- OUTLOOK
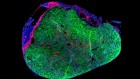
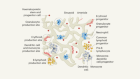
How organoids are advancing the understanding of chronic kidney disease
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 615, S10-S11 (2023)
doi: https://doi.org/10.1038/d41586-023-00652-7
This article is part of Nature Outlook: Chronic kidney disease, an editorially independent supplement produced with the financial support of third parties. About this content.
References
Taguchi, A. et al. Cell Stem Cell 14, 53–67 (2014).
Tucker, N. R. et al. Circulation. 142, 466–482 (2020).
Vanslambrouck, J. M. et al. Nature Commun. 13, 5943 (2022).
Shi, M. et al. Nature Biotechnol. 41, 252–261 (2023).
Wiersma, L. E. et al. Stem Cell Res. Ther. 13, 208 (2022).
Tran, T. et al. Cell Stem Cell 29, 1083–1101 (2022).

 Researchers tackle chronic kidney disease
Researchers tackle chronic kidney disease
 SGLT2 inhibitors breathe life into kidney-disease care
SGLT2 inhibitors breathe life into kidney-disease care
 Stop denying kidney transplants to non-citizens
Stop denying kidney transplants to non-citizens
 The pursuit of dialysis equity
The pursuit of dialysis equity
 Confronting racial and ethnic disparities in diabetic kidney disease
Confronting racial and ethnic disparities in diabetic kidney disease
 Could implantable artificial kidneys end the need for dialysis?
Could implantable artificial kidneys end the need for dialysis?
 The genetic revolution transforming kidney disease
The genetic revolution transforming kidney disease
 Chronic kidney disease: highlights from research
Chronic kidney disease: highlights from research