Abstract
HMGB1 is passively released by injured or dying cells and aggravates inflammatory processes. The release of HMGB1 and calcium overload have each been reported to be important mediators of H2O2-induced injury. However, a potential connection between these two processes remains to be elucidated. In the present study, we employed H2O2-induced hepatocytes to investigate how calcium overload takes place during cellular injury and how the extracellular release of HMGB1 is regulated by this overload. In addition, we investigated the use of 58-F, a flavanone extracted from Ophiopogon japonicus, as a potential therapeutic drug. We show that the PLCγ1–IP3R–SOC signalling pathway participates in the H2O2-induced disturbance of calcium homoeostasis and leads to calcium overload in hepatocytes. After a rise in intracellular calcium, two calcium-dependent enzymes, PKCα and CaMKIV, are activated and translocated from the cytoplasm to the nucleus to modify HMGB1 phosphorylation. In turn, this promotes HMGB1 translocation from the nucleus to the cytoplasm and subsequent extracellular release. 58-F effectively rescued the hepatocytes by suppressing the PLCγ1–IP3R–SOC signalling pathway and decreasing the calcium concentration in cells, thus reducing HMGB1 release.
Similar content being viewed by others
Introduction
Calcium is a universal second messenger involved in a remarkably wide range of cellular processes.1 Disordered cytosolic calcium signalling can lead to severe damage or result in cell death.2,3 In non-excitable cells, Ca2+ signals are generated by the phospholipase C (PLC)-mediated hydrolysis of phosphatidylinositol bisphosphate (PIP2) to yield 1,4,5- trisphosphate (IP3), leading to the subsequent activation of the inositol trisphosphate receptor (IP3R). This mediates the release of Ca2+ from the endoplasmic reticulum (ER),4 followed by transmembrane Ca2+ entry through the opening of store-operated calcium (SOC) channels.5 SOC channels are the predominant mechanism of calcium entry in both excitable and non-excitable cells and are activated by the depletion of internal calcium stores, for example, from the ER. Upon opening, SOC channels promote calcium entry through the plasma membrane (PM), a major mechanism for Ca2+ influx.6,7 So far, two major molecular components of the SOC channel signalling pathway have been identified: stromal interaction molecule 1 (STIM1) and Orai1.8,9 STIM1 serves as a calcium sensor that can directly bridge the ER to PM at specialized junctions, aggregating into puncta in response to calcium store depletion and triggering the activation of SOC channels located in the PM.10 Orai1 channels comprise six monomers and are localized diffusely in the PM of resting cells. They are recruited into puncta by STIM1 through a direct interaction, opening SOC channels to mediate store-operated calcium entry (SOCE) to ensure the optimal refilling of the ER.11,12 SOCE plays a major role in Ca2+ influx in non-excitable cells, including hepatocytes.13 Patch-clamp experiments in liver cells showed that only one type of SOC channel, a highly Ca2+-selective channel, could be detected.14,15 Therefore, SOC channels are a research hotspot in the physiology and pathology of liver disease.
Hydrogen peroxide (H2O2) is a key mediator underlying cellular oxidative stress and is involved in a wide variety of pathological processes. It can cause intracellular Ca2+ overload in various cell types due to oxidative stress.16–18 Therefore, any therapeutic approach that can prevent H2O2-induced intracellular Ca2+ overload and improve intracellular Ca2+ regulation would be beneficial for cells. On the other hand, PLCγ1, the first protein in the PLCγ1–IP3R–SOC Ca2+ signalling pathway, is upregulated as a result of H2O2-induced oxidative stress. PLC isozymes are subdivided into three types (β, γ, δ), and the γ type includes two isoforms (PLCγ1 and PLCγ2). While PLCγ1 shows a ubiquitous expression pattern, PLCγ2 is mainly expressed in B-cells.19 Moreover, it is well established that PLCγ1 undergoes direct phosphorylation on tyrosine residues in response to H2O2 treatment.20,21 However, to the best of our knowledge, whether PLCγ is involved in H2O2-induced Ca2+ release in hepatocytes remains unknown.
High mobility group box 1 (HMGB1) is a highly conserved 30 kDa DNA-binding protein. In response to injury, HMGB1 is passively released from stressed cells,22 and excessive extracellular HMGB1 adversely contributes to injury-elicited pathogenesis.23 In the same way, HMGB1 plays a key role in various forms of liver injury.24 The release of HMGB1 is controlled by two critical steps that regulate the flux of HMGB1 from the nucleus to the cytoplasm and subsequently from the cytoplasm to the extracellular compartment. The phosphorylation of HMGB1 at critical serine residues is essential for its translocation from the nucleus to cytoplasm.25 The activation of two calcium-mediated protein kinases, classical protein kinase C (PKC) and Ca2+/calmodulin-dependent protein kinase IV (CaMKIV), is required for HMGB1 phosphorylation.26,27 PKC has many isoenzymes, and among them, PKCα is involved in HMGB1 release.26 CaMKs are a family of proteins comprising CaMK I–IV. Activation typically requires Ca2+/calmodulin binding and can be augmented or sustained by phosphorylation. The identity of the specific CaMK family members involved in hypoxia-induced HMGB1 release is uncertain, but H2O2 treatment has been shown to activate CaMKIV in hepatocytes.28 In the present report, we employed these two calcium-dependent enzymes to determine whether they participate in HMGB1 phosphorylation associated with secretion.
Oxidative stress sensitizes hepatocytes to either calcium overload29 or HMGB1 release.30 Although HMGB1 and calcium have been separately reported to be important mediators of oxidative stress-induced injury, the potential relationship between them remains unknown. Here, we evaluate the hypothesis that SOCE activation causes calcium influx leading to calcium overload after H2O2 treatment, followed by the activation of PKCα and CaMKIV and HMGB1 release in hepatocytes. Our findings support this hypothesis, demonstrating that SOCE activation leads to a cytosolic calcium increase and HMGB1 release from cells after H2O2 treatment. In addition, the compound 5,8-dimethoxy-6-methyl-7-hydroxy-3-3(2-hydroxy-4-methoxybenzyl) chroman-4-one (58-F) is a flavanone extracted from Ophiopogon japonicas, which has been widely distributed and used clinically in mainland China,29,31 and we recently reported that 58-F protects against ROS-induced liver injury.32 In the present study, we explore the protective contribution of 58-F to H2O2-induced calcium homoeostasis and HMGB1 release.
