Abstract
Transfer of type-1 helper T-conditioned (Th1-conditioned) cells promotes functional recovery with enhanced axonal remodeling after spinal cord injury (SCI). This study explored the molecular mechanisms underlying the beneficial effects of pro-inflammatory Th1-conditioned cells after SCI. The effect of Th1-conditioned cells from interferon-γ (ifn-γ) knockout mice (ifn-γ−/− Th1 cells) on the recovery after SCI was reduced. Transfer of Th1-conditioned cells led to the activation of microglia (MG) and macrophages (MΦs), with interleukin 10 (IL-10) upregulation. This upregulation of IL-10 was reduced when ifn-γ−/− Th1 cells were transferred. Intrathecal neutralization of IL-10 in the spinal cord attenuated the effects of Th1-conditioned cells. Further, IL-10 is robustly secreted from Th1-conditioned cells in an ifn-γ-dependent manner. Th1-conditioned cells from interleukin 10 knockout (il-10−/−) mice had no effects on recovery from SCI. These findings demonstrate that ifn-γ-dependent secretion of IL-10 from Th1 cells, as well as native MG/MΦs, is required for the promotion of motor recovery after SCI.
Similar content being viewed by others
Main
In mammals, once the central nervous system (CNS) is injured, in contrast to peripheral nervous system, neural regeneration and functional recovery are very limited.1 Until recently, immune reactions have been considered detrimental after CNS injuries. For example, infiltrating macrophages (MΦs) and resident microglia (MG) are considered deleterious to recovery after CNS injuries2, 3, 4 and T cells are pathogenic in the injured CNS.4, 5, 6 Hence, massive dose of glucocorticoid has been infused to patients after spinal cord injury (SCI) to attenuate immune reactions in the CNS, although there are no convincing evidences that prove significant efficacy of the treatment. However, in some conditions, T cells are beneficial for repair of the injured CNS, although this notion remains controversial.4, 7, 8, 9 These contradictory findings regarding the role of T cells after CNS injuries could be explained by differences in the subsets of helper T cells. In support of this hypothesis, a previous study demonstrated that adoptive transfer of interferon-γ (IFN-γ)-producing type-1 helper T-conditioned (Th1-conditioned) cells promote functional recovery after SCI in mice.10 Enhanced axonal remodeling of corticospinal tract (CST) and serotonergic fibers are also observed in mice that undergo Th1-cell transfer. Although type-2 helper cells (Th2 cells) are considered neuroprotective in some situations,11, 12 this previous study did not demonstrate enhanced recovery from SCI after transfer of Th2-conditioned cells.10 Furthermore, transfer of IL-17-producing helper T (Th17) cells, pathogenic in multiple sclerosis (MS) and in an animal model of MS,13 limits recovery in the acute phase after SCI.10 Importantly, upregulation of the anti-inflammatory/neuroprotective M2 subtype of MG/MΦs was observed in the injured spinal cord after transfer of Th1 cells that had previously been considered to be involved in the onset and progression of autoimmune diseases such as MS.14, 15 In the current study, we explored the mechanism underlying the restorative effects of transferred Th1 cells after SCI in mice.
Results
Therapeutic effects of Th1 cells after SCI depend on IFN-γ
The objective of this study was to explore the mechanism behind the effects of adoptively transferred Th1-conditioned cells on the functional recovery after SCI. We first assessed whether IFN-γ, a major cytokine secreted by Th1 cells,16 was required for the effects. We isolated cluster of differentiation 4 (CD4)+ T cells from spleens of wild-type (WT) and interferon-γ (ifn-γ)-knockout (ifn-γ−/−) mice. The cells were then cultured with IL-2/IL-12 and anti-IL-4 neutralizing antibody to induce differentiation into Th1 cells. We confirmed with enzyme-linked immunosorbent assay (ELISA) that IFN-γ secretion from Th1 ifn-γ−/− cells was totally abrogated compared with WT Th1 cells and Th17 cells (Figure 1a). In addition, abundant expression of T-bet, a T-box transcription factor of the Th1 master gene,17 was observed in cultured WT Th1-conditioned cells by flow cytometry (Figure 1b). T-bet in ifn-γ−/− Th1-conditioned cells was expressed at an intermediate level between Th0 and Th1 cells (Figure 1b).
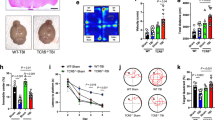
Improved recovery induced by Th1 cells after SCI depends on IFN-γ. Enhanced recovery from SCI by Th1 transfer is dependent on interferon-γ (ifn-γ) in transferred Th1 cells. (a) Level of IFN-γ secreted from Th1 cells, Th1 ifn-γ−/− cells, and Th17 cells, which was detected by ELISA(n=3). (b) Comparison of T-bet production in helper T cells differentiated ex vivo, which was assessed by flow cytometry histogram. Representative data from three independent experiments. (c) Time course of hindlimb locomotion using the BMS with adoptive transfer of 1.0 × 107 each helper T-cell subsets (PBS, n=7; Th1 n=7; Th1 ifn-γ−/−, n=5). (d) Time course of the grid-walk test (PBS, n=4; Th1, n=6; Th1 ifn-γ−/−, n=4). Data are presented as mean±S.E.M. *P<0.05, ***P<0.001 versus the PBS group, #P<0.05 versus Th1 group (two-way ANOVA with repeated measures, Bonferroni post-test)
Mouse vertebrae were laminectomized and the exposed spinal cords were contused at the level between thoracic vertebrae 9 (T9) and 10 (T10) by an impactor with a force of 60 kdyn. On the first day after contusion, the hindlimbs of all mice were completely paraplegic and gradually displayed partial recovery of motor function after day 1. At 4 days after contusion SCI, 1.0 × 107 WT and ifn-γ−/− Th1-conditioned cells were transferred intraperitoneally (i.p.) into the mice and recovery of motor function was assessed using the Basso Mouse Scale (BMS).18 Enhanced motor recovery was observed in mice that received Th1 ifn-γ−/− cell transfer compared with control mice, but the extent of the improvement was less than that observed in mice receiving a transfer of WT Th1-conditioned cells (Figure 1c).
