Abstract
Inactivated Sendai virus particles (hemagglutinating virus of Japan envelope (HVJ-E)) have a novel antitumor effect: HVJ-E fused to prostate cancer cells via cell surface receptor causes apoptosis of prostate cancer cells in vitro and in vivo. HVJ-E also induces antitumor immunity by activating natural killer (NK) cells and cytotoxic T cells and suppressing regulatory T cells in vivo. We conducted an open-label, single-arm, phase I/II clinical trial in patients with castration-resistant prostate cancer (CRPC) to determine the safety and efficacy of intratumoral and subcutaneous injection of HVJ-E. Patients with CRPC who were docetaxel-resistant or could not receive docetaxel treatment were eligible. HVJ-E was injected directly into the prostate on day 1 and subcutaneously on days 5, 8 and 12 in two 28-day treatment cycles using a 3+3 dose-escalation design. The primary end points were to evaluate safety and tolerability of HVJ-E. The secondary end points were to analyze tumor immunity and antitumor effect. The study is registered at UMIN Clinical Trials Registry, number UMIN000006142. Seven patients were enrolled, and six patients received HVJ-E. Grade 2 or 3 adverse events (Common Terminology Criteria for Adverse Events Ver. 4.0) were urinary retention and lymphopenia from which the patients recovered spontaneously. No Grade 4 adverse events were observed. Radiographically, three patients had stable disease in the low-dose group, and one patient had stable disease and two had progressive disease in the high-dose group. The prostate-specific antigen (PSA) declined from 14 to 1.9 ng ml−1 in one patient in the low-dose group after two cycles of HVJ-E treatment, and the PSA response rate was 16.6%. NK cell activity was elevated from day 12 to day 28 after HVJ-E administration, whereas serum interleukin-6, interferon (IFN)-α, IFN-β and IFN-γ levels were not affected by HVJ-E treatment. Intratumoral and subcutaneous injections of HVJ-E are feasible and PSA response was observed in a subgroup of CRPC patients.
Similar content being viewed by others
Introduction
Castration-resistant prostate cancer (CRPC) is still a lethal disease even after the development of a new generation of hormonal drugs or chemotherapy, and thus the development of novel therapeutic approaches is required. Immune checkpoint inhibitor therapies (anti-cytotoxic T-lymphocyte antigen-4 (anti-CTLA-4) or anti-programmed cell death-1 (anti-PD-1)) and antigen-specific immunotherapies (dendritic cell-based vaccines or DNA and recombinant protein-based vaccine) were also tried in preclinical and clinical settings.1, 2
Sendai virus, also known as hemagglutinating virus of Japan (HVJ) is a mouse parainfluenza virus, not a human pathogen, and has cell fusion activity.3 Irradiation by ultraviolet light causes the fragmentation of virus RNA and inactivates HVJ by causing it to lose the ability to replicate, but ultraviolet-inactivated HVJ envelope (HVJ-E) still has cell fusion ability. HVJ-E selectively binds to the ganglioside GD1a, which is highly expressed on CRPC cells, and causes apoptosis in prostate cancer cells.4, 5 HVJ-E also induces antitumor immunity by activating natural killer (NK) cells and cytotoxic T cells and also suppresses regulatory T cells in vivo.6 In a xenograft model of colon cancer and renal cancer, HVJ-E treatment induced the secretion of type I interferon (IFN) and interleukin-6 (IL-6) from the dendritic cells, resulting in the eradication of mouse tumor cells by activated cytotoxic T lymphocytes and NK cells.7 Dendritic cells activated by HVJ-E also suppress the regulatory T cells via IL-6.8
On the basis of these results in vitro and in vivo, we conducted an open-label, single-arm phase I/II clinical trial in CRPC patients to determine the safety and efficacy of intratumoral and subcutaneous injection of HVJ-E.
