Abstract
Mesenchymal stem cells (MSCs), derived from adult tissues, are multipotent progenitor cells, which hold great promise for regenerative medicine. Recent studies have shown that MSCs are immunosuppressive in vivo and in vitro in both animals and humans. However, the mechanisms that govern these immune modulatory functions of MSCs remain largely elusive. Some studies with bulk populations of MSCs indicated that soluble factors such as PGE2 and TGFβ are important, while others support a role for cell-cell contact. In this study, we intended to clarify these issues by examining immunosuppressive effects of cloned MSCs. We derived MSC clones from mouse bone marrow and showed that the majority of these clones were able to differentiate into adipocytes and osteoblast-like cells. Importantly, cells from these clones exhibited strong inhibitory effects on TCR activation-induced T cell proliferation in vitro, and injection of a small number of these cells promoted the survival of allogeneic skin grafts in mice. Conditioned medium from MSC cultures showed some inhibitory effect on anti-CD3 induced lymphocyte proliferation independent of PGE2 and TGFβ. In comparison, direct co-culture of MSCs with stimulated lymphocytes resulted in much stronger immunosuppressive effect. Interestingly, the suppression was bi-directional, as MSC proliferation was also reduced in the presence of lymphocytes. Taking together, our findings with cloned MSCs demonstrate that these cells exert their immunosuppressive effects through both soluble factor(s) and cell-cell contact, and that lymphocytes and MSCs are mutually inhibitory on their respective proliferation.
Similar content being viewed by others
Introduction
Mesenchymal stem cells (MSCs) are multipotent progenitors existing in adult tissues 1, 2. They are able to differentiate into various lineages such as adipocytes, osteoblasts, and other cell types in vitro as well as in vivo. It has been shown in animal models that MSCs could specifically migrate to wound sites and help repair damaged tissues 3. Besides tissue repair and regeneration, it has been recently found that MSCs also possess an immunoregulatory property 4, 5, 6, 7, 8, 9. MSCs inhibit mitogen- or antigen- stimulated lymphocyte proliferation 10, 11. MSCs have also been successfully used for the treatment of some human cases of graft-versus-host-disease (GVHD) 12, 13, 14, though different results are reported by other studies 11.
Bone marrow stem cells can be classified as being either CD34+ or CD34−; CD34+ cells give rise to blood cells, while CD34− cells are more primitive and can differentiate into many cell types, including even CD34+ cells. Bone marrow MSCs were first characterized by Friedenstein and colleagues more than thirty years ago 15. In their undifferentiated state, MSCs are spindle-shaped and very much resemble fibroblasts. Although some biological characteristics of MSCs have been revealed, there are no cell surface markers that specifically and uniquely identify them. The cell surface molecules expressed by MSCs were first characterized by Majumdar et al. 16, who found that MSCs express integrin chains α1, 2, 3, 5, 6, v, and β1, 3, and 4; in addition ICAM-1, ICAM-2, VCAM-1, CD72, and LFA-3 were also detected. Interestingly, exposure of MSCs to IFNγ increased the expression of both MHC class I and class II molecules on the cell surface 17, 18. In general, in vitro expanded MSCs do not express the hematopoietic or endothelial surface markers CD31, CD34 or CD45, but do stain positively for CD29, CD44, CD73, CD105, CD106 and CD166 19, 20. Some studies have shown that they also express Flk-1 7. Bone marrow-derived MSCs can be cloned and expanded in vitro more than a million-fold and still retain the ability to differentiate into several mesenchymal lineages. Thus, MSCs possess great potential for clinical applications, especially in the utilization of their immunosuppressive properties.
Though the immunosuppressive property of mesenchymal stem cells is well established 4, 10, 21, 22, 23, 24, 25, 26, the mechanisms by which these cells exert their immunosuppressive function are still unclear. There have been various attempts to elucidate the mechanisms of MSC-mediated immunosuppression using the whole population of MSCs derived by various methods. These studies have yielded variable results and no consensus conclusion has been reached. Some studies have shown that soluble factors such as TGFβ 22 and PGE2 6 mediate the immunosuppressive effect of MSCs 27, 28, 29; while other researchers have argued that direct cell-cell contact is the major mechanism 30, 31, 32. In the present study, we generated MSC clones from mouse bone marrow and verified that the majority of these clones possessed differentiation potential. They potently inhibited lymphocyte proliferation in vitro and promoted the survival of allogeneic skin graft in mice. We found that, while soluble mediators from MSCs contribute to the inhibitory effect, cell-cell contact seems to play a more important role in MSC-mediated immune inhibitory function. We also found that MSCs exposed to stimulated lymphocytes had dramatically reduced proliferation and enhanced immunosuppressive capacity.
