Abstract
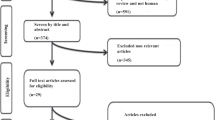
To date, there has been inconclusive evidence regarding the effect of magnesium supplements on blood pressure (BP). This meta-analysis was conducted to assess the effect of magnesium supplementation on BP and to establish the characteristics of trials showing the largest effect size. Primary outcome measures were systolic blood pressure (SBP) and diastolic blood pressure (DBP) at the end of the follow-up period. One hundred and forty-one papers were identified, of which 22 trials with 23 sets of data (n=1173), with 3 to 24 weeks of follow-up met the inclusion criteria, with a supplemented elemental magnesium range of 120–973 mg (mean dose 410 mg). 95% confidence intervals (CI) were calculated using DerSimonian and Laird's random-effects model, with effect size calculated using Hedges G. Combining all data, an overall effect of 0.36 and 0.32 for DBP and SBP, respectively, was observed (95% CI 0.27–0.44 for DBP and 0.23–0.41 for SBP), with a greater effect being seen for the intervention in crossover trials (DBP 0.47, SBP 0.51). Effect size increased in line with increased dosage. Although not all individual trials showed significance in BP reduction, combining all trials did show a decrease in SBP of 3–4 mm Hg and DBP of 2–3 mm Hg, which further increased with crossover designed trials and intake >370 mg/day. To conclude, magnesium supplementation appears to achieve a small but clinically significant reduction in BP, an effect worthy of future prospective large randomised trials using solid methodology.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
References
Lawes CMM, Vander Hoorn S, Rodgers A . The International Society of Hypertension, global burden of blood-pressure-related disease. Lancet 2008; 371, 1513–1518.
Bo S, Pisu E . Role of magnesium in cardiovascular disease prevention, insulin sensitivity and diabetes. Curr Opin Lipidol 2008; 19, 50–56.
Ma J, Folsom AR, Melnick SL, Eckfeldt JH, Sharrett AR, Nabulsi AA et al. Associations of serum and dietary magnesium with cardiovascular disease, hypertension, diabetes and carotid arterial wall thickness: the ARIC study. J Clin Epidemiol 1995; 48, 927–940.
Kawano Y, Matsuoka H, Takishita S, Omae T . Effects of magnesium supplementation in hypertensive patients, assessment by office, home, and ambulatory blood pressures. Hypertension 1998; 32, 260–265.
Altura BM . Importance of Mg in physiology and medicine and the need for ion selective electrodes. Scand J Clin Lab Invest 1994; 54 (Suppl 217), 5–9.
Department of Health. Dietary Reference Values for Food Energy and Nutrients for the United Kingdom. Report of the Panel on Dietary Reference Values, Committee on Medical Aspects of Food and Nutrition Policy. HMSO: London, 1991.
Bohl CH, Volpe SL . Magnesium and exercise. Crit Rev Food Sci Nutr 2002; 42, 533–563.
Choudhury A, Lip GYH . Exercise and hypertension. J Hum Hypertens 2005; 19, 585–587.
Burgess E, Lewanczuk R, Bolli P, Chockalingam A, Cutler H, Taylor G et al. Recommendations on potassium, magnesium and calcium. Canad Med Assoc J 1999; 160 (Suppl 9), S35–S45.
Dickinson HO, Nicolson D, Campbell F, Cook JF, Beyer FR, Ford GA et al. Magnesium supplementation for the management of essential hypertension in adults. Cochrane Database Syst Rev 2006; (19), CD004640.
Jee SH, Edgar R, Miller III, Guallar E, Singh VK, Appel LJ et al. The effect of magnesium supplementation on blood pressure: a meta-analysis of randomized clinical trials. Am J Hypertens 2002; 15, 691–696.
Hedges LV, Olkin I . Statistical Methods for Meta-Analysis. Academic Press: Orlando, 1985.
Morris SB . Distribution of the standardized mean change effect size for meta-analysis on repeated measures. Br J Math Stat Psychol 2000; 53 (Part 1), 17–29.
DerSimonian R, Laird N . Meta-analysis in clinical trials. Control Clin Trials 1986; 7, 177–187.
Guerrero-Romero F, Tamez-Perez HE, Gonzalez-Gonzalez G, Salinas-Martinez AM, Montes-Villarreal J, Trevino-Ortiz JH et al. Oral magnesium supplementation improves insulin sensitivity in non-diabetic subjects with insulin resistance. A double-blind placebo-controlled randomized trial. Diab Metab 2004; 30, 253–258.
Henderson DG, Schierup J, Schodt T . Effect of magnesium supplementation on blood pressure and electrolyte concentrations in hypertensive patients receiving long term diuretic treatment. Br Med J 1986; 293, 664–665.
Doyle L, Flynn A, Cashman K . The effect of magnesium supplementation on biochemical markers of bone metabolism or blood pressure in healthy young adult females. Eur J Clin Nutr 1999; 53, 255–261.
Sacks FM, Willett WC, Smith A, Brown LE, Rosner B, Moore TJ . Effect on blood pressure of potassium, calcium and magnesium in women with low habitual intake. Hypertension 1998; 31, 131–138.
Witteman JCM, Grobbee DE, Derkx FHM, Bouillon R, de Bruijn AM, Hofman A . Reduction of blood pressure with oral magnesium supplementation in women with mild to moderate hypertension. Am J Clin Nutr 1994; 60, 129–135.
