Abstract
The CB1 cannabinoid receptor, the main molecular target of endocannabinoids and cannabis active components, is the most abundant G protein-coupled receptor in the mammalian brain. In particular, the CB1 receptor is highly expressed in the basal ganglia, mostly on terminals of medium-sized spiny neurons, where it plays a key neuromodulatory function. The CB1 receptor also confers neuroprotection in various experimental models of striatal damage. However, the assessment of the physiological relevance and therapeutic potential of the CB1 receptor in basal ganglia-related diseases is hampered, at least in part, by the lack of knowledge of the precise mechanism of CB1 receptor neuroprotective activity. Here, by using an array of pharmacological, genetic and pharmacogenetic (designer receptor exclusively activated by designer drug) approaches, we show that (1) CB1 receptor engagement protects striatal cells from excitotoxic death via the phosphatidylinositol 3-kinase/Akt/mammalian target of rapamycin complex 1 pathway, which, in turn, (2) induces brain-derived neurotrophic factor (BDNF) expression through the selective activation of BDNF gene promoter IV, an effect that is mediated by multiple transcription factors. To assess the possible functional impact of the CB1/BDNF axis in a neurodegenerative-disease context in vivo, we conducted experiments in the R6/2 mouse, a well-established model of Huntington’s disease, in which the CB1 receptor and BDNF are known to be severely downregulated in the dorsolateral striatum. Adeno-associated viral vector-enforced re-expression of the CB1 receptor in the dorsolateral striatum of R6/2 mice allowed the re-expression of BDNF and the concerted rescue of the neuropathological deficits in these animals. Collectively, these findings unravel a molecular link between CB1 receptor activation and BDNF expression, and support the relevance of the CB1/BDNF axis in promoting striatal neuron survival.
Similar content being viewed by others
Main
The CB1 receptor is the most abundant G protein-coupled receptor in the mammalian brain.1 This receptor is engaged by endocannabinoids, a family of prostanoid-like neural messengers, as well as by Δ9-tetrahydrocannabinol (THC), the main active component of the hemp plant Cannabis sativa.1, 2, 3 Endocannabinoid signaling serves as a major feedback mechanism aimed at preventing excessive pre-synaptic activity, thereby tuning the functionality and plasticity of many synapses. In particular, the CB1 receptor is very highly expressed in GABAergic terminals of the forebrain, where it mediates endocannabinoid-dependent inhibition of GABA release.1
In concert with this well-established neuromodulatory function, one of the most remarkable biological actions of the CB1 receptor is to prevent neuronal death. This effect has been reported in many different animal models of acute brain damage and chronic neurodegeneration, and has raised hope about the possible clinical use of cannabinoids as neuroprotective drugs.1, 4, 5, 6 However, the assessment of the physiological relevance and therapeutic potential of the CB1 receptor in neurological diseases is hampered, at least in part, by the lack of knowledge on the precise molecular mechanisms of CB1 receptor neuroprotective activity.5, 7 It is well established that CB1 receptor engagement inhibits excitotoxic neurotransmission by blunting pre-synaptic glutamate release, and this has been put forward as a major event underlying CB1 receptor-mediated neuroprotection.1, 6, 8, 9 However, it is plausible that additional processes contribute to the neuroprotective activity of the CB1 receptor. Specifically, studies conducted in the mouse and rat brain have reported a close association between CB1 receptor activity and the expression of brain-derived neurotrophic factor (BDNF),5, 7 one of the master neurotrophins in the mammalian forebrain.10 Moreover, acute intravenous administration of THC to healthy volunteers increases BDNF levels in the serum,11 thus suggesting that a CB1/BDNF connection could also exist in humans.
A putative CB1/BDNF connection might be particularly relevant in the striatum, and influence their related motor disorders (e.g., Huntington’s disease (HD) and Parkinson’s disease), as, for example, (1) the CB1 receptor is highly expressed in medium-sized spiny neurons (MSNs), the cells that constitute ~90% of total striatal neurons, and plays a key role in the control of motor behavior by basal ganglia circuitry;4, 12 (2) BDNF and its high-affinity receptor, TrkB, exert a pivotal function in MSN generation, survival and plasticity;13, 14, 15 and (3) striatal CB1 receptor,16 BDNF17 and TrkB18 expression declines along disease progression in animal models of HD, and restoration of CB1 receptor,19 BDNF20 or TrkB21, 22 function prevents HD-like neurodegeneration.
In spite of these concerted changes in CB1 receptor activity and BDNF expression, no causative link between the two events has been defined yet. Hence, here we sought to establish a molecular connection between CB1 receptor activation and BDNF expression in the striatum, and to assess the possible neuroprotective relevance of this putative CB1/BDNF axis.
Results
The CB1 receptor protects cultured striatal cells from excitoxicity via PI3K/Akt/mTORC1/BDNF
The CB1 cannabinoid receptor is a pleiotropic G protein-coupled receptor that modulates various pathways potentially involved in the control of cell survival such as phosphatidylinositol 3-kinase (PI3K)/Akt, mitogen-activated protein kinases (extracellular signal-regulated kinase (ERK), c-Jun N-terminal kinase (JNK) and p38) and cAMP/protein kinase A (PKA).23 To study the mechanism of CB1 receptor-mediated neuroprotection, we first used STHdhQ7/Q7 mouse striatal neuroblasts, a widely used neuron-like cell line24 that expresses functional CB1 receptors.19 Cells were incubated with two paradigmatic cannabinoid receptor agonists (THC, the major active ingredient of marijuana, and HU-210, a highly-potent synthetic derivative of THC) and evaluated how the aforementioned pathways were affected. Exposure of cells to cannabinoids led to a rapid (15 min) and transient (15–30 min) phosphorylation (activation) of Akt, which was followed by a transient (30 min) phosphorylation (activation) of ribosomal S6 protein, a canonical substrate of the Akt/mammalian target of rapamycin complex 1 (mTORC1) pathway (Figure 1a and Supplementary Figure S1a). This effect was dose dependent (Supplementary Figure S1b). In contrast, the phosphorylation status of ERK, JNK, p38 and PKA substrates was not changed by cannabinoids (Figure 1a).
The CB1 receptor protects cultured striatal cells from NMDA-induced excitoxicity via PI3K/Akt/mTORC1/BDNF. (a) STHdhQ7/Q7 cells were incubated for the times indicated with vehicle, 0.5-μM THC or 10-nM HU-210. Cells were lysed and western blot analyses were conducted. Quantification of mean optical density (O.D.) values relative to those of loading controls (respective total proteins, or α-tubulin in the case of PKA phosphorylated substrates) as well as representative blots are shown (n=3–4 experiments). (b, c) STHdhQ7/Q7 cells were preincubated for 5 h in Locke’s solution with or without 1-mM NMDA together with vehicle, 0.5-μM THC, 10-nM HU-210, 0.2-μM wortmanin, 0.1-μM Akti-1/2, 30-nM rapamycin and/or 25-nM K252a, and subsequently incubated for 24 h in NMDA-free medium. Relative cell viability is shown (n=6–8 experiments). (d) STHdhQ7/Q7 cells were transfected with a non-targeted siRNA or with siRNAs directed against BDNF or TrkB, and subsequently incubated for 5 h with or without NMDA, THC and/or HU-210 as in b. Relative cell viability is shown (n=4–6 experiments). (e) Primary mouse striatal neurons were incubated for 30 min in Locke’s medium with or without 50-μM NMDA, together with vehicle, 0.3-μM THC, 10-nM HU-210, 0.25-μM SR141716, 0.1-μM Akti-1/2, 20-nM rapamycin and/or 10-nM K252a, and subsequently incubated for 2 h in NMDA-free medium. Relative cell viability is shown (n=4–6 experiments). Data were analyzed using ANOVA with post hoc Student-Newman-Keuls test. *P<0.05 and **P<0.01 from the corresponding vehicle-treated cells
These findings prompted us to test the involvement of the PI3K/Akt/mTORC1 pathway in CB1 receptor-mediated neuroprotection. We used STHdhQ7/Q7 cells exposed to the well-established excitotoxin N-methyl-d-aspartate (NMDA) because the CB1 receptor is known to exert cytoprotection in that experimental system.19 In agreement with some authors,25, 26 but, owing to unobvious reasons, in disagreement with others,27 we could readily detect transcripts encoding NMDA receptor subunits in STHdhQ7/Q7 cells (threshold cycle (Ct) values: NR1, 35; NR2A, 35; NR2B, 27; NR2C, 32; and NR2D, 34). These values support that NR2B and NR2C might be responsible for NMDA-induced responses in STHdhQ7/Q7 cells, and that these cells express very low levels of other NMDA receptor subunits. Our STHdhQ7/Q7 cells were sensitive to NMDA in a dose-dependent manner (Supplementary Figure S2). From these dose-dependency assays, which were similar to those previously reported by Xifro et al.,26 we selected the standard dose of 1 mM NMDA for further experiments. THC and HU-210 rescued cells from 1-mM NMDA induced death, and blockade of PI3K (with wortmannin), Akt (with Akti-1/2) or mTORC1 (with rapamycin) abrogated cannabinoid-evoked cytoprotection (Figure 1b).