Consistent results were obtained when the grid-walk test was performed, which assesses voluntary movement control mediated by the corticospinal and the rubrospinal systems.19 Transfer of Th1 ifn-γ−/− cells led to a significantly greater frequency of hindlimb dropping (mistakes) compared with that of WT Th1 cells (Figure 1d). Thus, IFN-γ in Th1-conditioned cells contributes to improved functional recovery.
ifn-γ-dependent activation of MG by adoptive transfer of Th1-conditioned cells
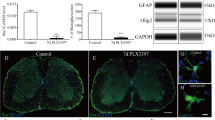
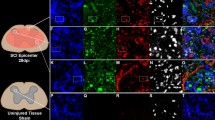
Previous observations with flow cytometry after SCI showed that transfer of Th1-conditioned cells led to an increase in MG/MΦs and to upregulation of the neuroprotective M2 subtype: CD206+ cells among the MΦs and arginase 1+(Arg1) cells among the MG.10 Morphological analysis by immunohistochemistry for ionized calcium-binding adapter molecule 1 (Iba1) in the contused spinal cord revealed that with Th1 transfer, MG/MΦs increased, enlarged, and were more round compared with those in control mice (Figures 2a and b). This observation is consistent with the previous data that showed both activation of MG/MΦs with CD11b and CD45 immunoreactivity using flow cytometry and upregulation of the M2 subtype, which has characteristics including anti-inflammatory effects, phagocytic behavior, and a round shape compared with the pro-inflammatory, destructive, and ramified M1 subtype.10 MG/MΦs were assessed quantitatively using flow cytometry20 and microglial activation by Th1-cell transfer after SCI was shown to depend on IFN-γ (Figures 2c and d).
Microglial activation induced by Th1-cell transfer depends on IFN-γ. Adoptive transfer of Th1-conditioned cells after SCI leads to activation of MG/MΦs at the injured site, and microglial activation is dependent on ifn-γ in transferred Th1 cells. (a) Immunohistochemistry for MG/MΦs labeled with anti-Iba1 antibody. Spinal cords removed on day 10 after SCI were cut transversely. The section at 0 mm corresponds to the epicenter of the contusion and the distance shown is caudal from the epicenter. Scale bar, 500 μm. (b) Higher magnification views of (a). Scale bar, 100 μm. (c) Representative flow cytometry profile of MG/MΦs that accumulated in the spinal cord on SCI day 6, 2 days after the injection of PBS or cultured T cells. Upper dot plots indicate the side-scatter/forward-scatter profile by which CD11b/CD45 profiles were gated. In lower dot plots, CD11b intermediate CD45 intermediate corresponds to MG, whereas CD11b high CD45 high corresponds to MΦs. The leftmost dot plots indicate a profile using isotype-matched immunoglobulins as a control. (d) The number of MG or MΦs that accumulated in the spinal cord on day 6 after SCI, 2 days after the injection of PBS or Th1-conditioned cells. PBS, n=3; Th1, n=4; Th1 ifn-γ−/−, n=3. Leukocytes isolated from the spinal cords of two to four mice were analyzed in each experiment. *P<0.05 (one-way ANOVA with Bonferroni post-test)
IL-10 produced from MG/MΦs contributes to repair after SCI
It was hypothesized that some molecules secreted from MG/MΦs have a role in the enhanced functional recovery induced by Th1-cell transfer after SCI. Intracellular cytokine staining of MG/MΦs indicated that interleukin 10 (IL-10), which is considered to be cerebroprotective after an ischemic stroke21 and is one of the M2 anti-inflammatory markers,22 was upregulated in MG/MΦs in the spinal cord after transfer of Th1-conditioned cells (Figure 3a). This upregulation was reduced if Th1 ifn-γ−/− cells were adoptively transferred (Figure 3a), demonstrating that IFN-γ secreted from Th1-conditioned cells contributes to IL-10 production from MG/MΦs. We previously demonstrated that neutralization of IL-10 from Th1 cells attenuates the functional recovery initiated by the transfer of Th1 cells after SCI.10 However, it remains to be determined whether IL-10 secretion in the CNS after Th1 transfer has neuroprotective effects, because anti-IL-10-neutralizing antibody could block not only IL-10 secretion from transferred Th1 cells but also from native cells in the injured CNS, as shown in our previous experiment. To assess whether IL-10 produced by MG/MΦs in the CNS is required for the in vivo effects, anti-IL-10-neutralizing antibody or control IgG was injected into the cerebral ventricles (i.c.v.) using an osmotic pump catheterized to the right lateral ventricle for 7 days after SCI in mice. Th1-conditioned lymphocytes were injected i.p. to these mice on day 4 after SCI. Compared with treatment with control IgG, antibody infusion significantly suppressed motor recovery at time points later than 4 weeks after SCI, as assessed by BMS scoring (Figure 3b). Although there were no significant differences observed in the grid-walk test (Figure 3c), the ameliorated recovery of motor functions by Th1-cell transfer was attenuated in the inclined-plane test (Figure 3d). Therefore, IL-10 secreted from the cells in the CNS is a partial contributor to enhanced motor recovery after SCI.