Guerrero-Romero F, Rodriguez-Moran M . The effect of lowering blood pressure by magnesium supplementation in diabetic hypertensive adults with low serum magnesium levels: a randomized, double-blind, placebo-controlled clinical trial. J Hum Hypertens 2009; 23, 245–251.
Rodriguez-Moran M, Guerrero-Romero F . Oral magnesium supplementation improves insulin sensitivity and metabolic control in type 2 diabetic subjects. Diabetes Care 2003; 26, 1147–1152.
Purvis JR, Cummings DM, Landsman P, Carroll R, Barakat H, Bray J et al. Effect of oral magnesium supplementation on selected cardiovascular risk factors in non-insulin-dependent diabetics. Arch Family Med 1994; 3, 503–508.
Hattori K, Saito K, Sano H, Fukuzaki H . Intracellular magnesium deficiency and effect of oral magnesium on blood pressure and red cell sodium transport in diuretic-treated hypertensive patients. Jpn Circ J 1988; 52, 1249–1256.
Borrello G, Mastroroberto P, Curcio F, Chello M, Zofrea S, Mazza ML . The effects of magnesium oxide on mild essential hypertension and quality of life. Curr Ther Res 1996; 57, 767–774.
Zemel PC, Zemel MB, Urberg M, Douglas FL, Geiser R, Sowers JR . Metabolic and hemodynamic effects of magnesium supplementation in patients with essential hypertension. Am J Clin Nutr 1990; 51, 665–669.
The ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group. Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs diuretic: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). JAMA 2002; 288, 2981–2997.
Mizushima S, Cappuccio FP, Nichols R, Elliott P . Dietary magnesium intake and blood pressure: a qualitative overview of the observational studies. J Hum Hypertens 1998; 12, 447–453.
Lee S, Park HK, Son SP, Lee CW, Kim IJ, Kim HJ . Effects of oral magnesium supplementation on insulin sensitivity and blood pressure in normo-magnesemic nondiabetic overweight Korean adults. Nutr Metab Cardiovasc Dis 2009; 19, 781–788.
Lind L, Lithell H, Pollare T, Ljunghall S . Blood pressure response during long-term treatment with magnesium is dependent on magnesium status. Am J Hypertens 1991; 4, 674–679.
Ferrara LA, Iannuzzi R, Castaldo A, Iannuzzi A, Russo AD, Mancini M . Long-term magnesium supplementation in essential hypertension. Cardiology 1992; 81, 25–33.
Wirell MP, Wester PO, Stegmayr BG . Nutritional dose of magnesium in hypertensive patients on beta blockers lowers systolic blood pressure: a double-blind cross-over study. J Intern Med 1994; 236, 189–195.
Plum-Wirell M, Stegmay BG, Weste PO . Nutritional magnesium supplementation does not change blood pressure nor serum or muscle potassium and magnesium in untreated hypertension. A double-blind crossover study. Magn Res 1994; 7, 277–283.
Itoh K, Kawasaki T, Nakamur M . The effects of high oral magnesium supplementation on blood pressure, serum lipids and related variables in apparently healthy Japanese subjects. Br J Nutr 1997; 78, 737–750.
Sanjuliani AF, Fagundes VGA, Francischetti EA . Effects of magnesium on blood pressure and intracellular ion levels of Brazilian hypertensive patients. Intern J Cardiol 1996; 56, 177–183.
Paolisso G, Di Maro G, Cozzolino D, Salvatore T, D’Amore A, Lama D et al. Chronic magnesium administration enhances oxidative glucose metabolism in thiazide treated hypertensive patients. Am J Hypertens 1992; 5, 681–686.
Cappuccio FP, Markandu ND, Beynon GW, Shore AC, Sampson B, MacGregor GA . Lack of effect of oral magnesium on high blood pressure: a double blind study. Br Med J 1985; 291, 235–238.
Widman L, Wester PO, Stegmayr BK, Wirell M . The dose-dependent reduction in blood pressure through administration of magnesium. Am J Hypertens 1993; 6, 41–45.
Nielsen FH, Lukaski HC . Update on the relationship between magnesium and exercise. Magn Res 2006; 19, 180–189.
Acknowledgements
The authors are grateful to Dr David Wellsted and the Centre for Lifespan and Chronic Illness Research (CLiCIR), University of Hertfordshire, for their invaluable advice and support on this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kass, L., Weekes, J. & Carpenter, L. Effect of magnesium supplementation on blood pressure: a meta-analysis. Eur J Clin Nutr 66, 411–418 (2012). https://doi.org/10.1038/ejcn.2012.4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2012.4
Keywords
This article is cited by
-
The Association between Dietary Magnesium Intake and Telomere Length in Adults with Hypertension
The Journal of nutrition, health and aging (2022)
-
The Effects of Magnesium Supplementation on Blood Pressure and Obesity Measure Among Type 2 Diabetes Patient: a Systematic Review and Meta-analysis of Randomized Controlled Trials
Biological Trace Element Research (2021)
-
Effects of magnesium citrate, magnesium oxide and magnesium sulfate supplementation on arterial stiffness in healthy overweight individuals: a study protocol for a randomized controlled trial
Trials (2019)
-
Nutrients and Nutraceuticals for the Management of High Normal Blood Pressure: An Evidence-Based Consensus Document
High Blood Pressure & Cardiovascular Prevention (2019)
-
Synergistic effect of fruit–seed mixed juice on inhibition of angiotensin I-converting enzyme and activation of NO production in EA.hy926 cells
Food Science and Biotechnology (2019)