As BDNF plays a key protective role on MSNs, and an association between BDNF expression and CB1 receptor function occurs in several pathophysiological settings,5, 7 we examined the possible involvement of BDNF in cannabinoid-induced neuroprotection. K252a, an inhibitor of the tyrosine kinase activity of the BDNF receptor TrkB, abrogated THC- and HU-210-induced neuroprotection (Figure 1c). A similar preventive effect was observed when BDNF or TrkB expression was silenced with specific siRNAs (which diminished total BDNF or TrkB mRNA levels to 29±10% or 47±10% of control siRNA-transfected cells, respectively; n=4–6 experiments, P<0.01; Figure 1d). Likewise, the involvement of the PI3K/Akt/mTORC1/BDNF axis in CB1 receptor-evoked neuroprotection was also evident (1) when quinolinic acid instead of NMDA was used as excitotoxin (Supplementary Figure S3), and (2) when primary mouse striatal neurons (Ct values of NMDA receptor subunits: NR1, 28; NR2A, 31; NR2B, 26; NR2C, 32; and NR2D, 30) instead of STHdhQ7/Q7 cells were used as cellular model (Figure 1e). Specifically, the protective effect of cannabinoids in those two experimental systems was prevented by the CB1-selective antagonist SR141716 (rimonabant) or upon blockade of the PI3K/Akt/mTORC1/BDNF pathway (Supplementary Figure S3 and Figure 1e).
The CB1 receptor induces BDNF promoter IV via PI3K/Akt/mTORC1
The BDNF gene consists of multiple promoters and 5′ untranslated exons, together with a common 3′ protein-coding exon. After transcription and splicing, one of the 5′ exons is joined to the single coding exon, therefore resulting in different BDNF mRNA forms but an identical BDNF protein.28, 29 To obtain direct evidence for the CB1 receptor-mediated control of BDNF expression in STHdhQ7/Q7 cells, we evaluated the effect of cannabinoids on the best characterized Bdnf gene promoters by using exon-specific qPCR primers. THC upregulated total BDNF transcripts (Ct=23) and, specifically, exon IV-containing BDNF transcripts (Ct=27; Figure 2a). Hence, Bdnf promoter IV was subsequently studied in further detail. THC-induced accumulation of exon IV-containing transcripts was mimicked by HU-210 and prevented by SR141716 (Figure 2b). As for cannabinoid-evoked neuroprotection (see above), blockade of the PI3K/Akt/mTORC1 pathway prevented the cannabinoid-induced increase of exon IV-containing transcripts (Figure 2b).
The CB1 receptor induces BDNF promoter IV via PI3K/Akt/mTORC1. (a) STHdhQ7/Q7 cells were incubated for 15 h with vehicle or 0.5-μM THC and the levels of BDNF transcripts with the indicated 5′ exons were determined (n=3–4 experiments). (b) STHdhQ7/Q7 cells were incubated for 15 h with vehicle or 0.5-μM THC, 10-nM HU-210, 0.25-μM SR141716, 0.2-μM wortmannin, 0.1-μM Akti-1/2 and/or 30-nM rapamycin, and the levels of BDNF transcripts containing exon IV were determined (n=3–4 experiments). (c) STHdhQ7/Q7 cells were transfected with a construct harboring a 0.5-kb human BDNF promoter IV fused to the luciferase reporter gene and subsequently incubated for 15 h with 0.5-μM THC, 10-nM HU-210, 0.1-μM Akti-1/2 and/or 30-nM rapamycin. Relative promoter activity is shown (n=4–6 experiments). (d) STHdhQ7/Q7 cells were incubated for 24 h with vehicle or 0.5-μM THC,10-nM HU-210, 0.1-μM Akti-1/2 and/or 30-nM rapamycin, and the levels of BDNF protein were determined (n=3–4 experiments). (e, f) Primary mouse striatal neurons were incubated with vehicle or 0.3-μM THC, 10-nM HU-210, 0.25-μM SR141716 and/or 0.1-μM Akti-1/2, and the levels of exon IV-containing and total BDNF transcripts (e; qPCR; 15-h incubation with the additions; n=3–4 experiments) as well as of BDNF protein were determined (f; western blot; 24-h incubation with the additions; n=4 experiments; quantification of mean±S.E.M. optical density (O.D.) values relative to those of β-actin as well as a representative blot are shown). Data were analyzed using ANOVA with post hoc Student-Newman-Keuls test. *P<0.05 and **P<0.01 from the corresponding vehicle-treated cells
We next used additional approaches to substantiate a CB1 receptor-induced activation of BDNF promoter IV. (1) We transfected STHdhQ7/Q7 cells with a construct that contains a human BDNF promoter IV fused to the luciferase reporter gene,30 and found that promoter IV activity was enhanced by THC and HU-210, this effect being abrogated by blockade of Akt or mTORC1 (Figure 2c). (2) BDNF protein levels, as determined by ELISA in STHdhQ7/Q7 cell-culture extracts, were also increased by THC and HU-210 in an Akt- and mTORC1-dependent manner (Figure 2d). (3) We isolated primary mouse striatal neurons and found that CB1 receptor agonism increased both exon IV-containing (Ct=29) and total BDNF transcripts (Ct=27), as determined by qPCR (Figure 2e), as well as BDNF protein levels, as determined by western blot (Figure 2f; we were unable to reliably quantify BDNF by ELISA in neuron-culture supernatants). These neuron cultures had only ~5% (n=3 cultures) of contaminating glial fibrillary acidic protein (GFAP)-positive cells (assumed to be astroglia), and their content in BDNF/GFAP-double-positive cells relative to total BDNF-positive cells was negligible (Supplementary Figure S4). (4) We prepared mouse-brain organotypic cultures and found that THC increased striatal BDNF protein expression, as evidenced by western blot and immunofluorescence (Supplementary Figure S5).
Multiple transcription factors are involved in the CB1 receptor-mediated induction of BDNF promoter IV
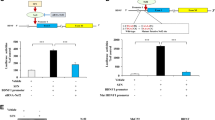
We next aimed at characterizing the specific regions of BDNF promoter IV involved in the CB1 receptor-dependent control of gene transcription. For this purpose, STHdhQ7/Q7 cells were transfected with BDNF promoter IV-luciferase reporter constructs containing mutations in cis-elements that control neuronal BDNF promoter IV upon different stimuli.30, 31 The cannabinoid-evoked activation of wild-type BDNF promoter IV was not evident when mutations were introduced in (1) bHLH-PAS transcription factor-response element (PasRE), to which neuronal PAS domain protein 4 (NPAS4)-aryl hydrocarbon receptor nuclear translocator 2 (ARNT2) dimers bind; (2) Ca2+-response element 1 (CaRE1), to which calcium-responsive transcription factor (CaRF) binds; (3) upstream stimulatory factor-binding element (UBE), to which upstream stimulatory factors (USFs) bind; (4) cAMP/Ca2+-response element (CRE), to which cAMP response element-binding protein (CREB) binds; (5) basic helix-loop-helix B2 (BHLHB2)-response element (BHLHB2-RE); and (6) conserved E-box element 2 (cEbox2; Figure 3a). Cannabinoid action on BDNF promoter IV was not affected when the NFκB-response element (NFκB-RE) was mutated (Figure 3a).
Multiple transcription factors are involved in the CB1 receptor-mediated induction of BDNF promoter IV. (a) STHdhQ7/Q7 cells were transfected with a construct harboring a WT 0.5-kb human BDNF promoter IV fused to the luciferase reporter gene or with the same construct containing mutations (m) in the indicated response elements (RE). Cells were subsequently incubated for 15 h with vehicle, 0.5-μM THC or 10-nM HU-210. Promoter activity relative to vehicle incubations is shown (n=4–6 experiments). (b) STHdhQ7/Q7 cells were transfected with a non-targeted siRNA or siRNAs directed against the indicated transcription factors. After 24 h, they were transfected with the aforementioned WT BDNF promoter IV reporter construct, and, after an additional 24-h period, cells were incubated with vehicle, 0.5-μM THC or 10-nM HU-210 for 15 h. Left: promoter activity relative to vehicle incubations; right: knock-down (KD) efficacy of the siRNAs directed against the corresponding transcription factor (siTF; n=4–6 experiments). Data were analyzed using unpaired Student’s t-test. *P<0.05 and **P<0.01 from the corresponding vehicle-treated cells or siControl-transfected cells (b, left). (c) STHdhQ7/Q7 cells were incubated for 30 min with vehicle, 0.5-μM THC or 10-nM HU-210, lysed and used for western blot analyses. Quantification of mean optical density (O.D.) values of pCREB relative to those of total CREB as well as a representative blot are shown (n=3–4 experiments)
To evaluate the involvement of the best-defined transcription factors that bind to the aforementioned BDNF promoter IV regulatory elements, we silenced the expression of NPAS4, CaRF, USF and CREB with specific siRNAs and measured cannabinoid-evoked activation of the wild-type BDNF promoter IV. Knocking-down the expression of any of these transcription factors abrogated the cannabinoid-induced activation of BDNF promoter IV (Figure 3b), thus suggesting that all of them are necessary for the latter process to occur. Accordingly, CREB phosphorylation in its critical activatory S133 residue was enhanced by cannabinoid challenge (Figure 3c).