Materials and methods
Study design
This study was a single-arm, open-label, single-center, phase I/II study of HVJ-E in patients with CRPC who were docetaxel resistant or could not receive docetaxel treatments. The primary end points were to evaluate safety and tolerability. The secondary end points were to assess the induction of antitumor immunity and the antitumor effect. This study was conducted at Osaka University Hospital in Japan between 2011 and 2014 in accordance with the Declaration of Helsinki. The study protocol was approved by the institutional review board, and written informed consent was obtained from each patient. The study is registered at UMIN Clinical Trials Registry, number UMIN000006142.
Patients
Eligible patients had to have CRPC and be docetaxel resistant or unable to receive docetaxel treatment and have a prostate in which HVJ-E could be administered. Patients were confirmed to have prostate cancer pathologically. Enzalutamide or abiraterone acetate were not available during this study. The definition of CRPC was prostate-specific antigen (PSA) progression under castration levels of testosterone (<50 ng dl−1). Other inclusion criteria included serum PSA levels of <100 ng ml−1, age ⩾20–⩽90 years, provision of informed consent, Eastern Cooperative Oncology Group performance status 0 or 1, life expectancy of >12 weeks and adequate organ function, including that of the liver, kidney and bone marrow. Major exclusion criteria were brain metastasis, positive skin-prick test for HVJ-E, a history of systemic chemotherapy, radiation and/or immunotherapy within 6 weeks of enrollment, the comorbidity of malignancy, active autoimmune disease and the systemic administration of an immunosuppressant. Patients with low levels of corticosteroid administration (prednisolone <10 mg day−1) for >6 months were not excluded. Exclusion criteria included patients with brain metastasis, positive skin-prick test for HVJ-E, uncontrolled active infection, patients who received systemic chemotherapy, radiation therapy and/or immunotherapy within 6 weeks of enrollment, patients who underwent a clinical trial of unapproved treatments within 4 weeks of enrollment, patients with active autoimmune disease, patients with histories of malignant diseases within 2 years, patients who received organ transplantations or were taking immunosuppressant or patients with abnormal thromboplastin time or activated partial thromboplastin time. Patients being treated with low-dose corticosteroids for >6 months for prostate cancer were eligible.
HVJ-E preparation
HVJ-E was manufactured at GenomIdea Inc. (Osaka, Japan). HVJ was irradiated by the treatment with β-propiolactone and ultraviolet irradiation, which caused the alkylation and the fragmentation of the RNA genome. HVJ-E was purified by four steps of column chromatography, stabilized by lyophilization and stored at 4 °C. The lyophilized HVJ-E was dissolved in distilled water for injection.
Treatment schedule
A 3+3 design was used to determine the maximum tolerated dose of HVJ-E administration. HVJ-E was administered directly to the prostate via transrectal ultrasound-guided injection with a PEIT (percutaneous ethanol injection therapy) needle on day 1, followed by subcutaneous administration on days 5, 8 and 12 in 28-day treatment cycles (Figure 1). The intratumoral injection was carried out by an injection machine driven by air pressure (228AHBZ00005000; Nemoto Kyorindo, Tokyo, Japan) that can control injection speed and solution volume (1.0–1.5 ml) under ultrasound guidance.9 Treatment was repeated for two cycles. Two dose levels were evaluated (low dose of 3000 mNAU and high dose of 10 000 mNAU). The maximum sample size of each dose group was 6 patients for a total of 12 patients. After the patients in the low-dose group completed two cycles, the independent data monitoring committee evaluated safety to determine commencement of the high-dose treatment.
Safety and efficacy assessments
Patients were monitored in hospital from day 1 to day 14 and at each outpatient visit on days 21 and 28 of each cycle. The National Cancer Institute’s Common Terminology Criteria for Adverse Events version 4.0 was used for the coding of adverse events. Serum PSA levels were measured on days 0, 28 and 56. Computed tomography and bone scintigraphy were performed before treatments and after cycles 1 and 2 for radiological assessment.