Neutralization of IL-10 in the CNS attenuates functional recovery by Th1 cells transfer. IL-10 expressed in the CNS partially contributes to functional recovery after SCI with adoptive transfer of Th1-conditioned cells. (a) Upper histograms: comparison of IL-10 production from MG/MΦs evaluated using histograms of intracellular cytokine staining. The histogram is representative of four independent experiments. All histograms were gated from the populations of MG or MΦs as shown in Figure 2c. Lower graph: quantification of IL-10 production as indicated above. *P<0.05 versus the PBS group, #P<0.05 versus Th1 group (one-way ANOVA, Bonferroni post-test). (b–d) Functional recovery from SCI evaluated by: BMS scores (b), grid-walk test (c), and inclined-plane test (d) in Th1-conditioned cell-transferred SCI mice treated with control IgG or anti-IL-10 antibody into the cerebral ventricles (i.c.v.; control rat IgG+Th1, n=15; anti-IL-10+Th1, n=13 (BMS scores and inclined-plane test)/control IgG+Th1, n=9; anti-IL-10+Th1, n=8 (grid-walk test)). *P<0.05, **P<0.01 versus control IgG+Th1 group (two-way ANOVA with repeated measures, Bonferroni post-test)
ifn-γ-dependent secretion of IL-10 from Th1 cells have a pivotal role in improved recovery after SCI
We next performed in vitro experiments to confirm whether we can recapitulate IL-10 upregulation from MG and MΦs by Th1-conditioned lymphocytes. First, we cultured MG from neonatal mouse brains and mouse femoral bone-derived MΦs. Secretion of IL-10 was measured using ELISA after MG (Figure 4a), or MΦs (Figure 4b) cultured in 96-well plates were treated with conditioned media (CM) of Th1 cells, Th1 ifn-γ−/− cells, and Th17 cells or recombinant IFN-γ (Figure 4 upper schematic). Even at the starting point, high levels of IL-10 were observed in Th1-cell group (Figures 4a and b), demonstrating that CM of Th1 cells themselves contained abundant IL-10 compared with Th1 ifn-γ−/− cells and Th17 cells. Although IL-10 expression from MG/MΦs unexpectedly did not surge, IL-10 levels from MG or MΦs treated with CM of Th1 cells were significantly higher than only CM of Th1 cells at 3 h after the treatment (Figures 4a–c). It is suggested that comparatively small amounts of IL-10 were secreted from cultured MG/MΦs in the early phase after treatment of Th1 CM. As Th1 cells robustly secreted neuroprotective IL-10 (Figures 4a and b), we examined whether genetic deletion of il-10 in transferred Th1-conditioned cells decreased the effects of the Th1 cells in SCI mice. As a result, Th1 interleukin 10 knockout (il-10−/−) cells transfer completely diminished the ameliorative effects of Th1 cells transfer on hindlimb locomotion after SCI, as assessed by BMS scoring (Figure 4d).
In vitro assay for IL-10 detection in MG/MΦ culture and in vivo experiment using il-10-knockout mice. Neonatal mouse brain-derived MG or mouse femoral bone marrow-derived MΦs were cultured on 96-well plate. The MG or the MΦs were treated with the T-cell conditioned media (CM) or recombinant IFN-γ and, thereafter, IL-10 levels at different time points were measured by using ELISA (schematic drawn in an upper panel). IL-10 surge from MG/MΦs was not observed in the in vitro assay unlike in the injured spinal cord after Th1-cell transfer. However, Th1 cells secreted robust IL-10 in an ifn-γ-dependent manner, and this IL-10 secretion from Th1 cells had a pivotal role in improved recovery after SCI. (a) Time course of IL-10 level detected by ELISA in MG culture media after treatment with T-cell CM or IFN-γ (medium, n=4; Th1, n=4; Th1 w/o MG: Th1 cells without MG, n=4; Th1 ifn-γ−/−, n=3; IFN-γ (recombinant IFN-γ at 20 ng/ml), n=3; Th17, n=2). (b) Time course of IL-10 level detected by ELISA in macrophage (MΦ) culture media after treatment with T-cell CM or IFN-γ (medium, n=4; Th1, n=4; Th1 w/o microglia (MG): Th1 cells without MΦs, n=4; Th1 ifn-γ−/−, n=3; IFN-γ: recombinant IFN-γ at 20 ng/ml, n=3; Th17, n=2). (c) IL-10 level in MG or MΦ culture media at 3 h after treatment with T-cell CM or IFN-γ (MG: medium, n=4; Th1, n=4; Th1 cells without MG, n=4; Th1 ifn-γ−/−, n=3; IFN-γ: recombinant IFN-γ at 20 ng/ml, n=3; MΦs: medium, n=4; Th1, n=4; Th1 w/o MΦ: Th1 cells without MG, n=4; Th1 ifn-γ−/−, n=3; IFN-γ: recombinant IFN-γ at 20 ng/ml, n=3). **P<0.01, ***P<0.001 versus the medium group, ##P<0.01, ###P<0.001 versus Th1 group (one-way ANOVA, Bonferroni post-test). (d) BMS scores in Th1 or Th1 il-10−/−-transferred SCI mice (PBS, n=5; Th1, n=5; Th1 il-10−/−, n=6). *P<0.05, **P<0.01, ***P<0.001 versus the PBS group (two-way ANOVA with repeated measures, Bonferroni post-test)
Th1-conditioned lymphocytes secrete neurotrophic factors
Candidate neurotrophic factors in Th1-conditioned cells that promote neuroprotection were investigated after contusion SCI and the expression of neurotrophic factors, such as glia-derived neurotrophic factor (GDNF) and neurotrophin 3 (NT-3), in Th1-conditioned cells was shown to be higher than that in Th17 cells, which limited functional recovery after SCI.10 It has been shown that GDNF is neuroprotective after SCI23 and that NT-3 promotes growth and differentiation of neurons and synapses.24 In the current study, the expression levels of GDNF and NT-3 among Th1 cells, Th1 ifn-γ−/− cells, and Th17 cells were compared using ELISA. GDNF expression was higher in Th1 cells than that in Th1 ifn-γ−/− cells or Th17 cells (Figure 5a), although expression of NT-3 was not significantly different between Th1 cells and Th1 ifn-γ−/− cells (Figure 5b).
