Abstract
Background/Objectives:
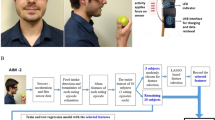
The SenseCam is a camera worn on a lanyard around the neck that automatically captures point-of-view images in response to movement, heat and light (every 20–30 s). This device may enhance the accuracy of self-reported dietary intake by assisting participants’ recall of food and beverage consumption. It was the objective of this study to evaluate if the wearable camera, SenseCam, can enhance the 24-h dietary recall by providing visual prompts to improve recall of food and beverage consumption.
Subject/Methods:
Thirteen volunteer adults in Oxford, United Kingdom, were recruited. Participants wore the SenseCam for 2 days while continuing their usual daily activities. On day 3, participants’ diets were assessed using an interviewer-administered 24-h recall. SenseCam images were then shown to the participants and any additional dietary information that participants provided after viewing the images was recorded. Energy and macronutrient intakes were compared between the 24-h recall and 24-h recall+SenseCam.
Results:
Data from 10 participants were included in the final analysis (8 males and 2 females), mean age 33±11 years, mean BMI 25.9±5.1 kg/m2. Viewing the SenseCam images increased self-reported energy intake by approximately 1432±1564 kJ or 12.5% compared with the 24-h recall alone (P=0.02). The increase was predominantly due to reporting of 41 additional foods (241 vs 282 total foods) across a range of food groups. Eight changes in portion size were made, which resulted in a negligible change to energy intake.
Conclusions:
Wearable cameras are promising method to enhance the accuracy of self-reported dietary assessment methods.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Thompson FE, Subar A . Dietary assessment methodology. In: Coulston A, Boushe C (eds). Nutrition in the Prevention and Treatment of Disease. Academic Press: San Diego, 2001, pp 3–30.
Livingstone MB, Black AE . Markers of the validity of reported energy intake. J Nutr 2003; 133 (Suppl 3), 895S–920S.
Jonnalagadda SS, Mitchell DC, Smiciklas-Wright H, Meaker KB, Heel NV, Karmally W et al. Accuracy of energy intake data estimated by a multiplepass, 24-hour dietary recall technique. J Am Diet Assoc 2000; 100: 303–311.
Sawaya AL, Tucker K, Tsay R, Willett W, Saltzman E, Dallal GE et al. Evaluation of four methods for determining energy intake in young and older women: comparison with doubly labeled water measurements of total energy expenditure. Am J Clin Nutr 1996; 63: 491–499.
Briefel R, Sempos CT, McDowell M, Chien S, Alaimo K . Dietary methods research in the third National Health and Nutrition Examination Survey: underreporting of energy intake. Am J Clin Nutr 1997; 65: 1203S–1209S.
Heywood P, Harvey P, Marks GC . An evaluation of energy intakes in the 1983 Australian National Dietary Survey of Adults. Eur J Clin Nutr 1993; 47: 604–606.
Pikholz C, Swinburn B, Metcalf P . Under-reporting of energy intake in the 1997 National Nutrition Survey. N Z Med J 2004; 117: 1–11.
Tran KM, Johnson RK, Soultanakis RP, Matthews DE . In-person vs telephone-administered multiple-pass 24-hour recalls in women: validation with doubly labeled water. J Am Diet Assoc 2000; 100: 777–783.
Bathalon GP, Tucker KL, Hays NP, Vinken AG, Greenberg AS, McCrory MA et al. Psychological measures of eating behavior and the accuracy of 3 common dietary assessment methods in healthy postmenopausal women. Am J Clin Nutr 2000; 71: 739–745.
Kroke A, Klipstein-Grobusch K, Voss S, Möseneder J, Thielecke F, Noack R et al. Validation of a self-administered food-frequency questionnaire administered in the European Prospective Investigation into Cancer and Nutrition (EPIC) Study: comparison of energy, protein, and macronutrient intakes estimated with the doubly labeled water, urinary nitrogen, and repeated 24-h dietary recall methods. Am J Clin Nutr 1999; 70: 439–447.
Thompson FE, Subar AF, Loria CM, Reedy JL, Baranowski T . Need for technological innovation in dietary assessment. J Am Diet Assoc 2010; 110: 48–51.
Illner A, Freisling H, Boeing H, Huybrechts I, Crispim S, Slimani N . Review and evaluation of innovative technologies for measuring diet in nutritional epidemiology. Int J Epidemiol 2012; 41: 1187–1203.
Blanton CA, Moshfegh AJ, Baer DJ, Kretsch MJ . The USDA Automated Multiple-Pass Method accurately estimates group total energy and nutrient intake. J Nutr 2006; 136: 2594–2599.
