Abstract
Background/Objectives:
Nutritional intervention with oral nutritional supplements (ONS) has been shown to increase quality of life in malnourished patients. We investigated whether post-hospital supplementation with ONS is cost-effective according to international benchmarks in malnourished patients.
Subjects/Methods:
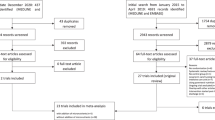
In total, 114 malnourished patients (50.6±16.1 years, 57 female) with benign gastrointestinal disease were included and randomised to receive either ONS for 3 months and dietary counselling at discharge (intervention, n=60) or only dietary counselling at discharge (control group, n=54). Nutritional status was assessed with Subjective Global Assessment. Intervention patients documented daily intake of ONS; quality of life was assessed with Short-Form (SF)-36 Health Survey and SF-36 values were transformed into health-status utilities. Quality-adjusted life years (QALYs) were calculated by adopting the area under the curve method. We used two different pricing scenarios for ONS (minimum price: €2.30 and maximum: €2.93/tetrapack). The incremental cost-effectiveness ratio (ICER) of supplementation with ONS was calculated for both price scenarios. All analyses were corrected for age and gender.
Results:
Intervention patients consumed 2.4±0.8 ONS per day. Intervention and control patients did not differ in their health status utilities at baseline (0.594±0.017 vs 0.619±0.018), but after 3 months, the health status utilities were significantly higher in intervention patients than in control patients (0.731±0.015 vs 0.671±0.016, P=0.028). Intervention was associated with significantly higher costs (ICER: €9497 and €12 099/additional QALY, respectively) but deemed cost-effective according to international thresholds (<€50 000/QALY).
Conclusions:
A 3-month intervention with ONS increases quality of life in malnourished patients. This treatment appears to be cost-effective according to international benchmarks.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Beattie AH, Prach AT, Baxter JP, Pennington CR (2000). A randomised controlled trial evaluating the use of enteral nutritional supplements postoperatively in malnourished surgical patients. Gut 46, 813–818.
Braga M, Gianotti L (2005). Preoperative immunonutrition: cost-benefit analysis. JPEN J Parenter Enteral Nutr 2, S57–S61.
Brazier J, Roberts J, Deverill M (2002). The estimation of a preference-based measure of health from the SF-36. J Health Econ 21, 271–292.
Claxton K (1999). The irrelevance of inference: a decision-making approach to the stochastic evaluation of health care technologies. J Health Econ 18, 341–364.
Dalziel K, Segal L (2007). Time to give nutrition interventions a higher profile: cost-effectiveness of 10 nutrition interventions. Health Promot Int 22, 271–283.
Darmon P, Lochs H, Pichard C (2008). Economic impact and quality of life as endpoints of nutritional therapy. Curr Opin Clin Nutr Metab Care 11, 452–458.
Detsky AS, McLaughlin JR, Baker JP, Johnston N, Whittaker S, Mendelson RA et al. (1987). What is subjective global assessment of nutritional status? JPEN J Parenter Enteral Nutr 11, 8–13.
Efron B (1979). Bootstrap methods: another look at the jackknife. Ann Statist 7, 1–26.
Elia M, Stratton RJ (2008). A cost-utility analysis in patients receiving enteral tube feeding at home and in nursing homes. Clin Nutr 27, 416–423.
Gianotti L, Braga M, Frei A, Greiner R, Di CV (2000). Health care resources consumed to treat postoperative infections: cost saving by perioperative immunonutrition. Shock 14, 325–330.
Jones NE, Suurdt J, Ouelette-Kuntz H, Heyland DK (2007). Implementation of the Canadian Clinical Practice Guidelines for Nutrition Support: a multiple case study of barriers and enablers. Nutr Clin Pract 22, 449–457.
Lochs H (2006). ESPEN guidelines on adult enteral nutrition. Clin Nutr 25, 177–360.
Lothgren M, Zethraeus N (2000). Definition, interpretation and calculation of cost-effectiveness acceptability curves. Health Econ 9, 623–630.
McWhirter JP, Pennington CR (1994). Incidence and recognition of malnutrition in hospital. BMJ 308, 945–948.
Norman K, Kirchner H, Freudenreich M, Ockenga J, Lochs H, Pirlich M (2008a). Three month intervention with protein and energy rich supplements improve muscle function and quality of life in malnourished patients with non-neoplastic gastrointestinal disease—a randomized controlled trial. Clin Nutr 27, 48–56.