Materials and Methods
Reagents, antibodies and mice
The following reagents were purchased from Sigma-Aldrich (St. Louis, MO): RPMI-1640 medium, α-MEM medium, lipopolysachride (LPS), phorbol myristate acetate (PMA), ionomycin and glutamine. Heat-inactivated fetal bovine serum (FBS) and phytohemagglutinin (PHA) were purchased from Life Technologies (Grand Island, NY). Fluorescein-conjugated monoclonal antibodies against CD11b, CD13, CD34, MHC class I, MHC class II, Sca-1, and respective isotype controls were from BD/PharMingen (San Jose, CA). Mice of strains C57BL/6 (H-2b) and BALB/c (H-2d) were obtained from Jackson Laboratories (Bar Harbor, ME). Mice were housed in an American Association for Accreditation of Laboratory Animal Care-accredited animal facility at Robert Wood Johnson Medical School. Animal protocols were approved by the Institutional Animal Care and Use Committee.
MSC culture
Bone marrow from 6-10 week old C57BL/6 mice was flushed out of tibia and femur bones with PBS. Cells were filtered through 40 μm nylon mesh, and plated in 25 cm2 tissue culture dishes in α-MEM medium supplemented with 10% FBS, 2 mM glutamine, 100 U/mL penicillin, and 100 μg/mL streptomycin (Invitrogen, Carlsbad, CA). All non-adherent cells were removed after 24 h. The medium was replenished every three days. MSC clones were generated by limiting dilution. Briefly, when cells were confluent, they were harvested, diluted and seeded in 96-well plates by limited dilution. Medium was changed every 4-5 d until clones grew out. Only those clones contained individually in each well were picked and expanded. Most tests were carried out using at least 3 clones with similar results. Only data from clone #12 were shown. Cells were always used before the 20th passage.
Differentiation of MSCs
MSCs were made to differentiate into adipocytes in vitro by treatment with 0.5 mM isobutylmethylxanthin, 60 μM indomethacin, 10 nM dexamethasone and 10 μg/ml insulin. MSCs were thus grown in 24-well plates for 10 d. The presence of adipocytes was verified by staining for triglycerides with oil red O (Sigma-Aldrich), an indicator of intracellular lipid accumulation, according to established protocols 33. MSCs were also cultured with osteoinductive medium consisting of DMEM supplemented with 10% FBS, β-mercaptoethanol, 10 nM dexamethasone, 100 μM L-ascorbic acids, and 10 mM β-glycerophosphate. These cultures were maintained for 20 d, and then stained with Alizarin Red S to identify calcium deposition, an indicative property of osteoblasts.
Immunofluorescence and Flow cytometry
Surface markers were stained by incubating cells with each corresponding antibody for 30 min in dark according to the product instructions. Cells were then washed twice with PBS containing 1% FBS and resuspended in 0.5 ml PBS. Flow cytometry was performed on a FACScan flow cytometer (BD Immunocytometry, San Jose, CA) using Cellquest software for data acquisition and analysis.
Proliferation assay
For co-culture experiments, cells from MSC clones were plated in 96-well plates at 1 × 104 cells per well in 100 μl of complete medium consisting of RPMI-1640 supplemented with 10% FBS, 2 mM glutamine, 2-ME, 100 U/mL penicillin, and 100 μg/mL streptomycin. Splenocytes (3 × 105/well) isolated from C57BL/6 or BALB/c mice were then added to each well in 100 μl of complete medium, resulting in a MSC to splenocyte ratio of 1:30, unless specified otherwise. Anti-CD3 antibody was added at 1μg/ml. After 48 h, 3H-thymidine (0.5 μCi) was added to each well and incubation was continued for another 6 h. Cells were harvested and 3H-thymidine incorporation was counted using a Wallac Microbeta scintillation counter (Perkin-Elmer, Wellesley, MA).
Skin transplantation
Full-thickness skin grafts from BALB/c mice were transplanted onto the backs of 6- to 8-week-old C57BL/6 male mice, with five mice per treatment group, as follows. One day before skin transplantation, 3 × 106 MSCs were injected via the tail vein into the intended recipient C57BL/6 mice. For the graft, skin was removed from the tail of euthanized BALB/c donors. Prepared skin was placed on sterile filter paper moistened with Hanks' balanced salt solution (HBSS) buffered with HEPES (pH 7.4; Sigma Chemical Co., St. Louis, MO) and maintained at room temperature until use (within 2 h). The dorsal surface of the anesthetized recipient mouse was shaved and sterilized with 70% ethanol. A graft bed was prepared with fine scissors by removing an area of epidermis and dermis down to the level of the intrinsic muscle. Grafts of size 1.0–1.5 cm square were fitted to the prepared bed without suturing and then covered with petroleum jelly-impregnated gauze and an adhesive plastic bandage. After 7 d, the bandage was removed. Skin graft survival was assessed daily by visual and tactile examination. Rejection was defined as necrosis of the entire epidermal surface of the graft. The skin transplantation protocol was approved by the IACUC of Robert Wood Johnson Medical School.
