sport 2001; 72: 288–292.
Betts JA, Richardson JD, Chowdhury EA, Holman GD, Tsintzas K, Thompson D . The causal role of breakfast in energy balance and health: a randomized controlled trial in lean adults. Am J Clin Nutr 2014; 100: 539–547.
Jequier E, Schutz Y . Long term measurements of energy expenditure in humans using a respiration chamber. Am J Clin Nutr 1983; 38: 989–998.
de Jonge L, Bray GA . The thermic effect of food and obesity: a critical review. Obes Res 1997; 5: 622–631.
Edholm OG, Fletcher JG, Widdowson EM, McCance RA . The energy expenditure and food intake of individual men. Br J Nutr 1955; 9: 286–300.
Carey DG, Jenkins AB, Campbell LV, Freund J, Chisholm DJ . Abdominal fat and insulin resistance in normal and overweight women: direct measurements reveal a strong relationship in subjects at both low and high risk of NIDDM. Diabetes 1996; 4: 633–638.
Haus E, Smolensky M . Biological clocks and shift work: circadian dysregulation and potential long term effects. Cancer Cause Control 2006; 17: 489–500.
Havel PJ, Kasim-Karakas S, Mueller W, Johnson PR, Gingerion RL, Stent JS . Relationship of plasma leptin to plasma insulin and adiposity in normal weight and overweight women: effects of dietary fat content and sustained weight loss. J Clin Endocrinol Metab 1996; 81: 4406–4413.
Schoeller DA, Cella LK, Sinha MK, Caro JF . Entrainment of the diurnal rhythm of plasma leptin to meal timing. J Clin Invest 1997; 100: 1882–1887.
Blom WAM, Stafleu A, de Graaf C, Kok FJ, Schaafsma G, Henriks HFJ . Ghrelin response to carbohydrate-enriched breakfast is related to Insulin. Am J Clin Nutr 2005; 1: 367–375.
Astrup A, Toubro S, Cannon S, Hein P, Madsen J . Thermogenic synergism between ephedrine and caffeine in healthy volunteers: a double-blind, placebo-controlled study. Metabolism 1991; 40: 323–329.
Kaneyoshi I, Miyasita A, Inugami M, Fukuda K, Yamazaki K, Yo M . Differences in the time or frequency of meals, alcohol and caffeine ingestion and smoking found between morning and evening types. Psych Rep 2014; 57: 391–396.
Boschloo A, Ouwehand C, Dekker S, Lee N, de Groot R, Krabbendam L, Jolles J . The relationship between breakfast skipping and school performance in adolescents. Mind Brain Educ 2012; 6: 81–88.
Reeves S, McMeel Y, Halsey L, Huber J . Breakfast habits, beliefs and measures of health and wellbeing in a nationally representative UK sample. Appetite 2013; 3: 51–57.
de la Hunty A, Ashwell M . Are people who regularly eat breakfast cereals slimmer than those who don’t? A systematic review of the evidence. Nutr Bull 2007; 32: 118–128.
Garaulet M, Gomez-Abellan P, Alburerque-Bejar JJ, Lee YC, Orddovas JM, Scheer FAJL . Timing of food intake predicts weight loss effectiveness. Int J Obes 2013; 37: 604–611.
Goldstone AP, Prechtl de Hernandez CG, Beaver JD, Muhammed K, Croese C, Bell G et al. Fasting biases brain reward systems towards high-calorie foods. Eur J Neurosci 2009; 30: 1625–1635.
Ruxton CHS, Kirk RT . Breakfast: a review of associations with measures of dietary intake, physiology and biochemistry. Br J Nutr 1997; 78: 199–213.
Jarvandi S, Yan Y, Schootman M . Income disparity and risk of death: the importance of health behaviours and other mediating factors. PLoS ONE 2012; 7: e49929.
Acknowledgements
This study was supported by Kellogg’s Company who funded the project and discussed initial ideas that helped inform the design. They were not involved in data collection, analysis or interpretation. We are grateful to Leigh Gibson who allowed us to use his caffeine questionnaire and all the volunteers who participated in this study. Trial registered with the ISRCTN, trial number ISRCTN89657927 (http://www.controlled-trials.com/ISRCTN89657927/). Ethical clearance for the study was granted by the University of Roehampton Ethics Committee (Ref: LSC 11/010).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Author Contributions
JH, LH and SR contributed to study design; LH, JH, SR and TS contributed to study coordination; TS, LH, JH, SR, MVM and JE contributed to data collection; TS contributed to supervision of data collection; TS and JH contributed to data analyses, SR contributed to drafting of manuscript; all authors contributed to input on data and manuscript.
Rights and permissions
About this article
Cite this article
Reeves, S., Huber, J., Halsey, L. et al. A cross-over experiment to investigate possible mechanisms for lower BMIs in people who habitually eat breakfast. Eur J Clin Nutr 69, 632–637 (2015). https://doi.org/10.1038/ejcn.2014.269
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2014.269