- NEWS AND VIEWS
AI shows promise for breast cancer screening
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 577, 35-36 (2020)
doi: https://doi.org/10.1038/d41586-019-03822-8
References
McKinney, S. M. et al. Nature 577, 89–94 (2020).
Neri, E. et al. Insights Imaging 10, 44 (2019).
Lehman, C. D. et al. JAMA Intern. Med. 175, 1828–1837 (2015).
Kohli, A. & Jha, S. J. Am. Coll. Radiol. 15, 535–537 (2018).

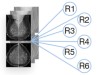 Read the paper: International evaluation of an AI system for breast cancer screening
Read the paper: International evaluation of an AI system for breast cancer screening
 The final frontier in cancer diagnosis
The final frontier in cancer diagnosis
 Deep learning detects impending organ injury in the clinic
Deep learning detects impending organ injury in the clinic