Results
Release of HMGB1 following H2O2-induced hepatocyte injury/death is involved in calcium entry
Our previous studies found that H2O2 could induce apoptosis by disrupting cellular calcium homoeostasis.33 To confirm the effect of H2O2 on cell injury/death, we examined the release of lactate dehydrogenase (LDH) from cells to media as well as the levels of HMGB1 in the media, cytosol and nucleus. After incubation with 500 μM H2O2 for varying times, the levels of LDH in the cellular media increased approximately 2.5 and 3-fold at 8 and 12 h, respectively (Figure 1a). HMGB1 is passively released to the extracellular space upon cellular injury/death by almost all cells that have a nucleus, and it acts as a signal to neighbouring cells of ongoing damage.23 Moreover, 500 μM H2O2 led to an increase in HMGB1 release into the media (Figure 1b), and western blot analysis of cytosolic and nuclear lysates revealed that the amount of HMGB1 protein progressively increased in the cytosol and decreased in the nucleus after H2O2 treatment (Figures 1c and d). Pretreatment with 100 μg/ml N-acetylcysteine (NAC), a common antioxidant, decreased the content of HMGB1 in the media (Figure 1b). However, HMGB1 levels in the cytosol and nucleus continued to trend the same way with or without the antioxidant (Figures 1e and f). Further, we tested the effects of calcium signalling pathway inhibitors on HMGB1 release. HMGB1 levels in the cellular media induced by H2O2 exposure were markedly reduced by pretreatment with 10 μM U73122 (a PLC inhibitor) or 50 μM 2-APB (an IP3R inhibitor) (Figure 1b). These findings indicate that cellular injury or death caused by H2O2 leads to the release of HMGB1 and that this process is regulated by a calcium signalling pathway.
HMGB1 release induced by H2O2 is calcium dependent. (a) The rate of cell injury was measured using a Cytotoxicity LDH Assay Kit. (b) The cells were pre-treated with 100 μg/ml NAC, 50 μM 2-APB or 10 μM U73122 for 16 h, then co-incubated with H2O2 for 8 h, and HMGB1 levels in media were measured by ELISA. (c and d) The cells were treated with 500 μM H2O2, and a western blot was used to measure HMGB1 protein levels in the cytosolic/nuclear fractions at 4, 6, 8 and 12 h. (e and f) The cells were pre-treated with NAC for 16 h, then co-incubated with H2O2 for 8 h and HMGB1 levels in the cytosolic/nuclear were measured by western blot. Shown are representative results from one of three independent experiments. *P<0.05, **P<0.01, ***P<0.001, compared with the control; #P<0.05, ###P<0.001, compared with the H2O2 treatment group.
PLCγ1–IP3R–SOC participate in H2O2-induced calcium entry into cells
To determine whether H2O2 affects calcium signalling in hepatocytes through SOC channels, we performed calcium imaging of hepatocytes stimulated with 500 μM and 1 mM H2O2 in a calcium-free buffer (plus 1 mM EGTA). We observed an increase in the height of the left peaks representing Ca2+ transients in the cytoplasm, due to calcium release from intracellular store(s) for example, from the ER (Figure 2a). After replacing the extracellular medium with a 2 mM calcium chloride solution, an increase in the heights of the right peaks representing Ca2+ transients in the cytoplasm from media were observed (Figure 2a), indicating extracellular calcium influx through the PM due to the depletion of ER stores. Furthermore, NAC was used to assess whether the calcium influx was caused by oxidative stress, and we observed a significant reduction of H2O2-induced left and right peaks after NAC pretreatment (Figures 2c and d).
Changes in real-time Ca2+ fluorescence intensity induced by H2O2. (a) The cells were stimulated with 500 μM and 1 mM H2O2 in Ca2+-free buffer, followed by the addition of 2 mM CaCl2 to the medium. (c) The cells were pre-treated with 100 μg/ml NAC for 24 h, followed by stimulation with 500 μM H2O2 and the subsequent addition of 2 mM CaCl2 to the medium. (e) The cells were pre-treated with 50 μM 2-APB or 10 μM U73122 for 24 h, followed by stimulation with 500 μM H2O2 and the subsequent addition of 2 mM extracellular Ca2+. (b, d and f) The quantification of intracellular Ca2+ at the peak after adding H2O2 and CaCl2, respectively. (g and h) Changes in real-time Ca2+ fluorescence intensity of transfected cells induced by H2O2. Intracellular Ca2+ was quantified at the peak after adding CaCl2. (i and j) The expression of STIM1 in transfected cells detected by western blot. Shown are representative results from one of three independent experiments. *P<0.05, **P<0.01, ***P<0.001, compared with the control; &&P<0.01, &&&P<0.001, compared with the NC-siRNA.
To investigate the possible involvement of PLC in H2O2-induced cytosolic calcium increases, cells were pre-treated with 10 μM U73122 before H2O2 addition. The two peaks representing calcium entry into the cytoplasm were significantly reduced when cells were pre-treated with U73122 before H2O2 addition, revealing that PLC contributes to the cytosolic calcium increase. PLC is known to stimulate IP3R in the ER membrane through the synthesis of IP3. Thus, to determine whether this pathway is important for H2O2-induced calcium increase, cells were pre-incubated with 50 μM 2-APB (an IP3R inhibitor), which also led to significantly reduced H2O2-induced cytosolic calcium (Figures 2e and f). In addition, we assessed the role of SOC channels in this calcium influx by knocking down STIM1 with shRNA (Figures 2i and j). si-STIM1 inhibited the elevation of the right peak but not the left peak of calcium influx, indicating that SOC channels affect extracellular calcium influx without altering ER Ca2+ store release (Figures 2g and h). Together, these results support the notion that PLC induces a signalling cascade through IP3 and the subsequent stimulation of SOC channels to mediate H2O2-induced cytosol calcium increase.
To further validate proteomic changes that might be responsible for the H2O2-induced cytosolic calcium increase, the levels of some related proteins were assessed via western blot. Cells were exposed to H2O2 at concentrations of 100, 500 or 1000 μM for 4 h or 500 μM for 1, 2, 3 or 4 h. The results revealed that both STIM1 and Orai1 protein levels increased in a H2O2 concentration- and time-dependent manner (Figures 3a–d). Furthermore, NAC and 2-APB reversed this H2O2-induced increase in STIM1 and Orai1 levels (Figures 3e–h).