Results
Bone marrow derived MSCs are strongly immunosuppressive in vitro
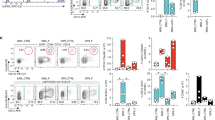
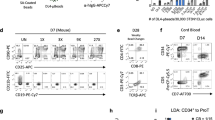
MSCs were derived from mouse bone marrow according to an established protocol 7, 25. These cells exhibited spindle-shaped morphology and continuous proliferation. MSCs from the 8th passage were analyzed for expression of cell surface molecules by flow cytometry. As reported in other studies, these cells were found to express MHC class Ia (Kb and Db) and Sca-1, but were negative for MHC class II (I-A), CD11b, CD31 and CD34 (Figure 1A). They were capable of differentiating into adipocytes and osteoblasts when cultured under appropriate conditions (Figure 1B). Thus, these cells possessed the typical properties of MSCs. To better characterize these cells, we derived clones from first-passage cells, and performed the same analysis on each clone. Of 100 clones examined, most had identical properties, except for a small number of them that expressed CD11b, CD45 or CD34 (data not shown). When cultured under conditions permissive for differentiation, the majority of these clones underwent differentiation, with almost 100% of cells apparently acquiring the characteristics of adipocytes or osteoblasts. Due to their uniformity, cloned MSCs were used for most of the subsequent functional assays.
Cell surface markers of MSCs and differentiation of MSCs into adipocytes and osteoblasts. (A) At passage 8, cells were harvested and stained for the indicated surface markers as described in Materials and Methods. (B) MSCs at passage #8 were grown under the respective conditions for differentiation into adipocytes or osteoblasts. Cells were cultured and stained as described in Methods and Materials. Data are representative of three separate experiments.
To examine their immunoregulatory capacity, MSCs from our cloned lines were added at various ratios to freshly-isolated splenocytes activated with anti-CD3 antibody. We found that lymphocyte proliferation was strongly inhibited by the presence of MSCs, and the effect was correlated with the number of added MSCs (Figure 2A). Significant inhibition of activation-induced lymphocyte proliferation was observed even at a 1:60 ratio of MSCs to splenocytes.
MSCs inhibit lymphocyte proliferation in vitro. (A) Various numbers of MSCs were added to splenocytes stimulated with anti-CD3 antibody (1 μg/ml) and splenocyte proliferation was measured by 3H-thymidine incorporation. The MSC to lymphocyte ratio is indicated. (B) MSCs were added to immunomagnetically-purified CD4+ T cells (MACs beads, Miltenyi) stimulated with PHA (5 μg/ml), or (C) immunomagnetically-purified CD19+ B cells (MACs beads, Miltenyi) stimulated with LPS (5 μg/ml), at a 1:30 ratio of MSCs to responder cells. Values represent means ± SD. Similar results were obtained from more than five experiments.
To examine the effect of MSCs on various lymphocyte subpopulations, we added MSCs to cultures of purified PHA-stimulated CD4+ T lymphocyte and LPS-stimulated B lymphocytes. We found that MSCs dramatically inhibited the proliferation of both types of lymphocytes (Figure 2B and 2C). Therefore, the effect of MSCs on lymphocyte proliferation is not limited to a specific subset.
MSCs inhibit the rejection of allogeneic skin grafts
While MSCs inhibit lymphocyte proliferation in vitro, they have also been shown by some studies to suppress immune response in vivo 4, 10, 34. To confirm that the cloned MSCs generated in our study maintain this capacity, we used the mouse model of allogeneic skin transplantation. Recipient BALB/c mice were injected i.v. with 3 × 106MSCs, and skin transplantation from C57Bl/6 donors was carried out the next day. As shown in Figure 3, transfusion of MSCs greatly improved the survival of the skin grafts, from a mean survival time of 10 d (control group) to 27 d in the MSC-treated group.
MSCs prolong the survival of allogeneic skin grafts in mice. One day before the transplantation, 3×106 MSCs were injected into intended recipient C57Bl/6 mice. Allogeneic skin graft from a BALB/c mouse was made onto the back of each recipient. Rejection was evaluated as described in Materials and Methods.
The immunosuppressive property of MSCs is not MHC restricted
T cells responses are strictly affected by the MHC haplotypes of antigen-presenting cells (APC). Since MSCs can also suppress LPS-induced B cell proliferation, however, it is unlikely that the effect of MSCs on T cells is restricted by the MHC haplotype. To verify that MHC haplotypes are not important in the immunosuppressive property of MSCs, autologous and allogeneic MSCs were added to the cultures. We found that the origin of the MSCs made no difference; both autologous and allogeneic MSCs inhibited splenocyte proliferation to a similar extent (Figure 4). We similarly found that the age and gender of the mouse from which MSCs were derived had no bearing on their immunosuppressive functionality (data not shown).
