Abstract
Background/objectives:
Adherence to the Mediterranean diet (MD), high in fruits, vegetables and monounsaturated fats, has been associated with lower body mass index. Associations with measured body fat, including regional adiposity, have not been previously investigated. We examined the associations between the alternate Mediterranean diet score (aMED), anthropometry and measured adiposity by dual-energy x-ray absorptiometry (DXA).
Subjects/methods:
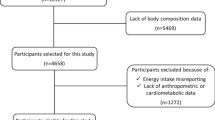
This study included 248 healthy females, aged 18–44 years from the BioCycle Study. Each woman’s aMED (range 0–9) was calculated from up to eight 24-h dietary recalls over 1–2 menstrual cycles (>97% had ⩾7 recalls). Multiple linear regression was used to determine whether aMED and its specific components were associated with total and regional adiposity after adjusting for age, race, education, physical activity and energy intake.
Results:
Participants had an average (s.d.) aMED of 4.2 (1.7) and percent body fat of 29.5 (6.0)%. Significant inverse associations were found between aMED and all the examined adiposity measures except waist-to-hip ratio. Among the DXA measures, a 1-unit increment in aMED was associated with a 0.06 (95% confidence interval (CI): −0.09, −0.02) lower trunk-to-leg fat ratio (T/L), a measure of upper to lower body fat. In an analysis examining T/L as an outcome with the separate components of the aMED, T/L was lower with increased legume consumption (β=−0.280, 95% CI: −0.550, −0.010) but was higher with increased consumption of red and processed meat (β=0.060, 95% CI: 0.002, 0.117).
Conclusions:
Adherence to the aMED was associated with lower total and regional adiposity, adding to the mounting evidence of the health benefits of the MD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Centers for Disease Control and Prevention. Overweight and obesity. http://www.cdc.gov/obesity/data/adult.html (cited 18 June 2012).
Flegal KM, Carroll MD, Kit BK, Ogden CL . Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999–2010. JAMA 2012; 307: 491–497.
Pasquali R, Patton L, Gambineri A . Obesity and infertility. Curr Opin Endocrinol Diabetes Obes 2007; 14: 482–487.
Zera C, McGirr S, Oken E . Screening for obesity in reproductive-aged women. Prev Chronic Dis 2011; 8: A125.
Jacques PF, Tucker KL . Are dietary patterns useful for understanding the role of diet in chronic disease? Am J Clin Nutr 2001; 73: 1–2.
Bach-Faig A, Berry EM, Lairon D, Reguant J, Trichopoulou A, Dernini S et al. Mediterranean diet pyramid today. Science and cultural updates. Public Health Nutr 2011; 14: 2274–2284.
Willett WC, Sacks F, Trichopoulou A, Drescher G, Ferro-Luzzi A, Helsing E et al. Mediterranean diet pyramid: a cultural model for healthy eating. Am J Clin Nutr 1995; 61: 1402S–1406S.
Buckland G, Bach A, Serra-Majem L . Obesity and the Mediterranean diet: a systematic review of observational and intervention studies. Obes Rev 2008; 9: 582–593.
Branchtein L, Schmidt MI, Mengue SS, Reichelt AJ, Matos MC, Duncan BB . Waist circumference and waist-to-hip ratio are related to gestational glucose tolerance. Diabetes Care 1997; 20: 509–511.
Snijder MB, van Dam RM, Visser M, Seidell JC . What aspects of body fat are particularly hazardous and how do we measure them? Int J Epidemiol 2006; 35: 83–92.
Wactawski-Wende J, Schisterman EF, Hovey KM, Howards PP, Browne RW, Hediger M et al. BioCycle study: design of the longitudinal study of the oxidative stress and hormone variation during the menstrual cycle. Paediatr Perinat Epidemiol 2009; 23: 171–184.
Posner BM, Smigelski C, Duggal A, Morgan JL, Cobb J, Cupples LA . Validation of two-dimensional models for estimation of portion size in nutrition research. J Am Diet Assoc 1992; 92: 738–741.
