A fleet of COVID-19 vaccine candidates is moving through human studies — and facing concerns that clinical trials are being rushed and patient safety is being compromised. That’s not happening, so it’s not what keeps me up at night. My main worry? The obstacles to getting pandemic vaccines out to the world when, and if, evidence of safety and efficacy do come in. Most of the logistics that will slow delivery are getting scant attention. We must plan for these, to speed things up without compromising safety.
I am not an immunologist, virologist or epidemiologist. For the past 30 years, I have worked as a biotechnology venture capitalist. This May, I was appointed chair of the UK Vaccine Taskforce. Our main job is to identify, manufacture and develop the most promising pandemic vaccines and deliver them rapidly to the populations that need them. COVID-19 gives us an opportunity to create a permanent system for supplying vaccines for future pandemics, quickly and safely; this process must become as routine and reliable as crafting the yearly influenza vaccine.
Time and again, I’ve see outstanding science slowed down by the ‘boring stuff’ — practicalities. That includes delays in manufacturing scale-up and legal approvals slowing pivotal US trials of one of my UK company’s potentially life-saving drugs, or progress hampered by logistics, regulatory disagreements and inadequate data disclosure, as we saw in the Ebola pandemic. Often, the problem is not the science or the clinical trials, but the infrastructure. We must take pains now to make sure this does not stall future pandemic vaccines.
Who gets a COVID vaccine first? Access plans are taking shape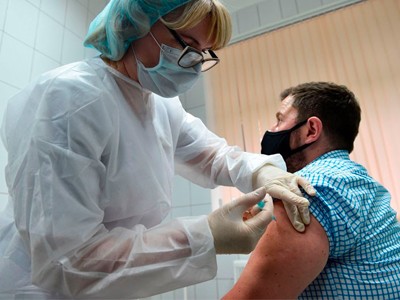
When I agreed to lead the vaccine task force in the United Kingdom, I set conditions to allow quick work. For example, government processes usually require sequential approval from each department involved, but our task force operates at speed and in parallel, and we are funding scale-up of manufacturing in parallel with clinical trials. We have a single ministerial approval process for spending commitments. Such streamlining is essential for developing rapid pandemic countermeasures and decision-making.
An ideal pandemic vaccine would be acceptably safe for everyone, effective in inducing a durable protective immune response, rapidly scalable, stable at room temperature, single dose and cost effective. None of the current candidates has all these characteristics. The front-runner mRNA vaccines demand (very) cold storage, at least two injections and, in some cases, site-of-care dilutions, raising costs and complicating delivery. We need to invest and focus on making vaccines easier to manufacture, transport and administer.
Annual flu vaccines provide a good model for fast regulatory approvals that don’t compromise safety. The shot is developed anew each year for that year’s flu virus, and approval follows a well-worn path. Once a pandemic vaccine format (for instance, mRNA or specific viral vector) has been approved, regulators should consider what new risks a specific vaccine poses, and nimble clinical trials could be designed to mitigate these risks and speed future approvals.
The underdog coronavirus vaccines that the world will need if front runners stumble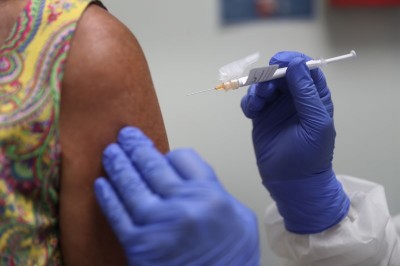
Countries can set up provisions for conditional approval now, to enable the rapid distribution of pandemic vaccines before full authorization is secured. The fact that the US Food and Drug Administration has specified criteria for authorization is a step in the right direction. We also need globally networked infrastructure for real-time, proactive surveillance of adverse events and effectiveness once the vaccines are in use, because it is critical to maintaining public trust and safety.
Over time, we should adopt techniques from cancer-drug development to improve vaccine trials, in particular by connecting immune responses and other biomarkers to clinical outcomes. For COVID-19, controlled human challenge studies could play a part in generating rapid safety and efficacy data when there are treatments to protect volunteers from severe disease.
Manufacture must also be streamlined and global capacity boosted. We need to build flexible and scalable vaccine facilities around the world that can be commandeered for pandemic use when needed. They should be financially sustainable, with a workforce and infrastructure. Investing in low-cost, highly scalable, sterile filling technologies such as high-throughput plastic moulding (to replace costly glass vials) could also save lives.
COVID-vaccine results are on the way — and scientists’ concerns are growing
But I believe the greatest need is for a permanent global pandemic-vaccine purchasing and funding facility so that rich and poor countries can get vaccination in parallel. The COVAX initiative for COVID-19, co-led by GAVI, a funder of immunizations for low-income nations, and supported with, among others, a £500-million (US$647-million) pledge from the United Kingdom, is a promising start. COVAX allows rich countries to buy vaccines for poor countries, alongside buying vaccines for their own citizens. But we were nine months into the pandemic before agreements were formalized. If a global pandemic-vaccine financing mechanism had already been established — as many called for after Ebola — then funding commitments could have taken less than a month, with supply agreements following quickly behind. No bilateral agreements would be needed.
All these efforts must be set up to last beyond COVID-19. At least nine coronaviruses from bats have not crossed into humans. These, plus other zoonotic diseases — and mutations in current strains — make future pandemics likely. Our challenge is to go from unknown infection to vaccination as fast as possible – ideally, in less than six months.


 COVID-vaccine results are on the way — and scientists’ concerns are growing
COVID-vaccine results are on the way — and scientists’ concerns are growing
 The underdog coronavirus vaccines that the world will need if front runners stumble
The underdog coronavirus vaccines that the world will need if front runners stumble
 Who gets a COVID vaccine first? Access plans are taking shape
Who gets a COVID vaccine first? Access plans are taking shape
 Ebola teaches tough lessons about rapid research
Ebola teaches tough lessons about rapid research