CB1 receptor antagonism attenuates BDNF upregulation induced by pharmacogenetic activation of striatal neurons
To evaluate the relevance of the CB1 receptor in the physiological control of striatal BDNF expression, we selectively manipulated MSN activity by the designer receptor exclusively activated by designer drug (DREADD) pharmacogenetic technique. This tool is based on the molecular evolution of muscarinic acetylcholine receptors, leading to a Gq protein-coupled receptor with negligible affinity for the native agonist (acetylcholine) but to which the pharmacologically inert agonist clozapine-N-oxide (CNO) binds with high potency and efficacy,32 thus allowing the remote control of neuronal activity in specific cell populations in vivo.33
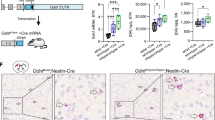
First, we validated this experimental approach in vitro. STHdhQ7/Q7 cells were nucleofected with a plasmid encoding a DREADD-Gq (hM3Dq) fused to mCherry (or only mCherry) and subsequently treated with CNO (or vehicle). CNO-induced activation of hM3Dq led to an accumulation of both exon IV-containing and total BDNF transcripts, and SR141716 prevented this effect (Figure 4a). Next, we injected stereotactically C57BL/6J mice with a recombinant adeno-associated viral vector encoding hM3Dq-mCherry (or only mCherry) into the dorsolateral (motor) striatum (Figure 4b). The expression of the transgene was driven by the calcium/calmodulin-dependent protein kinase II-α (CaMKIIα) promoter in order to confine it to MSNs and avoid other cell populations (e.g., interneurons and glia). Animals were subsequently treated with CNO (or vehicle) in conditions that evoke neuronal activation (one injection of CNO at 10 mg/kg body weight).34 This procedure triggered the expression of exon IV-containing and total BDNF transcripts in the striatum in situ, and, of note, treatment with SR141716 (one injection at 1 mg/kg body weight) produced per se the opposite effect to CNO and attenuated the CNO-triggered upregulation of BDNF expression (Figure 4b).
CB1 receptor antagonism attenuates BDNF upregulation induced by pharmacogenetic activation of striatal neurons. (a) STHdhQ7/Q7 cells were nucleofected with a construct expressing hM3Dq-mCherry (or mCherry alone as control). Two days after, cells were treated with 50-μM CNO (or H2O as vehicle) plus 0.25-μM SR141716 (or 0.1% DMSO as vehicle) for 4 h, and the levels of exon IV-containing and total BDNF transcripts were determined by qPCR (n=3–4 experiments). KCl (25 mM) was used as a control of activity-dependent BDNF expression upregulation. (b) Eight-week-old C57BL/6J mice were injected stereotactically into the dorsolateral striatum with a recombinant adeno-associated virus encoding hM3Dq-mCherry (or only mCherry as control) under the control of the CaMKIIα promoter (n=6–8 animals per group). Left: Example of a mouse brain injected with the mCherry construct. The site of infection in the striatum is outlined. Right: Levels of exon IV-containing and total BDNF transcripts in the dorsolateral striatum as determined by qPCR 4 h after i.p. injection of CNO (10 mg/kg body weight) with or without SR141716 (1 mg/kg body weight) or the corresponding vehicles. Data were analyzed using unpaired Student’s t-test. *P<0.05 and **P<0.01 from the corresponding Veh/Veh group; #P<0.05 and ##P<0.01 from the corresponding Veh/CNO group
Pathophysiological relevance of CB1 receptor-mediated striatal BDNF upregulation in HD
To assess the functional impact of the CB1/BDNF axis in a neurodegenerative-disease context in vivo, we used the R6/2 mouse, a well-established model of HD.35 This devastating disease constitutes so far the best paradigm to study the neuroprotective role of the CB1 receptor as this receptor is highly expressed in the basal ganglia by MSNs, the cells that constitute ~90% of total striatal neurons and primarily degenerate in HD, and plays a key role in the control of motor behavior, one of the processes that is typically affected in HD.4, 12 In addition, an early and remarkable downregulation of CB1 receptor expression has been documented as one of the most characteristic neurochemical alterations of MSNs in HD animal models36, 37, 38 and HD patients.39, 40 Moreover, we19 and others41 have provided genetic evidence for a neuroprotective role of the CB1 receptor in HD mouse models.
To test whether this neuroprotective effect relies on BDNF signaling, we injected sterotactically 3.5- to 4-week-old R6/2 mice (or wild-type littermates) with a recombinant adeno-associated viral vector encoding CB1 receptor (or empty vector) into the dorsolateral striatum. This procedure allowed the subsequent re-expression of the CB1 receptor (Figure 5a) as well as BDNF protein (Figure 5b), total BDNF mRNA (Figure 5c; Ct=26) and exon IV-containing BDNF mRNA (Figure 5d; Ct=29). Reactivation of the CB1/BDNF axis also normalized the HD-like molecular-pathology profile of these animals, as determined by the recovered levels of the MSN marker dopamine- and cAMP-regulated phosphoprotein of 32 KDa (DARPP-32; Figure 6a; confirmation by stereological counting shown in Supplementary Figure S6), the pan-GABAergic-neuron marker glutamic acid decarboxylase 67 kDa isoform (GAD-67; Figure 6b), the post-synaptic marker post-synaptic density protein 95 (PSD-95; Figure 6c) and the mTORC1-activity marker phosphorylated (activated) ribosomal S6 protein (Figure 6d). In addition, CB1 receptor re-expression rescued striatal atrophy, the main neuropathological hallmark of HD, as determined by MRI analysis (Figure 7). Cortical and hippocampal volumes, used as controls, were not significantly different in 8-week-old wild-type and R6/2 mice injected with CB1 receptor-encoding or empty viral vectors (Supplementary Figure S7). (We note that overexpression of the CB1 receptor in the striata of wild-type mice did not lead to a significant upregulation of BDNF or other markers of neuronal integrity/functionality. As MSNs express very large amounts of CB1 receptors, it is conceivable that the CB1 receptor-response system would be essentially saturated in the normal setting but not in conditions of restricted receptor function such as HD. In this regard, agonist-stimulated [35S]GTPγS-binding studies have shown that when higher expression levels of CB1 receptors occur, for example, in the striatum versus other brain regions,42 in GABAergic versus glutamatergic terminals43 or in CB1+/+ versus CB1+/− mice,44 the receptors couple with little efficacy to G proteins, thus making signaling in CB1 highly expressing systems refractory to stimulation by mere increases in total receptor numbers.)