The immunosuppressive function of MSCs is not MHC-restricted. Allogeneic (BALB/c) or syngeneic (C57Bl/6) MSCs were co-cultured with splenocytes from C57Bl/6 mice stimulated with anti-CD3 antibody for 48 h, and splenocyte proliferation was measured after a 6 h pulse with 3H-thymidine. Values represent means ± SD. Data are representative of four experiments.
MSCs incompletely inhibit PMA and ionomycin induced lymphocyte proliferation
Lymphocyte proliferation induced by either antigen presentation or antibody against the TCR complex results from signal transduction triggered at the antigen receptor, from which a cascade of signaling process leads to the activation of protein kinase C (PKC) and the calcium/calcineurin pathway. To determine the mechanism by which MSCs exert their immunosuppressive function, we examined which step of the signaling pathway is affected by MSCs, i.e., surface complex formation or intracellular signaling processes. We used stimulation with PMA and ionomycin to mimic the PKC and calcium signals triggered by cell surface TCR activation. To our surprise, we found that lymphocyte proliferation induced by PMA plus ionomycin was only partially inhibited by co-culturing with MSCs, while inhibition of anti-CD3 antibody-induced proliferation was nearly 100% with the same number of MSCs (Figure 5A). It is possible that PMA/ionomycin may alter the ability of MSCs to exert their inhibitory effects on lymphocytes. To rule out this possibility, MSCs were pre-treated with PMA and ionomycin for 2 d, and tested for inhibition on anti-CD3-induced T cell proliferation immediately after wash. As shown in Figure 5B, pretreatment with PMA/ionomycin did not change the inhibitory function of MSCs. Therefore, it is likely that the inhibitory function of MSCs results at least in part from an interference with the initiation of cell surface signaling.
Lymphocyte proliferation induced by PMA + ionomycin was less effectively inhibited by MSCs. (A) Splenocytes were stimulated with PMA (50 ng/ml) and ionomycin (1 μM) with or without the presence of MSCs, and their proliferation was measured after 48 h. (B) Splenocytes were stimulated with anti-CD3 in the presence of MSCs or MSCs pretreated with PMA (50 ng/ml) and ionomycin (1 μM) for 2 d. P/I = PMA/ionomycin. Values represent means± SD. Data are representative of three separate experiments.
Both soluble factor(s) and cell-cell contact are important in MSC-mediated immunosuppression
Several studies have investigated the mechanisms by which MSCs inhibit immune responses, yet it is unclear how MSCs exert their immunosuppressive function. Some studies have suggested that soluble molecules such as IL-10, TGFβ and PGE2 are important in mediating the inhibitory effects of MSCs; while others have shown that cell-cell contact is critical. To determine whether soluble factors released by MSCs are sufficient to achieve immunosuppression, we supplemented splenocyte cultures with conditioned medium derived from MSCs cultured with or without activated lymphocytes. We found that conditioned medium from cultures of MSCs alone caused partial inhibition of lymphocyte proliferation (Figure 6A). We next checked the potential involvement of factors previously reported to contribute to the inhibitory function of MSCs, by culturing splenocytes with MSCs and stimulating the splenocytes with anti-CD3 in the presence of monoclonal antibodies against IL10 or TGFβ, or indomethacin which blocks prostaglandin (PG) E2 production, at concentrations known to be effective. We found that these reagents either alone or in combinations had no effect on resultant lymphocyte proliferation (Figure 6B), indicating that IL-10, TGFβ, and PGE2 are not critically involved in the immunosuppressive function of MSCs.
Soluble factor(s) are involved in the immunosuppressive function of MSCs. (A) C57Bl/6 splenocytes were stimulated with anti-CD3 antibody and cultured in medium supplemented with 50% conditioned medium from MSC cultures. Super(SPL): culture supernatant from activated splenocytes (splenocytes were stimulated with anti-CD3 in 25 cm2 flasks at 2×106 cells/ml for 2 d, and then the culture supernatant was collected); Super(MSC): culture supernatant from MSCs (MSCs were cultured in 25 cm2 flasks at 1×105 cells/ml for 2 d, and then culture supernatant was harvested); Super(MSC/SPL): culture supernatant from co-culture of MSCs and activated splenocytes (MSCs were cultured with anti-CD3-activated splenocytes in 25 cm2 flasks for 2 d, and then culture supernatant was collected). (B) C57Bl/6 splenocytes were cultured with MSCs and stimulated with anti-CD3 in the presence of indomethacin (10 μg/ml), or monoclonal antibodies (50 μg/ml) against IL-10 and TGFβ, or their combinations. Indo = Indomethacin. Proliferation was measured after 48 h. The incorporation of 3H-thymidine is shown relative to that of the control. Values are the means±SD from three independent experiments.