GDNF secretion from Th1 cells is dependent on IFN-γ. Expression of neurotrophic factors in cultured helper T cells. GDNF (a), and NT-3 (b) in the supernatant of Th1, Th1 ifn-γ−/−, and Th17 cells detected by ELISA (Th1, n=3; Th1 ifn-γ−/−, n=3; Th17, n=3). **P<0.01, ***P<0.001; NS, not significant (one-way ANOVA with Bonferroni post-test)
Discussion
The current study demonstrated that ifn-γ-dependent secretion of IL-10 from Th1 cells as well as from MG/MΦs is required for the enhanced recovery from SCI induced by Th1 transfer (Figure 6). It is surprising that expression of the neuroprotective cytokine IL-10 is upregulated from MG/MΦs in an ifn-γ-dependent manner (Figure 3a), although pro-inflammatory Th1 cells were transferred after SCI. However, effects of these cytokines especially IL-10 upregulation in the CNS are partial (Figures 3b and d). Th1 cell-transferred spinal cord after SCI showed accumulation of activated round MG and MΦs around the injured dorsal and lateral CST, although activated and ramified MG/MΦs are also observed without treatment after SCI (Figures 2a and b). It is suggested that the increased proportion of neuroprotective M2 MG/MΦs induced by Th1 cells transfer10 may protect and repair injured neuronal fibers, including the CST. To elucidate the progression of IFN-γ from Th1 cells leading to IL-10 upregulation in MG/MΦs, we treated cultured MG/MΦs with Th1 CM or recombinant IFN-γ and measured IL-10 levels (Figures 4a–c). The result suggests that Th1 cells themselves secrete abundant IL-10 and, comparatively, an unexpectedly small amount of IL-10 was secreted from MG/MΦs when treated with Th1 CM. It is possible that the cell state of the cultured MG/MΦs in our system may be different from in vivo MG/MΦs after SCI (Figure 3a) and that other micro-environmental factors, such as astrocyte activity, may be required to robustly elevate IL-10 secretion from MG/MΦs. Whereas experiments neutralizing IL-10 in the CNS only attenuated the effects of Th1-conditioned cells transfer (Figures 3b and d), transfer of Th1-conditioned cells derived from il-10−/− mice showed complete abrogation of the restorative effects of Th1 cells (Figure 4d). Thus, ifn-γ-dependent secretion of IL-10 from transferred Th1 cells (Figures 4a and b) may contribute to the entirety of the effects by directly shifting the CNS into a neuroprotective state25 in addition to increasing the proportion of the neuroprotective M2 subtype of MG/MΦs observed and upregulation of Arg1, CD206,10 and IL-10 (Figure 6). Indeed, transfer of Th1-conditioned cells has enhanced restorative effects compared with just inducing viral expression of IL-10 in the CNS after SCI.25 This may be caused by shifting systems in the periphery, such as MΦs in the lymph nodes into a neuroprotective state, as well as the CNS with Th1-cell transfer. On the other hand, IFN-γ did not have direct effects on IL-10 upregulation from MG/MΦs (Figures 4a–c). We conclude that ifn-γ is required to maintain transferred Th1 cells to abundantly secrete IL-10 rather than directly upregulating IL-10 from MG/MΦs in the lesion site after SCI. Our result is consistent with a report that ifn-γ mediates IL-10 reactivation by parasite-reactive Th1 cells.26 The notion may be consistent with our previous report that IFN-γ is necessary for maintaining Th1 cells to promote neurite outgrowth from cortical neurons rather than directly elongating neurites.27 On the other hand, other mechanism independent of ifn-γ may be partially responsible for IL-10 secretion from Th1 cells, because comparatively very small amounts of IL-10 were still secreted from Th1 ifnγ−/− cells (Figures 4a and b). This residual secretion of IL-10 may be attributed to ifn-γ-independent activation of signal transducer and activator of transcription 4, as previously reported.28
Schematic representation showing molecular mechanism of restorative effects of transferred Th1-conditioned lymphocytes on recovery after SCI. ifn-γ-dependent secretion of IL-10 from transferred Th1-conditioned cells contributes to an increase of M2 subtype of MG/MΦs, as shown by the upregulation of IL-10, arginase 1 (Arg1), and CD206, leading to restorative effects on functional recovery after SCI
In general, inflammation is considered to be detrimental to the CNS injury, but there are some reports demonstrating that pro-inflammatory T cells are beneficial to the CNS injury. Those T cells may be attributed to the functions of Th1 cells in ifn-γ-dependent manner. Indeed, IFN-γ promotes neuronal differentiation29 and neurogenesis.30 Secretion of IFN-γ by the transferred Th1-conditioned cells has a role in MG activation (Figures 2c and d), leading to functional recovery from SCI. It has been suggested that activated MG induce neuronal differentiation31 and are neuroprotective.22 In addition, the beneficial role of MΦs in the injured CNS is known.32, 33
IFN-γ contributes to the upregulation of GDNF in Th1 cells (Figure 5a), which may have positive effects on neuroprotection after SCI. Thus, the in vivo effects of IFN-γ secreted by Th1-conditioned cells are important for functional recovery after SCI. However, it should be noted that Th1-conditioned cells lacking IFN-γ still had limited beneficial effects (Figures 1c and d). These remnant effects may be mediated by neuroprotective IL-10 (Figures 4a and b) and trophic factors, such as NT-3 (Figure 5b).
Taken together, pro-inflammatory Th1 cells have restorative effects on functional recovery after SCI in ifn-γ- and il-10-dependent manner. There are many side effects after massive dose of glucocorticoid treatment such as increased susceptibility to infection, gastroinstestinal ulcer, diabetes mellitus, and mental disorder. Therefore, our study provides new insights into future immunomodulatory treatment after CNS trauma (for example, transfer of Th1 cells or skewing to Th1), which not only promotes beneficial immune reactions but also attenuates harmful ones such as devastating Th17 cells.
