- OUTLOOK
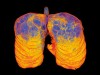
Zombie cells hold clues to COPD progression
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 581, S7-S9 (2020)
doi: https://doi.org/10.1038/d41586-020-01374-w
This article is part of Nature Outlook: COPD, an editorially independent supplement produced with the financial support of third parties. About this content.
References
Rashid, K. et al. Sci. Rep. 8, 9023 (2018).
Kim, S.-J. et al. Aging Cell 18, e12914 (2019).
Houssaini, A. et al. JCI Insight 3, e93203 (2018).
Cheng, X.-Y. et al. Oncotarget 8, 22513–22523 (2017).
Justice, J. N. et al. EBioMedicine 40, 554–563 (2019).
Yin, H.-L. et al. Medicine 96, e6836 (2017).
Xu, M. et al. Nature Med. 24, 1246–1256 (2018).

 Research round-up: COPD
Research round-up: COPD
 Redefining the diagnostic criteria for COPD
Redefining the diagnostic criteria for COPD
 The therapeutic potential of exosomes
The therapeutic potential of exosomes
 Should physicians still be prescribing steroid inhalers as a first-line treatment for COPD?
Should physicians still be prescribing steroid inhalers as a first-line treatment for COPD?
 The environmental concerns driving another inhaler makeover
The environmental concerns driving another inhaler makeover
 How should vulnerable people be protected during wildfires?
How should vulnerable people be protected during wildfires?
 Tracking hotbeds of COPD in Latin American
Tracking hotbeds of COPD in Latin American