The most effective inhibition, however, was achieved when MSCs were added directly to the activated lymphocyte cultures (Figure 7A). To examine the role of cell-cell contact, MSCs were seeded into wells of a 24-well plate in a 50 μl volume, such that only about half of the well was covered, while the other half remained dry. After incubation overnight to allow the MSCs to adhere, the wells were washed twice and fresh medium was added. Splenocytes were then added, followed by the anti-CD3 antibody. As seen in the micrographs of Figure 7B, splenocytes grew well in the half-well that is absent of MSCs, while there was no growth on the side containing MSCs. Since this system allows sharing of the medium in the whole well while isolating the cell contact aspect, it directly demonstrates that cell-cell contact between lymphocytes and MSCs is much more effective than soluble factor(s) alone in the induction of immunosuppression.
Cell-cell contact is important in the immunosuppressive function of MSCs. (A) C57Bl/6 splenocytes were stimulated with anti-CD3 antibody in the presence of MSCs (1:30 ratio of MSC to splenocytes) or 50% MSC-conditioned medium. Cultures were photographed after 48 h under phase contrast microscopy (100×). (B) Wells of a 48-well culture plate were seeded on only one side by adding 5 ×103 MSCs in 50 μl. After overnight incubation to allow the cells to adhere, the wells were washed twice with complete medium and splenocytes were added and stimulated with anti-CD3 antibody. Cell aggregation at 48 h was observed using a phase contrast microscope. Data are representative of three separate experiments.
Immunosuppression by MSCs is enhanced by pre-exposure to stimulated lymphocytes
As we have shown, lymphocyte proliferation is more effectively inhibited by directly co-culturing with MSCs, compared to that with conditioned medium from MSCs culture (Figure 7A). We postulate that the interaction between lymphocytes and MSCs might affect the immunosuppressive ability of MSCs. To test this directly, we co-cultured MSCs with TCR-stimulated splenocytes for two days. We then harvested these pre-treated MSCs and, in turn, added them to indicator cultures of fresh splenocytes, and measured their effect on lymphocyte proliferation stimulated by anti-CD3. MSCs pretreated by exposure to activated lymphocytes were more potent inhibitors of lymphocyte proliferation than untreated MSCs (Figure 8). Interestingly, we found that activated splenocytes not only enhanced the immunosuppressive capacity of MSCs, but also inhibited their growth (Figure 9). Therefore, in a co-culture of MSCs and activated splenocytes, there is bidirectional inhibition of cell proliferation.
Pre-culture of MSCs with lymphocytes enhances their immunosuppressive capacity. Splenocytes were activated by anti-CD3 (1 μg/ml) for two days. After that, activated splenocyctes were harvested and co-cultured with MSCs for 1 day at a 1:30 ratio (MSCs: splenocytes). MSCs were then washed twice to remove splenocytes, and the remaining adherent MSCs were harvested. These pre-treated MSCs were in turn cultured with fresh splenocytes (at a 1:30 ratio); and the fresh splenocytes were stimulated with anti-CD3. Proliferation was determined after 48 h. Control indicates MSCs that did not receive pretreatment. Values represent means ± SD. Data are representative of two separate experiments.
Activated lymphocytes inhibit the growth of MSCs. Splenocytes were activated by anti-CD3 (1 μg/ml) for two days. After that, activated splenocyctes were harvested. MSCs were co-cultured with these activated splenocytes in 96-well plates at the indicated ratios of MSCs to splenocytes for 72 h. Cultures were then washed 2 times to remove splenocytes, and the left cells were cultured with medium containing 3H thymidine for 6 h. Values represent means ±SD. Data are representative of four separate experiments.
Discussion
Stem cells have two distinct characteristics that distinguish them from other cell types. Firstly, they are unspecialized and can renew themselves for long periods without significant changes in their general properties. Secondly, under certain physiologic or experimental conditions, stem cells can be induced to differentiate into various specialized cell types. The promise of embryonic stem (ES) cells in regenerative medicine is very exciting; however, there has been a surprising lack of attention to the possible immunological conflict between the graft recipient and the tissues regenerated from stem cells, especially those of embryonic origin, which are almost always allogeneic in nature 35. There is clear evidence that immunological rejection of transplanted fetal and ES cell-derived tissues occurs very frequently 6, 36. On the other hand, unlike ES cells, MSCs are highly immunosuppressive. In various systems, though not all, it has been shown that MSCs can suppress proliferation and cytokine production by T cells stimulated with mitogens or properly presented antigens.
