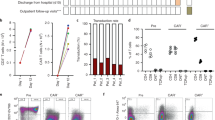
Abstract
Successful utilization of SCT modalities often requires utilization of both red cell and platelet transfusions. In this retrospective evaluation of clinical factors affecting transplant engraftment and transfusion utilization at a single transplant center in 505 patients from 2005 through 2009, we found that graft type, donor type and the conditioning regimen intensity significantly affected both the neutrophil engraftment time (P<0.001) and the platelet engraftment time (P<0.001). SCT patients required an average of 6.2 red cell units, and 7.9 platelet transfusions in the first 100 days with a wide s.d. Among auto-SCT patients, 5% required neither RBC nor platelet transfusions. Some reduced-intensity transplants were also associated with no transfusion need, and in allogeneic transplants, conditioning regimen intensity was positively correlated with platelet transfusion events as assessed by multivariate analysis. Other patient characteristics such as gender, graft type, donor type, underlying disease and use of TBI were all independently associated with transfusion needs in SCT patients. Further studies are required to understand the means to minimize transfusions and potential related complications in SCT patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Sullivan KM, Parkman R, Walters MC . Bone marrow transplantation for non-malignant disease. Am Soc Hematol Educ Program 2000;, 319–338 (PMID: 11701549).
Meijer E, Dekker AW, Lokhorst HM, Petersen EJ, Nieuwenhuis HK, Verdonck LF . Low incidence of infectious complications after nonmyeloablative compared with myeloablative allogeneic stem cell transplantation. Transpl Infect Dis 2004; 6: 171–178.
Yamazaki R, Kuwana M, Mori T, Okazaki Y, Kawakami Y, Ikeda Y et al. Prolonged thrombocytopenia after allogeneic hematopoietic stem cell transplantation: associations with impaired platelet production and increased platelet turnover. Bone Marrow Transplant 2006; 38: 377–384.
Link H, Boogaerts MA, Carella AM, Ferrant A, Gadner H, Gorin NC et al. A controlled trial of recombinant human granulocyte-macrophage colony-stimulating factor after total body irradiation, high-dose chemotherapy, and autologous bone marrow transplantation for acute lymphoblastic leukemia or malignant lymphoma. Blood 1992; 80: 2188–2195.
Trivedi M, Martinez S, Corringham S, Medley K, Ball ED . Optimal use of G-CSF administration after hematopoietic SCT. Bone Marrow Transplant 2009; 43: 895–908.
Grewal SS, Barker JN, Davies SM, Wagner JE . Unrelated donor hematopoietic cell transplantation: marrow or umbilical cord blood? Blood 2003; 101: 4233–4244.
Solh M, Brunstein C, Morgan S, Weisdorf D . Platelet and red blood cell utilization and transfusion independence in umbilical cord blood and allogeneic peripheral blood hematopoietic cell transplants. Biol Blood Marrow Transplant 2011; 17: 710–716.
Ramírez P, Brunstein CG, Miller B, Defor T, Weisdorf D . Delayed platelet recovery after allogeneic transplantation: a predictor of increased treatment-related mortality and poorer survival. Bone Marrow Transplant 2011; 46: 981–986.
Kanda J, Kawabata H, Chao NJ . Iron overload and allogeneic hematopoietic stem-cell transplantation. Expert Rev Hematol 2011; 4: 71–80.
Sloan JM, Ballen K . SCT in Jehovah’s witnesses: the bloodless transplant. Bone Marrow Transplant 2008; 41: 837–844.
Gajewski JL, Johnson VV, Sandler SG, Sayegh A, Klumpp TR . A review of transfusion practice before, during, and after hematopoietic progenitor cell transplantation. Blood 2008; 112: 3036–3047.
Stroncek D, Rebullo P . Platelet transfusions. Lancet 2007; 370: 427–438.
British Committee for Standards in Haematology, Blood Transfusion Task Force. Guidelines for the use of platelet transfusions. Br J Haematol 2003; 122: 10–23.
Schichter SJ, Kaufman RM, Assmann SF, McCullough J, Triuizi DJ, Strauss RG et al. Dose of prophylactic platelet transfusions and prevention of hemorrhage. N Engl J Med 2010; 362: 600–613.
Wandt H, Schaefer-Eckart K, Frank M, Birkmann J, Wilhelm M . A therapeutic platelet transfusion strategy is safe and feasible in patients after autologous peripheral blood stem cell transplantation. Bone Marrow Transplant 2006; 37: 387–392.
Radia R, Pamphilon D . Transfusion strategies in patients undergoing stem-cell transplantation. Expert Rev Hematol 2011; 4: 213–220.
Bernstein SH, Nademanee AP, Vose JM, Tricot G, Fay JW, Negrin RS et al. A multicenter study of platelet recovery and utilization in patients after myeloablative therapy and hematopoietic stem cell transplantation. Blood 1998; 91: 3509–3517.
Prebet T, Ladaique P, Ferrando M, Chabannon C, Faucher C, De Lavallade H et al. Platelet recovery and transfusion needs after reduced intensity conditioning allogeneic peripheral blood stem cell transplantation. Exp Hematol 2010; 83: 55–60.
Ganguly S, Bradley JP, Patel JS, Tilzer L . Role of transfusion in stem cell transplantation: a freedom-from-transfusion (FFT), cost and survival analysis. J Med Econ 2010; 13: 55–62.
Pihlstedt P, Paulin T, Sundberg B, Nilsson B, Ringden O . Blood transfusion in marrow graft recipients. Ann Hematol 1992; 65: 66–70.
Osterwalder B, Gratwohl A, Reusser P, Tichelli A, Speck B . Hematological support in patients undergoing allogeneic bone marrow transplantation. Recent Results Cancer Res 1988; 108: 44–52.
Schuster RS . Stem cell transplantation and hematopoietic growth factors. Curr Hematol Rep 2002; 1: 103–109.
Bussel JB, Pinheiro MP . Eltrombopag. Cancer Treat Res 2011; 157: 289–303.
Kuter DJ . Romiplostim. Cancer Treat Res 2011; 157: 267–288.
Acknowledgements
This study was supported in part by a Robert I Weed Summer Student Hematology Fellowship (to JP) and in part by federal funds from the Biomedical Advanced Research and Development Authority (BARDA), Office of the Assistant Secretary for Preparedness and Response, Office of the Secretary, Department of Health and Human Services (HHS), under Contract No. HHSO100200800058C (to YC). We thank Elva Mikk for aid in manuscript preparation and Diane Nichols for data management.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Liesveld, J., Pawlowski, J., Chen, R. et al. Clinical factors affecting engraftment and transfusion needs in SCT: a single-center retrospective analysis. Bone Marrow Transplant 48, 691–697 (2013). https://doi.org/10.1038/bmt.2012.194
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2012.194
Keywords
This article is cited by
-
Red blood cell transfusion burden by day 30 predicts mortality in adults after single-unit cord blood transplantation
Bone Marrow Transplantation (2019)
-
Beyond immune thrombocytopenia: the evolving role of thrombopoietin receptor agonists
Annals of Hematology (2017)
-
Impact of ABO blood group mismatch in alemtuzumab-based reduced-intensity conditioned haematopoietic SCT
Bone Marrow Transplantation (2015)