SOC participates in the H2O2-induced disturbance of calcium homoeostasis. (a–h) Western blot for STIM1 and Orai1 protein. Cells were stimulated with H2O2 at varying concentrations (100 μM, 500 μM or 1 mM) for 4 h (a and b) or were stimulated for varying periods of time (1, 2, 3 or 4 h) with 500 μM H2O2 (c and d). Cells were pre-treated with 100 μg/ml NAC (e and f) or 50 μM 2-APB (g and h) or 10 μM U73122 (i and j) for 21 h, then co-incubated with 500 μM H2O2 for 3 h. PLCγ1 and p-PLCγ1 were detected by western blot. Shown are representative results from one of three independent experiments. *P<0.05, **P<0.01, ***P<0.001, compared with the control; #P<0.05, ##P<0.01, compared with the H2O2-treated group.
Because the PLC–IP3R pathway triggers SOC channels, we tested the levels of phosphorylated and total PLCγ1 after H2O2 treatment. Our results showed that H2O2 did not stimulate an increase in total PLCγ1 protein, but the levels of phosphorylated protein increased. These changes were significantly attenuated by the PLCγ1 inhibitor U73122 (Figures 3i and j).
HMGB1 secretion and translocation are Ca2+ dependent
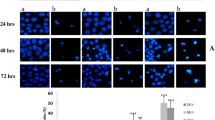
To determine whether intracellular calcium overload could induce cell injury, cells were treated with different concentrations (10, 25 and 50 μM) of A23187, a calcium ionophore and intracellular Ca2+ levels were examined using Fluo-4/AM. Intracellular fluorescence signals gradually increased from 10 to 50 μM in a concentration-dependent manner with A23187 treatment (Figures 4a and b). However, the bright fluorescence signals induced by A23187 were dampened by co-treatment with 1 mM EGTA, a calcium chelator. We also measured the release of LDH into the media under these conditions by ELISA assay (Figures 4c and d) and observed a significant concentration- and time-dependent increase with the A23187 treatment (Figures 4c and d). These results indicate that intracellular calcium overload induces cellular injury.
A23187-induced cell injury. (a and b) Intracellular Ca2+ levels at 24 h after A23187 treatment (10, 25, 50 μM) or in the presence of 1 mM EGTA plus A23187 treatment (25 μM, 50 μM) visualized by confocal microscopy. (c and d) The rate of cell injury assessed using the Cytotoxicity LDH Assay Kit. Shown are representative results from one of three independent experiments. *P<0.05, **P<0.01, ***P<0.001, compared with the control; #P<0.05, compared with the 25 μM A23187-treated group; &&P<0.01, compared with the 50 μM A23187-treated group.
Similarly, HMGB1 levels in the cellular media increased with increasing concentrations of A23187 treatment (10, 25 or 50 μM) in a concentration-dependent manner and also markedly increased at 24 and 48 h in a time-dependent manner (Figures 5a and b). Under the same conditions, the HMGB1 levels in the nucleus gradually decreased after A23187 treatment (10, 25 or 50 μM), consistent with a corresponding increase in cytosolic levels (Figures 5c and d). Similar results were observed with different time periods of A23187 incubation (Figures 5e and f). Furthermore, in cells treated with 25 μM A23187 combined with 1 mM EGTA, HMGB1 levels in the media and cytosol significantly decreased, coincident with an increase in nuclear levels (Figures 5g–i). Together, these results indicate that A23187 induces HMGB1 translocation and release through an increase in intracellular calcium.
A23187-induced HMGB1 translocation and release in hepatocytes. (a and b) HMGB1 contents in culture media were determined using ELISA. (c–f) HMGB1 protein levels in cytosolic/nuclear fractions were measured by western blot. After incubation with A23187 (10, 25 or 50 μM) for 30 min followed by 24 h without A23187 (a, c and d) or 25 μM A23187 for 30 min followed by 12, 24 or 48 h without A23187 (b, e and f), the media and cells were harvested. (g) Cells were incubated with both 25 μM A23187 and 1 mM EGTA for 30 min, and HMGB1 levels were measured in culture media by ELISA. (h and i) HMGB1 levels in cytosolic/nuclear fractions were measured by western blot. Shown are representative results from one of three independent experiments. *P<0.05, **P<0.01, ***P<0.001, compared with the control; #P<0.05, ##P<0.01, compared with the A23187-treated group.
It is reported that PKCα and CaMKIV are involved in HMGB1 phosphorylation and release.26,34 To elucidate whether HMGB1 release from hepatocytes under oxidative stress is also dependent on these kinases, we examined changes in nuclear PKCα and CaMKIV levels and their interaction with HMGB1 after H2O2 exposure. The content of PKCα in the nucleus after H2O2 treatment increased at approximately 4–5 h, then decreased from 6 h. CaMKIV content increased at approximately 5–6 h and went down at 8 h (Figures 6a and b). The results of immunoprecipitation analysis of HMGB1 with PKCα or CaMKIV showed that both PKCα and CaMKIV can directly interact with HMGB1 in the nucleus over different time periods (Figure 6c).
Intracellular calcium mediates the translocation and release of HMGB1 by PKCα and CaMKIV. (a)The nuclear levels of PKCα and CaMKIV were examined by western blot after H2O2 treatment (a and b) or A23187 treatment (d and e). (c and f) The cells were stimulated with H2O2 or A23187, and nuclear extracts were harvested at each time point, immunoprecipitated with anti-HMGB1 and protein A agarose, and subjected to western blot analysis for PKCα and CaMKIV expression. Shown are representative results from one of three independent experiments. *P<0.05, **P<0.01, ***P<0.001, compared with the control.
Owing to the calcium-dependence of PKCα and CaMKIV activity, we also measured the role of A23187 in the interactions of PKCα and CaMKIV with HMGB1. The results showed that the nuclear levels of PKCα increased at 0.5 and 1 h but decreased at 2–3 h after A23187 treatment. Additionally, the levels of CaMKIV increased at 0.5–2 h and went down at 3 h after A23187 treatment. This indicates that both kinases are induced by A23187 treatment but that CaMKIV induction persists longer than PKCα induction (Figures 6d and e). To observe whether the interactions of PKCα or CaMKIV with HMGB1 in the nucleus are also regulated by calcium, nuclear extracts isolated from cells treated with or without A23187 were immunoprecipitated with anti-HMGB1. Both PKCα and CaMKIV could be observed in the resulting western blot (Figure 6f). These results suggest that PKCα and CaMKIV directly bind to HMGB1 in A23187-treated cells.