Materials and Methods
Mice
C57BL/6j mice were purchased from Charles River Laboratories (Wilmington, MA, USA). As previously reported, ifn-γ−/− mice34 and il-10−/− mice35 on the C57BL/6 background were used. All mice used in this study were housed in specific pathogen-free conditions and were treated and cared for in accordance with the guidelines of Osaka University pertaining to the treatment of experimental animals.
Animal model of SCI
Adult (7–9 weeks old) female C57BL/6 mice were anesthetized with sodium pentobarbital (50 mg/kg; Kyoritsu Seiyaku, Tokyo, Japan). Following dorsal laminectomy (at the T9–T10 level), the spinal cord was contused with a force of 60 kdyn using an Infinite Horizon Impactor (Precision Systems & Instrumentation, Fairfax Station, VA, USA), as previously described.36 The muscle and skin layers were then sutured. The bladder was expressed daily using manual abdominal pressure until 10 days after injury. Food and water were provided ad libitum.
Adoptive transfer of cultured T cells
The procedure was performed according to a previously described procedure.10 The procedure is briefly indicated as following: spleens were collected from the mice. CD4+ T cells were isolated using magnet sorting with anti-CD4 magnet beads (Miltenyi Biotec, Cologne, Germany). CD4+ T cells were stimulated with anti-CD3-ɛ/anti-CD28 antibodies (5 μg/ml, respectively, eBioscience, San Diego, CA, USA) coated on 24-well plates (Greiner Bio-One, Kremsmünster, Austria). Th1-conditioned cells were differentiated by the addition of recombinant IL-2 (25 U/ml; R&D Systems/TECHNE, Minneapolis, MN, USA), IL-12 (10 U/ml; R&D systems), and anti-IL-4 antibodies (25% culture supernatant of hybridoma; clone HB-188; American Type Culture Collection, Manassas, VA, USA). Th17-conditioned cells were differentiated by the addition of recombinant IL-6 (20 ng/ml; R&D systems), IL-23 (20 ng/ml; R&D systems), TGF-β1 (3 ng/ml; R&D systems), anti-IL-4 antibodies (25% culture supernatant of the hybridoma), and anti-IFN-γ antibodies (1% culture supernatant of hybridoma; clone HB-170; American Type Culture Collection) in the presence of anti-IL-2 antibody (10 μg/ml; R&D Systems). Th0 cells were cultured in the presence of only IL-2 (25 U/ml; R&D Systems). On day 4, the helper T cells were collected. The cells were centrifuged at 1000 × g for 20 min with Lympholyte-M (Cedarlane Laboratories, Burlington, Ontario, Canada), and the intermediate layer was collected to eliminate the dead cells. The cells were restimulated for 3 h with anti-CD3-ɛ and anti-CD28 antibodies. On day 4 after SCI, helper T cells (1.0 × 107) suspended in 500 μl phosphate-buffered saline (PBS) were injected i.p. into mice. As a control, 500 μl PBS was injected into mice after SCI.
Behavioral analysis
Hindlimb motor function was evaluated using the BMS open-field locomotor test, in which scores range from 0 to 9.18 BMS scores were recorded on days 1, 3, and 7 after injury, and once weekly thereafter for a total of 6 weeks.
The grid-walk test was also performed to evaluate hindlimb locomotion.19 Deficits in descending motor control were examined by assessing the ability of mice to step on a square framework, 26 cm on a side, consisting of 1-cm2 grids made of round metal bars. Analysis was performed by counting the number of errors (that is, dropping the hindlimb from the grid) in 50 steps for each hindlimb. The mean percentage of errors was then calculated. Error percentages were not calculated before 2 weeks after SCI because, before this time, animals were unable to move their hindlimbs owing to insufficient recovery.
A subset of animals was analyzed using the inclined-plane test,10 which evaluates the animal’s ability to maintain body position on a board raised incrementally to increasing angles. Performance on the inclined plane correlates with the integrity of the rubrospinal tract (and other nonpyramidal pathways) after SCI. Animals were tested at days 1, 3, 7 after injury, and once weekly thereafter for a total of 6 weeks. Mice were tested in each position, after which the angle was increased incrementally by 5°. The maximum angle at which the animal could maintain a stationary position on the board for 10 s was recorded. Investigators were blinded to the treatment protocol and recorded behavioral scores.
Tissue preparation and histochemistry
For histochemistry, animals were perfused with 4% paraformaldehyde and preserved spinal cord tissues were collected. The entire spine was dissected out and post-fixed in 4% paraformaldehyde for 3 h at 4 °C. The spinal cord was removed from the vertebral column and stored for 12 h in 15% sucrose in 0.2 M PBS at 4 °C. The spinal cord was then placed in 30% sucrose in 0.2 M PBS for 24 h at 4 °C. The spinal cord was embedded in Tissue Tek OCT compound (Sakura, Tokyo, Japan) and immediately frozen on dry ice at −80 °C. A series of 20-μm transverse sections were cut on a cryostat and mounted on Matsunami Adhesive Silan-coated glass slides (Matsunami Glass, Osaka, Japan). After washing three times with PBS, all sections were blocked in PBS containing 5% BSA and 0.3% Triton X-100 for 1 h at room temperature. The sections were then incubated with polyclonal anti-Iba1 antibody (1 : 200; Wako, Osaka, Japan) overnight at 4 °C, washed three times with PBS, and incubated with fluorescein-conjugated secondary antibodies (1 : 500; Life Technologies, Carlsbad, CA, USA) for 1 h at room temperature. Sections were then rinsed three times in PBS and mounted. The sections were viewed under an inverted light microscope equipped with epifluorescence optics and a dry condenser for phase-contrast microscopy (DP70, Olympus, Tokyo, Japan).