Enforced re-expression of the CB1 receptor rescues BDNF expression in the striata of R6/2 mice. R6/2 mice (3.5–4 weeks old) and WT littermates were injected stereotactically into the dorsolateral striatum with a recombinant adeno-associated virus (AAV) encoding HA-tagged CB1 receptor or the empty vector as control (n=10–12 animals per group). At week 8 of age, animals were killed for histological and qPCR analyses in the striatum. (a) CB1 receptor immunoreactivity (relative values of CB1 receptor-positive area/total cell nuclei). Slices from the dorsolateral striatum of CB1−/− mice70 were used as control of staining specificity. Representative images are shown. (b) BDNF immunoreactivity (relative values of BDNF-positive area/total cell nuclei). Slices from the dorsolateral striatum of neuron-specific, neurofilament L-conditional BDNF knockout (Bdnffloxed/-;Nefl-Cre/+) mice (generated at Michael Sendtner’s laboratory, University of Würzburg, Germany) were used as control of staining specificity. Representative images are shown. (c) Levels of total BDNF transcripts. (d) Levels of exon IV-containing BDNF transcripts. Data were analyzed using unpaired Student’s t-test. *P<0.05 and **P<0.01 from the corresponding WT-empty group; ##P<0.01 from the corresponding R6/2-empty group
Enforced re-expression of the CB1 receptor rescues HD-like molecular-pathology markers in the striata of R6/2 mice. R6/2 mice (3.5–4 weeks old) and WT littermates were injected stereotactically into the dorsolateral striatum with a recombinant adeno-associated virus (AAV) encoding HA-tagged CB1 receptor or the empty vector as control (n=10–12 animals per group). At week 8 of age, animals were killed for histological analyses in the striatum. (a) DARPP-32 immunoreactivity (relative values of DARPP-32-positive cells/total cell nuclei). Representative images are shown. (b) GAD-67 immunoreactivity (relative values of GAD-67-positive area/total cell nuclei). (c) PSD-95 immunoreactivity (relative values of PSD-95-positive area/total cell nuclei). (d) Phospho-S6 immunoreactivity (relative values of pS6-positive cells/total cell nuclei). Data were analyzed using unpaired Student’s t-test. *P<0.05 and **P<0.01 from the corresponding WT-empty group; #P<0.05 and ##P<0.01 from the corresponding R6/2-empty group
Enforced re-expression of the CB1 receptor rescues HD-like striatal atrophy in R6/2 mice. R6/2 mice (3.5–4 weeks old) and WT littermates were injected stereotactically into the dorsolateral striatum with a recombinant adeno-associated virus (AAV) encoding HA-tagged CB1 receptor or empty vector as control (n=10–12 animals per group). The volume of the striatum and lateral ventricles relative to total brain volume of 8-week-old animals is represented. Representative MRI pictures are shown. Striata are outlined. Data were analyzed using unpaired Student’s t-test. **P<0.01 from the corresponding WT-empty group; ##P<0.01 from the corresponding R6/2-empty group
Finally, we analyzed a series of post-mortem human caudate-putamen samples for concerted changes in CB1 receptor and BDNF immunoreactivity. In line with Zuccato and Cattaneo,17 we found a significant reduction of CB1 receptor-positive, BDNF-positive and CB1/BDNF-double-positive neurons in HD patients compared to control subjects (Supplementary Figure S8a). Western blot analyses, which had previously shown a decrease in CB1 receptor protein expression in caudate-putamen specimens of HD patients,19 evidenced a parallel reduction of BDNF protein expression in those samples (Supplementary Figure S8b). This was associated to a concomitant decrease in the levels of pCREB (Supplementary Figure S8b), a key signaling marker of the CB1/BDNF axis described above. These findings therefore suggest that a functional link between the CB1 receptor and BDNF could also occur in the human brain.
Discussion
Here we show that, in the mouse striatum, CB1 receptor engagement upregulates BDNF expression, through which it can confer neuroprotection against excitotoxicity in vitro and mutant huntingtin-induced toxicity in vivo. On mechanistic grounds, this CB1 receptor-mediated induction of BDNF gene expression relies on the activation of the PI3K/Akt/mTORC1 pathway, which, in turn, targets BDNF promoter IV, a promoter that is also responsive to various types of neuronal activity-related stimuli in the mouse, rat and human BDNF gene.10, 29, 30 The induction of BDNF promoter IV evoked by the CB1 receptor-mediated activation of the PI3K/Akt/mTORC1 pathway appears to be a complex process, as several responsive elements and transcription factors are involved. The observation that CREB is necessary for the CB1 receptor-mediated induction of BDNF promoter IV fits with the pivotal role of this transcription factor in the regulation of BDNF action.10, 45 In fact, mice with a specific knock-in mutation in the CRE of Bdnf promoter IV display impaired sensory experience-induced expression of BDNF and defective development of cortical inhibitory circuits.46 It is thus conceivable that the rapid and pleiotropic triggering of Ca2+-, cAMP-, ERK- and/or Akt-related signals will converge in the immediate/early activation of CREB and CaRF, which, by binding to CRE30 and CaRE1,31, 47 respectively, could initiate BDNF promoter IV transcription. Of note, and in line with our data, the Ca2+ influx-dependent early activation of CRE/CaRE3 (via CREB) and CaRE1 (via CaRF) in the rat BDNF promoter IV is abrogated by genetic or pharmacological blockade of PI3K signaling.31 Upon CREB and CaRF activation, at later time points other transcription factors, such as NPAS4 via PasRE,30, 48 could be important for sustaining the transcriptional activity of BDNF promoter IV under different conditions, including CB1 receptor activation, as reported here.
The relation between CB1 receptor activation and BDNF expression appears to be a region-specific process. Thus, this association has been clearly established in the mouse hippocampus by experiments involving CB1 receptor gain of function (CB1 receptor pharmacological agonism) and loss of function (CB1 receptor genetic inactivation, CB1 receptor pharmacological antagonism) conducted in various in vitro (tissue slices, cell cultures) and in vivo (whole mice) experimental systems.8, 49, 50, 51, 52, 53, 54 In line with our present study in the mouse dorsolateral striatum, THC administration increased BDNF expression in the rat ventral striatum.55 However, and in striking contrast with the hippocampus and the striatum, BDNF expression in the mouse cortex, which expresses high levels of the CB1 receptor,1 was unaffected by either THC administration19, 51 or CB1 receptor genetic ablation,19, 52 while another study found only very marginal increases in BDNF levels in the medial prefrontal cortex and the frontoparietal cortex upon THC injection to rats.55 Hence, albeit for hitherto unknown molecular reasons, BDNF expression seems to be much more refractory to CB1 receptor activation in the cortex than in the striatum or hippocampus.
This zonation of the CB1/BDNF axis in the brain is certainly relevant in the context of our findings because MSNs are known to receive BDNF from the cortex via the well-established corticostriatal pathway.56 In addition, significant amounts of BDNF mRNA have been found in the striatum, thus indicating that striatal BDNF can also be produced in situ.19, 29, 57, 58 Moreover, our DREADD experiments, by allowing the remote and selective control of MSN activity, provide robust evidence for the activity-dependent production of BDNF in mouse MSNs in vivo. Further support to this notion comes from the findings that mutant huntingtin affects axonal transport of BDNF in striatal neurons but not in cortical neurons,59 and that dopamine receptor heteromers control BDNF production by striatal neurons in situ.60 All these observations do not downplay the corticostriatal pathway as a key source of BDNF for MSNs in the normal brain. For example, in our hands, significant amounts of BDNF transcripts are readily detected in the adult-mouse striatum, but their levels are lower than those found in the cortex (mRNA levels in the striatum relative to the cortex: total BDNF, 24±2%; BDNF-IV, 20±4%; n=8 animals). However, it is likely that, under particular pathophysiological situations, BDNF production can increase in the striatum in situ, thereby complementing the bulk supply of BDNF from the cortex with a local –and thus spatially privileged- extra source of the neurotrophin for MSNs. The multiple lines of evidence provided by this study, together with the aforementioned lack of effect of CB1 receptor activation on cortical BDNF expression, strongly support that the CB1 receptor-mediated upregulation of striatal BDNF is a striatum-autonomous effect rather than the consequence of an enhanced anterograde supply of BDNF from the cortex. Nonetheless, the CB1/BDNF connection in MSNs can be more complex and be accompanied, for example, by a reciprocal BDNF-dependent control of CB1 receptor function.61
A key unanswered question in many neurodegenerative diseases is what precise factors dictate the selective damage of a particular neuronal population. Regarding HD, the disease has long been known to be caused by an expanded polyglutamine tract in the N-terminal domain of the huntingtin protein,62 but the mechanisms by which MSNs are highly vulnerable to mutant huntingtin are still incompletely understood. We19 and others41 have provided genetic evidence for a neuroprotective role of the CB1 receptor in two transgenic models of HD, which could open similar studies on other neurodegenerative diseases, such as Alzheimer’s disease,63, 64, 65 in which CB1 receptor levels are known to be downregulated during disease state. Unfortunately, the precise relevance of CB1 receptor and BDNF downregulation in HD pathology are not completely understood. For example, regarding the latter issue, Plotkin et al.66 have recently shown that, although reduced BDNF availability in the striatum may contribute to HD pathology,17 a major pathogenic mechanism seems to rely on an aberrant BDNF signaling via p75 neurotrophin receptors located on indirect-pathway MSNs, which adds to the previously reported alterations of BDNF signaling via TrkB.21, 22 These possibilities notwithstanding, here we cogently show that, in the striatum of the R6/2 mouse in vivo, changes in CB1 receptor expression parallel changes in the expression of BDNF and key markers of disease neuropathology, thus supporting the notion that BDNF may be a bona fide marker not only of HD neurodegeneration17 but also of CB1 receptor-evoked neuroprotection.
