Abstract
Background/Objectives:
Plasma zinc is an important biomarker of zinc status, but the concentration is depressed by inflammation.
Subjects/Methods:
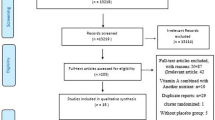
Apparently healthy adults, who tested positive twice for human immunodeficiency virus (HIV) but who had not reached stage IV or clinical AIDS, were randomly allocated to receive a food supplement (n=17 and 21) or the food plus a micronutrient capsule (MN; n=10 men and n=33 women) containing 15 mg zinc/day. We used the inflammation biomarkers, C-reactive protein (CRP) and α1-acid glycoprotein (AGP), to identify subjects with and without inflammation and determine the effect of inflammation on the response of plasma zinc concentrations to the MN and food supplements.
Results:
There were no differences between men and women either in plasma zinc or in the responses to the supplements and their data were combined. Plasma zinc was lower in those with inflammation than without. Repeated measures analysis of variance (ANOVA) showed that inflammation blocked increases in plasma zinc, and there was an approximate 10% increase in plasma zinc concentration in response to the MN supplement (P=0.023) in those without inflammation. Subgroup analysis showed mean changes in plasma zinc of 0.95 and −0.83 μmol/l (P=0.031) in response to the MN and food treatments, respectively, in those without inflammation at both time points.
Conclusions:
Inflammation seems to block any increase in plasma zinc after MN supplement and it is important to identify those without inflammation to determine the effectiveness of a zinc supplementation program.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Abebe Y, Bogale A, Hambidge KM, Stoecker B, Bailey KB, Gibson RS (2007). Phytate, zinc, iron and calcium content of selected raw and prepared foods consumed in rural Sidama, Southern Ethiopia, and implications for bioavailability. J Fd Comp Anal 20, 161–168.
Aggett PJ, Favier A (1993). Zinc. Int J Vit Nutr Res 63, 301–307.
Bates CJ, Pentieva KD, Prentice A, Mansoor MA, Finch S (1999). Plasma pyridoxal phosphate and pyridoxic acid and their relationship to plasma homocysteine in a representative sample of British men and women aged 65 years and over. Brit J Nutr 81, 191–201.
Baum MK, Shor-Posner G, Guoyan Z, Hong L, Quesada JA, Campa A et al. (1997). HIV-1 infection in women is associated with severe nutritional deficiencies. J Acqu Imm Def Syndr 16, 272–278.
Beisel WR (1976). Trace elements in infectious processes. Med Clin North Am 60, 831–849.
Brown KH (1998). Effect of infections on plasma zinc concentration and implications for zinc status assessment in low-income countries. Am J Clin Nutr 68, 425S–429S.
Brown KH, Lanata CF, Yuen ML, Peerson JM, Butron B, Lonnerdal B (1993). Potential magnitude of misclassification of a population's trace element status due to infection: example from a survey of young Peruvian children. Am J Clin Nutr 58, 549–554.
Brown KH, Wessells KR, Hess SY (2007). Zinc bioavailability from zinc-fortified foods. Int J Vit Nutr Res 77, 174–181.
Calvin J, Neale G, Fotherby KJ, Price CP (1988). The relative merits of acute phase proteins in the recognition of inflammatory conditions. Ann Clin Biochem 25, 60–66.
Cousins RJ, Leinart AS (1988). Tissue-specific regulation of zinc metabolism and metallothionein genes by interleukin 1. FASEB J 2, 2884–2890.
Dacie JV, Lewis SM (1995). Practical Haematology. Churchill Livingston: London, 559–563.
Darboe MK, Thurnham DI, Morgan G, Adegbola RA, Secka O, Solon J et al. (2007). Effectiveness of the new IVACG early high-dose vitamin A supplementation scheme compared to the standard WHO protocol: a randomised controlled trial in Gambian mothers and infants. Lancet 369, 2088–2096.
