Abstract
Background/Objectives:
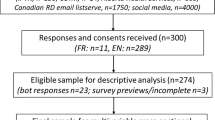
Recommendations state that all hospital patients should be screened for malnutrition and for each level of risk, a suitable care plan should be available. This study investigates current practice at ward level regarding adherence to a care plan generated from a nutrition screening tool, and then aims to improve basic nutritional support actions by modifying a care plan and finally evaluates change in practice.
Subjects/Methods:
Pro formas were completed on nutrition care plans of 100 patients. Subsequently, 7 focus groups were conducted, which included 30 ward staff and 6 dietitians. Care plans were re-designed using information from focus groups, followed by a second set of pro formas on the care plans of 103 patients.
Results:
Themes regarding barriers and facilitators for completion of care plans were derived from the focus groups including: ‘duplication’, ‘time pressures’, ‘leadership support’, ‘operational issues’, ‘document style’ and ‘training’. Pro formas before and after re-design showed that nutritional support actions increased from 13 (9%) to 98 (52%) for patients at moderate or severe risk of malnutrition (P=0.033).
Conclusions:
Focus groups allowed engagement with ward staff to explore how care plans were used, which assisted in re-designing the care plan, while the pro formas identified limitations of initial procedures and then evaluated change. Subsequently, basic nutritional support actions that resulted from screening improved. The suitability of care plans to facilitate basic nutritional support and documentation was enhanced. However, improvements are still required, emphasising the necessity for continued training and a strategic approach to the delivery of basic nutritional care.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Council of Europe. Food and Nutritional Care in Hospitals: How to Prevent Undernutrition Nutrition Programmes in Hospitals Group for the Committee of Experts on Nutrition, Food & Safety and Consumer Health. Strasbourg: Council of Europe 2003.
National Collaborating Centre for Acute Care. Nutrition Support in Adults: Oral Nutrition Support, Enteral Tube Feeding and Parenteral Nutrition. NICE Clinical Guideline 32: London, 2006.
Department of Health Essence of Care Benchmarking for Food and Drink. Her Majesty’s Stationery Office, United Kingdom 2010.
National Patient Safety Agency Patient Environment Action Team Assessment. National Patient Safety Agency, London 2010.
Westergren A, Wann-Hansson C, Bergh Börgdal E, Sjölander J, Strömblad R, Klevsgård R et al. Malnutrition prevalence and precision in nutritional care differed in relation to hospital volume – a cross-sectional survey. Nutr J 2009; 8: 1–8.
Russell C, Elia M Nutrition Screening Survey in the UK in 2008. British Association of Enteral and Parenteral Nutrition 2008.
Stratton RJ, Green CJ, Elia M Disease-Related Malnutrition: An Evidence-Based Approach to Treatment. CAB International: Wallingford, 2003.
British Association for Parenteral and Enteral Nutrition. Hospital Food as Treatment. British Association for Parenteral and Enteral Nutrition: Maidenhead, Berks, 1999.
Weekes CE, Spiro A, Baldwin C, Whelan K, Thomas JE, Parkin D et al. A review of the evidence for the impact of improving nutritional care on nutritional and clinical outcomes and cost. J Hum Nutr Diet 2009; 22: 324–335.
Department of Health Equity and Excellence. Liberating the NHS: 2010 The Stationery Office, United Kingdom http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@en/@ps/documents/digitalasset/dh_117794.pdf Accessed 24 June 2011.
Kruizenga HM, Van Tulder MW, Seidell JC, Thijs A, Ader HJ, Van Bokhorst-de van der Schueren MA . Effectiveness and cost effectiveness of early screening and treatment of malnourished patients. Am J Clin Nutr 2005; 82: 1082–1089.
Kondrup J, Johansen N, Plum LM, Bak L, Larsen IH, Martinsen A et al. Incidence of nutritional risk and causes of inadequate nutritional care in hospitals. Clin Nutr 2002; 21: 461–468.
Brugler LJ, DiPrinzio MJ, Bernstein L . The five-year evolution of a malnutrition treatment program in a community hospital. Jt Comm J Qual Improv 1999; 25: 191–206.
Rypkema S, Adang G, Dicke E, Naber H, de Swart T, Disselhorst B et al. Cost-effectiveness of an interdisciplinary intervention in geriatric inpatients to prevent malnutrition. J Nutr Health Aging 2003; 8: 122–127.
O’Flynn J, Peake H, Hickson M, Foster D, Frost G . The prevalence of malnutrition in hospitals can be reduced: results from three consecutive cross-sectional studies. Clin Nutr 2005; 24: 1078–1088.
Miles M, Huberman M Qualitative Data Analysis: A Source Book for New Methods. Sage Publications: Thousand Oaks, CA, 1994.
Thomas JM, Isenring E, Kellett E . Nutritional status and length of stay in patients admitted to an Acute Assessment Unit. J Hum Nutr Diet 2007; 20: 320–328.
Ruxton CH, Gordon J, Kirkwood L, McMillan B, Ryan E . Risk of malnutrition in a sample of acute and long-stay NHS Fife in-patients: an audit. J Hum Nutr Diet 2008; 21: 81–90.
Edington J, Boorman J, Durrant ER, Perkins A, Giffin CV, James R et al. Prevalence of malnutrition on admission to four hospitals in England. The Malnutrition Prevalence Group. Clin Nutr 2000; 19: 191–195.
Smoliner C, Norman K, Wagner K, Hartig W, Lochs H, Pirlich M . Malnutrition and depression in the institutionalised elderly. Br J Nutr 2009; 102: 1663–1667.
Stratton RJ, Hackston A, Longmore D, Dixon R, Price S, Stroud M et al. Malnutrition in hospital outpatients and inpatients: prevalence, concurrent validity and ease of use of the ‘Malnutrition Universal Screening Tool (MUST)’. Brit J Nutr 2004; 92: 799–808.
Jefferies D, Johnson M, Ravens J . Nurturing and nourishing: the nurses’ role in nutritional care. J Clin Nurs 2011; 20: 317–330.
Nursing and Midwifery Council The Code: Standards of Conduct, Performance and Ethics for Nurses and Midwives 2008 Nursing and Midwifery Council London.
British Dietetic Association Code of Professional Conduct. The British Dietetic Association Birmingham 2008.
O’Cathain A, Murphy E, Nicoll J . Why, and how, mixed methods research is undertaken in health services research in England: a mixed methods approach Health Service Research. BMC Health Serv Res 2007; 7: 85.
Acknowledgements
We thank E Rowlands for assistance with some of the data collection, and nurses, patients and dietitians who participated and gave their valuable comments regarding this evaluation process. This research was fully funded by the Chairman’s Research Prize Scholarship. CC undertook data collection, analysis of qualitative work from the transcriptions and assisted with the manuscript. EB assisted with data collection and assisted with the manuscript; SB designed the study and undertook data analysis on quantitative data, and prepared the manuscript. All authors critically reviewed the manuscript and approved the final version. This work was undertaken at the Manchester Biomedical Research Centre (http://www.manchesterbrc.org/).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Cooper, C., Brierley, E. & Burden, S. Improving adherence to a care plan generated from the Malnutrition Universal Screening Tool. Eur J Clin Nutr 67, 174–179 (2013). https://doi.org/10.1038/ejcn.2012.196
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2012.196
Keywords
This article is cited by
-
The Integrated Nutrition Pathway for Acute Care (INPAC): Building consensus with a modified Delphi
Nutrition Journal (2015)