Abstract
Background/Objective:
Little is known about the precise role of parental migrant status (MS) and educational level (EL) on adiposity and various eating habits in young children. Therefore, we assessed their independent contribution in preschoolers.
Subjects/Methods:
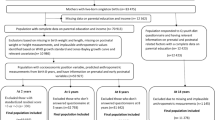
Of 655 randomly selected preschoolers, 542 (5.1±0.6 years; 71% of parental MS and 37% of low parental EL) were analysed. Body composition was measured by bioelectrical impedance. Eating habits were assessed using a semiqualitative food frequency questionnaire and analysed according to five messages developed by the Swiss Society for Nutrition, based on factors implicated in childhood obesity: (1) ‘Drinking water and decreasing sweetened drinks’, (2) ‘Eating fruit and vegetables’, (3) ‘Decreasing breakfast skipping’, (4) ‘Reducing fatty and sweet foods’ and (5) ‘Reducing the intake of meals and snacks in front of television’.
Results:
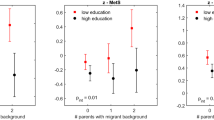
Children of migrant and low EL parents had higher body fat, ate more meals and snacks while watching television and had more fruit and fatty foods compared with their respective counterparts (all P⩽0.04). Children of low EL parents also consumed less water and vegetables compared with their counterparts (all P⩽0.04). In most instances, we found an independent contribution of parental MS and EL to adiposity and eating habits. A more pronounced effect was found if both parents were migrants or of low EL. Differences in adiposity and eating habits were relatively similar to the joint parental data when assessed individually for maternal and paternal MS and EL.
Conclusions:
Parental MS and EL are independently related to adiposity and various eating habits in preschoolers.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Birch LL, Marlin DW (1982). I don’t like it; I never tried it: effects of exposure on two-year-old children's food preferences. Appetite 3, 353–360.
Blass EM, Anderson DR, Kirkorian HL, Pempek TA, Price I, Koleini MF (2006). On the road to obesity: television viewing increases intake of high-density foods. Physiol Behav 88, 597–604.
Bowman SA, Gortmaker SL, Ebbeling CB, Pereira MA, Ludwig DS (2004). Effects of fast-food consumption on energy intake and diet quality among children in a national household survey. Pediatrics 113, 112–118.
Caprio S, Daniels SR, Drewnowski A, Kaufman FR, Palinkas LA, Rosenbloom AL et al. (2008). Influence of race, ethnicity, and culture on childhood obesity: implications for prevention and treatment: a consensus statement of Shaping America's Health and the Obesity Society. Diabetes Care 31, 2211–2221.
Coon KA, Goldberg J, Rogers BL, Tucker KL (2001). Relationships between use of television during meals and children's food consumption patterns. Pediatrics 107, E7.
Coon KA, Tucker KL (2002). Television and children's consumption patterns. A review of the literature. Minerva Pediatr 54, 423–436.
Drewnowski A, Darmon N, Briend A (2004). Replacing fats and sweets with vegetables and fruits—a question of cost. Am J Public Health 94, 1555–1559.
Dubois L, Farmer A, Girard M, Peterson K (2008). Social factors and television use during meals and snacks is associated with higher BMI among pre-school children. Public Health Nutr 11, 1267–1279.
Ebenegger V, Marques-Vidal P, Barral J, Kriemler S, Puder JJ, Nydegger A (2010). Eating habits of preschool children with high migrant status in Switzerland according to a new food frequency questionnaire. Nutr Res 30, 104–109.
Ekelund U, Sardinha LB, Anderssen SA, Harro M, Franks PW, Brage S et al. (2004). Associations between objectively assessed physical activity and indicators of body fatness in 9- to 10-y-old European children: a population-based study from 4 distinct regions in Europe (the European Youth Heart Study). Am J Clin Nutr 80, 584–590.
Evenson KR, Catellier DJ, Gill K, Ondrak KS, McMurray RG (2008). Calibration of two objective measures of physical activity for children. J Sports Sci 26, 1557–1565.
Field AE, Gillman MW, Rosner B, Rockett HR, Colditz GA (2003). Association between fruit and vegetable intake and change in body mass index among a large sample of children and adolescents in the United States. Int J Obes Relat Metab Disord 27, 821–826.
Forshee RA, Anderson PA, Storey ML (2008). Sugar-sweetened beverages and body mass index in children and adolescents: a meta-analysis. Am J Clin Nutr 87, 1662–1671.
Hendy HM (1999). Comparison of five teacher actions to encourage children's new food acceptance. Ann Behav Med 21, 20–26.
Huerta M, Bibi H, Haviv J, Scharf S, Gdalevich M (2006). Parental smoking and education as determinants of overweight in Israeli children. Prev Chronic Dis 3, A48.