Antitumor immunity and antitumor efficacy assessments
Antitumor immunity was assessed by the measurement of serum IL-6, IFN-α, IFN-β and IFN-γ levels at pretreatment, day 12 and day 28 of each cycle. Serum NK cell activity was also assessed at pretreatment, day 12 and day 28 of each cycle. The serum anti-HVJ-E antibody titer was measured by anti-parainfluenza virus titer. Antitumor efficacy was assessed by radiological examination of the tumor by computed tomography and by serum PSA levels. The overall response was assessed based on the Response Evaluation Criteria in Solid Tumors (RECIST) criteria version 1.1. The radiological examinations were performed at pretreatment and day 28±3 of each cycle. The serum PSA was measured at pretreatment and day 28 of each cycle, and the response was defined as a reduction of at least 50% from the baseline value.
Statistical analysis
Sample size was based on a previous clinical trial of HVJ-E for melanoma (UMIN000002376). The treated population for the efficacy analysis was defined as all patients who received 1 or 2 cycles of HVJ-E treatment. Paired t-test was performed to analyze the changes in IFNs, IL-6, NK cell activity and anti-HVJ-E antibody titer. A P-value of <0.05 was considered to indicate statistical significance.
Results
Patient characteristics
Seven patients with CRPC were enrolled in the study between 2011 June and 2014 December, and their characteristics are summarized in Table 1. The median age of the patients was 69 years (range 63–83 years). Five of the 7 patients had received docetaxel before enrollment and had experienced resistance to docetaxel. Two patients with no prior docetaxel treatments refused to receive chemotherapy. Six patients had bone metastasis. Four patients were assigned to the low-dose group, and three patients were assigned to the high-dose group. One patient in the low-dose group retracted treatment consent after one cycle of low-dose therapy and did not undergo the second cycle of low-dose treatment due to the progression of disease. The other three patients in the low-dose group and all three patients in the high-dose group completed both cycles of treatment (Figure 2). Thus six patients were assessed for the safety and tolerability of HVJ-E, and seven patients were assessed for the induction of antitumor immunity and antitumor effect.
Adverse events
Generally, the HVJ-E therapy was well tolerated and showed a favorable safety profile. No serious adverse events were reported. Grade 2 or Grade 3 adverse events were urinary retention or lymphopenia, respectively (Table 2). Other adverse events were Grade 1 local reaction at the site of subcutaneous injection of HVJ-E. Two patients in the low-dose group and one patient in the high-dose group developed urinary retention on the day of or 1 day after HVJ-E injection into the prostate. No Grade 4 or Grade 5 adverse events occurred.
PSA response to treatments
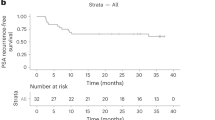
Six patients could be evaluated for response to treatment (Figure 3). Complete response was found in one patient in the low-dose group. In this patient (LD2), PSA levels were reduced from 14.8 ng ml−1 at the baseline to 1.96 ng ml−1 at the end of cycle 2. PSA levels in the other five patients were not reduced after 2 cycles of HVJ-E treatment. The PSA response rate (>50% PSA decline in pretreatment PSA following HVJ-E treatment) was 16.6%.
Radiological response
Radiographically, three patients had stable disease in the low-dose group, and one patient (HD3) had a stable disease and two (HD1 and HD2) had progressive disease in the high-dose group according to the RECIST criteria.
Immune response to HVJ-E treatment
There was no significant change in serum IFN-α, IFN-β, IFN-γ and IL-6 levels and NK cell activity during the HVJ-E treatments (Figure 4). Titers of anti-HVJ-E antibody were significantly elevated at day 28 of cycle 2 compared with those measured at pretreatment (P=0.031).
