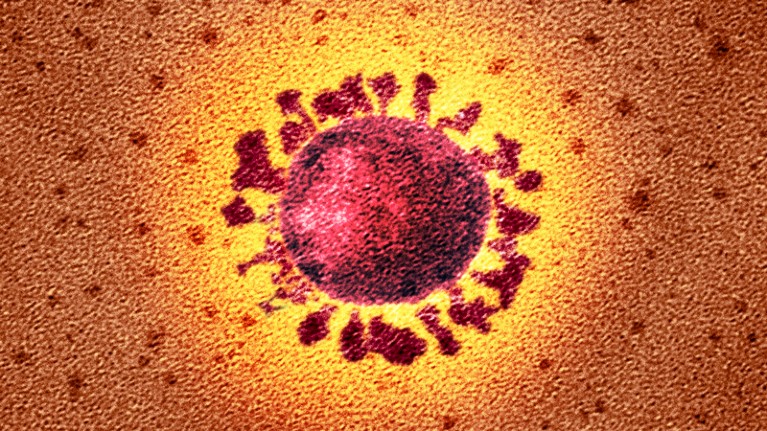
The coronavirus SARS-CoV-2 as seen using a transmission electron microscope.Credit: National Infection Service/SPL
Last week, the leaders of Ghana, Pakistan, Senegal and South Africa joined more than 100 former heads of government, senior officials and leading researchers in an open letter urging that scientific research and intellectual property on coronavirus vaccines be shared freely — and that vaccines be distributed fairly — so that the poorest countries do not lose out. It is unfortunate that such a letter needed to be written in the middle of the worst pandemic of the past 50 years. But it was unavoidable, because some governments — including those funding the first wave of research and clinical trials — have not yet committed to the principles of fully open science and innovation.
This contrasts sharply with the rapid sharing of findings and expertise among researchers that is being reported daily. This week, we cover one of many examples of such collaboration. Since January, researchers have been working across the globe and around the clock to reveal the structures of key proteins that make up the new coronavirus. Their achievements are the result of free-flowing exchange between university laboratories and national synchrotron facilities in countries including China, Germany, the United Kingdom and the United States. Work that would normally have taken months — possibly even years — has been completed in weeks. But rather than building on this cooperation, some countries are retreating into a kind of techno-protectionism, which serves neither science nor society.
The sprint to solve coronavirus protein structures — and disarm them with drugs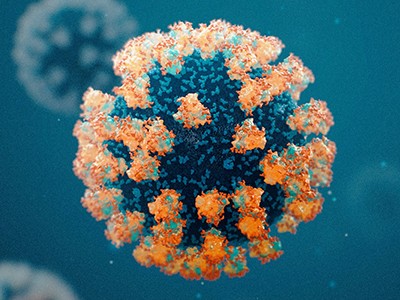
On 10 January, when researchers in China and Australia shared the genome sequence1 for SARS-CoV-2 online, a global network of biologists interested in the structure of viral proteins set to work. The network included the Center for Structural Genomics of Infectious Diseases, a consortium of 40 scientists across 8 institutions in the United States and Canada, which played a central part in the project.
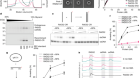
Top of the consortium’s to-do list was to plan which proteins to tackle first, and which lab would take on which protein; the teams then set about getting high-resolution snapshots of these proteins, which enable the virus to enter cells and replicate. Thanks to this work and similar efforts elsewhere, teams have now solved more than 170 structures of whole or partial proteins alone or bound to a drug or receptor. The visualizations generated by this work can be used to find ways to neutralize the virus with drugs or vaccines.
Simultaneously, a team of structural biologists at ShanghaiTech University in China began the task of revealing the structure of a key enzyme, Mpro, that the virus needs to replicate. Work that took two months for SARS-CoV, the virus that caused the outbreak of severe acute respiratory syndrome (SARS) in 2003, this time took just one week. The team deposited its results in the Protein Data Bank — an open-access digital repository for 3D biological structures — ready for researchers around the world to access. As they worked, Shanghai team members collaborated with structural biologists at the University of Oxford, UK, to share knowledge and avoid overlap.
Profile of a killer: the complex biology powering the coronavirus pandemic
But when it comes to distributing some of the fruits of that knowledge, this spirit of cooperation looks to be at risk. It is crucial that any vaccine, once proved to work, can be manufactured and distributed quickly in every country. For this to happen, the holders of intellectual property must pool their know-how — as the developers of open-source software do — so that companies large and small can participate in this emergency effort. Such intellectual-property sharing initiatives are under way, but, as Nature went to press, neither the US nor UK governments seemed ready to support these efforts, preferring to work according to a more conventional model whereby intellectual property for a vaccine is held by those that developed it, and then licensed to anyone wanting to manufacture it.
This is unacceptable during a pandemic, when lives are at stake and the world’s population needs to be immunized. The research that has got us to this point has been pooled, and governments around the world are shouldering much of the risk of funding the vaccine effort. For these reasons, intellectual property has to be shared.
Patent pooling is not simple, but there’s a wealth of literature from life-sciences patent law and case studies from the field of development studies that can help to make it work. And there is an important principle at stake. There is little justice, as economist Mariana Mazzucato at University College London often argues, if citizens have to bear many of the financial risks in such an endeavour, but most of the profits go to a small group of companies (and possibly a few universities) once a vaccine is ready to be rolled out.
Scientists are not exempt from competition: the race to publish a paper or patent a molecule is all too common. But in the race to solve the structure of SARS-CoV-2, the competitors have mostly worked together and shared credit — and that is how they, and the hundreds of researchers working in complementary fields, must continue to work as vaccines and drugs move into clinical trials.
It is a tribute to those scientists involved so far that they immediately understood that a pandemic requires a vastly different way of working. It is a tragedy that some national governments do not.

 The sprint to solve coronavirus protein structures — and disarm them with drugs
The sprint to solve coronavirus protein structures — and disarm them with drugs
 Profile of a killer: the complex biology powering the coronavirus pandemic
Profile of a killer: the complex biology powering the coronavirus pandemic
 The race for coronavirus vaccines: a graphical guide
The race for coronavirus vaccines: a graphical guide
 Coronavirus drugs trials must get bigger and more collaborative
Coronavirus drugs trials must get bigger and more collaborative
 Hopes rise for coronavirus drug remdesivir
Hopes rise for coronavirus drug remdesivir
 Coronavirus and COVID-19: Keep up to date
Coronavirus and COVID-19: Keep up to date