Huybrechts I, De Backer G, De Bacquer D, Maes L, De Henauw N (2009). Relative validity and reproducibility of a food-frequency questionnaire for estimating food intakes among flemish preschoolers. Int J Environ Res Public Health 6, 382–399.
Kimm SY, Barton BA, Berhane K, Ross JW, Payne GH, Schreiber GB (1997). Self-esteem and adiposity in black and white girls: the NHLBI Growth and Health Study. Ann Epidemiol 7, 550–560.
Kriemler S, Puder J, Zahner L, Roth R, Braun-Fahrlander C, Bedogni G (2009). Cross-validation of bioelectrical impedance analysis for the assessment of body composition in a representative sample of 6- to 13-year-old children. Eur J Clin Nutr 63, 619–626.
Lasserre AM, Chiolero A, Cachat F, Paccaud F, Bovet P (2007). Overweight in Swiss children and associations with children's and parents’ characteristics. Obesity (Silver Spring) 15, 2912–2919.
Muckelbauer R, Libuda L, Clausen K, Toschke AM, Reinehr T, Kersting M (2010). Immigrational background affects the effectiveness of a school-based overweight prevention program promoting water consumption. Obesity (Silver Spring) 18, 528–534.
Munoz KA, Krebs-Smith SM, Ballard-Barbash R, Cleveland LE (1997). Food intakes of US children and adolescents compared with recommendations. Pediatrics 100, 323–329.
Nicklas TA, Yang SJ, Baranowski T, Zakeri I, Berenson G (2003). Eating patterns and obesity in children. The Bogalusa Heart Study. Am J Prev Med 25, 9–16.
Niederer I, Kriemler S, Zahner L, Burgi F, Ebenegger V, Hartmann T et al. (2009). Influence of a lifestyle intervention in preschool children on physiological and psychological parameters (Ballabeina): study design of a cluster randomized controlled trial. BMC Public Health 9, 94.
Patrick H, Nicklas TA (2005). A review of family and social determinants of children′s eating patterns and diet quality. J Am Coll Nutr 24, 83–92.
Prader A, Largo RH, Molinari L, Issler C (1989). Physical growth of Swiss children from birth to 20 years of age. First Zurich longitudinal study of growth and development. Helv Paediatr Acta Suppl 52, 1–125.
Reilly JJ (2002). Assessment of childhood obesity: national reference data or international approach? Obes Res 10, 838–840.
Sausenthaler S, Kompauer I, Mielck A, Borte M, Herbarth O, Schaaf B et al. (2007). Impact of parental education and income inequality on children's food intake. Public Health Nutr 10, 24–33.
Tohill BC, Seymour J, Serdula M, Kettel-Khan L, Rolls BJ (2004). What epidemiologic studies tell us about the relationship between fruit and vegetable consumption and body weight. Nutr Rev 62, 365–374.
Turrell G, Kavanagh AM (2006). Socio-economic pathways to diet: modelling the association between socio-economic position and food purchasing behaviour. Public Health Nutr 9, 375–383.
Wolfe WS, Campbell CC, Frongillo Jr EA, Haas JD, Melnik TA (1994). Overweight schoolchildren in New York State: prevalence and characteristics. Am J Public Health 84, 807–813.
Acknowledgements
This study was principally supported by the Swiss National Science Foundation (Grant No. 3200B0-116837) and Health Promotion Switzerland (Project No. 2104). Additional funding was obtained from a research award for Interdisciplinary Research from the University of Lausanne, a Takeda research award, the Wyeth Foundation for the Health of children and adolescents, the Freie Akademische Gesellschaft and an unrestricted educational grant from Nestlé. We thank Professors R Gaillard, S Fanconi and F Ohl who had helped to make this study possible. A special thank to all the children, their parents, the schoolteachers and the respective school health services.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Ebenegger, V., Marques-Vidal, PM., Nydegger, A. et al. Independent contribution of parental migrant status and educational level to adiposity and eating habits in preschool children. Eur J Clin Nutr 65, 210–218 (2011). https://doi.org/10.1038/ejcn.2010.248
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2010.248
Keywords
This article is cited by
-
Cardiometabolic risk profile among children with migrant parents and role of parental education: the IDEFICS/I.Family cohort
International Journal of Obesity (2023)
-
Socioeconomic position and body composition in childhood in high- and middle-income countries: a systematic review and narrative synthesis
International Journal of Obesity (2021)
-
Factors associated with water consumption among children: a systematic review
International Journal of Behavioral Nutrition and Physical Activity (2019)
-
The relationship between body mass index and children’s presentations to a tertiary pediatric emergency department
Italian Journal of Pediatrics (2018)
-
The Swiss Preschoolers’ health study (SPLASHY): objectives and design of a prospective multi-site cohort study assessing psychological and physiological health in young children
BMC Pediatrics (2016)