- NEWS AND VIEWS
Life of a liver awaiting transplantation
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 557, 40-41 (2018)
doi: https://doi.org/10.1038/d41586-018-04458-w
References
Nasralla, D. et al. Nature 557, 50–56 (2018).
Clark, E. A., Terasaki, P. I., Opelz, G. & Mickey, M. R. N. Engl. J. Med. 291, 1099–1102 (1974)
Eltzschig, H. K. & Eckle, T. Nature Med. 17, 1391–1401 (2011).
Verhoeven, C. J. et al. J. Hepatol. 61, 672–684 (2014).
Vogel, T. et al. PLoS ONE 12, e0188494 (2017).
Orman, E. S. et al. Liver Transplant. 19, 59–68 (2013).

 Read the paper: A randomized trial of normothermic preservation in liver transplantation
Read the paper: A randomized trial of normothermic preservation in liver transplantation
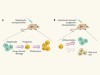 The versatile and plastic liver
The versatile and plastic liver
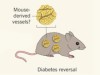 Interspecies pancreas transplants
Interspecies pancreas transplants