Abstract
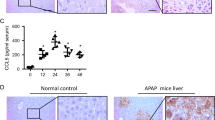
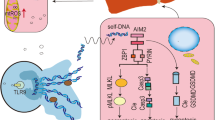
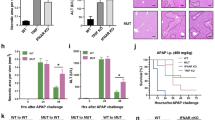
The metabolic intermediate of acetaminophen (APAP) can cause severe hepatocyte necrosis, which triggers aberrant immune activation of liver non-parenchymal cells (NPC). Overzealous hepatic inflammation determines the morbidity and mortality of APAP-induced liver injury (AILI). Interleukin-1 receptor (IL-1R) signaling has been shown to play a critical role in various inflammatory conditions, but its precise role and underlying mechanism in AILI remain debatable. Herein, we show that NLRP3 inflammasome activation of IL-1β is dispensable to AILI, whereas IL-1α, the other ligand of IL-1R1, accounts for hepatic injury by a lethal dose of APAP. Furthermore, Kupffer cells function as a major source of activated IL-1α in the liver, which is activated by damaged hepatocytes through TLR4/MyD88 signaling. Finally, IL-1α is able to chemoattract and activate CD11b+Gr-1+ myeloid cells, mostly neutrophils and inflammatory monocytes, to amplify deteriorated inflammation in the lesion. Therefore, this work identifies that MyD88-dependent activation of IL-1α in Kupffer cells plays a central role in the immunopathogenesis of AILI and implicates that IL-1α is a promising therapeutic target for AILI treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Garlanda C, Dinarello CA, Mantovani A. The interleukin-1 family: back to the future. Immunity 2013; 39: 1003–1018.
Dinarello CA. Immunological and inflammatory functions of the interleukin-1 family. Ann Rev Immunol 2009; 27: 519–550.
Werman A, Werman-Venkert R, White R, Lee JK, Werman B, Krelin Y et al. The precursor form of IL-1alpha is an intracrine proinflammatory activator of transcription. Proc Natl Acad Sci USA 2004; 101: 2434–2439.
Chen CJ, Kono H, Golenbock D, Reed G, Akira S, Rock KL. Identification of a key pathway required for the sterile inflammatory response triggered by dying cells. Nat Med 2007; 13: 851–856.
Afonina IS, Tynan GA, Logue SE, Cullen SP, Bots M, Luthi AU et al. Granzyme B-dependent proteolysis acts as a switch to enhance the proinflammatory activity of IL-1alpha. Mol Cell 2011; 44: 265–278.
Gross O, Yazdi AS, Thomas CJ, Masin M, Heinz LX, Guarda G et al. Inflammasome activators induce interleukin-1alpha secretion via distinct pathways with differential requirement for the protease function of caspase-1. Immunity 2012; 36: 388–400.
Schroder K, Tschopp J. The inflammasomes. Cell 2010; 140: 821–832.
Dinarello CA. Interleukin-1 in the pathogenesis and treatment of inflammatory diseases. Blood 2011; 117: 3720–3732.
Kayagaki N, Warming S, Lamkanfi M, Vande Walle L, Louie S, Dong J et al. Non-canonical inflammasome activation targets caspase-11. Nature 2011; 479: 117–121.
Freigang S, Ampenberger F, Weiss A, Kanneganti TD, Iwakura Y, Hersberger M et al. Fatty acid-induced mitochondrial uncoupling elicits inflammasome-independent IL-1alpha and sterile vascular inflammation in atherosclerosis. Nat Immunol 2013; 14: 1045–1053.
Tannahill GM, Curtis AM, Adamik J, Palsson-McDermott EM, McGettrick AF, Goel G et al. Succinate is an inflammatory signal that induces IL-1beta through HIF-1alpha. Nature 2013; 496: 238–242.
Chen GY, Nunez G. Sterile inflammation: sensing and reacting to damage. Nat Rev Immunol 2010; 10: 826–837.
James LP, Mayeux PR, Hinson JA. Acetaminophen-induced hepatotoxicity. Drug Metab Dispos: Biol Fate Chem 2003; 31: 1499–1506.
Maher JJ. DAMPs ramp up drug toxicity. J Clin Investig 2009; 119: 246–249.
Williams CD, Farhood A, Jaeschke H. Role of caspase-1 and interleukin-1beta in acetaminophen-induced hepatic inflammation and liver injury. Toxicol Appl Pharmacol 2010; 247: 169–178.
Williams CD, Antoine DJ, Shaw PJ, Benson C, Farhood A, Williams DP et al. Role of the Nalp3 inflammasome in acetaminophen-induced sterile inflammation and liver injury. Toxicol Appl Pharmacol 2011; 252: 289–297.
