- OUTLOOK
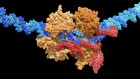
A CRISPR edit for heart disease
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature 555, S23-S25 (2018)
doi: https://doi.org/10.1038/d41586-018-02482-4
This article is part of Nature Outlook: The future of medicine, an editorially independent supplement produced with the financial support of third parties. About this content.
References
Abifadel, M. et al. Nature Genet. 34, 154–156 (2003).
Cohen, J. et al. Nature Genet. 37, 161–165 (2005).
Cohen, J. C., Boerwinkle, E., Mosley, T. H. Jr & Hobbs, H. H. N. Engl. J. Med. 354, 1264–1272 (2006).
Ding, Q. et al. Circ. Res. 115, 488–492 (2014).
Wang, X. et al. Arterioscler. Thromb. Vasc. Biol. 36, 783–786 (2016).
Pollin, T. I. et al. Science 322, 1702–1705 (2008).
Musunuru, K. et al. N. Engl. J. Med. 363, 2220–2227 (2010).
Stitziel, N. O. et al. J. Am. Coll. Cardiol. 16, 2054–2063 (2017).
Koschinsky, M. & Boffa, M. Expert Opin. Ther. Targets 18, 747–757 (2014).
Komor, A. C., Kim, Y. B., Packer, M. S., Zuris, J. A. & Liu, D. R. Nature 533, 420–424 (2016).
Gaudelli, N. M. et al. Nature 551, 464–471 (2017).
Chadwick, A. C., Wang, X. & Musunuru, K. Arterioscler. Thromb. Vasc. Biol. 37, 1741–1747 (2017).
Koornneef, A. et al. Mol. Ther. 19, 731–740 (2011).
Refaey, M. et al. Circ. Res. 121, 923–929 (2017).
Amoasii, L. et al. Sci. Transl. Med. 9, eaan8081 (2017).

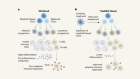
 Bringing down the cost of cancer treatment
Bringing down the cost of cancer treatment
 Infection forecasts powered by big data
Infection forecasts powered by big data
 Four stories of antibacterial breakthroughs
Four stories of antibacterial breakthroughs