Norman K, Pichard C, Lochs H, Pirlich M (2008b). Prognostic impact of disease-related malnutrition. Clin Nutr 27, 5–15.
Raftery J (2001). NICE: faster access to modern treatments? Analysis of guidance on health technologies. BMJ 323, 1300–1303.
Reinhold T, Bruggenjurgen B, Schlander M, Rosenfeld S, Hessel F, Willich SN (2010). Economic analysis based on multinational studies—methods for adapting findings to national contexts. J Public Health 18: 327–335.
Richardson G, Manca A (2004). Calculation of quality adjusted life years in the published literature: a review of methodology and transparency. Health Econ 13, 1203–1210.
Russell C (2007). The impact of malnutrition on healthcare costs and economic considerations for the use of oral nutritional supplements. Clin Nutr 2, 25–32.
Senkal M, Zumtobel V, Bauer KH, Marpe B, Wolfram G, Frei A et al. (1999). Outcome and cost-effectiveness of perioperative enteral immunonutrition in patients undergoing elective upper gastrointestinal tract surgery: a prospective randomized study. Arch Surg 134, 1309–1316.
Simmons SF, Zhuo X, Keeler E (2010). Cost-effectiveness of nutrition interventions in nursing home residents: a pilot intervention. J Nutr Health Aging 14, 367–372.
Smedley F, Bowling T, James M, Stokes E, Goodger C, O’Connor O et al. (2004). Randomized clinical trial of the effects of preoperative and postoperative oral nutritional supplements on clinical course and cost of care. Br J Surg 91, 983–990.
Thompson SG, Barber JA (2000). How should cost data in pragmatic randomised trials be analysed? BMJ 320, 1197–1200.
Ware Jr JE, Gandek B, Kosinski M, Aaronson NK, Apolone G, Brazier J et al. (1998). The equivalence of SF-36 summary health scores estimated using standard and country-specific algorithms in 10 countries: results from the IQOLA Project. International Quality of Life Assessment. J Clin Epidemiol 51, 1167–1170.
Ware Jr JE., Sherbourne CD (1992). The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 30, 473–483.
Willich SN, Reinhold T, Selim D, Jena S, Brinkhaus B, Witt CM (2006). Cost-effectiveness of acupuncture treatment in patients with chronic neck pain. Pain 125, 107–113.
Witt CM, Reinhold T, Jena S, Brinkhaus B, Willich SN (2009). Cost-effectiveness of acupuncture in women and men with allergic rhinitis: a randomized controlled study in usual care. Am J Epidemiol 169, 562–571.
Zethraeus N, Johannesson M, Jonsson B, Lothgren M, Tambour M (2003). Advantages of using the net-benefit approach for analysing uncertainty in economic evaluation studies. Pharmacoeconomics 21, 39–48.
Acknowledgements
This study was financially supported by a grant from Fresenius Kabi, Bad Homburg, Germany.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Registered at Clinical Trials.gov: NCT00168935
Rights and permissions
About this article
Cite this article
Norman, K., Pirlich, M., Smoliner, C. et al. Cost-effectiveness of a 3-month intervention with oral nutritional supplements in disease-related malnutrition: a randomised controlled pilot study. Eur J Clin Nutr 65, 735–742 (2011). https://doi.org/10.1038/ejcn.2011.31
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2011.31
Keywords
This article is cited by
-
Study protocol for an open labelled randomised controlled trial of perioperative oral nutrition supplement in breast and colorectal cancer patients undergoing elective surgery
Trials (2021)
-
Cost-effectiveness analysis of oral nutritional supplements with nutritional counselling in head and neck cancer patients undergoing radiotherapy
Cost Effectiveness and Resource Allocation (2021)
-
Economic evaluation of an extended nutritional intervention in older Australian hospitalized patients: a randomized controlled trial
BMC Geriatrics (2018)
-
Effect on body weight, quality of life and appetite following individualized, nutritional counselling to home-living elderly after rehabilitation – An open randomized trial
The Journal of nutrition, health and aging (2017)
-
The Cost-Effectiveness of Oral Nutrition Supplementation for Malnourished Older Hospital Patients
Applied Health Economics and Health Policy (2017)