Imaeda AB, Watanabe A, Sohail MA, Mahmood S, Mohamadnejad M, Sutterwala FS et al. Acetaminophen-induced hepatotoxicity in mice is dependent on Tlr9 and the Nalp3 inflammasome. The J Clin Investig 2009; 119: 305–314.
Hoque R, Sohail MA, Salhanick S, Malik AF, Ghani A, Robson SC et al. P2X7 receptor-mediated purinergic signaling promotes liver injury in acetaminophen hepatotoxicity in mice. Am J Physiol Gastrointest Liver Physiol 2012; 302: G1171–G1179.
Xie Y, Williams CD, McGill MR, Lebofsky M, Ramachandran A, Jaeschke H. Purinergic receptor antagonist A438079 protects against acetaminophen-induced liver injury by inhibiting p450 isoenzymes, not by inflammasome activation. Toxicol Sci: Off J Soc Toxicol 2013; 131: 325–335.
Lukens JR, Vogel P, Johnson GR, Kelliher MA, Iwakura Y, Lamkanfi M et al. RIP1-driven autoinflammation targets IL-1alpha independently of inflammasomes and RIP3. Nature 2013; 498: 224–227.
Mao K, Chen S, Chen M, Ma Y, Wang Y, Huang B et al. Nitric oxide suppresses NLRP3 inflammasome activation and protects against LPS-induced septic shock. Cell Res 2013; 23: 201–212.
Horai R, Asano M, Sudo K, Kanuka H, Suzuki M, Nishihara M et al. Production of mice deficient in genes for interleukin (IL)-1α, IL-1β, IL-1α/β, and IL1 receptor antagonist shows that IL-1β is crucial in turpentine induced fever development and glucocorticoid secretion. J Exp Med 1998; 187: 1463–1475.
Rogers HW, Sheehan KC, Brunt LM, Dower SK, Unanue ER, Schreiber RD. Interleukin 1 participates in the development of anti-Listeria responses in normal and SCID mice. Proc Natl Acad Sci USA 1992; 89: 1011–1015.
Yazdi AS, Guarda G, Riteau N, Drexler SK, Tardivel A, Couillin I et al. Nanoparticles activate the NLR pyrin domain containing 3 (Nlrp3) inflammasome and cause pulmonary inflammation through release of IL-1alpha and IL-1beta. Proc Natl Acad Sci USA 2010; 107: 19449–19454.
Lu JY, Sadri N, Schneider RJ. Endotoxic shock in AUF1 knockout mice mediated by failure to degrade proinflammatory cytokine mRNAs. Genes Dev 2006; 20: 3174–3184.
Watanabe H, Ohtsuka K, Kimura M, Ikarashi Y, Ohmori K, Kusumi A et al. Details of an isolation method for hepatic lymphocytes in mice. J Immunol Methods 1992; 146: 145–154.
Van Rooijen N, Sanders A. Liposome mediated depletion of macrophages: mechanism of action, preparation of liposomes and applications. J Immunol Methods 1994; 174: 83–93.
Acharya M, Lau-Cam CA. Simple reversed-phase HPLC method with spectrophotometric detection for measuring acetaminophen-protein adducts in rat liver samples. Sci World J 2012; 2012: 145651.
Liu ZX, Han D, Gunawan B, Kaplowitz N. Neutrophil depletion protects against murine acetaminophen hepatotoxicity. Hepatology 2006; 43: 1220–1230.
Ishida Y, Kondo T, Kimura A, Tsuneyama K, Takayasu T, Mukaida N. Opposite roles of neutrophils and macrophages in the pathogenesis of acetaminophen-induced acute liver injury. Eur J Immunol 2006; 36: 1028–1038.
Roberts RA, Ganey PE, Ju C, Kamendulis LM, Rusyn I, Klaunig JE. Role of the Kupffer cell in mediating hepatic toxicity and carcinogenesis. Toxicol Sci: Off J Soc Toxicol 2007; 96: 2–15.
Szabo G, Csak T. Inflammasomes in liver diseases. J Hepatol 2012; 57: 642–654.
Fisher JE, McKenzie TJ, Lillegard JB, Yu Y, Juskewitch JE, Nedredal GI et al. Role of Kupffer cells and toll-like receptor 4 in acetaminophen-induced acute liver failure. J Surg Res 2013; 180: 147–155.
Ju C, Reilly TP, Bourdi M, Radonovich MF, Brady JN, George JW et al. Protective role of Kupffer cells in acetaminophen-induced hepatic injury in mice. Chem Res Toxicol 2002; 15: 1504–1513.
