People - Concepts & Themes / Alamy Stock Vector
Certain viral infections (for example, measles) are known to have lasting effects on immune responses to other infections. But little is known about how COVID-19 affects subsequent responses to other pathogens, particularly for people who experience mild COVID-19.
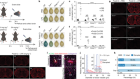
Sparks et al. used elaborate systems immunology and longitudinal single-cell multi-omics to see what happens to the immune system after recovery from mild COVID-19 and after an encounter with its next antigenic exposure — in this case, vaccination against influenza — several weeks or months later.
During 2020, they enrolled and compared people who had recovered from mild COVID-19 with age- and sex-matched control participants who had never had the disease. They were surprised to find that male recoverees had better responses to vaccination against influenza than those of female recoverees (and also had better responses than those of males who never had COVID-19). This was due to an altered baseline immune status that was sustained after recovery, which made the immune system more ‘poised’ to respond to vaccination.
This study not only adds to the understanding of the changing immune states in humans in response to mild COVID-19 but also provides a basis for the study of other, more complex immunological scenarios.
Nature (2023)

 Read more research highlights selected by the Nature Medicine team
Read more research highlights selected by the Nature Medicine team