- NEWS
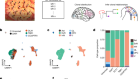
Thousands of people will help scientists to track the long-term health effects of the coronavirus crisis
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 582, 326 (2020)
doi: https://doi.org/10.1038/d41586-020-01643-8

 Coronavirus and COVID-19: Keep up to date
Coronavirus and COVID-19: Keep up to date
 Will antibody tests for the coronavirus really change everything?
Will antibody tests for the coronavirus really change everything?
 Coronavirus blood-clot mystery intensifies
Coronavirus blood-clot mystery intensifies
 How countries are using genomics to help avoid a second coronavirus wave
How countries are using genomics to help avoid a second coronavirus wave
 Dozens of coronavirus drugs are in development — what happens next?
Dozens of coronavirus drugs are in development — what happens next?
 Coronavirus vaccine trials have delivered their first results — but their promise is still unclear
Coronavirus vaccine trials have delivered their first results — but their promise is still unclear
 Anti-vaccine movement could undermine efforts to end coronavirus pandemic, researchers warn
Anti-vaccine movement could undermine efforts to end coronavirus pandemic, researchers warn