Holt MP, Yin H, Ju C. Exacerbation of acetaminophen-induced disturbances of liver sinusoidal endothelial cells in the absence of Kupffer cells in mice. Toxicol Lett 2010; 194: 34–41.
Callery MP, Kamei T, Flye MW. Kupffer cell blockade inhibits induction of tolerance by the portal venous route. Transplantation 1989; 47: 1092–1094.
Sato K, Yabuki K, Haba T, Maekawa T. Role of Kupffer cells in the induction of tolerance after liver transplantation. J Surg Res 1996; 63: 433–438.
Yang R, Zou X, Koskinen ML, Tenhunen J. Ethyl pyruvate reduces liver injury at early phase but impairs regeneration at late phase in acetaminophen overdose. Crit care 2012; 16: R9.
Xu J, Zhang X, Monestier M, Esmon NL, Esmon CT. Extracellular histones are mediators of death through TLR2 and TLR4 in mouse fatal liver injury. J Immunol 2011; 187: 2626–2631.
Moles A, Murphy L, Wilson CL, Chakraborty JB, Fox C, Park EJ et al. A TLR2/S100A9/CXCL-2 signaling network is necessary for neutrophil recruitment in acute and chronic liver injury in the mouse. J Hepatol 2013; 60: 782–791.
Cavassani KA, Moreira AP, Habiel D, Ito T, Coelho AL, Allen RM et al. Toll like receptor 3 plays a critical role in the progression and severity of acetaminophen-induced hepatotoxicity. PLoS ONE 2013; 8: e65899.
Yohe HC, O'Hara KA, Hunt JA, Kitzmiller TJ, Wood SG, Bement JL et al. Involvement of Toll-like receptor 4 in acetaminophen hepatotoxicity. Am J Physiol Gastrointest Liver Physiol 2006; 290: G1269–G1279.
Wang X, Sun R, Wei H, Tian Z. High-mobility group box 1 (HMGB1)-Toll-like receptor (TLR)4-interleukin (IL)-23-IL-17A axis in drug-induced damage-associated lethal hepatitis: Interaction of gammadelta T cells with macrophages. Hepatology 2013; 57: 373–384.
Shah N, Montes de Oca M, Jover-Cobos M, Tanamoto K, Muroi M, Sugiyama K et al. Role of toll-like receptor 4 in mediating multiorgan dysfunction in mice with acetaminophen induced acute liver failure. Liver Transplant: Off Publ Am Assoc Study Liver Dis Int Liver Transplant Soc 2013; 19: 751–761.
Lotze MT, Tracey KJ. High-mobility group box 1 protein (HMGB1): nuclear weapon in the immune arsenal. Nat Rev Immunol 2005; 5: 331–342.
Garcia-Arnandis I, Guillen MI, Gomar F, Pelletier JP, Martel-Pelletier J, Alcaraz MJ. High mobility group box 1 potentiates the pro-inflammatory effects of interleukin-1beta in osteoarthritic synoviocytes. Arthritis Res Ther 2010; 12: R165.
Jaeschke H, Liu J. Neutrophil depletion protects against murine acetaminophen hepatotoxicity: another perspective. Hepatology 2007; 45: 1588–1589.
Saito C, Yan HM, Artigues A, Villar MT, Farhood A, Jaeschke H. Mechanism of protection by metallothionein against acetaminophen hepatotoxicity. Toxicol Appl Pharmacol 2010; 242: 182–190.
Mitchell JR, Jollow DJ, Potter WZ, Davis DC, Gillette JR, Brodie BB. Acetaminophen-induced hepatic necrosis. I. Role of drug metabolism. J Pharmacol Exp Therap 1973; 187: 185–194.
Antoine DJ, Williams DP, Kipar A, Laverty H, Park BK. Diet restriction inhibits apoptosis and HMGB1 oxidation and promotes inflammatory cell recruitment during acetaminophen hepatotoxicity. Mol Med 2010; 16: 479–490.
Martin-Murphy BV, Holt MP, Ju C. The role of damage associated molecular pattern molecules in acetaminophen-induced liver injury in mice. Toxicol Lett 2010; 192: 387–394.
Chen GY, Tang J, Zheng P, Liu Y. CD24 and Siglec-10 selectively repress tissue damage-induced immune responses. Science 2009; 323: 1722–1725.
Eigenbrod T, Park JH, Harder J, Iwakura Y, Nunez G. Cutting edge: critical role for mesothelial cells in necrosis-induced inflammation through the recognition of IL-1 alpha released from dying cells. J Immunol 2008; 181: 8194–8198.