Moshfegh AJ, Rhodes DG, Baer DJ, Murayi T, Clemens JC, Rumpler WV et al. The US Department of Agriculture Automated Multiple-Pass Method reduces bias in the collection of energy intakes. Am J Clin Nutr 2008; 88: 324–332.
Subar AF, Kirkpatrick SI, Mittl B, Zimmerman TP, Thompson FE, Bingley C et al. The Automated Self-Administered 24-Hour Dietary Recall (ASA24): a resource for researchers, clinicians, and educators from the National Cancer Institute. J Acad Nutr Diet 2012; 112: 1134–1137.
Google 2013, (cited 16 May 2013). Available from http://www.google.com/glass/start/what-it-does/.
Arab L, Wesseling-Perry K, Jardack P, Henry J, Winter A . Eight self-administered 24-hour dietary recalls using the Internet are feasible in African Americans and Whites: the energetics study. J Am Diet Assoc 2010; 110: 857–864.
Arab L, Estrin D, Kim DH, Burke J, Goldman J . Feasibility testing of an automated image-capture method to aid dietary recall. Eur J Clin Nutr 2011; 65: 1156–1162.
Hodges S, Williams L, Berry E, Izadi S, Srinivasan J, Butler A et al. SenseCam: a retrospective memory aid. In: Dourish P, Friday A (eds). UbiComp 2006: Ubiquitous Computing; 2006 Sep 17-21; Springer-Verlag: Orange County, California, USA, 2006, pp 177–193.
Gemmell J, Williams L, Wood K, Lueder R, Brown G (eds). Passive capture and ensuing issues for a personal lifetime store. Proceedings of the 1st ACM workshop on continuous archival and retrieval of personal experiences. 15th October, Microsoft, New York, USA, 2004.
Cherry S . Total recall [life recording software]. Spectrum, IEEE 2005; 42: 24–30.
Hodges S, Berry E, Wood K . SenseCam: a wearable camera which stimulates and rehabilitates autobiographical memory. Memory 2011; 19: 685–696.
Browne G, Berry E, Kapur N, Hodges S, Smyth G, Watson P et al. SenseCam improves memory for recent events and quality of life in a patient with memory retrieval difficulties. Memory 2011; 19: 713–722.
Berry E, Kapur N, Williams L, Hodges S, Watson P, Smyth G et al. The use of a wearable camera, SenseCam, as a pictorial diary to improve autobiographical memory in a patient with limbic encephalitis: a preliminary report. Neuropsychol Rehabi 2007; 17: 582–601.
Doherty AR, Hodges SE, King A, Smeaton AF, Berry E, Moulin CJA et al. Wearable Cameras in Health: The State of the Art and Future Possibilities. Am J Prev Med 2012; 44: 320–323.
Kelly P, Doherty AR, Hamilton A, Matthews A, Batterham AM, Nelson M et al. Evaluating the feasibility of measuring travel to school using a wearable camera. Am J Prev Med 2012; 2012: 5.
Kelly P, Doherty A, Berry E, Hodges S, Batterham AM, Foster C . Can we use digital life-log images to investigate active and sedentary travel behaviour? Results from a pilot study. Int J Behav Nutr Phys Act 2011; 8: 44.
Kerr J, Marshall SJ, Godbole S, Chen J, Legge A, Doherty AR et al. Using the SenseCam to improve classifications of sedentary behavior in free-living settings. Am J Prev Med 2013; 44: 290–296.
Doherty AR, Kelly P, Kerr J, Marshall SJ, Oliver M, Badland H et al. Use of wearable cameras to assess population physical activity behaviours: an observational study. Lancet Public Health Science Conference 2012; 380: S35.
O'Loughlin G, Cullen SJ, McGoldrick A, O'Connor S, Warrington GD . Using a wearable camera to increase the accuracy of dietary analysis. Am J Prev Med 2013; 44: 297–301.
Probst Y . Food portion images for dietary assessement: graduated food portion photos of Australian foods. The University of Wollongong: Wollongong, 2012.
Doherty AR, Moulin CJ, Smeaton AF . Automatically assisting human memory: a sensecam browser. Memory 2010; 19: 785–795.
Sun M, Fernstrom JD, Jia W, Hackworth SA, Yao N, Li Y et al. A wearable electronic system for objective dietary assessment. J Am Diet Assoc 2010; 110: 45–47.
Higgins JA, LaSalle AL, Zhaoxing P, Kasten MY, Bing KN, Ridzon SE et al. Validation of photographic food records in children: are pictures really worth a thousand words&quest. Eur J Clin Nutr 2009; 63: 1025–1033.
Daugherty BL, Schap TE, Ettienne-Gittens R, Zhu FM, Bosch M, Delp EJ et al. Novel technologies for assessing dietary intake: evaluating the usability of a mobile telephone food record among adults and adolescents. J Med Internet Res 2012; 14: e58.