Fung TT, McCullough ML, Newby PK, Manson JE, Meigs JB, Rifai N et al. Diet-quality scores and plasma concentrations of markers of inflammation and endothelial dysfunction. Am J Clin Nutr 2005; 82: 163–173.
Trichopoulou A, Costacou T, Bamia C, Trichopoulos D . Adherence to a Mediterranean diet and survival in a Greek population. N Engl J Med 2003; 348: 2599–2608.
Craig CL, Marshall AL, Sjostrom M, Bauman AE, Booth ML, Ainsworth BE et al. International physical activity questionnaire: 12-country reliability and validity. Med Sci Sports Exerc 2003; 35: 1381–1395.
Lumley T, Diehr P, Emerson S, Chen L . The importance of the normality assumption in large public health data sets. Annu Rev Public Health 2002; 23: 151–169.
Martinez-Gonzalez MA, de lF-A, Nunez-Cordoba JM, Basterra-Gortari FJ, Beunza JJ, Vazquez Z et al. Adherence to Mediterranean diet and risk of developing diabetes: prospective cohort study. BMJ 2008; 336: 1348–1351.
Romaguera D, Norat T, Mouw T, May AM, Bamia C, Slimani N et al. Adherence to the Mediterranean diet is associated with lower abdominal adiposity in European men and women. J Nutr 2009; 139: 1728–1737.
Trichopoulou A, Naska A, Orfanos P, Trichopoulos D . Mediterranean diet in relation to body mass index and waist-to-hip ratio: the Greek European Prospective Investigation into Cancer and Nutrition Study. Am J Clin Nutr 2005; 82: 935–940.
Panagiotakos DB, Chrysohoou C, Pitsavos C, Stefanadis C . Association between the prevalence of obesity and adherence to the Mediterranean diet: the ATTICA study. Nutrition 2006; 22: 449–456.
Panagiotakos DB, Polystipioti A, Papairakleous N, Polychronopoulos E . Long-term adoption of a Mediterranean diet is associated with a better health status in elderly people; a cross-sectional survey in Cyprus. Asia Pac J Clin Nutr 2007; 16: 331–337.
Rossi M, Negri E, Bosetti C, Dal ML, Talamini R, Giacosa A et al. Mediterranean diet in relation to body mass index and waist-to-hip ratio. Public Health Nutr 2008; 11: 214–217.
Schroder H, Marrugat J, Vila J, Covas MI, Elosua R . Adherence to the traditional mediterranean diet is inversely associated with body mass index and obesity in a spanish population. J Nutr 2004; 134: 3355–3361.
Schroder H, Mendez MA, Ribas-Barba L, Covas MI, Serra-Majem L . Mediterranean diet and waist circumference in a representative national sample of young Spaniards. Int J Pediatr Obes 2010; 5: 516–519.
Shubair MM, McColl RS, Hanning RM . Mediterranean dietary components and body mass index in adults: the peel nutrition and heart health survey. Chronic Dis Can 2005; 26: 43–51.
Beunza JJ, Toledo E, Hu FB, Bes-Rastrollo M, Serrano-Martinez M, Sanchez-Villegas A et al. Adherence to the Mediterranean diet, long-term weight change, and incident overweight or obesity: the Seguimiento Universidad de Navarra (SUN) cohort. Am J Clin Nutr 2010; 92: 1484–1493.
Mendez MA, Popkin BM, Jakszyn P, Berenguer A, Tormo MJ, Sanchez MJ et al. Adherence to a Mediterranean diet is associated with reduced 3-year incidence of obesity. J Nutr 2006; 136: 2934–2938.
Romaguera D, Norat T, Vergnaud AC, Mouw T, May AM, Agudo A et al. Mediterranean dietary patterns and prospective weight change in participants of the EPIC-PANACEA project. Am J Clin Nutr 2010; 92: 912–921.
Sanchez-Villegas A, Bes-Rastrollo M, Martinez-Gonzalez MA, Serra-Majem L . Adherence to a Mediterranean dietary pattern and weight gain in a follow-up study: the SUN cohort. Int J Obes 2006; 30: 350–358.
