- NEWS
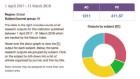
Massive health-record review links viral illnesses to brain disease
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 614, 18-19 (2023)
doi: https://doi.org/10.1038/d41586-023-00181-3
References
Levine, K. S. et al. Neuron https://doi.org/10.1016/j.neuron.2022.12.029 (2023).
Jamieson, G. A., Maitland, J. J., Wilcock, G. K., Craske, J. & Itzhaki, R. F. J. Med. Virol. 33, 224–227 (1991).
Bjornevik, K. et al. Science 375, 296–301 (2022).
Swaddiwudhipong, N. et al. J. Alz. Assoc. https://doi.org/10.1002/alz.12802 (2022).

 The quest to prevent MS — and understand other post-viral diseases
The quest to prevent MS — and understand other post-viral diseases
 Could long COVID be linked to herpes viruses? Early data offer a hint
Could long COVID be linked to herpes viruses? Early data offer a hint
 Are infections seeding some cases of Alzheimer’s disease?
Are infections seeding some cases of Alzheimer’s disease?