- OUTLOOK
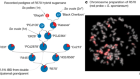
Cannabis’s chemical synergies
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 572, S12-S13 (2019)
doi: https://doi.org/10.1038/d41586-019-02528-1
This article is part of Nature Outlook: Cannabis, an editorially independent supplement produced with the financial support of third parties. About this content.
References
World Health Organization. WHO Expert Committee on Drug Dependence: Fortieth Report. WHO Tech. Rep. Ser. No. 1013 (WHO, 2018).
Ben-Shabat, S. et al. Eur. J. Pharmacol. 353, 23–31 (1998).
Johnson, J. R. et al. J. Pain Symptom Mgmt 39, 167–179 (2010).
Pamplona, F. A., da Silva, L. R. & Coan, A. C. Front. Neurol. 9, 759 (2018).
Lewis, M. A., Russo, E. B. & Smith, K. M. Planta Med. 84, 225–233 (2018).
Baron, E. P., Lucas, P., Eades, J. & Hogue, O. J. Headache Pain 19, 37 (2018).
Fukumoto, S. et al. Stress Health 24, 3–12 (2008).
Russo, E. B. & Marcu, J. Adv. Pharmacol. 80, 67–134 (2017).
Santiago, M., Sachdev, S., Arnold, J. C., McGregor, I. S. & Connor, M. Preprint at bioRxiv https://doi.org/10.1101/569079 (2019).

 The reality behind cannabidiol’s medical hype
The reality behind cannabidiol’s medical hype
 The bioengineering of cannabis
The bioengineering of cannabis
 Can cannabis go green?
Can cannabis go green?
 The professionalization of cannabis growing
The professionalization of cannabis growing
 Working out with weed
Working out with weed
 Weighing the dangers of cannabis
Weighing the dangers of cannabis
 Regulators need to rethink restrictions on cannabis research
Regulators need to rethink restrictions on cannabis research
 Cannabis research round-up
Cannabis research round-up