Cohen I, Rider P, Carmi Y, Braiman A, Dotan S, White MR et al. Differential release of chromatin-bound IL-1alpha discriminates between necrotic and apoptotic cell death by the ability to induce sterile inflammation. Proc Natl Acad Sci USA 2010; 107: 2574–2579.
Zheng Y, Humphry M, Maguire JJ, Bennett MR, Clarke MC. Intracellular interleukin-1 receptor 2 binding prevents cleavage and activity of interleukin-1alpha, controlling necrosis-induced sterile inflammation. Immunity 2013; 38: 285–295.
Kono H, Karmarkar D, Iwakura Y, Rock KL. Identification of the cellular sensor that stimulates the inflammatory response to sterile cell death. J Immunol 2010; 184: 4470–4478.
Jaeschke H, Williams CD, Ramachandran A, Bajt ML. Acetaminophen hepatotoxicity and repair: the role of sterile inflammation and innate immunity. Liver Int 2012; 32: 8–20.
Williams CD, Bajt ML, Farhood A, Jaeschke H. Acetaminophen-induced hepatic neutrophil accumulation and inflammatory liver injury in CD18-deficient mice. Liver Int: Off J Int Assoc Study Liver 2010; 30: 1280–1292.
Cover C, Liu J, Farhood A, Malle E, Waalkes MP, Bajt ML et al. Pathophysiological role of the acute inflammatory response during acetaminophen hepatotoxicity. Toxicol Appl Pharmacol 2006; 216: 98–107.
Marques PE, Oliveira AG, Pereira RV, David BA, Gomides LF, Saraiva AM et al. Hepatic DNA deposition drives drug-induced liver injury and inflammation in mice. Hepatology 2015; 61: 348–360.
Williams CD, Bajt ML, Sharpe MR, McGill MR, Farhood A, Jaeschke H. Neutrophil activation during acetaminophen hepatotoxicity and repair in mice and humans. Toxicol Appl Pharmacol 2014; 275: 122–133.
Choi DY, Ban JO, Kim SC, Hong JT. CCR5 knockout mice with C57BL6 background are resistant to acetaminophen-mediated hepatotoxicity due to decreased macrophages migration into the liver. Arch Toxicol 2014; 89: 211–220.
Holt MP, Cheng L, Ju C. Identification and characterization of infiltrating macrophages in acetaminophen-induced liver injury. J Leukoc Biol 2008; 84: 1410–1421.
You Q, Holt M, Yin H, Li G, Hu CJ, Ju C. Role of hepatic resident and infiltrating macrophages in liver repair after acute injury. Biochem Pharmacol 2013; 86: 836–843.
Yin H, Cheng L, Holt M, Hail N Jr., Maclaren R, Ju C. Lactoferrin protects against acetaminophen-induced liver injury in mice. Hepatology 2010; 51: 1007–1016.
Dinarello CA. Therapeutic strategies to reduce IL-1 activity in treating local and systemic inflammation. Curr Opin Pharmacol 2004; 4: 378–385.
Acknowledgements
We thank Dr. Yang Liu (Children’s Research Institute, DC) for his brilliant comments and critical reading of the manuscript, Xudong Zhao and Su Liu (Protein Science Core Facility, Chinese Academy of Sciences) for their technical support on serum chemistry analysis and Min Wang (Beijing Institute of Radiation Medicine) for technical support on the isolation and culture of primary hepatocytes. This work was supported by grants from the National Science Foundation of China (31030031 and 81220108018) and the Ministry of Science and Technology of China (2011CB946104) to HT.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Zhang, C., Feng, J., Du, J. et al. Macrophage-derived IL-1α promotes sterile inflammation in a mouse model of acetaminophen hepatotoxicity. Cell Mol Immunol 15, 973–982 (2018). https://doi.org/10.1038/cmi.2017.22
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cmi.2017.22
Keywords
This article is cited by
-
AIM2 regulates autophagy to mitigate oxidative stress in aged mice with acute liver injury
Cell Death Discovery (2024)
-
IL-33/ST2 antagonizes STING signal transduction via autophagy in response to acetaminophen-mediated toxicological immunity
Cell Communication and Signaling (2023)
-
Dose-dependent pleiotropic role of neutrophils during acetaminophen-induced liver injury in male and female mice
Archives of Toxicology (2023)
-
Celastrol-loaded biomimetic nanodrug ameliorates APAP-induced liver injury through modulating macrophage polarization
Journal of Molecular Medicine (2023)
-
Sapidolide A alleviates acetaminophen-induced acute liver injury by inhibiting NLRP3 inflammasome activation in macrophages
Acta Pharmacologica Sinica (2022)