- NEWS AND VIEWS
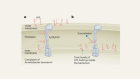
Selective killing of antibiotic-resistant bacteria from within
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 570, 449-450 (2019)
doi: https://doi.org/10.1038/d41586-019-01852-w
References
López-Igual, R. et al. Nature Biotechnol. https://doi.org/10.1038/s41587-019-0105-3 (2019).
Bikard, D. et al. Nature Biotechnol. 32, 1146–1150 (2014).
Citorik, R. J., Mimee, M. & Lu, T. K. Nature Biotechnol. 32, 1141–1145 (2014).
Hughes, D. & Andersson, D. I. Annu. Rev. Microbiol. 71, 579–596 (2017).
Nelson, E. J. et al. Nature Rev. Microbiol. 7, 693–702 (2009).
Ali, M., Nelson, A. R., Lopez, A. L. & Sack, D. A. PLoS. Negl. Trop. Dis. 9, e0003832 (2015).

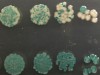 Read the paper: Engineered toxin–intein antimicrobials can selectively target and kill antibiotic-resistant bacteria in mixed population
Read the paper: Engineered toxin–intein antimicrobials can selectively target and kill antibiotic-resistant bacteria in mixed population
 Genetic ‘weapon’ picks off pathogens — but spares beneficial microbes
Genetic ‘weapon’ picks off pathogens — but spares beneficial microbes
 Bacterial persister cells tackled
Bacterial persister cells tackled