Effects of 58-F on the PLCγ1–IP3R–SOC signalling pathway in the H2O2-induced [Ca2+]i increase
Recently, we reported that 58-F protects against ROS-induced liver injury. In addition, we also showed that H2O2 could induce apoptosis by disrupting cellular calcium homoeostasis.33,35 The [Ca2+]i increase by H2O2 prompted us to investigate the possibility that the inhibition of Ca2+ influx by 58-F is at least partly due to the suppression of the PLCγ1–IP3R–SOC signalling pathway. The level of calcium entry into cells with or without 58-F pretreatment was detected by calcium imaging and confocal microscopy. In agreement with Figure 2, the stimulation of hepatocytes with 500 μM H2O2 in a calcium-free buffer led to an increase in cytosolic calcium due to the release of calcium from ER stores. After replacing the extracellular medium with a 2 mM CaCl2 solution, a further increase in cytosolic calcium through the PM was apparent, due to the depletion of ER stores. Notably, the fluorescence intensity after adding H2O2 and CaCl2 was attenuated by pretreatment with 50 or 100 μM 58-F (Figures 7a and b).
58-F reduces the H2O2-induced [Ca2+]i increase. (a) Cells were pre-treated with 10, 50 or 100 μM 58-F for 24 h, followed by stimulation with 500 μM H2O2 in a Ca2+-free buffer and the subsequent addition of 2 mM CaCl2 into the media. (b) The quantification of intracellular Ca2+ was performed at two peaks after adding H2O2 and CaCl2. (c–f) Cells were pre-treated with 10, 50 and 100 μM 58-F for 21 h, then co-incubated with 500 μM H2O2 for 3 h (c and d) or with 50 μM 58-F for 24, 48 and 72 h. (e and f) Western blot analysis of STIM1 and Orai1 proteins. (g and h) Cells were pre-treated with 10 μM U73122 or 5 0 μM 58-F for 21 h, then co-incubated with 500 μM H2O2 for 3 h, followed by western blot analysis of p-PLCγ1 and PLCγ1 proteins. Shown are representative results from one of three independent experiments. *P<0.05, compared with the control; #P<0.05, compared with the H2O2 treatment group.
To assess the effects of 58-F on the protein levels of members of the PLCγ1–IP3R–SOC signalling pathway, we measured the levels of STIM1, Orai1, PLCγ1 and p-PLCγ1 following treatment. The H2O2-induced increased levels of both STIM1 and Orai1 were reduced by pretreatment with 58-F at concentrations ranging from 10 to 100 μM or by pretreatment with 50 μM 58-F for different periods of time (24, 48 or 72 h) (Figures 7c–f). Furthermore, similar to the effects observed with U73122, 58-F significantly attenuated the increased levels of p-PLCγ1 induced by H2O2 without affecting the levels of total PLCγ1 (Figures 7g and h). These findings suggest that 58-F suppresses the H2O2-induced [Ca2+]i increase through PLCγ1-mediated SOC channels.
Effects of 58-F on the translocation and release of HMGB1 induced by H2O2
To confirm the cellular protective effect of 58-F, we examined the release of LDH from cells to media and the levels of HMGB1 in the media, cytosol and nucleus. The extracellular release of both LDH and HMGB1 was decreased after pretreatment with 10, 50 or 100 μM 58-F (Figures 8a and b). Additionally, the translocation of HMGB1 from the nucleus to the cytosol was also suppressed in time- and dose-dependent manners (Figures 8c–f).
58-F reduces the H2O2-induced translocation and release of HMGB1. (a) LDH release of cells after treatment with 10, 50 or 100 μM 58-F for 24 h. (b) HMGB1 levels in culture media were measured by ELISA. Cells were pre-treated with 50 μM 58-F for 16 h, then co-incubated with 500 μM H2O2 for 8 h. (c and d) HMGB1 protein levels in the cytosolic/nuclear fractions were measured by western blot. Cells were pre-treated with 10, 50 or 100 μM 58-F for 16 h, then co-incubated with H2O2 for 8 h. (e and f) HMGB1 protein levels in the cytosolic/nuclear fractions were measured by western blot. Cells were pre-treated with 50 μM 58-F for 24, 48 or 72 h. (g and h) PKCα and CaMKIV expression levels in the nucleus were measured by western blot. Cells were pre-treated with 50 μM 58-F for 20 or 19 h, then continuously co-treated with 500 μM H2O2 for 4 or 5 h. (i) Immunoprecipitation was performed with HMGB1 antibody, followed by western blot for PKCα or CaMKIV. Cells were pre-treated with 50 μM 58-F for 20 or 19 h, then co-incubated with 500 μM H2O2 for 4 or 5 h. Nuclear extracts were harvested, immunoprecipitated with anti-HMGB1 and protein A agarose, then subjected to western blot analysis for PKCα and CaMKIV. Shown are representative results from one of three independent experiments. *P<0.05, **P<0.01, ***P<0.001, compared with the control; #P<0.05, ##P<0.01, ###P<0.001, compared with the H2O2-treated group; △P<0.05, compared with the H2O2-treated 4 h group; &&P<0.01, compared with the H2O2-treated 5 h group.
Likewise, the nuclear levels of PKCα and CaMKIV in cells pre-treated with 50 μM 58-F were significantly less than those in cells with a single H2O2 treatment from 4 to 5 h (Figures 8g and h). To further assess the direct interaction of PKCα or CaMKIV with HMGB1, nuclear lysates were immunoprecipitated with anti-HMGB1, then subjected to western blot with PKCα or CaMKIV antibodies. The direct interaction of PKCα and CaMKIV with HMGB1 in the nucleus was inhibited by 58-F pretreatment (Figure 8i).