Preparation of leukocytes from injured spinal cords
The extraction of leukocytes from the spinal cord was performed according to a previously described procedure.37 First, mice were transcardially perfused with ice-cold PBS. The spinal cord was then dissected and suspended in Hank’s Balanced Salt Solution (Life Technologies) supplemented with 3% fetal bovine serum (FBS), 100 IU/ml penicillin, and 100 μg/ml streptomycin. The spinal cords were digested with collagenase D (5.0 mg/ml; Roche Diagnostics, Tokyo, Japan) plus 2.5 mM calcium chloride. After filtration with a 70-μm Cell Strainer (BD Biosciences, Franklin Lakes, NJ, USA), lysis of red blood cells with RBC Lysis Buffer (BioLegend, San Diego, CA, USA) and washing, the pellet, isolated by 38% Percoll centrifugation at 1500 × g for 20 min, was collected for flow cytometry.
Cell-surface and intracellular antigen staining
Cultured lymphocytes or collected leukocytes from mouse spinal cords were stimulated with 50 ng/ml phorbol 12-myristate 13-acetate (Sigma-Aldrich, St. Louis, MO, USA) and 750 ng/ml ionomycin (Calbiochem/EMD Millipore, Billerica, MA, USA) for 4 h and with 10 μg/ml brefeldin A (Sigma-Aldrich) for the last 2 h. The cells were suspended in Fixation Buffer (eBioscience) and surface stained with anti-CD45-Alexa647 (BioLegend) and anti-CD11b-PE (BioLegend). Intracellular staining was performed according to the manufacturer’s protocol, using anti-T-bet-PE (eBioscience) and anti-IL-10-FITC (BioLegend).
Flow cytometric analysis
Flow cytometry was performed with the FACSCalibur flow cytometer (BD Biosciences), and was analyzed using ProQuest (BD Biosciences) and FlowJo software (TreeStar, Ashland, OR, USA). Control experiments using isotype-matched immunoglobulins (BioLegend) were performed to determine the specificity of the signals of antibodies against specific antigens.
Infusion i.c.v
Following SCI, the right lateral ventricle of the mouse was stereotaxically perforated with a brain infusion kit 3 (ALZET, DURET Corporation, Cupertino, CA, USA; coordinates: 0.5 mm posterior to the bregma, 1.0 mm lateral to the bregma, 2 mm deep) and connected to an osmotic minipump (ALZET; pump model: 1007D) filled with 1 mg/ml anti-IL-10-neutralizing antibody (eBioscience; clone: JES5-16E3) or rat IgG (eBioscience). The anti-IL-10 antibody was infused for 7 days.
Culture of MG/MΦs and treatment of T-cell culture media
Culture of MG and MΦs was performed according to a previously described procedure.38 MG were obtained from the brain of C57BL/6j mice on postnatal day 1–2. The cerebral cortex of each mouse was dissected out and the meninges were eliminated. The brains were minced with surgical knives, and then digested with 0.25% trypsin for 15 min and 0.5 mg/ml DNase for the last 1 min at 37 °C. The cells were passed through a 70-μm Cell Strainer (BD Biosciences). The resultant cell suspension was diluted with Dulbecco’s Modified Eagle Medium (DMEM; Life Technologies) and spun down. The pellet was suspended with 10% FBS/1% penicillin and streptomycin/DMEM (DMEM growth medium) and plated on poly-L-lysine-coated 75-cm3 culture flask (Greiner Bio-One). On day 1 and every 3 days thereafter, DMEM growth medium was replaced. After >7 days, the flask was shaken for 30 min so that floating MG could be collected from the astrocyte monolayer sheet and cultured at the density of 3.3 × 104 cells in 100 μl growth medium for 1 well of 96-well plate (Greiner Bio-One). More than 90% of the cells were CD11b+ MG.
Bone marrow-derived MΦs were obtained from bilateral femoral bones of 9-week-old C57BL6/j mice. Marrow cores were flushed using 10-ml syringes filled with RPMI1640 (Invitrogen)/10% FBS. After trituration and lysis of red blood cells with RBC Lysis Buffer (BioLegend), the cells were washed in the medium, and then plated and cultured in RPMI1640 with 10% FBS, penicillin/streptomycin (RPMI growth medium), and M-CSF (50 ng/ml; BioLegend). Non-adherent cells were collected at day 4. On day 6, the cells were replated on 96-well plates at the density of 3.3 × 104 cells in 100 μl of RPMI growth medium for one well. On day 7, the cells were treated with the T-cell supernatant. More than 90% of the cells were CD11b+ MΦs.
One hundred microliters of CM of cultured T cells (collected 4 days after T-cell culture) or 40 ng/ml IFN-γ (BioLegend) dissolved in 100 μl medium were applied to MG or MΦs cultured as above. At 0, 1, 3, 6, and 24 h after treatment of T-cell CM, supernatant of the cultured cells were collected to detect IL-10 with ELISA.
Enzyme-linked immunosorbent assay
Th1, Th1 ifn-γ−/−, and Th17 cells were prepared as described above. Three hours after restimulation with anti-CD3-ɛ/anti-CD28 antibodies, cells were centrifuged and their supernatants were collected and stored at −80 °C until use. Concentrations of IFN-γ, IL-10, NT-3, and GDNF in the supernatants of each cell were analyzed using the ELISA kits, according to the manufacturer’s protocol (IFN-γ and IL-10: R&D Systems; NT-3: Emax Immunoassay System; GDNF: Promega, Fitchburg, WI, USA). Absorbance values were read at 450 nm on a plate reader (SpectraMax M2; Molecular Devices, Sunnyvale, CA, USA).