Similar to previous reports that utilized bulk MSCs 4, 6, 11, 22, 23, 24, 26, 32, 37, 38, 39, 40, we show here that cultured clones of MSCs are highly immunosuppressive both in vitro and in vivo. It is surprising that a single injection of a few million MSCs was able to greatly extend the survival time of transplanted skin. In previous reports, it has been shown that MSCs inhibit the mixed lymphocyte reaction (MLR) and proliferation induced by mitogen or specific antigen. In the current study, we found that MSCs inhibit the proliferation of splenocytes stimulated with PHA or anti-CD3 antibody, and of purified CD19+ cells stimulated with LPS. It is interesting that MSC inhibition of lymphocyte proliferation induced by PMA + Ionomycin was incomplete. Though we do not know the precise mechanism, it is possible that the effect of MSCs on lymphocyte proliferation is exerted prior to PKC activation and Ca2+ mobilization. Nevertheless, elucidation of the mechanisms that underlie this difference will provide useful information.
While a number of studies have examined the mechanisms of immunosuppression by MSCs, it remains unclear how these cells inhibit immune responses. Some studies have shown that soluble factors secreted by MSCs are the most critical mediators of their inhibitory function. Although it has been proposed that TGFβ 22 and PGE2 6 play important roles, conflicting data exist 23. In our study, we found no connection between these factors and immunosuppression by MSCs, corroborating the results of other studies that excluded these factors by using blocking antibodies. Furthermore, we have found insignificant levels of inhibitory cytokines such as TGFβ and IL10 in MSC culture supernatants (data not shown). Thus, it appears that the critical soluble factors involved in the immunosuppressive function of MSCs remain to be defined; it would be of great value to identify the responsible molecules.
In contrast to some studies that support a central role for soluble factors in the immunosuppression by MSCs, others suggest that cell-cell contact is more important 32, 41. In our study, we showed that while soluble factors do contribute, cell-cell contact is critical in the inhibitory function of MSC. We found that: 1) MSC co-culture was more effective than MSC-conditioned medium in inhibiting lymphocyte proliferation, and, 2), half-well co-culture experiments showed that only lymphocytes in the MSC-seeded half of the well are completely inhibited, while some proliferation still occurs on the side without MSCs. Thus, close proximity to MSCs was important in suppressing T cell responsiveness, indicating that direct contact between lymphocytes and MSCs is probably more important than soluble mediators in the immunosuppressive function of MSCs.
We also found that when MSCs are cultured with anti-CD3 antibody-activated lymphocytes, there is a bidirectional inhibition of growth: not only do MSCs affect lymphocytes, but splenocytes also influence MSCs. Interestingly, activated lymphocytes inhibit MSC proliferation, while at the same time enhancing their immunosuppressive capacity. We found that: 1) Conditioned medium from co-culture of MSCs + activated lymphocytes more potently inhibits lymphocyte proliferation than that from MSCs cultured alone; 2) MSCs pre-cultured with activated lymphocytes were more effective at inhibiting lymphocyte proliferation in subsequent indicator co-cultures. These results suggest that during the interaction between lymphocytes and MSCs, lymphocytes influence the function potential of MSCs. Since the interaction between lymphocytes and MSCs can enhance subsequent immunosuppression by MSCs, we believe that further understanding of the effect of splenocytes on MSCs might also help us understand the immunoregulatory function of MSCs.
In conclusion, our findings indicate that MSCs are strongly immunosuppressive both in vivo and in vitro, and this function is relatively non-specific. Both cell-cell contact and soluble factors are important. Lymphocytes and MSCs mutually affect each other, and the interaction between them simultaneously inhibits the growth of MSCs and enhances their immunosuppressive ability. Further elucidation of the regulation of the immunosuppressive capacity of MSCs will allow for their effective clinical use in the treatment of various autoimmune disorders, allergic reactions, and atherosclerosis, as well as in transplantation.
References
Herzog EL, Chai L, Krause DS . Plasticity of marrow-derived stem cells. Blood 2003; 102:3483–3493.
Prockop DJ, Gregory CA, Spees JL . One strategy for cell and gene therapy: harnessing the power of adult stem cells to repair tissues. Proc Natl Acad Sci USA 2003; 100 Suppl 1:11917–11923.
McFarlin K, Gao X, Liu YB, et al. Bone marrow-derived mesenchymal stromal cells accelerate wound healing in the rat. Wound Repair Regen 2006; 14:471–478.
Bartholomew A, Sturgeon C, Siatskas M, et al. Mesenchymal stem cells suppress lymphocyte proliferation in vitro and prolong skin graft survival in vivo. Exp Hematol 2002; 30:42–48.