Dawson JB, Ellis DJ, Newton-John H (1968). Direct estimation of copper in serum and urine by atomic absorption spectroscopy. Clin Chim Acta 21, 33–42.
English JL, Hambidge KM (1988). Plasma and serum zinc concentrations: effect of time between collection and separation. Clin Chim Acta 175, 211–215.
Fleck A, Myers MA (1985). Diagnostic and prognostic significance of acute phase proteins. In: Gordon AH, Koj A (eds). The Acute Phase Response to Injury and Infection. Elsevier Scientific Publishers: Amsterdam. pp 249–271.
Friis H, Sandstrom B (2002). Zinc and HIV infection. In: Friis H (ed). Micronutrients and HIV Infection, CRC Series in Modern Nutrition. CRC Press: Boca Raton, Florida, pp 159–181.
Galloway P, McMillan DC, Sattar N (2000). Effect of the inflammatory response on trace element and vitamin status. Ann Clin Biochem 37, 289–297.
Gibson RS, Abebe Y, Stabler S, Allen RH, Westcott JE, Stoecker BJ et al. (2008). Zinc, gravida, infection, and iron, but not vitamin B-12 or folate status, predict hemoglobin during pregnancy in Southern Ethiopia. J Nutr 138, 581–586.
Gibson RS, Fergusson EL (1998). Assessment of dietary zinc in a population. Am J Clin Nutr 68, 430S–434S.
Graham NMH, Sorensen D, Odaka N, Brookmeyer R, Chan D, Willett WC et al. (1991). Relationship of serum copper and zinc levels to HIV-1 seropositivity and progression to AIDS. J Acquir Immune Defic Syndr 4, 976–980.
Hambidge KM (2003). Biomarkers of trace mineral intake and status. J Nutr 133 (Suppl 3), 948S–955S. Links 133,948S-955S.
Hotz C, Brown KH eds). (2004). International Zinc Nutrition Consultative Group (IZiNCG) assessment of the risk of zinc deficiency in populations and options for its control. Food Nutr Bull 25, S94–S204.
Hotz C, Peerson JM, Brown KH (2003). Suggested lower cutoffs of serum zinc concentrations for assessing zinc status: reanalysis of the second National Health and Nutrition Examination Survey data (1976–1980). Am J Clin Nutr 78, 756–764.
Jansson LT, Kling S, Dallman PR (1986). Anemia in children with acute infections seen in primary care pediatric outpatient clinic. Pediatr Infect Dis J 5, 424–427.
Kasperek K, Kiem J, Iyengar GV, Feinendegen LE (1981). Concentration differences between serum and plasma of the elements cobalt, iron, mercury, rubidium, selenium and zinc determined by neutron activation analysis. Sci Total Environ 17, 133–143.
Mburu ASW, Mwaniki DL, Thurnham DI, Selenje L, de Wagt A, Muniu EM et al. (2004). Effects of multi-micronutrient supplements and food aid rations on the nutritional status and health of HIV+ adults (MINIFAR) (Report to UNICEF July 2004). 1–209. CPHR-KEMRI: Nairobi, Kenya. 1–7–2004.
Mburu ASW, Thurnham DI, Mwaniki DL, Muniu EM, Alumasa F, de Wagt A (2008). The influence and benefits of controlling for inflammation on plasma ferritin and hemoglobin responses following a multi-micronutrient supplement in apparently-healthy, HIV+ Kenyan adults. J Nutr 138, 613–619.
Murphy SP, Beaton GH, Calloway DH (1992). Estimated mineral intakes of toddlers: predicted prevalence of inadequacy in village populations in Egypt, Kenya, and Mexico. Am J Clin Nutr 56, 565–572.
Mwaniki DL, Omwega AM, Minui EM, Mutunga JN, Akelola R, Shako BR et al. (2001). Anaemia, Status of Iron, Vitamin A, Zinc in Kenya. The 1999 National Survey Report. 1–221.. Ministry of Health: Nairobi.