Woo J, Cheung B, Ho S, Sham A, Lam TH . Influence of dietary pattern on the development of overweight in a Chinese population. Eur J Clin Nutr 2008; 62: 480–487.
Dai J, Jones DP, Goldberg J, Ziegler TR, Bostick RM, Wilson PW et al. Association between adherence to the Mediterranean diet and oxidative stress. Am J Clin Nutr 2008; 88: 1364–1370.
Gaskins AJ, Rovner AJ, Mumford SL, Yeung E, Browne RW, Trevisan M et al. Adherence to a Mediterranean diet and plasma concentrations of lipid peroxidation in premenopausal women. Am J Clin Nutr 2010; 92: 1461–1467.
Schroder H . Protective mechanisms of the Mediterranean diet in obesity and type 2 diabetes. J Nutr Biochem 2007; 18: 149–160.
Kastorini CM, Milionis HJ, Esposito K, Giugliano D, Goudevenos JA, Panagiotakos DB . The effect of Mediterranean diet on metabolic syndrome and its components: a meta-analysis of 50 studies and 534,906 individuals. J Am Coll Cardiol 2011; 57: 1299–1313.
Gunderson EP, Murtaugh MA, Lewis CE, Quesenberry CP, West DS, Sidney S . Excess gains in weight and waist circumference associated with childbearing: The Coronary Artery Risk Development in Young Adults Study (CARDIA). Int J Obes Relat Metab Disord 2004; 28: 525–535.
Gunderson EP, Sternfeld B, Wellons MF, Whitmer RA, Chiang V, Quesenberry CP et al. Childbearing may increase visceral adipose tissue independent of overall increase in body fat. Obesity 2008; 16: 1078–1084.
Smith DE, Lewis CE, Caveny JL, Perkins LL, Burke GL, Bild DE . Longitudinal changes in adiposity associated with pregnancy. The CARDIA Study. Coronary Artery Risk Development in Young Adults Study. JAMA 1994; 271: 1747–1751.
Piers LS, Walker KZ, Stoney RM, Soares MJ, O’Dea K . Substitution of saturated with monounsaturated fat in a 4-week diet affects body weight and composition of overweight and obese men. Br J Nutr 2003; 90: 717–727.
Fung TT, Schulze M, Manson JE, Willett WC, Hu FB . Dietary patterns, meat intake, and the risk of type 2 diabetes in women. Arch Intern Med 2004; 164: 2235–2240.
Zhang C, Schulze MB, Solomon CG, Hu FB . A prospective study of dietary patterns, meat intake and the risk of gestational diabetes mellitus. Diabetologia 2006; 49: 2604–2613.
Acknowledgements
This work was supported by the Intramural Research Program of the Eunice Kennedy Shriver National Institute of Child Health and Human Development, National Institutes of Health (Contract no. HHSN275200403394C). The authors thank the BioCycle working group for comments and feedback on this work.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Boghossian, N., Yeung, E., Mumford, S. et al. Adherence to the Mediterranean diet and body fat distribution in reproductive aged women. Eur J Clin Nutr 67, 289–294 (2013). https://doi.org/10.1038/ejcn.2013.4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2013.4
Keywords
This article is cited by
-
Adherence to the Mediterranean diet as a possible additional tool to be used for screening the metabolically unhealthy obesity (MUO) phenotype
Journal of Translational Medicine (2023)
-
Association between adherence to the Mediterranean diet with cardiometabolic risk factors: a cross-sectional study on PERSIAN cohort study in Fasa
Scientific Reports (2023)
-
The association between dietary diabetic risk reduction score with anthropometric and body composition variables in overweight and obese women: a cross-sectional study
Scientific Reports (2023)
-
Adherence to the Mediterranean diet and its association with environmental footprints among women of childbearing age in the United Arab Emirates
European Journal of Nutrition (2022)
-
Defining the impact of dietary macronutrient balance on PCOS traits
Nature Communications (2020)