Statistical analysis
All values are expressed as mean±S.E.M. Motor function scores were analyzed using two-way ANOVA with repeated measures with a Bonferroni post-test for 2–3 groups. For all other data, a one-way ANOVA with a Bonferroni post-test collection was used. Values of P<0.05 were considered statistically significant.
Abbreviations
- CNS:
-
central nervous system
- CST:
-
corticospinal tract
- SCI:
-
spinal cord injury
- IFN-γ:
-
interferon-γ
- IL-10:
-
interleukin 10
- Th1 cells:
-
type-1 helper T cells
- Th2 cells:
-
type-2 helper T cells
- Th17:
-
IL-17-producing helper T cells
- NT-3:
-
neurotrophin 3
- CD4:
-
cluster of differentiation 4
- PBS:
-
phosphate-buffered saline
- GDNF:
-
glia-derived neurotrophic factor
- ELISA:
-
enzyme-linked immunosorbent assay
References
David S, Aguayo AJ . Axonal elongation into peripheral nervous system ‘bridges’ after central nervous system injury in adult rats. Science 1981; 214: 931–933.
Bye N, Habgood MD, Callaway JK, Malakooti N, Potter A, Kossmann T et al. Transient neuroprotection by minocycline following traumatic brain injury is associated with attenuated microglial activation but no changes in cell apoptosis or neutrophil infiltration. Exp Neurol 2007; 204: 220–233.
Beck KD, Nguyen HX, Galvan MD, Salazar DL, Woodruff TM, Anderson AJ . Quantitative analysis of cellular inflammation after traumatic spinal cord injury: evidence for a multiphasic inflammatory response in the acute to chronic environment. Brain 2010; 133: 433–447.
Donnelly DJ, Popovich PG . Inflammation and its role in neuroprotection, axonal regeneration and functional recovery after spinal cord injury. Exp Neurol 2008; 209: 378–388.
Potas JR, Zheng Y, Moussa C, Venn M, Gorrie CA, Deng C et al. Augmented locomotor recovery after spinal cord injury in the athymic nude rat. J Neurotrauma 2006; 23: 660–673.
Shichita T, Sugiyama Y, Ooboshi H, Sugimori H, Nakagawa R, Takada I et al. Pivotal role of cerebral interleukin-17-producing gammadeltaT cells in the delayed phase of ischemic brain injury. Nat Med 2009; 15: 946–950.
Hofstetter HH, Sewell DL, Liu F, Sandor M, Forsthuber T, Lehmann PV et al. Autoreactive T cells promote post-traumatic healing in the central nervous system. J Neuroimmunol 2003; 134: 25–34.
Ziv Y, Ron N, Butovsky O, Landa G, Sudai E, Greenberg N et al. Immune cells contribute to the maintenance of neurogenesis and spatial learning abilities in adulthood. Nat Neurosci 2006; 9: 268–275.
Chiu IM, Chen A, Zheng Y, Kosaras B, Tsiftsoglou SA, Vartanian TK et al. T lymphocytes potentiate endogenous neuroprotective inflammation in a mouse model of ALS. Proc Natl Acad Sci USA 2008; 105: 17913–17918.
Ishii H, Jin X, Ueno M, Tanabe S, Kubo T, Serada S et al. Adoptive transfer of Th1-conditioned lymphocytes promotes axonal remodeling and functional recovery after spinal cord injury. Cell Death Dis 2012; 3: e363.
Hendrix S, Nitsch R . The role of T helper cells in neuroprotection and regeneration. J Neuroimmunol 2007; 184: 100–112.
Derecki NC, Cardani AN, Yang CH, Quinnies KM, Crihfield A, Lynch KR et al. Regulation of learning and memory by meningeal immunity: a key role for IL-4. J Exp Med 2010; 207: 1067–1080.
Kebir H, Kreymborg K, Ifergan I, Dodelet-Devillers A, Cayrol R, Bernard M et al. Human TH17 lymphocytes promote blood-brain barrier disruption and central nervous system inflammation. Nat Med 2007; 13: 1173–1175.
Hafler DA . Multiple sclerosis. J Clin Invest 2004; 113: 788–794.
Fransson ME, Liljenfeldt LS, Fagius J, Tötterman TH, Loskog AS . The T-cell pool is anergized in patients with multiple sclerosis in remission. Immunology 2009; 126: 92–101.
Hu X, Ivashkiv LB . Cross-regulation of signaling pathways by interferon-gamma: implications for immune responses and autoimmune diseases. Immunity 2009; 31: 539–550.
Mullen AC, High FA, Hutchins AS, Lee HW, Villarino AV, Livingston DM et al. Role of T-bet in commitment of TH1 cells before IL-12-dependent selection. Science 2001; 292: 1907–1910.
Basso DM, Fisher LC, Anderson AJ, Jakeman LB, McTigue DM, Popovich PG . Basso Mouse Scale for locomotion detects differences in recovery after spinal cord injury in five common mouse strains. J Neurotrauma 2006; 23: 635–659.
Metz GA, Merkler D, Dietz V, Schwab ME, Fouad K . Efficient testing of motor function in spinal cord injured rats. Brain Res 2000; 883: 165–177.
Ford AL, Goodsall AL, Hickey WF, Sedgwick JD . Normal adult ramified microglia separated from other central nervous system macrophages by flow cytometric sorting. Phenotypic differences defined and direct ex vivo antigen presentation to myelin basic protein-reactive CD4+ T cells compared. J Immunol 1995; 154: 4309–4321.
Liesz A, Suri-Payer E, Veltkamp C, Doerr H, Sommer C, Rivest S et al. Regulatory T cells are key cerebroprotective immunomodulators in acute experimental stroke. Nat Med 2009; 15: 192–199.
David S, Kroner A . Repertoire of microglial and macrophage responses after spinal cord injury. Nat Rev Neurosci 2011; 12: 388–399.