Nemeth E, Valore EV, Territo M, Schiller G, Lichtenstein A, Ganz T (2003). Hepcidin, a putative mediator of anemia of inflammation, is a type II acute-phase protein. Blood 101, 2462–2463.
Papathakis PC, Rollins NC, Chantry CJ, Bennish ML, Brown KH (2007). Micronutrient status during lactation in HIV-infected and HIV-uninfected South African women during the first 6 mo after delivery. Am J Clin Nutr 85, 182–192.
Paracha PI, Jamil A, Northrop-Clewes CA, Thurnham DI (2000). Interpretation of vitamin A status in apparently-healthy Pakistani children using markers of sub-clinical infection. Am J Clin Nutr 72, 1164–1169.
Stuart J, Whicher JT (1988). Tests for detecting and monitoring the acute phase response. Arch Dis Child 63, 115–117.
Thompson D, Milford-Ward A, Whicher JT (1992). The value of acute phase protein measurements in clinical practice. Ann Clin Biochem 29, 123–131.
Thurnham DI (1997). Impact of disease on markers of micronutrient status. Proc Nutr Soc 56, 421–431.
Thurnham DI (2007). Bioequivalence of β-carotene and retinol. J Sci Fd Agric 87, 13–39.
Thurnham DI, Mburu ASW, Mwaniki DL, Muniu EM, Alumasa F, de Wagt A (2008). Using plasma acute-phase protein concentrations to interpret nutritional biomarkers in apparently healthy HIV-1-seropositive Kenyan adults. Brit J Nutr 100, 174–182.
Thurnham DI, McCabe GP, Northrop-Clewes CA, Nestel P (2003). Effect of subclinical infection on plasma retinol concentrations and assessment of prevalence of vitamin A deficiency: meta-analysis. Lancet 362, 2052–2058.
Wieringa FT, Dijkhuizen MA, West CE, Northrop-Clewes CA, Muhilal (2002). Estimation of the effect of the acute phase response on indicators of micronutrient status in Indonesian infants. J Nutr 132, 3061–3066.
Young B, Gleeson M, Cripps AW (1991). C-reactive protein: a critical review. Pathology 23, 118–124.
Acknowledgements
We thank the Government Chemist, Nairobi for zinc analyses and Pharma Natura, South Africa for the placebo and MN capsules. We also thank Arjan de Wagt for his enthusiastic assistance in setting up the study and many fruitful discussions of the results. We thank UNICEF and the Dutch Government for providing funds to do the work in Kenya under project number SSA/KENB/2002/00002302-03. The study sponsors had no part in the study design, in the collection, analysis and interpretation of data and in the writing of this paper or in our decision to submit for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Mburu, A., Thurnham, D., Mwaniki, D. et al. The influence of inflammation on plasma zinc concentration in apparently healthy, HIV+ Kenyan adults and zinc responses after a multi-micronutrient supplement. Eur J Clin Nutr 64, 510–517 (2010). https://doi.org/10.1038/ejcn.2010.33
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2010.33
Keywords
This article is cited by
-
The effect of inflammation on serum zinc concentrations and the prevalence estimates of population-level zinc status among Congolese children aged 6–59 months
European Journal of Clinical Nutrition (2017)
-
Evaluation of Serum Trace Element Levels and Superoxide Dismutase Activity in Patients with Inflammatory Bowel Disease: Translating Basic Research into Clinical Application
Biological Trace Element Research (2017)
-
Serum Zinc Concentration and C-Reactive Protein in Individuals with Human Immunodeficiency Virus Infection: the Positive Living with HIV (POLH) Study
Biological Trace Element Research (2016)
-
Correlation of selenium and zinc levels to antiretroviral treatment outcomes in Thai HIV-infected children without severe HIV symptoms
European Journal of Clinical Nutrition (2012)