Rollo ME, Ash S, Lyons-Wall P, Russell A . Trial of a mobile phone method for recording dietary intake in adults with type 2 diabetes: evaluation and implications for future applications. J Telemed Telecare 2011; 17: 318–323.
Barnard J, Tapsell L, Davies P, Brenninger V, Storlien L . Relationship of high energy expenditure and variation in dietary intake with reporting accuracy on 7 day food records and diet histories in a group of healthy adult volunteers. Eur J Clin Nutr 2002; 56: 358–367.
Hernández T, Wilder L, Kuehn D, Rubotzky K, Moser-Veillon P, Godwin S et al. Portion size estimation and expectation of accuracy. J Food Compost Anal 2006; 19: S14–S21.
Nelson M, Atkinson M, Darbyshire S . Food photography. I: The perception of food portion size from photographs. Br J Nutr 1994; 72: 649–663.
Ovaskainen M, Paturi M, Reinivuo H, Hannila M, Sinkko H, Lehtisalo J et al. Accuracy in the estimation of food servings against the portions in food photographs. Eur J Clin Nutr 2007; 62: 674–681.
Tooze JA, Subar AF, Thompson FE, Troiano R, Schatzkin A, Kipnis V . Psychosocial predictors of energy underreporting in a large doubly labeled water study. Am J Clin Nutr 2004; 79: 795–804.
Kretsch MJ, Fong AKH, Green MW . Behavioral and body size correlates of energy intake underreporting by obese and normal-weight women. J Am Diet Assoc 1999; 99: 300–306.
Lichtman SW, Pisarska K, Berman ER, Pestone M, Dowling H, Offenbacher E et al. Discrepancy between self-reported and actual caloric intake and exercise in obese subjects. N Engl J Med 1992; 327: 1893–1898.
Hebert JR, Clemow L, Pbert L, Ockene IS, Ockene JK . Social desirability bias in dietary self-report may compromise the validity of dietary intake measures. Int J Epidemiol 1995; 24: 389–398.
Hebert JR, Ma Y, Clemow L, Ockene IS, Saperia G, Stanek EJ et al. Gender differences in social desirability and social approval bias in dietary self-report. Am J Epidemiol 1997; 146: 1046–1055.
Black A, Goldberg G, Jebb S, Livingstone M, Cole T, Prentice A . Critical evaluation of energy intake data using fundamental principles of energy physiology: 2. Evaluating the results of published surveys. Eur J Clin Nutr 1991; 45: 583.
Poppitt S, Swann D, Black A, Prentice A . Assessment of selective under-reporting of food intake by both obese and non-obese women in a metabolic facility. Int J Obes 1998; 22: 303.
Bandini LG, Schoeller DA, Cyr HN, Dietz WH . Validity of reported energy intake in obese and nonobese adolescents. Am J Clin Nutr 1990; 52: 421–425.
Prentice AM, Black A, Coward W, Davies H, Goldberg G, Murgatroyd P et al. High levels of energy expenditure in obese women. BMJ 1986; 292: 983.
Johnson RK, Soultanakis RP, Matthews DE . Literacy and body fatness are associated with underreporting of energy intake in US low-income women using the multiple-pass 24-hour recall: a doubly labeled water study. J Am Diet Assoc 1998; 98: 1136–1140.
Berry E, Hampshire A, Rowe J, Hodges S, Kapur N, Watson P et al. The neural basis of effective memory therapy in a patient with limbic encephalitis. J Neurol Neurosurg Psychiatry 2009; 80: 1202–1205.
Acknowledgements
We thank the participants and the British Heart Foundation Heart Promotion Research Group, University of Oxford, for their expertise, guidance and technical support for SenseCam research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Gemming, L., Doherty, A., Kelly, P. et al. Feasibility of a SenseCam-assisted 24-h recall to reduce under-reporting of energy intake. Eur J Clin Nutr 67, 1095–1099 (2013). https://doi.org/10.1038/ejcn.2013.156
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2013.156
Keywords
This article is cited by
-
Automated wearable cameras for improving recall of diet and time use in Uganda: a cross-sectional feasibility study
Nutrition Journal (2023)
-
Validation of improved 24-hour dietary recall using a portable camera among the Japanese population
Nutrition Journal (2021)
-
Daily metabolic expenditures: estimates from US, UK and polish time-use data
BMC Public Health (2019)
-
Evaluation of a smartphone food diary application using objectively measured energy expenditure
International Journal of Behavioral Nutrition and Physical Activity (2017)
-
Smart-Glasses: Exposing and Elucidating the Ethical Issues
Science and Engineering Ethics (2017)