Discussion
A PLCγ1–IP3R–SOC signalling pathway is involved in the disturbance of calcium homoeostasis in hepatocytes induced by H2O2
Calcium signals, which can be induced by a variety of stimuli, control a myriad of functions in cells. Hepatocytes can increase their cytoplasmic Ca2+ concentration in two ways: release from intracellular storage pools, primarily ER,36 and the entry of extracellular calcium to maintain adequate Ca2+ stores. It is well established that PLCγ1 undergoes phosphorylation on tyrosine residues in response to H2O2 treatment.20,21 Under either physiological or pathological conditions, the activation of the PLCγ1 pathway produces IP3, which binds to its receptor IP3R in the ER and mobilizes Ca2+ out of ER. Subsequently, SOC channels are activated, leading to Ca2+ influx and the replenishing of ER stores. In our study, the role of PLCγ1-IP3R signalling in SOC was examined, and the results showed that H2O2-induced elevated [Ca2+]i was almost abolished and that the increased phosphorylation of PLCγ1 was reduced when cells were pre-treated with the generic PLC inhibitor U73122 or the IP3R inhibitor 2-APB. These findings are in agreement with earlier publications reporting that the phosphorylation and activation of PLC by a sulfhydryl oxidation-dependent mechanism, which leads to increased IP3 synthesis and subsequent activation of the IP3 receptor, induces the release of Ca2+ from intracellular stores37,38 and that the H2O2-induced [Ca2+]i rise could be prevented by U73122 or 2-APB.39 SOC is defined as enhanced Ca2+ import from the extracellular space after depletion of calcium in the ER.6,40 Among all Ca2+-permeable channels confirmed to be expressed in hepatocytes, SOC channels are the principal pathway for Ca2+ influx through the PM.35,41 To confirm whether SOC participates in H2O2-induced Ca2+ influx, we carried out a series of experiments. First, our data demonstrate that H2O2 elicits an increase in intracellular [Ca2+]i in the absence of extracellular calcium, indicating that H2O2 can mobilize calcium out of the ER. After adding CaCl2, an apparent extracellular Ca2+ influx was observed, and the overall rise in calcium concentration significantly increased. Furthermore, the antioxidant NAC inhibited Ca2+ influx from the extracellular space. These findings are in agreement with the view that H2O2 triggers Ca2+ release into the cytoplasm in two steps: Ca2+ release from internal stores, followed by SOC from the extracellular supply. Second, the protein levels of STIM1 and Orai1 increased after H2O2 treatment, while si-STIM1 almost abolished the H2O2-induced Ca2+ influx without affecting the release of Ca2+ from the ER (Figure 2). Moreover, NAC was found to inhibit the H2O2-induced increase of STIM1 and Orai1 protein levels. These findings confirm that Ca2+ enters cells through activated SOC channels with H2O2 stimulation. Together, we conclude that calcium overload in hepatocytes caused by H2O2 occurs through the PLCγ1–IP3R–SOC signalling pathway.
The increase of intracellular calcium can activate PKCα and CaMKIV to promote HMGB1 release
Extracellular HMGB1 is derived from either active secretion by innate immune cells or by passive release from dead or stressed cells as a late inflammatory mediator for infectious or noninfectious inflammation.24 The passive release of HMGB1 from dead/stressed cells is due to its export from the nucleus to the cytoplasm and subsequent release into the extracellular space due to increased cell membrane permeability.23,42 Youn and co-workers43 and Tsung Allan et al.28 have reported that HMGB1 release can be induced by A23187 in murine hepatocytes or in RAW264.7 cells and that this release is reduced by BAPTA, a chelator of Ca2+, indicating that Ca2+ plays a critical role in oxidative stress-induced HMGB1 release. Our results show that both HMGB1 and LDH contents in the media increased after H2O2 treatment and that HMGB1 levels in the media induced by H2O2 exposure are markedly reduced by pretreatment with either the antioxidant NAC or the calcium pathway inhibitors 2-APB or U73122. This confirms the finding that HMGB1 release from stressed/dead cells due to oxidative stress is regulated by calcium homoeostasis. To further verify the possibility that Ca2+ overload in the cytosol due to oxidative stress leads to HMGB1 release, we employed the calcium ionophore A23187. Our data show that increasing intracellular levels of calcium with A23187 results in the translocation of HMGB1 from the nucleus to the cytosol and its release to the extracellular space, which was markedly reduced by treatment with the calcium chelator EGTA.
Phosphorylation of serine residues within the HMGB1 nuclear localization signal may also contribute to the regulation of HMGB1 cytoplasmic translocation, which is a key step for its release into the extracellular space.22,25 Two calcium-dependent kinases, CaMKIV and PKCα, have been implicated in the regulation of HMGB1 phosphorylation and release.27,43 Signalling events upstream of PKCα and CaMKIV include Ca2+ release from the ER. We noted an increase in the levels of both PKCα and CaMKIV within the nucleus and an enhancement of their direct interaction with HMGB1 after A23187 stimulation. This is consistent with the results of H2O2 treatment, supporting the view that the H2O2-mediated increase in cytoplasmic Ca2+ is sufficient to activate CaMKIV and PKCα nuclear translocation and HMGB1 phosphorylation.
58-F intervention regulates intracellular calcium and reduces the release of HMGB1 induced by H2O2
Accumulating evidence directly implicates HMGB1 in various diseases, and it has been considered as a therapeutic target for sterile inflammation and infection.44 We recently reported that 58-F protected against ROS-induced liver injury, but the mechanism was still to be elicited. The results reported in this work indicate that 58-F inhibits calcium entry through SOC channels triggered by the PLCγ1-IP3R signalling pathway in response to oxidative damage. We also showed that 58-F suppresses HMGB1 translocation from the nucleus to the cytoplasm and its eventual extracellular release by inhibiting the activation of PKCα and CaMKIV.
Conclusion
In summary (Figure 9), we determined the role of the PLCγ1–IP3R–SOC signalling pathway in the regulation of calcium influx in cells undergoing oxidative stress and identified calcium homoeostasis in hepatocytes as a key mechanism regulating HMGB1 translocation from the nucleus to the cytoplasm for extracellular release. Our data further support the idea that calcium-dependent kinases PKCα and CaMKIV participate in HMGB1 phosphorylation, a key step leading to HMGB1 release. On the basis of these findings, 58-F, a flavanone extracted from O. japonicus, was shown to interfere with calcium overload caused by the response of the PLCγ1–IP3R–SOC signalling pathway to oxidative stress and with the PKCα- and CaMKIV-mediated regulation of HMGB1 release. These findings may be important for designing therapies to prevent hepatocytes from oxidative stress-induced injury/death.
HMGB1 release regulated by the PLCγ1–IP3R–SOC signalling pathway during calcium overload in hepatocytes. The proposed model showing the release of HMGB1 following H2O2 treatment. H2O2 activates the PLCγ1–IP3R–SOC signalling pathway, leading to calcium influx and the activation of calcium-dependent kinases PKCα and CAMKIV and triggering HMGB1 phosphorylation. Phosphorylated HMGB1 translocates from the nucleus to the cytoplasm and is ultimately released into the extracellular space.