Iannotti C, Ping Zhang Y, Shields CB, Han Y, Burke DA, Xu XM . A neuroprotective role of glial cell line-derived neurotrophic factor following moderate spinal cord contusion injury. Exp Neurol 2004; 189: 317–332.
Ghosh A, Greenberg ME . Distinct roles for bFGF and NT-3 in the regulation of cortical neurogenesis. Neuron 1995; 15: 89–103.
Zhou Z, Peng X, Insolera R, Fink DJ, Mata M . IL-10 promotes neuronal survival following spinal cord injury. Exp Neurol 2009; 220: 183–190.
Saraiva M, Christensen JR, Veldhoen M, Murphy TL, Murphy KM, O'Garra A . Interleukin-10 production by Th1 cells requires interleukin-12-induced STAT4 transcription factor and ERK MAP kinase activation by high antigen dose. Immunity 2009; 31: 209–219.
Ishii H, Kubo T, Kumanogoh A, Yamashita T . Th1 cells promote neurite outgrowth from cortical neurons via a mechanism dependent on semaphorins. Biochem Biophys Res Commun 2010; 402: 168–172.
Shaw MH, Freeman GJ, Scott MF, Fox BA, Bzik DJ, Belkaid Y et al. Tyk2 negatively regulates adaptive Th1 immunity by mediating IL-10 signaling and promoting IFN-gamma-dependent IL-10 reactivation. J Immunol 2006; 176: 7263–7271.
Wong G, Goldshmit Y, Turnley AM . Interferon-gamma but not TNF alpha promotes neuronal differentiation and neurite outgrowth of murine adult neural stem cells. Exp Neurol 2004; 187: 171–177.
Baron R, Nemirovsky A, Harpaz I, Cohen H, Owens T, Monsonego A . IFN-gamma enhances neurogenesis in wild-type mice and in a mouse model of Alzheimer’s disease. FASEB J 2008; 22: 2843–2852.
Butovsky O, Ziv Y, Schwartz A, Landa G, Talpalar AE, Pluchino S et al. Microglia activated by IL-4 or IFN-gamma differentially induce neurogenesis and oligodendrogenesis from adult stem/progenitor cells. Mol Cell Neurosci 2006; 31: 149–160.
Shechter R, London A, Varol C, Raposo C, Cusimano M, Yovel G et al. Infiltrating blood-derived macrophages are vital cells playing an anti-inflammatory role in recovery from spinal cord injury in mice. PLoS Med 2009; 6: e1000113.
Kigerl KA, Gensel JC, Ankeny DP, Alexander JK, Donnelly DJ, Popovich PG . Identification of two distinct macrophage subsets with divergent effects causing either neurotoxicity or regeneration in the injured mouse spinal cord. J Neurosci 2009; 29: 13435–13444.
Horino J, Fujimoto M, Terabe F, Serada S, Takahashi T, Soma Y et al. Suppressor of cytokine signaling-1 ameliorates dextran sulfate sodium-induced colitis in mice. Int Immunol 2008; 20: 753–762.
Hirotani T, Lee PY, Kuwata H, Yamamoto M, Matsumoto M, Kawase I et al. The nuclear IkappaB protein IkappaBNS selectively inhibits lipopolysaccharide-induced IL-6 production in macrophages of the colonic lamina propria. J Immunol 2005; 174: 3650–3657.
Engesser-Cesar C, Anderson AJ, Basso DM, Edgerton VR, Cotman CW . Voluntary wheel running improves recovery from a moderate spinal cord injury. J Neurotrauma 2005; 22: 157–171.
Serada S, Fujimoto M, Mihara M, Koike N, Ohsugi Y, Nomura S et al. IL-6 blockade inhibits the induction of myelin antigen-specific Th17 cells and Th1 cells in experimental autoimmune encephalomyelitis. Proc Natl Acad Sci USA 2008; 105: 9041–9046.
Kitayama M, Ueno M, Itakura T, Yamashita T . Activated microglia inhibit axonal growth through RGMa. PLoS One 2011; 6: e25234.
Acknowledgements
We thank Drs. T Nakayama, M Yamashita, and M Kuwahara at Chiba University for their technical advice on T-cell culture; Drs. K Morimoto and S Lee at Osaka University for their help in histological assessment; Ms Nakamura at Osaka University for her advise on surgical procedure; Dr. Y Souma at the National Institute of Biomedical Innovation for taking care of the IFN-γ knockout mice; and Drs. H Iijima, A Mukai, H at Osaka University for advice on knockout mice. This work was supported by a research grant from a Grant-in-Aid for Young Scientists (S) from the Japan Society for the Promotion of Science (JSPS).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Edited by A Verkhratsky
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Ishii, H., Tanabe, S., Ueno, M. et al. ifn-γ-dependent secretion of IL-10 from Th1 cells and microglia/macrophages contributes to functional recovery after spinal cord injury. Cell Death Dis 4, e710 (2013). https://doi.org/10.1038/cddis.2013.234
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cddis.2013.234
Keywords
This article is cited by
-
Inflammation after spinal cord injury: a review of the critical timeline of signaling cues and cellular infiltration
Journal of Neuroinflammation (2021)
-
Lentiviral Interleukin-10 Gene Therapy Preserves Fine Motor Circuitry and Function After a Cervical Spinal Cord Injury in Male and Female Mice
Neurotherapeutics (2021)
-
Plasma Erythropoietin, IL-17A, and IFNγ as Potential Biomarkers of Motor Function Recovery in a Canine Model of Spinal Cord Injury
Journal of Molecular Neuroscience (2020)
-
Resolution of inflammation-induced depression requires T lymphocytes and endogenous brain interleukin-10 signaling
Neuropsychopharmacology (2018)
-
NOX2 deficiency alters macrophage phenotype through an IL-10/STAT3 dependent mechanism: implications for traumatic brain injury
Journal of Neuroinflammation (2017)