Materials and Methods
Animals
Hemizygous male mice transgenic for exon 1 of the human huntingtin gene with a greatly expanded CAG tract (R6/2 mice; 155–175 CAG repeats)35 and wild-type littermates were purchased from The Jackson Laboratory (Bar Harbor, ME, USA). C57BL/6J mice (Harlan, Barcelona, Spain) were used to obtain organotypic and cell cultures, as well as to conduct DREADD experiments. Animals were maintained as described.19 All animal handling procedures were approved by the Complutense University Animal Research Committee in accordance with the directives of the European Commission.
Cell cultures
Conditionally, immortalized mouse striatal neuroblasts expressing wild-type huntingtin and infected with a defective retrovirus transducing the temperature-sensitive A58/U19 large T antigen (designated as STHdhQ7/Q7 cells),24 were grown at 33°C in DMEM supplemented with 10% fetal bovine serum, 1 mM sodium pyruvate, 2 mM l-glutamine and 400 μg/ml geneticin.
Primary striatal neurons were obtained from 2-day-old C57BL/6J mice using a papain dissociation system (Worthington, NJ, USA). Striata were dissected and cells were seeded on plates pre-coated with 0.1 mg/ml poly-d-lysine at 200 000 cells/cm2 in the Neurobasal medium supplemented with B27 and GlutaMax (Gibco, Carlsbad, CA, USA).
Cell viability
STHdhQ7/Q7 cells were transferred to a serum-free medium for 24 h and incubated for a further 5 h in home-made Locke’s solution (154-mM NaCl, 5.6-mM KCl, 2.3-mM CaCl2, 3.6-mM NaHCO3, 5-mM HEPES (Lonza, Verviers, Belgium), 20-mM glucose and 10-μM glycine), supplemented or not with NMDA, together with the cannabinoid receptor agonists THC (The Health Concept, Richelbach, Germany) or HU-210 (Tocris, Bristol, UK), the PI3K inhibitor wortmannin (Sigma-Aldrich, Barcelona, Spain), the Akt inhibitor Akti-1/2 (Calbiochem, San Diego, CA, USA), the mTORC1 inhibitor rapamycin (Tecoland, Irvine, CA, USA), the tyrosine kinase inhibitor K252a (Calbiochem) or the respective vehicle (DMSO, 0.1–0.2% (v/v) final concentration). The medium was subsequently replaced by NMDA/serum-free DMEM supplemented with the corresponding drugs, and cell viability was determined after 24 h by the 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) test.
Another set of STHdhQ7/Q7 cell-viability experiments was conducted with quinolinic acid (Sigma-Aldrich) as neurotoxic agent. STHdhQ7/Q7 cells were transferred to serum-free DMEM for 24 h and subsequently incubated in this medium, supplemented or not with quinolinic acid, together with THC, HU-210, the CB1-selective antagonist SR141716 (rimonabant; kindly given by Sanofi-Aventis, Montpellier, France), Akti-1/2, rapamycin and K252a, or the respective vehicle (DMSO, 0.1–0.2% (v/v) final concentration) for 24 h. Cell viability was determined by the MTT test.
Primary C57/BL6J-mouse striatal neurons, grown for 2 days in vitro, were incubated for 30 min in the aforementioned Locke’s solution, supplemented or not with NMDA, together with THC, HU-210, SR141716, Akti-1/2, rapamycin and K252a, or the respective vehicle (DMSO, 0.1–0.2% (v/v) final concentration). The medium was subsequently replaced by NMDA-free Neurobasal medium supplemented with B27 and GlutaMax (Gibco), plus the corresponding drugs, and cell viability was determined after 2 h by the MTT test.
Cell transfection/nucleofection
Cells were transfected transiently with an ON-TARGETplus SMARTpool mBdnf siRNA (Re. L-042566-00) or mTrkB (= mNtrk2) siRNA (Re. L-048017-00), or a non-targeted SMARTpool siRNA (Re. D-001810-10), using the DharmaFECT 1 transfection reagent (Thermo Fisher, Lafayette, CO, USA).
For the luciferase reporter assays, cells were transfected transiently with constructs expressing a 524-bp human BDNF promoter IV cloned into pGL4.15 (luc2P/Hygro), or the same promoter with mutated PasRE, CaRE, UBE, CRE, BHLHB2-RE, NFκB-RE or cEbox II sites also cloned into pGL4.15 (luc2P/Hygro), as described,30 using Lipofectamine 2000 (Invitrogen, Madrid, Spain). For normalization, a renilla/pGL4.83 construct (driven by the thymidine kinase promoter) was cotransfected. Luciferase assays were performed with the Dual-Glo luciferase assay system (Promega Biotech Ibérica, Barcelona, Spain).
Other promoter activity experiments were conducted in cells transfected transiently with ON-TARGETplus SMARTpool mNpas4 (Re. L-054722-01), mCarf (Re. L-051736-01), mUsf1 (Ref. L-040656-00) or mCreb1 (Re. L-040959-01) siRNAs, or the aforementioned non-targeted SMARTpool siRNA, using the DharmaFECT 1 transfection reagent (Thermo Fisher).
For DREADD experiments in vitro, cells were nucleofected with a construct expressing the hM3Dq receptor fused to mCherry (kindly provided by Bryan L Roth, University of North Carolina, Chapel Hill, NC, USA),34 or mCherry alone as control vector, under the CAG promoter, by using an Amaxa mouse-neuron nucleofector kit (Lonza, Madrid, Spain). Cells were treated in the serum-free medium, 2 days after nucleofection, with CNO (or H2O as vehicle) plus SR141716 (or 0.1% DMSO as vehicle).
Organotypic cultures
Corticostriatal slices (300-μm thick) were obtained from adult (8 weeks old) C57/BL6J mice, and cultured under semidry conditions in the Neurobasal medium supplemented with B27 (1%), N2 (1%), glutamine (1%), penicillin/streptomycin (1%), Fungizone (1%; Gibco) and ciprofloxacin (5 μg/ml), as described.19 Slices were incubated for 24 h with THC or vehicle (DMSO, 0.1% (v/v) final concentration) and subsequently fixed with formalin and processed in 15-μm sections, which were analyzed at equivalent regions of the rostral to caudal axis. Counting of BDNF and NeuN immunoreactivity (see below) was conducted in the dorsolateral striatum in a 1-in-6 series per slice.
Real-time PCR
RNA was isolated using TRIzol reagent or RNeasy (Invitrogen, Carlsbad, CA, USA). cDNA was obtained using Transcriptor (Roche, Basel, Switzerland). Real-time PCR (qPCR) assays were performed using the FastStart SYBR Green Master (Roche) and probes were obtained from the Universal Probe Library Set (Roche). The mRNA levels of the different BDNF exons were determined with previously described primers.29, 30 Other primers used are shown in Supplementary Table SI. Amplifications were run in a 7900 HT-Fast Real-time PCR system (Applied Biosystems, Foster City, CA, USA). Relative gene expression data were determined by the 2−ΔΔCt method. Each value was adjusted to β-actin levels as reference.
Viral vectors
HA-tagged rat CB1 cannabinoid receptor was subcloned in a rAAV expression vector with a CAG promoter by using standard molecular cloning techniques. Vectors were of an AAV1/AAV2-mixed serotype, and were generated by calcium phosphate transfection of HEK293T cells and subsequent purification as described.67, 68 R6/2 mice (3.5–4 weeks old) and their wild-type littermates were injected stereotactically with the viral vectors (in 1.5 μl PBS) into the dorsolateral striatum. Each animal received one bilateral injection at coordinates (to bregma): anteroposterior −0.5, lateral ±1.4, dorso-ventral −2.7. MRI analyses were conducted at 8 weeks of age. Mice were subsequently killed by intracardial perfusion and their brains were excised for immunofluorescence and qPCR analyses.
For DREADD experiments in vivo, 8-week-old male C57BL/6J animals were injected stereotactically with viral vectors expressing the hM3Dq receptor fused to mCherry (or mCherry as control) under a minimal CaMKIIα promoter into the dorsolateral striatum as described before.9 Six weeks after surgery, animals were injected with SR141716 (1 mg/kg body weight, i.p.) or vehicle (1% (v/v) DMSO in Tween 20 (Panreac, Barcelona, Spain)/saline (1 : 18, v/v)) and, 10 min later, with CNO (10 mg/kg body weight, i.p.) or vehicle (PBS). Animals were killed 4 h after the CNO injection, and their dorsolateral striata were quickly dissected on ice and frozen at −80°C for subsequent analyses.