Materials and methods
Drugs and reagents
Thirty percent H2O2 was purchased from Sinopharm Chemical Reagent Co. (Shanghai, China). 58-F was purchased from Shanghai Yilin Biotechnology Co., Ltd (Shanghai, China). A23187 was purchased from Abcam (Cambridge, MA, USA). 2-Aminoethoxydiphenyl borate(2-APB) and NAC were purchased from Sigma (St. Louis, MO, USA). EGTA was purchased from Amresco (Solon, OH, USA). U73122 was purchased from Selleck (Houston, TX, USA). Dulbecco’s modified Eagle’s medium (DMEM), fetal calf serum (FBS) and penicillin–streptomycin were purchased from Gibco (Carlsbad, CA, USA). Hanks and D-Hanks were purchased from Gino Biological Pharmaceutical Co., Ltd (Hangzhou, China). Fluo-4/AM, Pluronic F-127 and Cytotoxicity LDH Assay Kit were purchased from Dojindo (Kumamoto, Japan). Rabbit anti-rat antibodies against STIM1, PLCγ1, p-PLCγ1, GAPDH, β-actin were purchased from Santa Cruz Biotechnology (Dallas, TX, USA); Orai1, HMGB1, PKCα, CaMKIV, Histone H3 were purchased from Abcam. Goat anti-rabbit horseradish peroxidase-conjugated secondary antibody was purchased from Shanghai Excell Biotechnology Co., Ltd (Shanghai, China). The BCA protein assay kit, SDS-PAGE and Protein A agarose were purchased from (Shanghai, China). Enhanced chemiluminescence detection system was purchased from Millipore (Billerica, MA, USA). The HMGB1 enzyme-linked immunosorbent assay (ELISA) kit was purchased from Chondrex (Redmond, WA, USA). Nuclear and cytoplasmic extraction reagents was purchased from Shanghai Yisheng Biotechnology Co., Ltd (Shanghai, China).
Cellular culture and treatment
BNL.Cl2 cells were cultured in DMEM medium supplemented with 10% FBS, 1% penicillin and streptomycin at 37°C with 5% CO2, and the culture media were changed once every 2 days. At 80–90% confluence, cells were treated with various agents in medium with 2% FBS. For H2O2 treatment, cells were incubated with 100 μM, 500 μM or 1 mM H2O2 for 1, 2, 3 or 4 h. For NAC treatment, cells were pre-treated with 100 μg/ml NAC for 24 h. For inhibition experiments, the cells were pre-treated with 50 μM 2-APB or 10 μM U73122 for 24 h and then co-treated with 500 μM H2O2 for 3 h. For RNAi experiments, cells were transfected with NC-siRNA or STIM1-siRNA. For A23187 treatment, cells were treated with 10, 25 or 50 μM A23187 for 30 min; then, the medium was replaced with new DMEM with 2% FBS for 12, 24 or 48 h. Cells were co-treated with 25 μM A23187 and EGTA (25 μM) for 30 min. For 58-F administration, the cells were pre-treated with 58-F at 10, 50 or 100 μM for 24, 48 or 72 h and then exposed to 500 μM H2O2 for 3 h.
Measurement of intracellular Ca2+ concentration
Intracellular Ca2+ was monitored using the Ca2+-sensitive fluorescent indicator-Fluo-4/AM by confocal laser scanning microscopy. The cells were cultured in confocal dishes (105 cells/dish), then loaded with Fluo-4/AM (5 μM) and F127 (0.4%) at 37 °C for 30 min in darkness with modified Hank’s Buffered Salt Solution (HBSS) containing 25 mM Hepes, 150 mM NaCl, 5 mM KCl, 2 mM CaCl2, 0.4 mM MgCl2 and 25 mM d-glucose (pH 7.4). They were rinsed twice in HBSS and kept at room temperature for 10 min to allow the de-esterification of Fluo-4/AM. Then, cells were maintained in D-Hanks (Ca2+-free) buffer for 10 min before Ca2+ imaging. The green fluorescence of Fluo-4/AM was excited by an argon laser at 488 nm, and the emitted fluorescence was recorded through a 525 nm channel. The image was recorded every 10 s. For imaging with Fluo-4/AM, [Ca2+]i changes are presented as F/F0 ratios after background subtraction, where F was the change in fluorescence signal intensity, and F0 was the baseline before stimulus application.
LDH cytotoxicity assay
LDH release, which could reflect cell membrane integrity, was detected with an assay kit (Dojindo) according to the manufacturer’s instructions. Briefly, cells were cultured in 96-well microplates (7×103 cells/well) for 24 h in a CO2 incubator and then incubated with different treatments. First, 10 μl of Lysis Buffer was added to the well to induce maximum LDH release. After 30 min in a CO2 incubator, 100 μl of Working Solution was added into each well, and the plates were incubated in darkness at room temperature for 30 min. Subsequently, 50 μl of Stop Solution was added to each well, and the absorbance was measured at 490 nm using a microplate reader. The calculation was as follows: LDH release (%)=[A-C/B-C]×100%, where A is the absorbance of treated samples, and B and C are the absorbance of the maximum and the minimum, respectively.
ELISA assay
The cell culture medium was collected and used to measure HMGB1 levels by ELISA kits according to the manufacturer’s suggested protocol. Absorbance at 450 nm was measured using a microplate reader.
Preparation of cell extracts
Nuclear and cytosolic extracts were prepared using nuclear and cytoplasmic extraction reagents, according to the manufacturer’s instructions. The total protein extract was lysed in RIPA buffer and phenylmethylsulfonyl fluoride. The protein concentrations were determined by bicinchoninic acid assay.
Western blot analysis
Equal amounts of total cellular protein (20 μg per sample) were separated by SDS-PAGE and transferred to PVDF membranes that were blocked with 5% non-fat milk for 2 h and incubated with the primary antibodies overnight at 4 °C. The primary antibodies (diluted at 1 : 1000) used were as follows: anti-STIM1, anti-Orai1, anti-PLCγ1, anti-p-PLCγ1, anti-HMGB1, anti-PKCα, anti-CaMKIV anti-GAPDH, anti-β-actin, and anti-Histone H3 (1 : 500). The membranes were then washed three times (10 min/wash) with TBST and incubated with a 1 : 3000 dilution of goat anti-rabbit horseradish peroxidase-conjugated secondary antibody for 1 h at room temperature. After the final wash, the immunoreactive bands were detected on Fluor Chem E (Protein Simple) by enhanced chemiluminescence. The densities of bands were analysed using ImageJ software and expressed as ratios to β-actin or GAPDH or Histone H3.