Discussion
Prostate cancer is an ideal target disease for oncolytic virus therapy because the prostate gland is not necessary for survival and is also easy to access via the transrectal or transperineal pathway for the injection of virus.10 Several systems have been used to engineer a virus that could kill only prostate cancer cells.11 Adenovirus or herpes simplex virus 1 are the major viruses used in oncolytic virus therapy. These viruses were engineered to restrict replication to prostate cancer cells by the inactivation of viral genes and tumor-specific transcriptional control. CG7060 is an engineered adenovirus that can replicate only under the control of PSA promoter. Engineered adenovirus can infect, replicate in and lyse prostate cancer cells.12 Adenovirus vector carrying the human REIC/Dkk-3 gene mediates simultaneous induction of cancer-selective apoptosis and augmentation of antitumor immunity, and a phase I/II clinical study had been conducted.9, 13
HVJ-E is the envelope of an inactivated virus, not a human pathogen, and has no potential for replication. HVJ-E fuses to the prostate cancer cells via gangliosides such as GD1a, which is highly expressed by prostate cancer cells. GD1a is upregulated in several cancer cells and the central nervous system. HVJ-E induces cancer cell-selective apoptosis by activating tumor necrosis factor-related apoptosis-inducing ligand and Noxa in cancer cells via a signaling pathway involving a cytoplasmic helicase, retinoic-acid inducible gene-I and its adaptor, mitochondrial antiviral signaling protein (also known as IPS-1, CARDIF and VISA).5
The primary end points, safety and feasibility, were achieved in this phase I/II study. Only mild adverse events occurred. Urinary retention, hematuria and discomfort on micturition were thought to be due to insertion of the needle into the prostate, resulting in the spontaneous remission. HVJ-E treatment resulted in a PSA response rate of 16.6%, but no radiological complete or partial responses were observed according to the RECIST version 1.1 criteria. Even with the modified RECIST criteria, no complete or partial responses were observed. The levels of IFN-α, IFN-β, IFN-γ and IL-6 and the NK cell activity of the patient responding to the HVJ-E treatment did not change significantly with the HVJ-E treatment, whereas his anti-HVJ-E antibody titer increased. The decline in PSA in this patient might have been caused by the direct effect of HVJ-E on the prostate cancer or other unknown mechanisms of HVJ-E might exist.
Even if HVJ-E could induce an antitumor immune response, the tumor burden of metastatic prostate cancer might override the antitumor effect. ProstVac-VF is a viral-based vaccine for CRPC consisting of two poxvirus vectors (vaccinia and fowlpox) engineered to express PSA and T-cell co-stimulatory molecules.2 In the phase II trial of ProstVac-VF, patients with longer predicted survival had a greater increase in actual survival compared with patients with shorter predicted survival, suggesting that patients with less tumor burden could have fewer immunosuppressive factors from their tumor and thus would be less likely to benefit from vaccine therapy.14 HVJ-E might be also more effective in patients with lower tumor burden.
We did not perform prostate biopsy prior to HVJ-E injection into the prostate. Some CRPC patients who received radiotherapy to the prostate as primary treatment might no longer have viable prostate cancer cells. HVJ-E causes apoptosis in prostate cancer cells followed by activation of NK cells. The absence of viable tumor cells in the prostate might be one reason why HVJ-E treatment could induce a PSA response only in 16.6% of the patients.
Recently, the results of a phase 2, randomized, controlled trial of personalized peptide vaccine immunotherapy in chemotherapy-naive CRPC were reported.15 Selected peptides restricted with HLA-A02, -A24 or -A03 were chosen for each patient based on the evaluation of plasma antipeptide immunoglobulin G levels and cytotoxic T lymphocyte precursors in peripheral blood mononuclear cells. The median number of vaccinations was 32. The PSA response was improved by only 5.3% in patients with vaccination and dexamethasone (PSA response rate, 59.6%) compared with patients with dexamethasone alone (PSA response rate, 54.3%), whereas the median overall survival was significantly improved in patients with vaccination and dexamethasone (73.9 months) compared with patients with dexamethasone alone (34.9 months). In contrast, only two cycles of HVJ-E treatment were performed in this study. Two cycles of HVJ-E treatment might not be adequate to exert an antitumor effect. Moreover, follow-up of the enrolled patients was completed in 2 months. Repeated subcutaneous injections of HVJ-E and longer follow-up might be necessary to gain an objective response in CRPC.