Djouad F, Plence P, Bony C, et al. Immunosuppressive effect of mesenchymal stem cells favors tumor growth in allogeneic animals. Blood 2003; 102:3837–3844.
Aggarwal S, Pittenger MF . Human mesenchymal stem cells modulate allogeneic immune cell responses. Blood 2005; 105:1815–1822.
Deng W, Han Q, Liao L, et al. Allogeneic bone marrow-derived flk-1+Sca-1- mesenchymal stem cells leads to stable mixed chimerism and donor-specific tolerance. Exp Hematol 2004; 32:861–867.
Uccelli A, Zappia E, Benvenuto F, Frassoni F, Mancardi G . Stem cells in inflammatory demyelinating disorders: a dual role for immunosuppression and neuroprotection. Expert Opin Biol Ther 2006; 6:17–22.
Rasmusson I . Immune modulation by mesenchymal stem cells. Exp Cell Res 2006; 312:2169–2179.
Zappia E, Casazza S, Pedemonte E, et al. Mesenchymal stem cells ameliorate experimental autoimmune encephalomyelitis inducing T-cell anergy. Blood 2005; 106:1755–1761.
Sudres M, Norol F, Trenado A, et al. Bone marrow mesenchymal stem cells suppress lymphocyte proliferation in vitro but fail to prevent graft-versus-host disease in mice. J Immunol 2006; 176:7761–7767.
Le Blanc K, Rasmusson I, Sundberg B, et al. Treatment of severe acute graft-versus-host disease with third party haploidentical mesenchymal stem cells. Lancet 2004; 363:1439–1441.
Liu LH, Sun QY, Hu KX, et al. Establishment of a rhesus haploidentical hematopoietic stem cell and mesenchymal stem cell transplantation model by nonmyeloablative conditioning. Zhonghua Xue Ye Xue Za Zhi 2005; 26:385–388.
Ringden O, Uzunel M, Rasmusson I, et al. Mesenchymal stem cells for treatment of therapy-resistant graft-versus-host disease. Transplantation 2006; 81:1390–1397.
Friedenstein AJ, Gorskaja JF, Kulagina NN . Fibroblast precursors in normal and irradiated mouse hematopoietic organs. Exp Hematol 1976; 4:267–274.
Majumdar MK, Keane-Moore M, Buyaner D, et al. Characterization and functionality of cell surface molecules on human mesenchymal stem cells. J Biomed Sci 2003; 10:228–241.
Stagg J, Pommey S, Eliopoulos N, Galipeau J . Interferon-gamma-stimulated marrow stromal cells: a new type of nonhematopoietic antigen-presenting cell. Blood 2006; 107:2570–2577.
Chan JL, Tang KC, Patel AP, et al. Antigen-presenting property of mesenchymal stem cells occurs during a narrow window at low levels of interferon-gamma. Blood 2006; 107:4817–4824.
Vodyanik MA, Thomson JA, Slukvin II . Leukosialin (CD43) defines hematopoietic progenitors in human embryonic stem cell differentiation cultures. Blood 2006; 108:2095–2105.
Zheng B, Cao B, Li G, Huard J . Mouse adipose-derived stem cells undergo multilineage differentiation in vitro but primarily osteogenic and chondrogenic differentiation in vivo. Tissue Eng 2006; 12:1891–1901.
Le Blanc K, Ringden O . Immunobiology of human mesenchymal stem cells and future use in hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2005; 11:321–334.
Di Nicola M, Carlo-Stella C, Magni M, et al. Human bone marrow stromal cells suppress T-lymphocyte proliferation induced by cellular or nonspecific mitogenic stimuli. Blood 2002; 99:3838–3843.
Tse WT, Pendleton JD, Beyer WM, Egalka MC, Guinan EC . Suppression of allogeneic T-cell proliferation by human marrow stromal cells: implications in transplantation. Transplantation 2003; 75:389–397.
Krampera M, Glennie S, Dyson J, Scott D, Laylor R, Simpson E, Dazzi F . Bone marrow mesenchymal stem cells inhibit the response of naive and memory antigen-specific T cells to their cognate peptide. Blood 2003; 101:3722–3729.
Le Blanc K, Tammik L, Sundberg B, Haynesworth SE, Ringden O . Mesenchymal stem cells inhibit and stimulate mixed lymphocyte cultures and mitogenic responses independently of the major histocompatibility complex. Scand J Immunol 2003; 57:11–20.
Glennie S, Soeiro I, Dyson PJ, Lam EW, Dazzi F . Bone marrow mesenchymal stem cells induce division arrest anergy of activated T cells. Blood 2005; 105:2821–2827.
Rasmusson I, Ringden O, Sundberg B, Le Blanc K . Mesenchymal stem cells inhibit lymphocyte proliferation by mitogens and alloantigens by different mechanisms. Exp Cell Res 2005; 305:33–41.