Immunoprecipitation
A total of 500 μg of nuclear extract was incubated with 2 μg of anti-HMGB1 at 4 °C overnight on a rotator. Next, 30 μl of Protein A Agarose was spun briefly in a microcentrifuge at 500 g for 30 s and washed three times in PBS, then resuspended in 200 μl of PBS. A 40 μl slurry of Protein A agarose was added to each sample, followed by incubation for an additional 3 h at 4 °C on a rotator. The samples were spun briefly in a microcentrifuge at 500 g for 2 min and washed three times in PBS. Finally, the samples were resuspended in 40 μl of loading buffer for future analysis.
RNAi
We utilized the Smartpool siRNA from Dharmacon (Lafayette, CO, USA) that consists of four separate siRNA sequences against STIM1: GCGACTTCTGAAGAGTCTACC, GCTGCTGGTTTGCCTATATCC, GCGGTTTCCAGATTGTCAATA and GGATTTGACCCATTCCGATTC, and a control siRNA NC: TTCTCCGAACGTGTCACGT. The LV3(H1/RFG&Puro)-STIM1 and NC constructs were constructed and identified by Shanghai UsenLab Biotechnology Co., Ltd. (Shanghai, China). Cells were plated in a six-well plate or confocal dish in 10% DMEM without antibiotics, resulting in 80% confluence before transfection. In separate tubes, 1.5 μg of each plasmid was diluted in 250 μl serum-free DMEM. Each solution was combined with 5 μl of Lipofectamine 2000 and mixed gently, and the final transfection mixture was incubated for 20 min at room temperature. The cells were transfected with STIM1-siRNA or NC-siRNA according to the manufacturer’s protocol (Invitrogen, Carlsbad, CA, USA). Transfection efficiency was determined at 24 h by fluorescence microscopy, and mRNA and protein expression levels were measured 48 h after transfection.
Statistical analysis
Experiments were carried out in triplicate, and statistical analysis was performed using SPSS software. Significance between two groups was assessed using the paired or non-paired Student’s t-test (t-test), and significance among multiple groups was assessed using a one-factor analysis of variance (ANOVA) with the Dunnett’s post hoc test. P<0.05 was considered as a statistically significant difference.
References
Amcheslavsky A, Wood ML, Yeromin AV, Parker I, Freites JA, Tobias DJ et al. Molecular biophysics of Orai store-operated Ca2+ channels. Biophys J 2015; 108: 237–246.
Criddle DN . Reactive oxygen species, Ca2+ stores and acute pancreatitis; a step closer to therapy? Cell Calcium 2016; 60: 180–189.
Bhosale G, Sharpe JA, Sundier SY, Duchen MR . Calcium signaling as a mediator of cell energy demand and a trigger to cell death. Ann NY Acad Sci 2015; 1350: 107–116.
Irvine RF . 20 years of Ins(1,4,5)P3, and 40 years before. Nat Rev Mol Cell Biol 2003; 4: 580–585.
Tu C-L, Chang W, Bikle DD . Phospholipase Cγ1 is required for activation of store-operated channels in human keratinocytes. J Invest Dermatol 2005; 124: 187–197.
Prakriya M, Lewis RS . Store-operated calcium channels. Physiol Rev 2015; 95: 1383–1436.
Soboloff J, Rothberg BS, Madesh M, Gill DL . STIM proteins: dynamic calcium signal transducers. Nat Rev Mol Cell Biol 2012; 13: 549–565.
Lewis RS . The molecular choreography of a store-operated calcium channel. Nature 2007; 446: 284–287.
Parekh AB, Penner R . Store depletion and calcium influx. Physiol Rev 1997; 77: 901.
Rosado JA, Diez R, Smani T, Jardín I . STIM and Orai1 variants in store-operated calcium entry. Front Pharmacol 2015; 6: 325.
Lewis RS . Store-operated calcium channels: new perspectives on mechanism and function. Cold Spring Harb Perspect Biol 2011; 3: a003970.
Wu MM, Covington ED, Lewis RS . Single-molecule analysis of diffusion and trapping of STIM1 and Orai1 at endoplasmic reticulum–plasma membrane junctions. Mol Biol Cell 2014; 25: 3672–3685.
Aromataris EC, Castro J, Rychkov GY, Barritt GJ . Store-operated Ca2+ channels and stromal interaction molecule 1 (STIM1) are targets for the actions of bile acids on liver cells. Biochim Biophys Acta 2008; 1783: 874–885.
Litjens T, Harland ML, Roberts ML, Barritt GJ, Rychkov GY . Fast Ca(2+)-dependent inactivation of the store-operated Ca(2+) current (I(SOC)) in liver cells: a role for calmodulin. J Physiol 2004; 558 (Pt 1): 85–97.
Rychkov GY, Litjens T, Roberts ML, Barritt GJ . ATP and vasopressin activate a single type of store-operated Ca2+ channel, identified by patch-clamp recording, in rat hepatocytes. Cell Calcium 2005; 37: 183–191.
Palee S, Apaijai N, Shinlapawittayatorn K, Chattipakorn SC, Chattipakorn N . Acetylcholine attenuates hydrogen peroxide-induced intracellular calcium dyshomeostasis through both muscarinic and nicotinic receptors in cardiomyocytes. Cell Physiol Biochem 2016; 39: 341–349.
Suresh K, Servinsky L, Reyes J, Baksh S, Undem C, Caterina M et al. Hydrogen peroxide-induced calcium influx in lung microvascular endothelial cells involves TRPV4. Am J Physiol 2015; 309: L1467.
Uğuz AC, Öz A, Nazıroğlu M . Curcumin inhibits apoptosis by regulating intracellular calcium release, reactive oxygen species and mitochondrial depolarization levels in SH-SY5Y neuronal cells. J Recept Signal Transduct Res 2016; 36: 395–401.
Kim MJ, Kim E, Ryu SH, Suh P-G . The mechanism of phospholipase C-[gamma]1 regulation. Exp Mol Med 2000; 32: 101–109.
Bai X-C, Deng F, Liu A-L, Zou Z-P, Wang Y, Ke Z-Y et al. Phospholipase C-gamma1 is required for cell survival in oxidative stress by protein kinase C. Biochem J 2002; 363 (Pt 2): 395–401.
González-Pacheco FR, Caramelo C, Castilla MÁ, Deudero JJP, Arias J, Yagüe S et al. Mechanism of vascular smooth muscle cells activation by hydrogen peroxide: role of phospholipase C gamma. Nephrol Dial Transplant 2002; 17: 392–398.
Lu B, Wang C, Wang M, Li W, Chen F, Tracey KJ et al. Molecular mechanism and therapeutic modulation of HMGB1 release and action: an updated review. Expert Rev Clin Immunol 2014; 10: 713–727.
