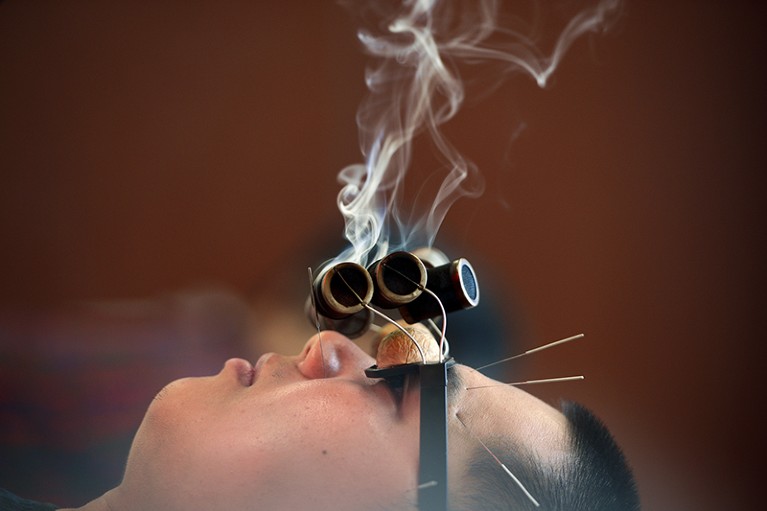
There is little substantial evidence for the efficacy of many treatments in traditional Chinese medicine.Credit: VCG/Getty
Donkeys are a hot item in Africa. In the past few years, prices for the animals and their hides have jumped so high that people have been stealing them. Some countries, including Niger, Tanzania and Botswana, have resorted to banning exports to preserve their donkey populations. And last month, Nigeria’s government moved to make the killing and export of donkeys illegal there.
This donkey rush is driven by the annual 15-billion-yuan (US$2.2-billion) market for ejiao, a gelatin made by boiling donkey skins. It is a highly prized ingredient in traditional Chinese medicine (TCM), believed to stop bleeding and fight coughs and cancer. Demand has surged over the past few decades as China’s wealthy population has grown: a 250-gram box can sell for a couple of hundred dollars. As prices have risen, and donkey populations have fallen inside China (from 9.4 million in 1996 to 4.6 million in 2016), the country has looked to Africa. Other animals are threatened more. The Chinese appetite for TCM remedies has helped to push species including tigers, rhinoceroses, sea horses and pangolins to the brink of extinction.
This situation is all the more troubling because there is little evidence that the preparations made from these animal products actually deliver the promised benefits. TCM is based on unsubstantiated theories about meridians and qi. Most Western-trained doctors and medical researchers regard TCM practices with scepticism: there is no substantial evidence that most of them work, and some signs that a few do harm.
How China is redrawing the map of world science
Signals about TCM from the Chinese government are contradictory. On the one hand, China advertises a belief in evidence-based medicine and has invested millions of yuan in programmes devoted to the modernization and standardization of TCM. That’s welcome — but so far, these programmes have only given a veneer of legitimacy to treatments that have not been rigorously tested in randomized, controlled clinical trials. On the other hand, TCM is big business that receives strong government support. Last January, the Chinese government decreased import taxes on donkey hides from 5% to 2% to ensure the supply. It enthusiastically promotes TCM around the world, often on the back of its massive Belt and Road Initiative, and it stifles criticism of TCM at home.
These mixed signals are now worryingly mirrored by the World Health Organization (WHO), which last week approved a new version of its International Classification of Diseases, a highly influential document that categorizes and assigns codes to medical conditions, and is used internationally to decide how doctors diagnose conditions and whether insurance companies will pay to treat them. The latest version, ICD-11, is the first to include a chapter on TCM — part of a warming to the practice under former director-general Margaret Chan, who led the WHO from 2006 to 2017.
TCM practitioners around the world have celebrated its incorporation into the document as crucial for the international spread of the system. So has China. On 26 May, a government newspaper called it a “major step for TCM’s internationalization” and a tremendous help in establishing TCM centres around the world.
From elsewhere, criticism has rained down on the WHO. The organization has defended its position. In a statement on 4 April, it insisted that the TCM chapter does not discuss particular remedies. Rather, it is meant to give doctors the chance to diagnose patients using both TCM and Western medicine — what it calls “optional dual coding”. These categories “do not refer to — or endorse — any form of treatment”, the statement says.
Traditional medicine should certainly not be dismissed: sometimes it is all that’s available in many parts of the world. Some life-saving therapies have come from natural products, and there are doubtless more to be found. Famously, the gold-standard malaria drug, artemisinin, was discovered in China — isolated from sweet wormwood (Artemisia annua), a herb used in TCM. It is also important to distinguish practices that do harm from those that might not work but are relatively benign, and those that might work but have not been tested rigorously.
Even so, the WHO chapter on traditional medicine is likely to backfire. It is broad-ranging and detailed, and risks legitimizing an unfounded underlying philosophy and some unscientific practice. It might contain only diagnostic criteria, but once diagnosed with a TCM-labelled condition, people will probably be prescribed TCM remedies. Whatever its aims, the WHO’s chapter is unlikely to do anything other than fuel the expanding sales of largely unproven treatments.
In defending the inclusion of TCM, the WHO referred to a mission to “share evidence-based information”. Everyone can agree on the desire to expand health care, and to do that in an evidence-based way. Collecting more evidence on TCM requires sustained and rigorous basic and clinical research to separate out harmful practices, those that have promise and those that have merely a placebo effect. The WHO’s association with medicines that are not properly tested and could even be harmful is unacceptable for the body that has the greatest responsibility and power to protect human health.

 Why Chinese medicine is heading for clinics around the world
Why Chinese medicine is heading for clinics around the world
 How China is redrawing the map of world science
How China is redrawing the map of world science
 Build a sustainable Belt and Road
Build a sustainable Belt and Road