- NEWS
COVID-vaccine results are on the way — and scientists’ concerns are growing
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 586, 16-17 (2020)
doi: https://doi.org/10.1038/d41586-020-02706-6

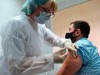 Who gets a COVID vaccine first? Access plans are taking shape
Who gets a COVID vaccine first? Access plans are taking shape
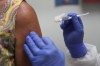 The underdog coronavirus vaccines that the world will need if front runners stumble
The underdog coronavirus vaccines that the world will need if front runners stumble
 The unequal scramble for coronavirus vaccines — by the numbers
The unequal scramble for coronavirus vaccines — by the numbers
 Coronavirus vaccines leap through safety trials — but which will work is anybody’s guess
Coronavirus vaccines leap through safety trials — but which will work is anybody’s guess
 India will supply coronavirus vaccines to the world — will its people benefit?
India will supply coronavirus vaccines to the world — will its people benefit?
 China’s coronavirus vaccines are leaping ahead – but face challenges as virus wanes
China’s coronavirus vaccines are leaping ahead – but face challenges as virus wanes
 The race for coronavirus vaccines: a graphical guide
The race for coronavirus vaccines: a graphical guide