HVJ-E treatment might be effective in certain subgroups of CRPC patients, and patients who might benefit from HVJ-E treatment should be determined. HVJ-E fuses to prostate cancer cells via GD1a, and the GD1a expression level might vary among cases.16 The analysis of GD1a expression in CRPC might help in patient selection for HVJ-E treatment. Because HVJ-E therapy caused no major adverse events, a higher dose of HVJ-E might exert more antitumor effect. The analysis of local histological and/or immune changes in prostate after HVJ-E treatment might provide clues about patient selection. We have started a clinical trial using higher dose of HVJ-E (30 000 and 60 000 mNAU) with a prostate biopsy performed before and after the HVJ-E injection to the prostate (UMIN000017092). Those patients with local advanced prostate cancer who do not meet the criteria for radical prostatectomy might also be good candidates for HVJ-E treatment. The combination of multiple immunotherapies could be another treatment strategy. The recent development of immune checkpoint inhibitors, anti-PD1 antibody or anti-CTLA4 antibody, open up new avenues for treating CRPC. A phase I/II study of ipilimumab in combination with radiotherapy showed that among 50 patients with metastatic CRPC, 8 patients had decline in PSA of >50%, 1 had a complete response and 6 had stable disease.17 In contrast, anti-PD-1 antibody nivolumab was administered to 17 patients with CRPC, but no objective responses were observed.18 Currently, the combination therapy of an immune checkpoint inhibitor with other immune therapy is in clinical trial. Clinical trials of ProstVac in combination with nivolumab and/or ipilimumab in patients with prostatic cancer (NCT02933255) or the combination of nivolumab and ipilimumab in patients with metastatic CRPC (NCT02601014, NCT02985957) have been registered. Clinical trials of ipilimumab in combination with sipuleucel-T (NCT01832870), GVAX (NCT01510288) and ProstVac-VF (NCT02506114) are also in progress. Because HVJ-E treatment is effective in a subgroup of CRPC patients, the combination of HVJ-E treatment with an immune checkpoint inhibitor might be more efficient.
In conclusion, HVJ-E injection into the prostate followed by subcutaneous injection was well tolerated and feasible, and the complete decline of PSA levels was observed in a subgroup of patients with metastatic CRPC. It is necessary to test whether the treatment with HVJ-E improves the survival of patients with CRPC. Further study should be also performed to seek patients who can benefit from this treatment.
References
Parimi S, Chi KN . Chemotherapy for metastatic castration-sensitive prostatecancer. Int J Urol 2016; 23: 726–733.
Schweizer MT, Drake CG . Immunotherapy for prostate cancer: recent developments and future challenges. Cancer Metastasis Rev 2014; 33: 641–655.
Kaneda Y . Update on non-viral delivery methods for cancer therapy: possibilities of a drug delivery system with anticancer activities beyond delivery as a new therapeutic tool. Expert Opin Drug Deliv 2010; 7: 1079–1093.
Hatano K, Miyamoto Y, Nonomura N, Kaneda Y . Expression of gangliosides, GD1a, and sialyl paragloboside is regulated by NF-κB-dependent transcriptional control of α2,3-sialyltransferase I, II, and VI in human castration-resistant prostate cancer cells. Int J Cancer 2011; 129: 1838–1847.
Matsushima-Miyagi T, Hatano K, Nomura M, Li-Wen L, Nishikawa T, Saga K et al. TRAIL and Noxa are selectively upregulated in prostate cancer cells downstream of the RIG-I/MAVS signaling pathway by nonreplicating Sendai virus particles. Clin Cancer Res 2012; 18: 6271–6283.
Kawaguchi Y, Miyamoto Y, Inoue T, Kaneda Y . Efficient eradication of hormone-resistant human prostate cancers by inactivated Sendai virus particle. Int J Cancer 2009; 124: 2478–2487.
Fujihara A, Kurooka M, Miki T, Kaneda Y . Intratumoral injection of inactivated Sendai virus particles elicits strong antitumor activity by enhancing local CXCL10 expression and systemic NK cell activation. Cancer Immunol Immunother 2008; 57: 73–84.
