- NEWS FEATURE
Superspreading drives the COVID pandemic — and could help to tame it

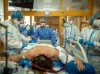
Restaurants and other crowded indoor spaces are prime spots for superspreading events, in which one person passes the virus to many others. Credit: Aaron Lavinsky/Star Tribune/Getty
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 590, 544-546 (2021)
doi: https://doi.org/10.1038/d41586-021-00460-x
References
Liu, Y., Eggo, R. M. & Kucharski, A. J. Lancet 395, E47 (2020).
Endo, A. et al. Wellcome Open Res. 5, 67 (2020).
Volz, E. et al. Preprint at medRxiv https://doi.org/10.1101/2020.12.30.20249034 (2021).
Lemieux, J. E. et al. Preprint at medRxiv https://doi.org/10.1101/2020.08.23.20178236 (2020).
Asadi, S. et al. Sci. Rep. 9, 2348 (2019).
Mürbe, D. et al. Preprint at https://doi.org/10.14279/depositonce-10375.3 (2020).
Viner, R. M. et al. JAMA Paediatr. 175, 143–156 (2021).
Edwards, D. A. et al. Proc. Natl Acad. Sci. USA 118, e2021830118 (2021).
Prentiss, M., Chu, A. & Berggren, K. K. Preprint at medRxiv https://doi.org/10.1101/2020.10.21.20216895 (2020).
Chang, S. et al. Nature 589, 82–87 (2021).
Lau, M. S. Y. et al. Proc. Natl Acad. Sci. USA 117, 22430–22435 (2020).
Endo, A. et al. Wellcome Open Res. 5, 239 (2021).

 COVID-19 rarely spreads through surfaces. So why are we still deep cleaning?
COVID-19 rarely spreads through surfaces. So why are we still deep cleaning?
 Rogue antibodies could be driving severe COVID-19
Rogue antibodies could be driving severe COVID-19
 Why many countries failed at COVID contact-tracing — but some got it right
Why many countries failed at COVID contact-tracing — but some got it right
 How Iceland hammered COVID with science
How Iceland hammered COVID with science
 The false promise of herd immunity for COVID-19
The false promise of herd immunity for COVID-19





