- NEWS AND VIEWS
Antibodies pose a double threat to HIV
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 561, 468-470 (2018)
doi: https://doi.org/10.1038/d41586-018-06773-8
References
Paula, A. A., Falcão, M. C. N. & Pacheco, A. G. AIDS Res. Ther. 10, 32 (2013).
Mendoza, P. et al. Nature 561, 479–484 (2018).
Bar-On, Y. et al. Nature Med. https://doi.org/10.1038/s41591-018-0186-4 (2018).
Sengupta, S. & Siliciano R. F. Immunity 48, 872–895 (2018).
Boritz, E. A. et al. Cell 166, 1004–1015 (2016).
Pegu, A., Hessell, A. J., Mascola, J. R. & Haigwood, N. L. Immunol. Rev. 275, 296–312 (2017).
Caskey, M. et al. Nature 522, 487–491 (2015).
Bar, K. J. et al. N. Engl. J. Med. 375, 2037–2050 (2016).
Scheid, J. F. et al. Nature 535, 556–560 (2016).
Ledgerwood, J. E. et al. Clin. Exp. Immunol. 182, 289–301 (2015).
Mayer, K. H. et al. PLoS Med. 14, e1002435 (2017).
Scheid, J. F. et al. Science 333, 1633–1637 (2011).
Zhou, T. et al. Science 329, 811–817 (2010).
Rothenberger, M. K. et al. Proc. Natl Acad. Sci. USA 112, E1126–E1134 (2015).
Kearney, M. F. et al. PLoS Pathog. 10, e1004010 (2014).
Hessell, A. J. et al. Nature Med. 22, 362–368 (2016).
Liu, J. et al. Science 353, 1045–1049 (2016).
Shingai, M. et al. Nature 503, 277–280 (2013).
Barouch, D. H. et al. Nature 503, 224–228 (2013).
Nishimura, Y. et al. Nature 543, 559–563 (2017).

 Read the paper: Combination therapy with anti-HIV-1 antibodies maintains viral suppression
Read the paper: Combination therapy with anti-HIV-1 antibodies maintains viral suppression
 Read the paper: Limiting HIV-1 escape by combination broadly neutralizing antibody therapy in viremic individuals
Read the paper: Limiting HIV-1 escape by combination broadly neutralizing antibody therapy in viremic individuals
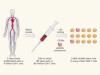 Finding latent needles in a haystack
Finding latent needles in a haystack
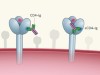 Tied down by its own receptor
Tied down by its own receptor