Kurooka M, Kaneda Y . Inactivated Sendai virus particles eradicate tumors by inducing immune responses through blocking regulatory T cells. Cancer Res 2007; 67: 227–236.
Kumon H, Ariyoshi Y, Sasaki K, Sadahira T, Araki M, Ebara S et al. Adenovirus vector carrying REIC/DKK-3 gene: neoadjuvant intraprostatic injection for high-risk localized prostate cancer undergoing radical prostatectomy. Cancer Gene Ther 2016; 23: 400–409.
Gujar SA, Pan DA, Marcato P, Garant KA, Lee PWK . Oncolytic virus-initiated protective immunity against prostate cancer. Mol Ther 2011; 19: 797–804.
Fukuhara H, Homma Y, Todo T . Oncolytic virus therapy for prostate cancer. Int J Urol 2010; 17: 20–30.
Li S, Simons J, Detorie N, O’Rourke B, Hamper U, DeWeese TL . Dosimetric and technical considerations for interstitial adenoviral gene therapy as applied to prostate cancer. Int J Radiat Oncol Biol Phys 2003; 55: 204–214.
Kumon H, Sasaki K, Ariyoshi Y, Ebara S, Hiraki T, Kanazawa S et al. Ad-REIC gene therapy: promising results in a patient with metastatic CRPC following chemotherapy. Clin Med Insights Oncol 2015; 9: 31.
Madan Ra, Gulley JL, Schlom J, Steinberg SM, Liewehr DJ, Dahut WL et al. Analysis of overall survival in patients with nonmetastatic castration-resistant prostate cancer treated with vaccine, nilutamide, and combination therapy. Clin Cancer Res 2008; 14: 4526–4531.
Yoshimura K, Minami T, Nozawa M, Kimura T, Egawa S, Fujimoto H et al. A phase 2 randomized controlled trial of personalized peptide vaccine immunotherapy with low-dose dexamethasone versus dexamethasone alone in chemotherapy-naive castration-resistant prostate cancer. Eur Urol 2016; 70: 35–41.
Hatano K, Miyamoto Y, Mori M, Nimura K, Nakai Y, Nonomura N et al. Androgen-regulated transcriptional control of sialyltransferases in prostate cancer cells. PLoS ONE 2012; 7: e31234.
Slovin SF, Higano CS, Hamid O, Tejwani S, Harzstark A, Alumkal JJ et al. Ipilimumab alone or in combination with radiotherapy in metastatic castration-resistant prostate cancer: results from an open-label, multicenter phase I/II study. Ann Oncol 2013; 24: 1813–1821.
Topalian SL, Hodi FS, Brahmer JR, Gettinger SN, Smith DC, McDermott DF et al. Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med 2012; 366: 2443–2454.
Acknowledgements
We thank Yasutomo Nasu (Department of Urology, Okayama University Graduate School of Medicine, Dentistry and Pharmaceutical Sciences, Okayama, Japan) for providing the injection machine and Katsuhisa Saito, Atsuhiro Saito and Chihiro Maruyama (Medical Center for Translational Research Osaka University Hospital) for supporting the clinical trial. This study was supported by the Japan Science and Technology Agency.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Toshihiro Nakajima is the CEO of GenomIdea, Inc. Yasufumi Kaneda is a stock-holder (0.3%) of GenomIdea, Inc. The other authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Fujita, K., Nakai, Y., Kawashima, A. et al. Phase I/II clinical trial to assess safety and efficacy of intratumoral and subcutaneous injection of HVJ-E in castration-resistant prostate cancer patients. Cancer Gene Ther 24, 277–281 (2017). https://doi.org/10.1038/cgt.2017.15
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cgt.2017.15
This article is cited by
-
Intratumoral injection of hemagglutinating virus of Japan-envelope vector yielded an antitumor effect for advanced melanoma: a phase I/IIa clinical study
Cancer Immunology, Immunotherapy (2020)