Western blot
Western blot analysis was conducted with antibodies raised against phosphorylated Akt (1 : 1000; Cell Signaling, Danvers, MA, USA), total Akt (1 : 1000; Cell Signaling), phosphorylated S6 ribosomal protein (1 : 1000; Cell Signaling), total S6 ribosomal protein (1 : 1000; Cell Signaling), phosphorylated ERK (1 : 1000; Cell Signaling), total ERK (1 : 1000; Cell Signaling), phosphorylated JNK (1 : 1000; Cell Signaling), total JNK (1 : 1000; Cell Signaling), phosphorylated p38 (1 : 1000; Cell Signaling), total p38 (1 : 1000 Cell Signaling), PKA phosphorylated substrates (1 : 1000; Cell Signaling), phosphorylated CREB (1 : 1000, Cell Signaling), total CREB (1 : 1000, Cell Signaling), BDNF (1 : 1000, Santa Cruz Biotechnology, Santa Cruz, CA, USA), α-tubulin (1 : 4000, Sigma-Aldrich) and β-actin (1 : 4000, Sigma-Aldrich), following standard procedures. Specifically, samples from cell cultures, organotypic cultures and human post-mortem brains (obtained from the Banco de Tejidos para Investigación Neurológica, Madrid, Spain, as previously described)19 were lysed in a buffer containing 50-mM Tris, 0.3% CHAPS, 1-mM EDTA, 1-mM EGTA, 50-mM NaF, 10-mM sodium β-glycerophosphate, 5-mM sodium pyrophosphate and 1-mM sodium orthovanadate (pH 7.5) supplemented with a protease inhibitor cocktail (Roche, Madrid, Spain), 0.1-mM PMSF and 1-μM microcystin. The running buffer consisted of 200-mM glycine, 25-mM Tris and 0.1% SDS (pH 8.3), and the transfer buffer contained 200-mM glycine, 25-mM Tris and 20% methanol (pH 8.3). Blots were incubated with Tris-buffered saline (20-mM Tris and 0.5-mM NaCl, pH 7.5)/Tween 20 (0.05%) supplemented with 1% bovine serum albumin. Densitometric analysis was performed with Quantity One software (Bio-Rad, Hercules, CA, USA).
Immunomicroscopy (mouse samples)
Coronal free-floating sections (30 μm-thick) were obtained from paraformaldehyde-perfused mouse brains. Organotipic cultures were obtained as described before. Samples were incubated with antibodies against CB1 cannabinoid receptor (1 : 500; Frontier Science, Hokkaido, Japan), HA (1 : 500, Roche), BDNF (1 : 300; generated at Michael Sendtner’s laboratory, University of Würzburg, Germany),19 DARPP-32 (1 : 1000; BD, Franklin Lakes, NJ, USA), GAD-67 (1 : 250; Chemicon, Temecula, CA, USA), PSD-95 (1 : 1000, Abcam, Cambridge, UK), phosphorylated S6 ribosomal protein (1 : 200; Cell Signaling) or NeuN (1 : 400; Chemicon), followed by staining with the corresponding highly cross-adsorbed Alexa Fluor 488, 594 or 647 antibodies (1 : 500; Molecular Probes, Leyden, The Netherlands).19 GFAP was stained with an anti-GFAP-Cy3 antibody (1 : 1000, Sigma-Aldrich). Samples were subsequently incubated with DAPI (1 : 10 000, Roche) for 10 min, washed with PBS and mounted in Mowiol (Calbiochem, Madrid, Spain). Counting of brain sections was conducted in the caudate-putamen area in a 1-in-10 series per animal, ranging from bregma +1.5 mm to −0.5 mm coronal coordinates. Data were calculated as immunoreactive area per total cell nuclei, except for DARPP-32, phospho-S6 and NeuN, in which immunoreactive cells per total cell nuclei were counted. Confocal fluorescence images were acquired using TCS-SP2 software and a SP2 AOBS microscope (Leica, Wetzlar, Germany). Pixel quantification and co-localization were analyzed with ImageJ software (National Institutes of Health, Bethesda, MA, USA).
Stereological counting of the total number of DARPP-32-positive cells in the rAAV-infected region of the mouse dorsolateral striatum (Supplementary Figure S6) was performed in 30-μm-thick sections with the aforementioned DARPP-32/HA/DAPI staining conditions and within the aforementioned coronal coordinates using the optical fractionator method. A 1-in-8 series per animal was analyzed in an Olympus BX61 microscope (Olympus, Tokyo, Japan) with newCAST software (Visiopharm, Horsholm, Denmark). Volumes were calculated by applying the Cavalieri estimator. The frame area was set to 5625 μm2 with a sampling interval of 240 μm at the x and y level, and the optical dissector constituting a 13-μm-thick fraction of the total section thickness. Results are expressed as number of DARPP-32-immunoreactive cells per mm3 of rAAV-infected region. Gundersen’s coefficient of error was always below 0.1.
Immunomicroscopy (human samples)
Paraffin-embedded post-mortem 4-μm-thick brain sections containing caudate-putamen were provided by the Tissue Bank at Hospital Universitario Fundación Alcorcón (Madrid, Spain), and were obtained and handled following the ethical guidelines of that institution. Samples (four sections per individual) were obtained from HD donors (grades 3–4; n=9; age (years old) and sex: 55♂, 47♀, 45♂, 45♂, 51♂, 51♀, 44♂, 77♀ and 49♂) and control subjects with no background of neuropsychiatric disease (n=7; age (years old) and sex: 45♂, 62♀, 36♂, 74♂, 79♂, 75♀ and 69♂). For immunofluorescence analyses,69 sections were incubated with anti-BDNF antibody (1 : 50; generated at Michael Sendtner’s laboratory) and subsequently with Alexa Fluor 546 antibody (Molecular Probes). Samples were then incubated with anti-CB1 cannabinoid receptor antibody (1 : 50; Affinity Bioreagents, Golden, CO, USA), followed by incubation with Alexa Fluor 488 antibody (Molecular Probes), and finally incubated with DAPI (1 : 10 000) for 10 min and washed with PBS. Then, sections were treated with 1% Sudan Black (Sigma-Aldrich) in 70% ethanol to quench endogenous autofluorescence and finally mounted in Mowiol.
ELISA
STHdhQ7/Q7 cells were transferred to the serum-free medium and incubated with vehicle (DMSO, 0.1–0.2% (v/v) final concentration) or THC, HU-210, Akti-1/2 and rapamycin for 24 h as described above. BDNF protein levels were determined upon scraping the cell culture well and combining it with its medium by using a BDNF ELISA System (Promega Biotech Ibérica).
Magnetic resonance imaging
The volume of the striatum, ventricles, cortex (comprising somatosensory and motor areas) and hippocampus was measured by magnetic resonance imaging in a BIOSPEC BMT 47/40 (Bruker, Ettlingen, Germany) operating at 4.7 T as described.19
Statistics
Data are presented as mean±S.E.M. Statistical comparisons were made by ANOVA with post hoc Student-Newman-Keuls test or by unpaired Student’s t-test, as indicated in each figure legend.
Abbreviations
- BDNF:
-
brain-derived neurotrophic factor
- CaMKIIα:
-
calcium/calmodulin-dependent protein kinase II-α
- CaRF:
-
calcium-responsive transcription factor
- CNO:
-
clozapine-N-oxide
- CREB:
-
cAMP response element-binding protein
- Ct:
-
threshold cycle
- DARPP-32:
-
dopamine- and cAMP-regulated phosphoprotein of 32 kDa
- DREADD:
-
designer receptor exclusively activated by designer drug
- ERK:
-
extracellular signal-regulated kinase
- GAD-67:
-
glutamic acid decarboxylase 67 kDa isoform
- GFAP:
-
glial fibrillary acidic protein
- HD:
-
Huntington’s disease
- JNK:
-
c-Jun N-terminal kinase
- MSN:
-
medium-sized spiny neuron
- mTORC1:
-
mammalian target of rapamycin complex 1
- NMDA:
-
N-methyl-d-aspartate
- NPAS4:
-
neuronal PAS domain protein 4
- PI3K:
-
phosphatidylinositol 3-kinase
- PKA:
-
cAMP-dependent protein kinase
- PSD-95:
-
post-synaptic density protein 95
- THC:
-
Δ9-tetrahydrocannabinol
- USF:
-
upstream stimulatory factor
References
Katona I, Freund TF . Endocannabinoid signaling as a synaptic circuit breaker in neurological disease. Nat Med 2008; 14: 923–930.
Gaoni Y, Mechoulam R . Isolation, structure and partial synthesis of an active constituent of hashish. J Am Chem Soc 1964; 86: 1646–1647.
Piomelli D . The molecular logic of endocannabinoid signalling. Nat Rev Neurosci 2003; 4: 873–884.
Fernandez-Ruiz J, Moreno-Martet M, Rodriguez-Cueto C, Palomo-Garo C, Gomez-Canas M, Valdeolivas S et al. Prospects for cannabinoid therapies in basal ganglia disorders. Br J Pharmacol 2011; 163: 1365–1378.
