- NEWS FEATURE
The next chapter for African genomics

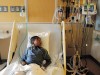
Graduate students at an infectious-disease lab in Ede, Nigeria, use the gene-editing tool CRISPR to detect Lassa virus in blood samples. Credit: Amy Maxmen
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 578, 350-354 (2020)
doi: https://doi.org/10.1038/d41586-020-00454-1
References
Sarfo, F. S. et al. Stroke 49, 1116–1122 (2018).
Siddle, K. J. et al. N. Engl. J. Med. 379, 1745–1753 (2018).
International Monetary Fund. Nigeria: Staff Report for the 2019 Article IV Consultation (IMF, 2019).
Ramachandran, V., Obado-Joel, J., Fatai, R., Masood, J. S. & Blessing, O. The New Economy of Africa: Opportunities for Nigeria’s Emerging Technology Sector (Center for Global Development, 2019).

 Ancient African genomes offer glimpse into early human history
Ancient African genomes offer glimpse into early human history
 Facing up to injustice in genome science
Facing up to injustice in genome science
 Indigenous groups look to ancient DNA to bring their ancestors home
Indigenous groups look to ancient DNA to bring their ancestors home
 Genomics is failing on diversity
Genomics is failing on diversity