- FROM THE ANALYST'S COUCH
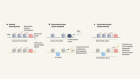
The multiple myeloma drug market
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Rent or buy this article
Prices vary by article type
from$1.95
to$39.95
Prices may be subject to local taxes which are calculated during checkout
Nature Reviews Drug Discovery 18, 579-580 (2019)
doi: https://doi.org/10.1038/d41573-019-00031-w

 Next generation antibody drugs: pursuit of the 'high-hanging fruit'
Next generation antibody drugs: pursuit of the 'high-hanging fruit'
 The market for chimeric antigen receptor T cell therapies
The market for chimeric antigen receptor T cell therapies