Gowran A, Noonan J, Campbell VA . The multiplicity of action of cannabinoids: implications for treating neurodegeneration. CNS Neurosci Ther 2011; 17: 637–644.
Shohami E, Cohen-Yeshurun A, Magid L, Algali M, Mechoulam R . Endocannabinoids and traumatic brain injury. Br J Pharmacol 2011; 163: 1402–1410.
Galve-Roperh I, Aguado T, Palazuelos J, Guzman M . Mechanisms of control of neuron survival by the endocannabinoid system. Curr Pharm Des 2008; 14: 2279–2288.
Marsicano G, Goodenough S, Monory K, Hermann H, Eder M, Cannich A et al. CB1 cannabinoid receptors and on-demand defense against excitotoxicity. Science 2003; 302: 84–88.
Chiarlone A, Bellocchio L, Blazquez C, Resel E, Soria-Gomez E, Cannich A et al. A restricted population of CB1 cannabinoid receptors with neuroprotective activity. Proc Natl Acad Sci USA 2014; 111: 8257–8262.
Park H, Poo MM . Neurotrophin regulation of neural circuit development and function. Nat Rev Neurosci 2013; 14: 7–23.
D'Souza DC, Pittman B, Perry E, Simen A . Preliminary evidence of cannabinoid effects on brain-derived neurotrophic factor (BDNF) levels in humans. Psychopharmacology (Berl) 2009; 202: 569–578.
Kreitzer AC . Physiology and pharmacology of striatal neurons. Annu Rev Neurosci 2009; 32: 127–147.
Ivkovic S, Ehrlich ME . Expression of the striatal DARPP-32/ARPP-21 phenotype in GABAergic neurons requires neurotrophins in vivo and in vitro. J Neurosci 1999; 19: 5409–5419.
Rauskolb S, Zagrebelsky M, Dreznjak A, Deogracias R, Matsumoto T, Wiese S et al. Global deprivation of brain-derived neurotrophic factor in the CNS reveals an area-specific requirement for dendritic growth. J Neurosci 2010; 30: 1739–1749.
Li Y, Yui D, Luikart BW, McKay RM, Rubenstein JL, Parada LF . Conditional ablation of brain-derived neurotrophic factor-TrkB signaling impairs striatal neuron development. Proc Natl Acad Sci USA 2012; 109: 15491–15496.
Pazos MR, Sagredo O, Fernandez-Ruiz J . The endocannabinoid system in Huntington's disease. Curr Pharm Des 2008; 14: 2317–2325.
Zuccato C, Cattaneo E . Brain-derived neurotrophic factor in neurodegenerative diseases. Nat Rev Neurol 2009; 5: 311–322.
Gines S, Bosch M, Marco S, Gavalda N, Diaz-Hernandez M, Lucas JJ et al. Reduced expression of the TrkB receptor in Huntington's disease mouse models and in human brain. Eur J Neurosci 2006; 23: 649–658.
Blazquez C, Chiarlone A, Sagredo O, Aguado T, Pazos MR, Resel E et al. Loss of striatal type 1 cannabinoid receptors is a key pathogenic factor in Huntington's disease. Brain 2011; 134: 119–136.
Xie Y, Hayden MR, Xu B . BDNF overexpression in the forebrain rescues Huntington's disease phenotypes in YAC128 mice. J Neurosci 2010; 30: 14708–14718.
Jiang M, Peng Q, Liu X, Jin J, Hou Z, Zhang J et al. Small-molecule TrkB receptor agonists improve motor function and extend survival in a mouse model of Huntington's disease. Hum Mol Genet 2013; 22: 2462–2670.
Simmons DA, Belichenko NP, Yang T, Condon C, Monbureau M, Shamloo M et al. A small molecule TrkB ligand reduces motor impairment and neuropathology in R6/2 and BACHD mouse models of Huntington's disease. J Neurosci 2013; 33: 18712–18727.
Pertwee RG, Howlett AC, Abood ME, Alexander SP, Di Marzo V, Elphick MR et al. International Union of Basic and Clinical Pharmacology. LXXIX. Cannabinoid receptors and their ligands: beyond CB1 and CB2 . Pharmacol Rev 2010; 62: 588–631.
Trettel F, Rigamonti D, Hilditch-Maguire P, Wheeler VC, Sharp AH, Persichetti F et al. Dominant phenotypes produced by the HD mutation in STHdh(Q111) striatal cells. Hum Mol Genet 2000; 9: 2799–2809.
Gines S, Ivanova E, Seong IS, Saura CA, MacDonald ME . Enhanced Akt signaling is an early pro-survival response that reflects N-methyl-D-aspartate receptor activation in Huntington's disease knock-in striatal cells. J Biol Chem 2003; 278: 50514–50522.
Xifro X, Garcia-Martinez JM, Del Toro D, Alberch J, Perez-Navarro E . Calcineurin is involved in the early activation of NMDA-mediated cell death in mutant huntingtin knock-in striatal cells. J Neurochem 2008; 105: 1596–1612.
Marullo M, Valenza M, Leoni V, Caccia C, Scarlatti C, De Mario A et al. Pitfalls in the detection of cholesterol in Huntington's disease models. PLoS Curr 2012; 4: e505886e9a1968.
Pruunsild P, Kazantseva A, Aid T, Palm K, Timmusk T . Dissecting the human BDNF locus: bidirectional transcription, complex splicing, and multiple promoters. Genomics 2007; 90: 397–406.
Aid T, Kazantseva A, Piirsoo M, Palm K, Timmusk T . Mouse and rat BDNF gene structure and expression revisited. J Neurosci Res 2007; 85: 525–535.
Pruunsild P, Sepp M, Orav E, Koppel I, Timmusk T . Identification of cis-elements and transcription factors regulating neuronal activity-dependent transcription of human BDNF gene. J Neurosci 2011; 31: 3295–3308.
Zheng F, Zhou X, Luo Y, Xiao H, Wayman G, Wang H . Regulation of brain-derived neurotrophic factor exon IV transcription through calcium responsive elements in cortical neurons. PLoS One 2011; 6: e28441.
Armbruster BN, Li X, Pausch MH, Herlitze S, Roth BL . Evolving the lock to fit the key to create a family of G protein-coupled receptors potently activated by an inert ligand. Proc Natl Acad Sci USA 2007; 104: 5163–5168.
Lee HM, Giguere PM, Roth BL . DREADDs: novel tools for drug discovery and development. Drug Discov Today 2014; 19: 469–473.
Alexander GM, Rogan SC, Abbas AI, Armbruster BN, Pei Y, Allen JA et al. Remote control of neuronal activity in transgenic mice expressing evolved G protein-coupled receptors. Neuron 2009; 63: 27–39.
Mangiarini L, Sathasivam K, Seller M, Cozens B, Harper A, Hetherington C et al. Exon 1 of the HD gene with an expanded CAG repeat is sufficient to cause a progressive neurological phenotype in transgenic mice. Cell 1996; 87: 493–506.
Denovan-Wright EM, Robertson HA . Cannabinoid receptor messenger RNA levels decrease in a subset of neurons of the lateral striatum, cortex and hippocampus of transgenic Huntington's disease mice. Neuroscience 2000; 98: 705–713.
McCaw EA, Hu H, Gomez GT, Hebb AL, Kelly ME, Denovan-Wright EM . Structure, expression and regulation of the cannabinoid receptor gene (CB1) in Huntington's disease transgenic mice. Eur J Biochem 2004; 271: 4909–4920.
Casteels C, Vandeputte C, Rangarajan JR, Dresselaers T, Riess O, Bormans G et al. Metabolic and type 1 cannabinoid receptor imaging of a transgenic rat model in the early phase of Huntington disease. Exp Neurol 2011; 229: 440–449.
Richfield EK, Herkenham M . Selective vulnerability in Huntington's disease: preferential loss of cannabinoid receptors in lateral globus pallidus. Ann Neurol 1994; 36: 577–584.
Glass M, Dragunow M, Faull RL . The pattern of neurodegeneration in Huntington's disease: a comparative study of cannabinoid, dopamine, adenosine and GABA(A) receptor alterations in the human basal ganglia in Huntington's disease. Neuroscience 2000; 97: 505–519.
Mievis S, Blum D, Ledent C . Worsening of Huntington disease phenotype in CB1 receptor knockout mice. Neurobiol Dis 2011; 42: 524–529.
Breivogel CS, Sim LJ, Childers SR . Regional differences in cannabinoid receptor/G-protein coupling in rat brain. J Pharmacol Exp Ther 1997; 282: 1632–1642.
Steindel F, Lerner R, Haring M, Ruehle S, Marsicano G, Lutz B et al. Neuron-type specific cannabinoid-mediated G protein signalling in mouse hippocampus. J Neurochem 2013; 124: 795–807.