Scaffidi P, Misteli T, Bianchi ME . Release of chromatin protein HMGB1 by necrotic cells triggers inflammation. Nature 2002; 418: 191–195.
Chen R, Hou W, Zhang Q, Kang R, Fan X-G, Tang D . Emerging role of High-Mobility Group Box 1 (HMGB1) in liver diseases. Mol Med 2013; 19: 357–366.
Youn JH, Shin J-S . Nucleocytoplasmic shuttling of HMGB1 is regulated by phosphorylation that redirects it toward secretion. J Immunol 2006; 177: 7889–7897.
Oh YJ, Youn JH, Ji Y, Lee SE, Lim KJ, Choi JE et al. HMGB1 is phosphorylated by classical protein kinase C and is secreted by a calcium-dependent mechanism. J Immunol 2009; 182: 5800–5809.
Zhang X, Wheeler D, Tang Y, Guo L, Shapiro RA, Ribar TJ et al. Calcium/calmodulin-dependent protein kinase (CaMK) IV mediates nucleocytoplasmic shuttling and release of HMGB1 during lipopolysaccharide stimulation of macrophages. J Immunol 2008; 181: 5015–5023.
Tsung A, Klune JR, Zhang X, Jeyabalan G, Cao Z, Peng X et al. HMGB1 release induced by liver ischemia involves Toll-like receptor 4–dependent reactive oxygen species production and calcium-mediated signaling. J Exp Med 2007; 204: 2913–2923.
Ito M, Sato-Masumoto N, Kobayashi F, Matsumura K . Distinguishing Ophiopogon and Liriope tubers based on DNA sequences. J Nat Med 2015; 69: 555–564.
Evankovich J, Cho SW, Zhang R, Cardinal J, Dhupar R, Zhang L et al. High Mobility Group Box 1 release from hepatocytes during ischemia and reperfusion injury is mediated by decreased histone deacetylase activity. J Biol Chem 2010; 285: 39888–39897.
Ge L-L, Kan L-D, Zhuge Z-B, Ma KE, Chen S-Q . Ophiopogon japonicus strains from different cultivation regions exhibit markedly different properties on cytotoxicity, pregnane X receptor activation and cytochrome P450 3A4 induction. Biomed Rep 2015; 3: 430–434.
Yan X, Ye T, Hu X, Zhao P, Wang X . 58-F, a flavanone from Ophiopogon japonicus, prevents hepatocyte death by decreasing lysosomal membrane permeability. Sci Rep 2016; 6: 27875.
Zhao P, Yan X, Wang X . H_2O_2 induced hepatocyte apoptosis by intracellular calcium homeostasis. Chin J Cell Biol 2015; 37: 1257–1262.
Ma L, Kim S-J, Oh KI . Calcium/calmodulin-dependent protein kinase is involved in the release of High Mobility Group Box 1 via the interferon-β signaling pathway. Immune Netw 2012; 12: 148–154.
Barritt GJ, Litjens TL, Castro J, Aromataris E, Rychkov GY . Store-operated Ca2+ channels and microdomains of Ca2+ in liver cells. Clin Exp Pharmacol Physiol 2009; 36: 77–83.
Rooney TA, Sass EJ, Thomas AP . Characterization of cytosolic calcium oscillations induced by phenylephrine and vasopressin in single fura-2-loaded hepatocytes. J Biol Chem 1989; 264: 17131–17141.
Sato H, Takeo T, Liu Q, Nakano K, Osanai T, Suga S et al. Hydrogen peroxide mobilizes Ca(2+) through two distinct mechanisms in rat hepatocytes. Acta Pharmacol Sin 2009; 30: 78–89.
Hong JH, Moon SJ, Byun HM, Kim MS, Jo H, Bae YS et al. Critical role of phospholipase Cγ1 in the generation of H2O2-evoked [Ca2+]i oscillations in cultured rat cortical astrocytes. J Biol Chem 2006; 281: 13057–13067.
Varela D, Simon F, Olivero P, Armisén R, Leiva-Salcedo E, Jørgensen F et al. Activation of H2O2-induced VSOR Cl- currents in HTC cells require phospholipase Cγ1 phosphorylation and Ca2+ mobilisation. Cell Physiol Biochem 2007; 20: 773–780.
Salido GM, Sage SO, Rosado JA . Biochemical and functional properties of the store-operated Ca2+ channels. Cell Signal 2009; 21: 457–461.
Barritt GJ, Chen J, Rychkov GY . Ca(2+) -permeable channels in the hepatocyte plasma membrane and their roles in hepatocyte physiology. Biochim Biophys Acta 2008; 1783: 651–672.
Vénéreau E, Ceriotti C, Bianchi ME . DAMPs from cell death to new life. Front Immunol 2015; 6: 422.
Oh YJ, Youn JH, Ji Y, Lee SE, Lim KJ, Choi JE et al. HMGB1 is phosphorylated by classical protein kinase C and is secreted by a calcium-dependent mechanism. J Immunol 2009; 182: 5800–5809.
Wan W, Cao L, Khanabdali R, Kalionis B, Tai X, Xia S . The emerging role of HMGB1 in neuropathic pain: a potential therapeutic target for neuroinflammation. J Immunol Res 2016; 2016: 6430423.
Acknowledgements
This work was supported by National Natural Science Funds of China (No. 81503367) and the Budget Research Project of Shanghai Education Commission (No. 2014YSN22).
Author information
Authors and Affiliations
Contributions
PZ: conception and design, collection and assembly of data, interpretation and manuscript writing. TY: collection and assembly of data. XY: collection and assembly of data. PL: conception and design. XW: conception and design, financial support, collection and assembly of data, data analysis and interpretation, manuscript writing and final approval of manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Edited by N Barlev
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Zhao, P., Ye, T., Yan, X. et al. HMGB1 release by H2O2-induced hepatocytes is regulated through calcium overload and 58-F interference. Cell Death Discov. 3, 17008 (2017). https://doi.org/10.1038/cddiscovery.2017.8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/cddiscovery.2017.8
This article is cited by
-
Pregabalin mitigates microglial activation and neuronal injury by inhibiting HMGB1 signaling pathway in radiation-induced brain injury
Journal of Neuroinflammation (2022)
-
The mechanism of HMGB1 secretion and release
Experimental & Molecular Medicine (2022)
-
Liver regeneration and inflammation: from fundamental science to clinical applications
Nature Reviews Molecular Cell Biology (2021)