Liu H, Kemeny DM, Heng BC, Ouyang HW, Melendez AJ, Cao T . The immunogenicity and immunomodulatory function of osteogenic cells differentiated from mesenchymal stem cells. J Immunol 2006; 176:2864–2871.
Mais A, Klein T, Ullrich V, Schudt C, Lauer G . Prostanoid pattern and iNOS expression during chondrogenic differentiation of human mesenchymal stem cells. J Cell Biochem 2006; 98:798–809.
Sotiropoulou PA, Perez SA, Gritzapis AD, Baxevanis CN, Papamichail M . Interactions between human mesenchymal stem cells and natural killer cells. Stem Cells 2006; 24:74–85.
Jiang XX, Zhang Y, Liu B, Zhang SX, Wu Y, Yu XD, Mao N . Human mesenchymal stem cells inhibit differentiation and function of monocyte-derived dendritic cells. Blood 2005; 105:4120–4126.
Potian JA, Aviv H, Ponzio NM, Harrison JS, Rameshwar P . Veto-like activity of mesenchymal stem cells: functional discrimination between cellular responses to alloantigens and recall antigens. J Immunol 2003; 171:3426–3434.
Ogawa R, Mizuno H, Watanabe A, Migita M, Hyakusoku H, Shimada T . Adipogenic differentiation by adipose-derived stem cells harvested from GFP transgenic mice-including relationship of sex differences. Biochem Biophys Res Commun 2004; 319:511–517.
Maitra B, Szekely E, Gjini K, et al. Human mesenchymal stem cells support unrelated donor hematopoietic stem cells and suppress T-cell activation. Bone Marrow Transplant 2004; 33:597–604.
Bradley JA, Bolton EM, Pedersen RA . Stem cell medicine encounters the immune system. Nat Rev Immunol 2002; 2:859–871.
Drukker M, Benvenisty N . The immunogenicity of human embryonic stem-derived cells. Trends Biotechnol 2004; 22:136–141.
Rasmusson I, Ringden O, Sundberg B, Le Blanc K . Mesenchymal stem cells inhibit the formation of cytotoxic T lymphocytes, but not activated cytotoxic T lymphocytes or natural killer cells. Transplantation 2003; 76:1208–1213.
Augello A, Tasso R, Negrini SM, Amateis A, Indiveri F, Cancedda R, Pennesi G . Bone marrow mesenchymal progenitor cells inhibit lymphocyte proliferation by activation of the programmed death 1 pathway. Eur J Immunol 2005; 35:1482–1490.
Meisel R, Zibert A, Laryea M, Gobel U, Daubener W, Dilloo D . Human bone marrow stromal cells inhibit allogeneic T-cell responses by indoleamine 2,3-dioxygenase-mediated tryptophan degradation. Blood 2004; 103:4619–4621.
Groh ME, Maitra B, Szekely E, Koc ON . Human mesenchymal stem cells require monocyte-mediated activation to suppress alloreactive T cells. Exp Hematol 2005; 33:928–934.
Beyth S, Borovsky Z, Mevorach D, et al. Human mesenchymal stem cells alter antigen-presenting cell maturation and induce T-cell unresponsiveness. Blood 2005; 105:2214–2219.
Acknowledgements
The authors wish to acknowledge Arthur I. Roberts for his critique of the manuscript. This work was supported in part by New Jersey Science Commission (NJSTC-2042-014-84), USPHS grants (AI43384, AI057596 and AI50222), and the National Space Biomedical Research Institute (IIH00405), which is supported by the National Aeronautics and Space Administration through the Cooperative Agreement NCC 9-58
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xu, G., Zhang, L., Ren, G. et al. Immunosuppressive properties of cloned bone marrow mesenchymal stem cells. Cell Res 17, 240–248 (2007). https://doi.org/10.1038/cr.2007.4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cr.2007.4
Keywords
This article is cited by
-
The secretion profile of mesenchymal stem cells and potential applications in treating human diseases
Signal Transduction and Targeted Therapy (2022)
-
Phosphatase SHP1 impedes mesenchymal stromal cell immunosuppressive capacity modulated by JAK1/STAT3 and P38 signals
Cell & Bioscience (2020)
-
Single-cell RNA sequencing of equine mesenchymal stromal cells from primary donor-matched tissue sources reveals functional heterogeneity in immune modulation and cell motility
Stem Cell Research & Therapy (2020)
-
Co-encapsulation and co-transplantation of mesenchymal stem cells reduces pericapsular fibrosis and improves encapsulated islet survival and function when allografted
Scientific Reports (2017)
-
Mesenchymal Stromal Cell Therapy in MDR/XDR Tuberculosis: A Concise Review
Archivum Immunologiae et Therapiae Experimentalis (2015)