Selley DE, Rorrer WK, Breivogel CS, Zimmer AM, Zimmer A, Martin BR et al. Agonist efficacy and receptor efficiency in heterozygous CB1 knockout mice: relationship of reduced CB1 receptor density to G-protein activation. J Neurochem 2001; 77: 1048–1057.
Greer PL, Greenberg ME . From synapse to nucleus: calcium-dependent gene transcription in the control of synapse development and function. Neuron 2008; 59: 846–860.
Hong EJ, McCord AE, Greenberg ME . A biological function for the neuronal activity-dependent component of Bdnf transcription in the development of cortical inhibition. Neuron 2008; 60: 610–624.
Tao X, West AE, Chen WG, Corfas G, Greenberg ME . A calcium-responsive transcription factor, CaRF, that regulates neuronal activity-dependent expression of BDNF. Neuron 2002; 33: 383–395.
Bloodgood BL, Sharma N, Browne HA, Trepman AZ, Greenberg ME . The activity-dependent transcription factor NPAS4 regulates domain-specific inhibition. Nature 2013; 503: 121–125.
Derkinderen P, Valjent E, Toutant M, Corvol JC, Enslen H, Ledent C et al. Regulation of extracellular signal-regulated kinase by cannabinoids in hippocampus. J Neurosci 2003; 23: 2371–2382.
Khaspekov LG, Brenz Verca MS, Frumkina LE, Hermann H, Marsicano G, Lutz B . Involvement of brain-derived neurotrophic factor in cannabinoid receptor-dependent protection against excitotoxicity. Eur J Neurosci 2004; 19: 1691–1698.
Rubino T, Vigano D, Premoli F, Castiglioni C, Bianchessi S, Zippel R et al. Changes in the expression of G protein-coupled receptor kinases and beta-arrestins in mouse brain during cannabinoid tolerance: a role for RAS-ERK cascade. Mol Neurobiol 2006; 33: 199–213.
Aso E, Ozaita A, Valdizan EM, Ledent C, Pazos A, Maldonado R et al. BDNF impairment in the hippocampus is related to enhanced despair behavior in CB1 knockout mice. J Neurochem 2008; 105: 565–572.
Beyer CE, Dwyer JM, Piesla MJ, Platt BJ, Shen R, Rahman Z et al. Depression-like phenotype following chronic CB1 receptor antagonism. Neurobiol Dis 2010; 39: 148–155.
Ferreira-Vieira TH, Bastos CP, Pereira GS, Moreira FA, Massensini AR . A role for the endocannabinoid system in exercise-induced spatial memory enhancement in mice. Hippocampus 2014; 24: 79–88.
Butovsky E, Juknat A, Goncharov I, Elbaz J, Eilam R, Zangen A et al. In vivo up-regulation of brain-derived neurotrophic factor in specific brain areas by chronic exposure to delta-9-tetrahydrocannabinol. J Neurochem 2005; 93: 802–811.
Altar CA, Cai N, Bliven T, Juhasz M, Conner JM, Acheson AL et al. Anterograde transport of brain-derived neurotrophic factor and its role in the brain. Nature 1997; 389: 856–860.
Timmusk T, Lendahl U, Funakoshi H, Arenas E, Persson H, Metsis M . Identification of brain-derived neurotrophic factor promoter regions mediating tissue-specific, axotomy-, and neuronal activity-induced expression in transgenic mice. J Cell Biol 1995; 128: 185–199.
Canals JM, Marco S, Checa N, Michels A, Perez-Navarro E, Arenas E et al. Differential regulation of the expression of nerve growth factor, brain-derived neurotrophic factor, and neurotrophin-3 after excitotoxicity in a rat model of Huntington's disease. Neurobiol Dis 1998; 5: 357–364.
Her LS, Goldstein LS . Enhanced sensitivity of striatal neurons to axonal transport defects induced by mutant huntingtin. J Neurosci 2008; 28: 13662–13672.
Hasbi A, Fan T, Alijaniaram M, Nguyen T, Perreault ML, O'Dowd BF et al. Calcium signaling cascade links dopamine D1-D2 receptor heteromer to striatal BDNF production and neuronal growth. Proc Natl Acad Sci USA 2009; 106: 21377–21382.
De Chiara V, Angelucci F, Rossi S, Musella A, Cavasinni F, Cantarella C et al. Brain-derived neurotrophic factor controls cannabinoid CB1 receptor function in the striatum. J Neurosci 2010; 30: 8127–8137.
The Huntington's Disease Collaborative Research Consortium. A novel gene containing a trinucleotide repeat that is expanded and unstable on Huntington's disease chromosomes. Cell 1993; 72: 971–983.
Benito C, Nunez E, Tolon RM, Carrier EJ, Rabano A, Hillard CJ et al. Cannabinoid CB2 receptors and fatty acid amide hydrolase are selectively overexpressed in neuritic plaque-associated glia in Alzheimer's disease brains. J Neurosci 2003; 23: 11136–11141.
Ramirez BG, Blazquez C, Gomez del Pulgar T, Guzman M, de Ceballos ML . Prevention of Alzheimer's disease pathology by cannabinoids: neuroprotection mediated by blockade of microglial activation. J Neurosci 2005; 25: 1904–1913.
Bedse G, Romano A, Cianci S, Lavecchia AM, Lorenzo P, Elphick MR et al. Altered expression of the CB1 cannabinoid receptor in the triple transgenic mouse model of Alzheimer's disease. J Alzheimers Dis 2014; 40: 701–712.
Plotkin JL, Day M, Peterson JD, Xie Z, Kress GJ, Rafalovich I et al. Impaired TrkB receptor signaling underlies corticostriatal dysfunction in Huntington's disease. Neuron 2014; 83: 178–188.
Monory K, Massa F, Egertova M, Eder M, Blaudzun H, Westenbroek R et al. The endocannabinoid system controls key epileptogenic circuits in the hippocampus. Neuron 2006; 51: 455–466.
Guggenhuber S, Monory K, Lutz B, Klugmann M . AAV vector-mediated overexpression of CB1 cannabinoid receptor in pyramidal neurons of the hippocampus protects against seizure-induced excitoxicity. PLoS One 2010; 5: e15707.
Benito C, Romero JP, Tolon RM, Clemente D, Docagne F, Hillard CJ et al. Cannabinoid CB1 and CB2 receptors and fatty acid amide hydrolase are specific markers of plaque cell subtypes in human multiple sclerosis. J Neurosci 2007; 27: 2396–2402.
Marsicano G, Wotjak CT, Azad SC, Bisogno T, Rammes G, Cascio MG et al. The endogenous cannabinoid system controls extinction of aversive memories. Nature 2002; 418: 530–534.
Acknowledgements
This work was supported by Spanish Ministerio de Economía y Competitividad (Grant no. SAF2012-35759) and Comunidad de Madrid (Grant no. S2010/BMD-2308) to MG, as well as by Estonian Ministry of Education and Research (Grant no. 0140143, IUT 19-18), Estonian Science Foundation (Grant no. 8844) and Estonian Academy of Sciences to PP and TT. AC is supported by Ministerio de Economía y Competitividad (FPI Program). LB is supported by an EMBO Long-Term Fellowship. We are grateful to Andrés de la Rocha, Alba Revilla, Elena García-Taboada, Carmen Vázquez, Cristina Benito and Julián Romero for expert technical assistance, and to Ana Rebolledo for helping in the provision of human samples.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Edited by L Greene
Supplementary Information accompanies this paper on Cell Death and Differentiation website
Supplementary information
Rights and permissions
Cell Death and Disease is an open-access journal published by Nature Publishing Group. This work is licensed under a Creative Commons Attribution 4.0 International Licence. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons licence, users will need to obtain permission from the licence holder to reproduce the material. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0
About this article
Cite this article
Blázquez, C., Chiarlone, A., Bellocchio, L. et al. The CB1 cannabinoid receptor signals striatal neuroprotection via a PI3K/Akt/mTORC1/BDNF pathway. Cell Death Differ 22, 1618–1629 (2015). https://doi.org/10.1038/cdd.2015.11
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cdd.2015.11
This article is cited by
-
Opposite physiological and pathological mTORC1-mediated roles of the CB1 receptor in regulating renal tubular function
Nature Communications (2022)
-
Apelin 13 Improves Anxiety and Cognition Via Hippocampal Increases BDNF Expression and Reduction Cell Death in Neonatal Alcohol Exposed Rats
International Journal of Peptide Research and Therapeutics (2021)
-
Cannabinoids and their derivatives in struggle against melanoma
Pharmacological Reports (2021)
-
Effect of acute physical exercise on motor sequence memory
Scientific Reports (2020)
-
Organized cannabinoid receptor distribution in neurons revealed by super-resolution fluorescence imaging
Nature Communications (2020)